Abstract
Anti-pronation taping is a treatment technique commonly used by clinicians in the management of lower extremity musculoskeletal pain and injury. The clinical efficacy of anti-pronation tape is described anecdotally and has some support through clinical trials for some foot conditions. However, the mechanism(s) underlying its clinical efficacy is unknown, but are broadly categorized under mechanical, neurophysiological and psychological hypotheses. This article explores these hypotheses and contributes to the understanding of the technique.
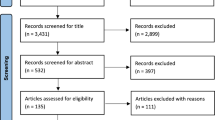
A computer database search was conducted to identify relevant experimental studies using an a priori defined search strategy. Data were extracted from reviewed articles and wherever possible mean differences between baseline and taped condition and the 95% confidence interval, as well as percentage change scores and effect size statistics were calculated. Articles were organized pertaining to the hypothetical mechanism investigated and presented accordingly into biomechanical, neurophysiological or psychological paradigms.
Overall, the research to date has focused predominantly on the mechanical paradigm with far fewer papers being found for the neurophysiological and psychological paradigms. The literature provides evidence that anti-pronation tape has a biomechanical effect, which has been demonstrated by increases in navicular height and medial longitudinal arch height, reductions in tibial internal rotation and calcaneal eversion and alteration of plantar pressure patterns, under both static (i.e. standing) and dynamic (i.e. walking, jogging, running) conditions. The reduction in pronation was dependent on the surrogate measure of pronation used, but generally ranged from as little as 5% increase in longitudinal arch height during jogging to as much as a 33% change in calcaneal eversion during walking. Preliminary evidence from few studies suggests that anti-pronation tape has a neurophysiological effect as it has been shown to reduce the activity of several muscles of the leg during dynamic tasks such as walking, hopping, cutting, back pedalling and drop jumps. Data were difficult to extract from these papers, but it would appear from a small study that the reduction is in the order of about 45% for tibialis posterior.
To date, there has been limited investigation of the psychological effects of anti-pronation tape. A main issue, as with most placebo or sham interventions for physical therapy research, is that of an appropriate comparator in this regard. Consequently, these effects are currently not well understood.
This article reports of evidence in support of anti-pronation tape exerting a biomechanical effect. As its name suggests, it does reduce pronation. There is emerging evidence of a neurophysiological effect, which is generally one of reduction in muscle activity, but caution is urged in over-interpreting a few studies on small sample sizes. Further research is required in this paradigm before sports medicine practitioners can utilize these findings in day-to-day clinical practice. Due to insufficient evidence, this article was unable to draw any conclusions as to the psychological effects of the tape, but the article does prompt the need for further exploration into the possible role of placebo in the clinical effects of antipronation taping.





Similar content being viewed by others
References
Dye RW. A strapping. J Natl Assoc Chiropodists 1939; 29: 11–2
van Gent RN, Siem D, van Middelkoop M, et al. Incidence and determinants of lower extremity running injuries in long dis tance runners: a systematic review. Br J Sports Med 2007; 41:469–80
Tauntan J, Ryan M, Clement D, et al. A retrospective case control analysis of 2002 running injuries. Br J Sports Med 2002; 36(2)1: 95–101
Jamali B, Walker M, Hoke B, et al. Windlass taping technique for symptomatic relief of plantar fasciitis. J Sport Rehab 2004; 13(3): 228–43
Saxelby J, Betts RP, Bygrave CJ. ‘Low-dye’ taping on the foot in the management of plantar-fasciitis. Foot 1997; 7(4): 205–9
Landorf KB, Radford JA Keenan AM, et al. Effectiveness of low-Dye taping for the short-term management of plantar fasciitis. J Am Podiatr Med Assoc 2005; 95(6): 525–30
Hyland MR, Webber-Gaffney A, Cohen L, et al. Randomised controlled trial of calcaneal taping, sham taping, and plantar fascia stretching for the short-term management of plantar heel pain. J Orthop Sports Phys Ther 2006; 36(6): 364–71
Radford JA, Landorf KB, Buchbinder R, et al. Effectiveness of low-Dye taping for the short-term treatment of plantar heel pain: a randomised trial. BMC Musculoskelet Disord 2006; 7:64
Hlavac HF. The foot book. Mountain View (CA): World Publications, 1977
Keenan AM, Tanner CM. The effect of high-Dye and low-Dye taping on rearfoot motion. J Am Podiatr Med Assoc 2001; 91(5): 255
Ator R, Gunn K, McPoil T, et al. The effect of adhesive strapping on medial longitudinal arch support before and after exercise. J Orthop Sports Phys Ther 1991; 14: 18–23
del Rossi G, Fiolkowski P, Horodyski MB, et al. For how long do temporary techniques maintain the height of the medicallongitudinal arch? Phys Ther Sport 2004; 5(2): 84–9
Scranton PE, Pedegana LR, Whitesel JP. Gait analysis: alterations in support phase forces using supportive devices. Am J Sports Med 1982; 10(1): 6–11
Harradine P, Herrington L, Wright R. The effect of low Dye taping upon rearfoot motion and position before and after exercise. Foot 2001; 11(2): 57–60
Holmes CF, Wilcox D, Fletcher JP. Effect of a modified, low dye medial longitudinal arch taping procedure on the subtalar joint neutral position before and after light exercise. J Orthop Sports Phys Ther 2002; 32(5): 194–201
Kersting UG. The role of footwear-independent variations in rearfoot movement on impact attenuation in heel-toe running. Res Sports Med 2006; 14: 117–34
Moss CL, Gorton B, Deters S. A comparison of prescribed rigid orthotic devices and athletic taping support used to modify pronation in runners. J Sport Rehab 1993; 2(3): 179–88
Vicenzino B, Feilding J, Howard R, et al. An investigation of the pronation effect of two taping methods after applicationand exercise [abstract]. Gait Posture 1997; 5(1): 1
Hopkins W. A new view of statistics. Internet Society for Sport Science [online]. Available from URL: http://www.sport sci.org/resource/stats. [Accessed 2007 Jan 13]
Subotnick SI. Use of tape for prevention and treatment of lower extremity athletic injuries. Mount Kisco (NY): Futura Publishing Co., 1975
Bartold SJ. The plantar fascia as a source of pain: biomechanics, presentation and treatment. J Bodywork Move Ther 2004; 8(3): 214–26
Vicenzino B, Griffiths SR, Griffiths LA, et al. Effect of antipronation tape and temporary orthotic on vertical navicular height before and after exercise. J Orthop Sports Phys Ther 2000; 30(6): 333
Meyer J, Kulig K, Landel R. Differential diagnosis and treatment of subcalcaneal heel pain: a case report. including commentary by Donatelli R with author response. J Orthop Sports Phys Ther 2002; 32(3): 114–24
Russo SJ, Chipchase LS. The effect of low-Dye taping on peak plantar pressures of normal feet during gait. Aust J Physiother 2001; 47(4): 239
Whitaker J, Kazuto A, Ishii S. Effect of the low-dye strap on pronation-sensitive mechanical attributes of the foot. J Am Podiatr Assoc 2003; 93(2): 118–23
Schulthies SS, Draper DO. A modified low-dye taping technique to support the medial longitudinal arch and reducee xcessive pronation. J Athlet Train 1995; 30(3): 266
McCloskey PJ. A study of the effect of Low Dye taping on the foot.Br J Podiatric Med Surg 1992; 4(3): 6–9
Wall K, Swanik K, Swanik C, et al. Augmented low-dye arch taping affects on muscle activity and ground reaction forces in people with pes planus. J Athlet Train 2005; 40(2): S–97
Crosby W, Humble RN. Rehabilitation of plantar facsciitis. Clin Podiatr Med Surg 2001; 18(2): 225–31
Vicenzino B, Franettovich M, McPoil T, et al. Initial effects of antipronation tape on the medial longitudinal arch during walking and running. Br J Sports Med 2005; 39(12): 939
Hadley A, Griffiths S, Griffiths L, et al. Antipronation taping and temporary orthoses: effects on tibial rotation position after exercise. J Am Podiatr Med Assoc 1999; 89(3): 118
Lange B, Chipchase L, Evans A. The effect of low-dye taping on plantar pressures, during gait, in subjects with navicular drop exceeding 10 mm. J Orthop Sports Phys Ther 2004; 34(4): 201–9
Sanzo P, Bauer T. The effects of low dye taping on foot pressure in subjects with plantar fasciitis. Proceedings of the XIII International Symposium for Biomechanics in Sport; 1996 Jul 18-22; Thunder Bay (ON): Lakehead University, 1996: 13–5
Vicenzino B, McPoil T, Buckland S. Plantar foot pressures after the augmented low-dye taping technique. J Athlet Train 2006; 42(3): 374–80
Elizondo M, Wojciechowski R, Cordova M, et al. The effects of arch taping on vertical ground reaction forces generated during a drop landing. J Athlet Train 2004; 39 Suppl. 2: 101
Reinschmidt C van den Bogert AJ, Murphy N, et al. Tibiocalcaneal motion during running, measured with external and bone markers. Clin Biomech 1997; 12(1): 8–16
Williams DS, McClay IS. Measurements used to characterize the foot and the medial longitudinal arch: reliability and validity. Phys Ther 2000; 80(9): 864–71
Radford JA, Burns J, Buchbinder R, et al. The effect of Low Dye taping on kinematic, kinetic, and electromyographic variables: a systematic review. J Orthop Sports Phys Ther 2006; 36(4): 232–41
Inman VT. The influence of the foot-ankle complex on the proximal skeletal structures. Artif Limbs 1969; 13(1): 59–65
Areblad M, Nigg BM, Ekstrand J, et al. Three-dimensional measurement of rearfoot motion during running. J Biomech 1990; 23(9): 933–40
McClay I, Manal K. The influence of foot abduction on differences between two-dimensional and three-dimensional rearfoot motion. Foot Ankle Int 1998; 19(1): 26–31
Orlin MN, McPoil TG. Plantar pressure assessment. Phys Ther 2000; 80(4): 399–409
Cornwall MW, McPoil TG. Reliability and validity of center-of pressure quantification. J Am Podiatr Med Assoc 2003; 93:142–9
Nigg BM. The role of impact forces and foot pronation: a new paradigm. Clin J Sports Med 2001; 11: 2–9
Fallon JB, Bent LR, McNulty PA, et al. Evidence for strong synaptic coupling between single tactile afferents from the sole of the foot and motoneurons supplying leg muscles. J Neurophysiol 2005; 94: 3795–804
Layne CS, Forth KE, Abercromby FJ. Spatial factors and muscle spindle input influence the generation of neuromuscular responses to stimulation of the human foot. Acta Astronautica 2005; 56: 809–19
Franettovich M, Chapman A, Vicenzino B. Tape that increase medial longitudinal arch height also reduces leg muscle activity: a preliminary study. Med Sci Sports Exerc 2008; 40(4): 593–600
Boergers RJ. Effects of arch taping on peak force, surface contact area, and neuromuscular activity at midstance [dissertation]. Eugene (OR): University of Oregon, 2000
Yi CH, Brunt D, Kim HD, et al. Effect of ankle taping and exercise on EMG and kinetics during landing. J Phys Ther Sci 2003; 15(2): 81–5
Lohrer H, Alt W, Gollhofer A. Neuromuscular properties and functional aspects of taped ankles. Am J Sports Med 1999; 27(1): 69
Alt W, Lohrer H, Gollhofer A. Functional properties of adhesive ankle taping: neuromuscular and mechanical effects before and after exercise. Foot Ankle Int 1999; 20(4): 238
Shima N, Maeda A, Hirohashi K. Delayed latency of peroneal reflex to sudden inversion with ankle taping or bracing. Int J Sports Med 2005; 26(6): 476
Karlsson J, Andreasson GO. The effect of external ankle support in chronic lateral ankle joint instability: an electromyographic study. Am J Sports Med 1992; 20(3): 257
Herrington L, Malloy S, Richards J. The effect of patella taping on vastus medialis oblique and vastus laterialis EMG activity and knee kinematic variables during stair descent. J Electromyogr Kinesiol 2005; 15(6): 604–7
Christou EA. Patellar taping increases vastus medialis oblique activity in the presence of patellofemoral pain. J Electromyogr Kinesiol 2004; 14(4): 495
Ng GYF, Cheng JMF. The effects of patellar taping on pain and neuromuscular performance in subjects with patellofemoral pain syndrome. Clin Rehabil 2002; 16(8): 821
Cowan SM, Bennell KL, Hodges PW. Therapeutic patellar taping changes the timing of vasti muscle activation in people with patellofemoral pain syndrome. Clin J Sport Med 2002; 12(6): 339–47
Parsons D, Gilleard W. The effect of patellar taping on quadriceps activity onset in the absence of pain. J Appl Biomech 1999; 15(4): 373
Gilleard W, McConnell J, Parsons D. The effect of patellar taping on the onset of vastus medialis obliquus and vastus lateralis muscle activity in persons with patellofemoral pain.Phys Ther 1998; 78(1): 25
MacGregor K, Gerlach S, Mellor R, et al. Cutaneous stimulation from patella tape causes a differential increase in vasti muscle activity in people with patellofemoral pain. J Orthop Res 2005; 23 (2): 351
Boelens P, Loos T. The effect of ankle tape on lower limb muscle activity [abstract]. Phys Ther 1986; 66(5): 763
Loos T, Boelens P. The effect of ankle tape on lower limb muscle activity. Int J Sports Med 1984; Suppl. 5: 45–6
Alexander CM, McMullan M, Harrison PJ. What is the effect of taping along or across a muscle on motorneurone excitability? A study using triceps surae. Man Ther 2008; 13(1): 57–62
Gray ER. The role of leg muscles in variations of the arches in normal and flat feet. Phys Ther 1969; 49(10): 1084–8
Hunt AE, Smith RM. Mechanics and control of the flat versus normal foot during the stance phase of walking. Clin Biomech 2004; 19: 391–7
Gray EG, Basmajian JV. Electromyography and cinematography of leg and foot (‘normal’ and flat) during walking. Anat Rec 1968; 161(1): 1–15
Acknowledgements
Melinda Franettovich is supported by the National Health and Medical Research Council. Andrew Chapman is supported by the Australian Research Council.
There are no relevant conflicts of interest for any author.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Franettovich, M., Chapman, A., Blanch, P. et al. A Physiological and Psychological Basis for Anti-Pronation Taping from a Critical Review of the Literature. Sports Med 38, 617–631 (2008). https://doi.org/10.2165/00007256-200838080-00001
Published:
Issue Date:
DOI: https://doi.org/10.2165/00007256-200838080-00001