Abstract
Background
Shared decision making (SDM) combines evidence-based medicine with individual patient preferences. Patients who are actively engaged in their own health care management with their physicians have been shown to experience not only increased compliance, but also higher satisfaction and better outcomes. We hypothesize that a computer-based learning module for breast reconstruction increases patient involvement in the decision-making process.
Materials and Methods
Women who underwent either immediate or delayed breast reconstruction at an academic teaching hospital from 2004 to 2007 were identified. Patients meeting inclusion criteria were mailed questionnaires on demographics, informational resources, and decision-making processes. Questionnaire results were divided into 2 groups for analysis: patients who received a standard surgeon consultation and patients who were shown a computer-based decision aid in addition to the standard consultation.
Results
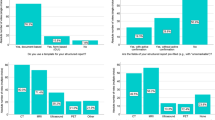
There were 358 women eligible for our study. A total of 255 patients (75.9%) responded to the survey; 168 patients were shown the computer-based decision aid and 87 patients were not. Patients who used the computer-based learning module reported a greater role in choosing the type of reconstruction (P < .001). Additionally, these patients reported a greater number of reconstructive options offered to them (P < .001) and were more satisfied with the amount of information provided by their reconstructive surgeon (P = .049).
Conclusions
A computer-based learning module allows patients to assimilate information and actively participate in choosing type of breast reconstruction. Use of this educational modality represents a simple and effective way to improve the shared decision-making process.

Similar content being viewed by others
References
Alderman AK, Wei Y, Birkmeyer JD. Use of breast reconstruction after mastectomy following the Women’s Health and Cancer Rights Act. JAMA. 2006;295:387–8.
Dean C, Chetty U, Forrest AP. Effects of immediate breast reconstruction on psychosocial morbidity after mastectomy. Lancet. 1983;1:459–62.
Charles C, Gafni A, Whelan T. Decision-making in the physician-patient encounter: revisiting the shared treatment decision-making model. Soc Sci Med. 1999;49:651–61.
Charles C, Gafni A, Whelan T. Shared decision-making in the medical encounter: what does it mean? (or it takes at least two to tango). Soc Sci Med. 1997;44:681–92.
Charles C, Gafni A, Whelan T. How to improve communication between doctors and patients. Learning more about the decision making context is important. BMJ. 2000;320:1220–1.
Coulter A. Partnerships with patients: the pros and cons of shared clinical decision-making. J Health Serv Res Policy. 1997;2:112–21.
Coulter A. Patient information and shared decision-making in cancer care. Br J Cancer. 2003;89:S15–6.
Coulter A, Ellins J. Effectiveness of strategies for informing, educating, and involving patients. BMJ. 2007;335:24–7.
Towle A, Godolphin W. Framework for teaching and learning informed shared decision making. BMJ. 1999;319:766–71.
Kaplan RM. Shared medical decision making. A new tool for preventive medicine. Am J Prev Med. 2004;26:81–3.
Sheridan SL, Harris RP, Woolf SH. Shared decision making about screening and chemoprevention. a suggested approach from the U.S. Preventive Services Task Force. Am J Prev Med. 2004;26:56–66.
Briss P, Rimer B, Reilley B, Coates RC, Lee NC, Mullen P, et al. Promoting informed decisions about cancer screening in communities and healthcare systems. Am J Prev Med. 2004;26:67–80.
Goodwin PJ, Black JT, Bordeleau LJ, Ganz PA. Health-related quality-of-life measurement in randomized clinical trials in breast cancer–taking stock. J Natl Cancer Inst. 2003;95:263–81.
Andersen MR, Bowen DJ, Morea J, Stein KD, Baker F. Involvement in decision-making and breast cancer survivor quality of life. Health Psychol. 2009;28:29–37.
Keating NL, Weeks JC, Borbas C, Guadagnoli E. Treatment of early stage breast cancer: do surgeons and patients agree regarding whether treatment alternatives were discussed? Breast Cancer Res Treat. 2003;79:225–31.
Keating NL, Guadagnoli E, Landrum MB, Borbas C, Weeks JC. Treatment decision making in early-stage breast cancer: should surgeons match patients’ desired level of involvement? J Clin Oncol. 2002;20:1473–9.
Waljee JF, Hawley S, Alderman AK, Morrow M, Katz SJ. Patient satisfaction with treatment of breast cancer: does surgeon specialization matter? J Clin Oncol. 2007;25:3694–8.
Katz SJ, Lantz PM, Janz NK, Fagerlin A, Schwartz K, Liu L, et al. Patient involvement in surgery treatment decisions for breast cancer. J Clin Oncol. 2005;23:5526–33.
Man-Son-Hing M, Laupacis A, O’Connor AM, Biggs J, Drake E, Yetsir E, Hart RG. A patient decision aid regarding antithrombotic therapy for stroke prevention in atrial fibrillation: a randomized controlled trial. JAMA. 1999;282:737–43.
Waljee JF, Rogers MA, Alderman AK. Decision aids and breast cancer: do they influence choice for surgery and knowledge of treatment options? J Clin Oncol. 2007;25:1067–73.
O’Brien MA, Whelan TJ, Villasis-Keever M, Gafni A, Charles C, Roberts R, et al. Are cancer-related decision aids effective? A systematic review and meta-analysis. J Clin Oncol. 2009;27:974–85.
Whelan T, Levine M, Willan A, Gafni A, Sanders K, Mirsky D, et al. Effect of a decision aid on knowledge and treatment decision making for breast cancer surgery: a randomized trial. JAMA. 2004;292:435–41.
Fallowfield LJ, Hall A, Maguire GP, Baum M. Psychological outcomes of different treatment policies in women with early breast cancer outside a clinical trial. BMJ. 1990;301:575–80.
Clauson J, Hsieh YC, Acharya S, Rademaker AW, Morrow M. Results of the Lynn Sage Second-Opinion Program for local therapy in patients with breast carcinoma. Changes in management and determinants of where care is delivered. Cancer. 2002;94:889–94.
Liang W, Burnett CB, Rowland JH, Meropol NJ, Eggert L, Hwang YT, et al. Communication between physicians and older women with localized breast cancer: implications for treatment and patient satisfaction. J Clin Oncol. 2002;20:1008–16.
Alderman AK, Hawley ST, Waljee J, Mujahid M, Morrow M, Katz SJ. Understanding the impact of breast reconstruction on the surgical decision-making process for breast cancer. Cancer. 2008;112:489–94.
Morrow M, Mujahid M, Lantz PM, Janz NK, Fagerlin A, Schwartz K, et al. Correlates of breast reconstruction: results from a population-based study. Cancer. 2005;104:2340–6.
Christian CK, Niland J, Edge SB, Ottesen RA, Hughes ME, Theriault R, et al. A multi-institutional analysis of the socioeconomic determinants of breast reconstruction: a study of the National Comprehensive Cancer Network. Ann Surg. 2006;243:241–9.
Yueh JH, Slavin SA, Bar-Meir ED, Merali HS, Houlihan MJ, Gautam S, et al. Impact of regional referral centers for microsurgical breast reconstruction: the New England perforator flap program experience. J Am Coll Surg. 2009;208:246–54.
Yermilov I, Chow W, Devgan L, Makary MA, Ko CY. What is the quality of surgery-related information on the internet? Lessons learned from a standardized evaluation of 10 common operations. J Am Coll Surg. 2008;207:580–6.
Moumjid N, Gafni A, Bremond A, Carrere MO. Shared decision making in the medical encounter: are we all talking about the same thing? Med Decis Making. 2007;27:539–46.
O’Connor AM, Mulley AG, Jr., Wennberg JE. Standard consultations are not enough to ensure decision quality regarding preference-sensitive options. J Natl Cancer Inst. 2003;95:570–1.
Graham ID, Logan J, O’Connor A, Weeks KE, Aaron S, Cranney A, et al. A qualitative study of physicians’ perceptions of three decision aids. Patient Educ Couns. 2003;50:279–83.
Heller L, Parker PA, Youssef A, Miller MJ. Interactive digital education aid in breast reconstruction. Plast Reconstr Surg. 2008;122:717–24.
Acknowledgments
The authors wish to acknowledge Sumner A. Slavin, MD and Donald J. Morris, MD for participation in the study. The authors also thank our breast surgeons Susan L. Troyan, MD, Mary Jane Houlihan, MD, and Valerie Staradub, MD for their help in patient recruitment. The work on this article was supported by grants from the Doris Duke Charitable Foundation (J.H.Y) and the Peter Jay Sharp Foundation (B.T.L, C.C., M.D.N., A.M.T.).
None of the authors have a financial interest in any of the products, devices, or drugs mentioned in this article.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Lee, B.T., Chen, C., Yueh, J.H. et al. Computer-Based Learning Module Increases Shared Decision Making in Breast Reconstruction. Ann Surg Oncol 17, 738–743 (2010). https://doi.org/10.1245/s10434-009-0869-7
Received:
Published:
Issue Date:
DOI: https://doi.org/10.1245/s10434-009-0869-7