Abstract
Background
Bilateral prophylactic mastectomy in women with increased breast cancer risk dramatically reduces breast cancer occurrence but little is known about psychosocial outcomes.
Methods
To examine long-term quality of life after bilateral prophylactic mastectomy, we mailed surveys to 195 women who had the procedure from 1979 to 1999 and to a random sample of 117 women at increased breast cancer risk who did not have the procedure. Measures were modeled on or drawn directly from validated instruments designed to assess quality of life, body image, sexuality, breast cancer concerns, depression, health perception, and demographic characteristics. We used logistic regression to examine associations between quality of life and other domains.
Results
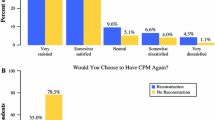
The response rate was 58%, with 106 women with and 62 women without prophylactic mastectomy returning complete surveys. Among women who underwent bilateral prophylactic mastectomy, 84% were satisfied with their decision to have the procedure; 61% reported high contentment with quality of life compared with an identical 61% of women who did not have the procedure (P = 1.0). Among all subjects, diminished contentment with quality of life was not associated with bilateral prophylactic mastectomy but with dissatisfaction with sex life (adjusted ratio [OR] = 2.5, 95% confidence interval [CI] = 1.0–6.2), possible depression (CES-D > 16, OR = 4.9, CI = 2.0–11.8), and poor or fair general health perception (OR = 8.3, 95% CI = 2.4–29.0).
Conclusions
The majority of women reported satisfaction with bilateral prophylactic mastectomy and experienced psychosocial outcomes similar to women with similarly elevated breast cancer risk who did not undergo prophylactic mastectomy. Bilateral prophylactic mastectomy appears to neither positively nor negatively impact long-term psychosocial outcomes.
Similar content being viewed by others
References
Pichert G, Bolliger B, Buser K, Pagani O. Evidence-based management options for women at increased breast/ovarian cancer risk. Ann Oncol 2003; 14:9–19
Hartmann LC, Schaid DJ, Woods JE, et al. Efficacy of bilateral prophylactic mastectomy in women with a family history of breast cancer. N Engl J Med 1999; 340:77–84
Hartmann LC, Sellers TA, Schaid DJ, et al. Efficacy of bilateral prophylactic mastectomy in BRCA1 and BRCA2 gene mutation carriers. J Natl Cancer Inst 2001; 93:1633–1637
Meijers-Heijboer H, van Geel B, van Putten WL, et al. Breast cancer after prophylactic bilateral mastectomy in women with a BRCA1 or BRCA2 mutation. N Engl J Med 2001; 345:159–164
Rebbeck TR, Friebel T, Lynch HT, et al. Bilateral prophylactic mastectomy reduces breast cancer risk in BRCA1 and BRCA2 mutation carriers: the PROSE Study Group. J Clin Oncol 2004; 22:1055–1062
Geiger AM, Yu O, Herrinton LJ, et al. A population-based study of bilateral prophylactic mastectomy efficacy in women at elevated risk for breast cancer in community practices. Arch Intern Med 2005; 165:516–520
Stefanek ME, Helzlsouer KJ, Wilcox PM, Houn F. Predictors of and satisfaction with bilateral prophylactic mastectomy. Prev Med 1995; 24:412–419
Borgen PI, Hill AD, Tran KN, et al. Patient regrets after bilateral prophylactic mastectomy. Ann Surg Oncol 1998; 5:603–606
Frost MH, Schaid DJ, Sellers TA, et al. Long-term satisfaction and psychological and social function following bilateral prophylactic mastectomy. JAMA 2000; 284:319–324
Hopwood P, Lee A, Shenton A, et al. Clinical follow-up after bilateral risk reducing (‘prophylactic’) mastectomy: mental health and body image outcomes. Psychooncology 2000; 9:462–472
Hatcher MB, Fallowfield L, A’Hern R. The psychosocial impact of bilateral prophylactic mastectomy: prospective study using questionnaires and semistructured interviews. BMJ 2001; 322:1–7
Metcalfe KA, Esplen MJ, Goel V, Narod SA. Psychosocial functioning in women who have undergone bilateral prophylactic mastectomy. Psychooncology 2004; 13:14–25
Metcalfe KA, Esplen MJ, Goel V, Narod SA. Predictors of quality of life in women with a bilateral prophylactic mastectomy. Breast J 2005; 11:65–69
Wagner EH, Greene SM, Hart G, et al. Building a research consortium of large health systems: the cancer research network. J Natl Cancer Inst Monogr 2005; 3–11
Dillman DA. (200) Mail and Internet Surveys. New York: John Wiley & Sons.
Brady MJ, Cella DF, Mo F, et al. Reliability and validity of the Functional Assessment of Cancer Therapy-Breast quality-of-life instrument. J Clin Oncol 1997; 15:974–986
Geiger AM, Mullen ES, Sloman PA, Edgerton BW, Petitti DB. Evaluation of a breast cancer patient information and support program. Eff Clin Pract 2000; 3:157–165
Horowitz M, Wilner N, Alvarez W. Impact of Event Scale: a measure of subjective stress. Psychosom Med 1979; 41:209–218
Hopwood P, Fletcher I, Lee A, Al Ghazal S. A body image scale for use with cancer patients. Eur J Cancer 2001; 37:189–197
Radloff LS. The CES-D Scale: A self-report depression scale for research in the general population. Appl Psychol Measure 1977; 1:385–401
Ware JE Jr, Sherbourne CD. The MOS 36-item short-form health survey (SF-36). I. Conceptual framework and item selection. Med Care 1992; 30:473–483
Centers for Disease Control and Prevention. Behaviorial Risk Factor Surveillance System, 2000 Questionnaire. Available at: http://www.cdc.gov/brfss/questionnaires/pdf-ques/2000brfss.pdf (last accessed April 29, 2006)
Willis GB. Cognitive Interviewing: A “How To” Guide. 1999. Available at: http://appliedresearch.cancer.gov/areas/cognitive/interview.pdf (last accessed April 30, 2006)
Willis GB, Lessler JT. Question Appraisal System (QAS-99). 1999. Available at: http://appliedresearch.cancer.gov/areas/cognitive/qas99.pdf (last accessed April 30, 3006)
Bromberger JT, Harlow S, Avis N, et al. Racial/ethnic differences in the prevalence of depressive symptoms among middle-aged women: The Study of Women’s Health Across the Nation (SWAN). Am J Public Health 2004; 94:1378–1385
Zahran HS, Kobau R, Moriarty DG, et al. Health-related quality of life surveillance—United States, 1993-2002. MMWR Surveill Summ 2005; 54:1–35
Metcalfe KA, Narod SA. Breast cancer risk perception among women who have undergone prophylactic bilateral mastectomy. J Natl Cancer Inst 2002; 94:1564–1569
Greene SM, Geiger AM, Harris E, Altschuler A, Nekhlyudov L, Barton M, Rolnick SJ, Fletcher S. Impact of IRB requirements on a multi-site Cancer Research Network study. Ann Epidemiol 2006; 16:275–278
Acknowledgment
This study was funded by the United States’ National Cancer Institute (U19 CA79689, Increasing Effectiveness of Cancer Control Interventions, Edward H. Wagner, M.D., P.I., and R01 CA090323, Patient Oriented Outcomes of Prophylactic Mastectomy, Ann M. Geiger, Ph.D., P.I.). Dr. Joann Elmore also was supported by the National Cancer Institute (K05 CA104699, Improving Accuracy and Outcomes of Breast Cancer Screening, Joann G. Elmore, M.D., P.I.).
Author information
Authors and Affiliations
Corresponding author
Additional information
Preliminary results of this research were presented at the annual meeting of the American Society of Preventive Oncology, San Francisco, CA, March 14, 2005; the International Society for Quality of Life Research Symposium, Boston, MA, June 27, 2004; and the annual meeting of the American Society of Clinical Oncology, New Orleans, LA, June 6, 2004.
Rights and permissions
About this article
Cite this article
Geiger, A.M., Nekhlyudov, L., Herrinton, L.J. et al. Quality of Life After Bilateral Prophylactic Mastectomy. Ann Surg Oncol 14, 686–694 (2007). https://doi.org/10.1245/s10434-006-9206-6
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1245/s10434-006-9206-6