Abstract
Objective
Because medical students experience a considerable amount of stress during training, academic leaders have recognized the importance of developing stress-management programs for medical students. The authors set out to identify all controlled trials of stress-management interventions and determine the efficacy of those interventions.
Methods
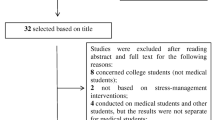
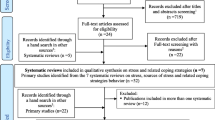
The authors searched the published English-language articles on PsycINFO and Pub Med, using a combination of the following search terms: stress-management, distress, burnout, coping, medical student, wellness. Both randomized, controlled trials and controlled, non-randomized trials of stress-management programs were selected and critically appraised.
Results
A total of 13 randomized, controlled trials or controlled, non-randomized trials were identified. Interventions included self-hypnosis, meditation, mindfulness-based stress-reduction, feedback on various health habits, educational discussion, changes in the length and type of curriculum, and changes in the grading system. Only one study was identified to be of very high quality, although several had described group differences at baseline, used blinding, had good follow-up, and used validated assessment tools. There was a wide heterogeneity of outcome measures used. Interventions that were supported by a reduction in stress and anxiety in medical students included mindfulness-based stress-reduction or meditation techniques, self-hypnosis, and pass/fail grading.
Conclusions
Significant opportunities to advance educational research in this field exist by developing more high-quality studies with particular attention to randomization techniques and standardizing outcome measures.
Similar content being viewed by others
References
Liaison Committee on Medical Education: Functions and Structure of a Medical School: Standards for Accreditation of Medical Education Programs Leading to the M.D. degree. May 2012; accessed 9/17/12 at http://www.lcme.org/functions.pdf
Dyrbye LN, Thomas MR, Shanafelt TD: Systematic review of depression, anxiety, and other indicators of psychological distress among U.S. and Canadian medical students. Acad Med 2006; 81:354–373
Compton MT, Carrera J, Frank E: Stress and depressive symptoms/dysphoria among U.S. medical students: results from alarge, nationally representative survey. J Nerv Ment Dis 2008; 196:891–897
Stewart SM, Lam TH, Betson CL, et al: Aprospective analysis of stress and academic performance in the first two years of medical school. Med Educ 1999; 33:243–250
Dyrbye LN, Massie FS Jr, Eacker A, et al: Relationship between burnout and professional conduct and attitudes among US medical students. JAMA 2010; 304:1173–1180
Thomas MR, Dyrbye LN, Huntington JL, et al: How do distress and well-being relate to medical student empathy? a multicenter study. J Gen Intern Med 2007; 22:177–183
Johnson NP, Michels PJ, Thomas JC: Screening tests identify the prevalence of alcohol use among freshman medical students and among students’ family of origin. JSC Med Assoc 1990; 86:13–14
Newbury-Birch D, Walshaw D, Kamali F: Drink and drugs: from medical students to doctors. Drug Alcohol Depend 2001; 64:265–270
Croen LG, Woesner M, Herman M, et al: A longitudinal study of substance use and abuse in a single class of medical students. Acad Med 1997; 72:376–381
Dyrbye LN, Thomas MR, Massie FS, et al: Burnout and suicidal ideation among U.S. medical students. Ann Intern Med 2008; 149:334–341
Chew-Graham CA, Rogers A, Yassin N: “I wouldn’t want it on my CV or their records:” medical students’ experiences of help-seeking for mental health problems. Med Educ 2003; 37:873–880
Harden RM, Grant J, Buckley G, et al: Best-evidence medical education. Adv Health Sci Educ Theory Pract 2000; 5:71–90
Hart IR, Harden RM: Best-evidence medical education (BEME): a plan for action. Med Teach 2000; 22:131–135
Holm M, Tyssen R, Stordal KI, et al: Self-development groups reduce medical school stress: a controlled intervention study. BMC Med Educ 2010; 10:23
Simard AA, Henry M: Impact of a short yoga intervention on medical students’ health: a pilot study. Med Teach 2009; 31:950–952
Hassed C, de Lisle S, Sullivan G, et al: Enhancing the health of medical students: outcomes of an integrated mindfulness and lifestyle program. Adv Health Sci Educ Theory Pract 2009; 14:387–398
Shapiro SL, Schwartz GE, Bonner G: Effects of mindfulness-based stress reduction on medical and premedical students. J Behav Med 1998; 21:581–599
Rosenzweig S, Reibel DK, Greeson JM, et al: Mindfulness-based stress reduction lowers psychological distress in medical students. Teach Learn Med 2003; 15:88–92
Finkelstein C, Brownstein A, Scott C, et al: Anxiety and stress reduction in medical education: an intervention. Med Educ 2007; 41:258–264
Warnecke E, Quinn S, Ogden K, et al: A randomised controlled trial of the effects of mindfulness practice on medical student stress levels. Med Educ 2011; 45:381–388
Whitehouse WG, Dinges DF, Orne EC, et al: Psychosocial and immune effects of self-hypnosis training for stress management throughout the first semester of medical school. Psychosom Med 1996; 58:249–263
Redwood SK, Pollak MH: Student-led stress management program for first-year medical students. Teach Learn Med 2007; 19:42–46
Adamson B, Covic T, Lincoln M: Teaching Time and Organizational Management Skills to First-Year Health Science Students: Does Training Make a Difference? Journal of Further and Higher Education 2004; 28:261–276
Das Gupta S, Charon R: Personal illness narratives: using reflective writing to teach empathy. Acad Med 2004; 79:351–356
Austenfeld JL, Paolo AM, Stanton AL: Effects of writing about emotions versus goals on psychological and physical health among third-year medical students. J Pers 2006; 74:267–286
Guthrie EA, Black D, Shaw CM, et al: Psychological stress in medical students: a comparison of two very different university courses. Stress Med 1997; 13:179–184
Kiessling C, Schubert B, Scheffner D, et al: First-year medical students’ perceptions of stress and support: a comparison between reformed and traditional track curricula. Med Educ 2004; 38:504–509
Dare AJ, Petrie KJ, Bagg W: Prepared for practice? medical students’ perceptions of a shortened final year medical programme. N Z Med J 2009; 122:32–43
Bloodgood RA, Short JG, Jackson JM, et al: A change to pass/fail grading in the first two years at one medical school results in improved psychological well-being. Acad Med 2009; 84:655–662
Reed DA, Shanafelt TD, Satele DW, et al: Relationship of pass/fail grading and curriculum structure with well-being among preclinical medical students: a multi-institutional study. Acad Med 2011; 86:1367–1373
Rohe DE, Barrier PA, Clark MM, et al: The benefits of pass-fail grading on stress, mood, and group cohesion in medical students. Mayo Clin Proc 2006; 81:1443–1448
Ball S, Bax A: Self-care in medical education: effectiveness of health-habits interventions for first-year medical students. Acad Med 2002; 77:911–917
Shapiro SL, Shapiro DE, Schwartz GE: Stress management in medical education: a review of the literature. Acad Med 2000; 75:748–759
Hammick M, Dornan T, Steinert Y: Conducting a best-evidence systematic review, part 1: from idea to data coding. BEME Guide No. 13. Med Teach 2010; 32:3–15
Guyatt GH, Sackett DL, Cook DJ: Users’ Guides to the Medical Literature, II: how to use an article about therapy or prevention, B: what were the results and will they help me in caring for my patients? Evidence-Based Medicine Working Group. JAMA 1994; 271:59–63
Prideaux D: Researching the outcomes of educational interventions: a matter of design: RTCs have important limitations in evaluating educational interventions. BMJ 2002; 324:126–127
Vitaliano PP, Maiuro RD, Mitchell E, et al: Perceived stress in medical school: resistors, persistors, adaptors, and maladaptors. Soc Sci Med 1989; 28:1321–1329
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Shiralkar, M.T., Harris, T.B., Eddins-Folensbee, F.F. et al. A Systematic Review of Stress-Management Programs for Medical Students. Acad Psychiatry 37, 158–164 (2013). https://doi.org/10.1176/appi.ap.12010003
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1176/appi.ap.12010003