Abstract
BACKGROUND: Medical students are rarely taught how to integrate communication and clinical reasoning. Not understanding the relation between these skills may lead students to undervalue the connection between psychosocial and biomedical aspects of patient care.
OBJECTIVE: To improve medical students’ communication and clinical reasoning and their appreciation of how these skills interrelate in medical practice.
DESIGN: In 2003, we conducted a randomized trial of a curricular intervention at Johns Hopkins University School of Medicine. In a 6-week course, participants learned communication and clinical reasoning skills in an integrative fashion using small group exercises with role-play, reflection and feedback through a structured iterative reflective process.
PARTICIPANTS: Second-year medical students.
MEASUREMENTS: All students interviewed standardized patients who evaluated their communication skills in establishing rapport, data gathering and patient education/counseling on a 5-point scale (1=poor; 5=excellent). We assessed clinical reasoning through the number of correct problems listed and differential diagnoses generated and the Diagnostic Thinking Inventory. Students rated the importance of learning these skills in an integrated fashion.
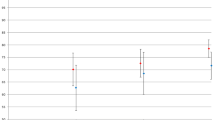
RESULTS: Standardized patients rated curricular students more favorably in establishing rapport (4.1 vs 3.9; P=.05). Curricular participants listed more psychosocial history items on their problem lists (65% of curricular students listing ≥1 item vs 44% of controls; P=.008). Groups did not differ significantly in other communication or clinical reasoning measures. Ninety-five percent of participants rated the integration of these skills as important.
CONCLUSIONS: Intervention students performed better in certain communication and clinical reasoning skills. These students recognized the importance of biomedical and psychosocial issues in patient care. Educators may wish to teach the integration of these skills early in medical training.
Similar content being viewed by others
References
Association of American Medical Colleges (AAMC). Learning objectives for medical student education—guidelines for medical schools: report I of the medical school objectives project. January 1998; Available from: http://www.aamc.org/meded/msop/. Accessed March 28, 2003.
Liaison Committee on Medical Education (LCME). Functions and structures of a medical school: standards for accreditation of medical education programs leading to the M.D. degree. July 2003; Available from: http://www.lcme.org/. Accessed July 16, 2003.
Accreditation Council for Graduate Medical Education (ACGME). Outcome project: enhancing residency education through outcomes assessment. Available from: http//www.acgme.org/Outcome/. Accessed March 28, 2003.
Evans RJ, Stanley RO, Mestrovic R, Rose L. Effects of communication skills training on students’ diagnostic efficiency. Med Educ. 1991;25:517–26.
Roter D, Hall JA, Kern DE, Barker LR, Cole KA, Roca RP. Improving physicians’ interviewing skills and reducing patients’ emotional distress: a randomized clinical trial. Arch Intern Med. 1995;155:1877–84.
Kempainen RR, Migeon MB, Wolf FM. Understanding our mistakes: a primer on errors in clinical reasoning. Med Teach. 2003;25:177–81.
Little P, Everitt H, Williamson I, et al. Observational study of effect of patient centredness and positive approach on outcomes of general practice consultations. BMJ. 2001;323:908–11.
Roter DL, Hall JA, Katz NR. Relations between physicians’ behaviors and analogue patients’ satisfaction, recall, and impressions. Med Care. 1987;25:437–51.
Mead N, Bower P. Patient-centred consultations and outcomes in primary care: a review of the literature. Patient Educ Couns. 2002;48:51–61.
Marvel MK, Epstein RM, Flowers K, Beckman HB. Soliciting patient’s agenda: have we improved? JAMA. 1999;281:283–7.
Levinson W, Roter D. Physicians’ psychosocial beliefs correlate with their patient communication skills. J Gen Intern Med. 1995;10:375–9.
Kern DE, Thomas PA, Howard DM, Bass EB. Curriculum Development for Medical Education: A Six-Step Approach. Baltimore, MD: The Johns Hopkins University Press; 1998.
Windish DM, Paulman PM, Goroll AH, Bass EB. Do clerkship directors think medical students are prepared for the clerkship years? Acad Med. 2004;79:56–61.
Bird J, Cohen-Cole SA. The three function model of the medical interview. Adv Psychosom Med. 1990;20:65–88.
Keller V, Carroll J. A new model for physician-patient communication. Patient Educ Couns. 1994;23:131–40.
Kurtz S, Silverman J. The Calgary-Cambridge Referenced Observation Guides: an aid to defining the curriculum and organizing the teaching in communication training programs. Med Educ. 1996;30:83–9.
Makoul G. The SEGUE Framework for teaching and assessing communication skills. Patient Educ Couns. 2001;23–34.
Stewart M, Brown JB, Weston WW, McWhinney IR, McWilliam CL, Freeman TR. Patient-Centered Medicine: Transforming the Clinical Method (Patient-Centered Case Series). Thousand Oaks, CA: Sage; 1995.
Novack DH, Dube C, Goldstein MG. Teaching medical interviewing: a basic course on interviewing and the physician-patient relationship. Arch Intern Med. 1992;152:1814–20.
Thomas RE. Teaching medicine with cases: student and teacher opinion. Med Educ. 1992;26:200–7.
Rogers JC, Swee DE, Ullian JA. Teaching medical decision making and students’ clinical problem solving skills. Med Teach. 1991;13:157–63.
Menahem S, Paget N. Role play for the clinical tutor: towards problem-based learning. Med Teach. 1990;12:57–61.
Kurtz SM, Silverman JD, Draper J. Teaching and Learning Communication Skills in Medicine. Oxford: Radcliffe Medical Press; 1998.
Bordage G, Grant J, Marsden P. Quantitative assessment of diagnostic ability. Med Educ. 1990;24:413–25.
Schmidt H. Integrating the teaching of basic sciences, clinical sciences, and biopsychosocial issues. Acad Med. 1998;73(suppl):S24–31.
Author information
Authors and Affiliations
Corresponding author
Additional information
The authors have no conflicts of interest to declare for this article or this research.
The authors received an unrestricted educational grant through the Program for Outpatient Education in Medicine of the Division of General Internal Medicine at the Johns Hopkins University School of Medicine that helped support the curricular evaluation. At the time of curricular inception, Dr. Windish was a research fellow on an Institution Research Service Award training grant supported by the Health Resources and Services Administration, Grant #2-32-HP 10025. Dr. Price was a research fellow on a training grant supported by the National Institutes of Health in Behavioral Research in Heart and Vascular Disease, Grant #HL007180. The authors are indebted to Dr. Eric Bass for his suggestions and Dr. Georges Bordage for allowing us to use the Diagnostic Thinking Inventory.
Rights and permissions
About this article
Cite this article
Windish, D.M., Price, E.G., Clever, S.L. et al. Teaching medical students the important connection between communication and clinical reasoning. J GEN INTERN MED 20, 1108–1113 (2005). https://doi.org/10.1111/j.1525-1497.2005.0244.x
Received:
Revised:
Accepted:
Issue Date:
DOI: https://doi.org/10.1111/j.1525-1497.2005.0244.x