Abstract
OBJECTIVE: We studied physician-patient dyads to determine how physician self-rated Spanish-language ability and cultural competence affect Spanish-speaking patients’ reports of interpersonal processes of care.
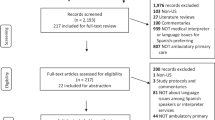
SETTING/PARTICIPANTS: Questionnaire study of 116 Spanish-speaking patients with diabetes and 48 primary care physicians (PCPs) at a public hospital with interpreter services.
MEASURES: Primary care physicians rated their Spanish ability on a 5-point scale and cultural competence by rating: 1) their understanding of the health-related cultural beliefs of their Spanish-speaking patients; and 2) their effectiveness with Latino patients, each on a 4-point scale. We assessed patients’ experiences using the interpersonal processes of care (IPC) in diverse populations instrument. Primary care physician responses were dichotomized, as were IPC scale scores (optimal vs nonoptimal). We analyzed the relationship between language and two cultural competence items and IPC, and a summary scale and IPC, using multivariate models to adjust for known confounders of communication.
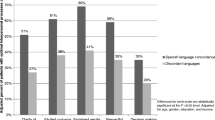
RESULTS: Greater language fluency was strongly associated with optimal IPC scores in the domain of elicitation of and responsiveness to patients, problems and concerns [Adjusted Odds Ratio [AOR], 5.25; 95% confidence interval [CI], 1.59 to 17.27]. Higher score on a language-culture summary scale was associated with three IPC domains — elicitation/responsiveness (AOR, 6.34; 95% CI, 2.1 to 19.3), explanation of condition (AOR, 2.7; 95% CI, 1.0 to 7.34), and patient empowerment (AOR, 3.13; 95% CI, 1.2 to 8.19)—and not associated with two more-technical communication domains.
CONCLUSION: Physician self-rated language ability and cultural competence are independently associated with patients’ reports of interpersonal process of care in patient-centered domains. Our study provides empiric support for the importance of language and cultural competence in the primary care of Spanish-speaking patients.
Similar content being viewed by others
References
Collins KS, Hughes HD, Doty MM, Ives BL, Edwards JN, Tenney K. Diverse Communities Common Concerns: Assessing Health Care Quality for Minority Americans. New York, NY: The Commonwealth Fund; 2002.
Nelson A. Unequal treatment: confronting racial and ethnic disparities in health care. J Natl Med Assoc. 2002;94:666–8.
Fiscella K, Franks P, Doescher MP, Saver BG. Disparities in health care by race, ethnicity, and language among the insured: findings from a national sample. Med Care. 2002;40:52–9.
Morales LS, Cunningham WE, Brown JA, Liu H, Hays RD. Are Latinos less satisfied with communication by health care providers? J Gen Intern Med. 1999;14:409–17.
Carrasquillo O, Orav EJ, Brennan TA, Burstin HR. Impact of language barriers on patient satisfaction in an emergency department. J Gen Intern Med. 1999;14:82–7.
Baker DW, Parker RM, Williams MV, Coates WC, Pitkin K. Use and effectiveness of interpreters in an emergency department. JAMA 1996;275:783–8.
Baker DW, Hayes R, Fortier JP. Interpreter use and satisfaction with interpersonal aspects of care for Spanish-speaking patients. Med Care. 1998;36:1461–70.
Perez-Stable EJ, Napoles-Springer A, Miramontes JM. The effects of ethnicity and language on medical outcomes of patients with hypertension or diabetes. Med Care. 1997;35:1212–9.
Todd KH, Samaroo N, Hoffman JR. Ethnicity as a risk factor for inadequate emergency department analgesia. JAMA. 1993;269:1537–9.
Carrillo JE, Green AR, Betancourt JR. Cross-cultural primary care: a patient-based approach. Ann Intern Med. 1999;130:829–34.
Bigby J, ed. Cross-Cultural Medicine. Philadelphia, PA: American College of Physicians; 2003.
Betancourt JR, Green AR, Carrillo JE. Cultural competence in health care: emerging frameworks and practical approaches. New York, NY: The Commonwealth Fund; 2002.
Brach C, Fraser I. Can cultural competency reduce racial and ethnic health disparities? A review and conceptual model. Med Care Res Rev. 2000;57(suppl 1):181–217.
Stewart AL, Napoles-Springer A, Perez-Stable EJ. Interpersonal processes of care in diverse populations. Milbank Q. 1999;77:305–39.
Lipsitz S, Laird NM, Harrington D. Generalized estimating equations for correlated binary data: using the odds ratio as a measure of association. Biometrika. 1991;78:153–60.
Roter DL, Hall JA, Aoki Y. Physician gender effects in medical communication: a meta-analytic review. JAMA. 2002;288:756–64.
Rivadeneyra R, Eldlerkin-Thompson V, Silver RC, Waitzkin H. Patient centeredness in medical encounters requiring an interpreter. Am J Med. 2000;108:470–4.
Lee LJ, Batal HA, Maselli JH, Kutner JS. Effect of Spanish interpretation method on patient satisfaction in an urban walkin clinic. J Gen Intern Med. 2002;17:641–5.
Cooper LA, Hill MN, Powe NR. Designing and evaluating interventions to eliminate racial and ethnic disparities in health care. J Gen Intern Med. 2002;17:477–86.
Crossing the Quality Chasm: A New Health System for the 21st Century. Washington, DC: Institute of Medicine; 2001.
Kaplan SH, Greenfield S, Ware Jr. JE. Assessing the effects of physician-patient interactions on the outcomes of chronic disease. Med Care. 1989;27(suppl 3):S110–127.
Author information
Authors and Affiliations
Corresponding author
Additional information
Dr Fernandez was funded in part by the UCSF/Hellman Early Family Career Award and by the UCSF Excellence Centers to Eliminate Ethnic/Racial Disparities. This project was funded in part by grant P30AG15272 under the Resource Centers for Minority Aging Research program, by the National Institute on Aging, the National Institute of Nursing Research, and The National Center on Minority Health and Health Disparities, National Institutes of Health.
Rights and permissions
About this article
Cite this article
Fernandez, A., Schillinger, D., Grumbach, K. et al. Physician language ability and cultural competence. J GEN INTERN MED 19, 167–174 (2004). https://doi.org/10.1111/j.1525-1497.2004.30266.x
Issue Date:
DOI: https://doi.org/10.1111/j.1525-1497.2004.30266.x