-
PDF
- Split View
-
Views
-
Cite
Cite
Robert van Deursen, Mechanical Loading and Off-Loading of the Plantar Surface of the Diabetic Foot, Clinical Infectious Diseases, Volume 39, Issue Supplement_2, August 2004, Pages S87–S91, https://doi.org/10.1086/383268
Close - Share Icon Share
Abstract
During weight-bearing activities, the feet are exposed to large forces, particularly when the activity is dynamic, such as walking. The pressure under the plantar surface during walking varies per foot area because of a number of factors related to the normal rollover during the stance phase of gait. Diabetes mellitus often results in loss of protective sensation and in structural changes that make the feet more susceptible to injury. Increased plantar pressure is an important factor in the development and maintenance of diabetic foot ulceration. Increased plantar pressures and associated ulcers need to be treated by off-loading of the plantar surface. Useful off-loading mechanisms include reduction of walking speed, alteration of foot rollover during gait, and transfer of load from affected areas to other areas of the foot or the lower leg. These plantar off-loading mechanisms could result in an optimization of treatment, but clinical effectiveness must be demonstrated.
Plantar ulceration is a common complication of diabetic neuropathy. Given the fact that plantar ulceration often initiates a process of further ulceration and ultimately amputation [1], it is crucial to prevent any such complications from the very beginning. Internal factors, such as loss of protective sensation, substantially contribute to the risk of ulceration [2]. On the other hand, mechanical loading of the feet as an external factor plays an equally important role in this process.
Here, I discuss the different aspects of mechanical loading of the foot and the ways of reducing mechanical load in biomechanical terms: first, the biomechanics of the normal foot during basic activities of daily living and the magnitude of the mechanical load the feet have to endure; second, the changes in the diabetic foot that lead to an increase of mechanical loading, compared with the normal foot; and third, the various interventions used to prevent and treat plantar ulceration in terms of their biomechanical mechanisms.
Mechanical Loading of The Foot
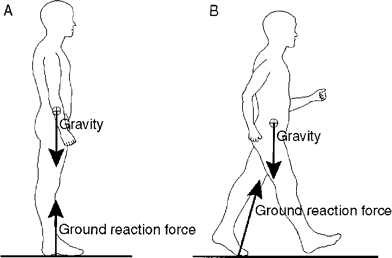
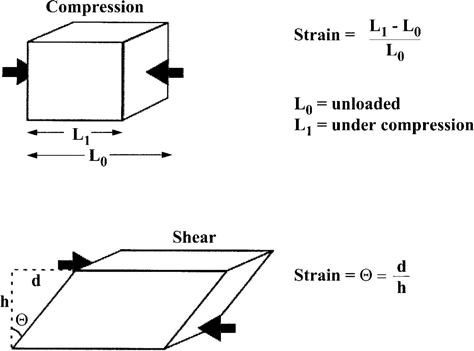
During weight-bearing activities, such as standing and walking, the plantar surface of the foot is exposed to ground reaction forces (GRFs; see figure 1). Such forces lead to tissue deformation. The relationship between force and deformation is expressed as the stress-strain relation. Stress is equal to normalized force (force per unit area to which the force is applied), otherwise known as pressure. Strain is equal to normalized deformation (percentage change from the original tissue dimensions; see figure 2). A stress perpendicular to the tissue surface will lead to a compressive strain. A stress parallel to the tissue surface (shear stress) will lead to a shear strain, depending on the presence of friction. Without sufficient friction, the surfaces slide over each other. The amount of strain in response to a particular stress depends on the characteristics of the tissue, expressed by a stress-strain curve.
Ground reaction forces (GRFs) to which the foot is exposed during standing (A) and walking (B). During quiet standing (A), gravity pulls at the body center of mass, which is opposed by the GRF of similar magnitude acting at the feet. During walking (B), the GRF acting at the feet not only opposes the pull of gravity at the body center of mass but also provides for progression of gait. The magnitude and direction of the force will be different than it is when standing still.
Calculation of strain (normalized deformation): the percentage change from the original tissue dimensions. For compression (top), this is the change in thickness; for shear strain (bottom), this is the angular change.
When a person is standing, the magnitude of the GRF is equal to body weight. Each foot experiences ∼50% of body weight distributed over the whole plantar weight-bearing surface. This is predominantly a vertically directed force, with negligible forces in the horizontal (shear) directions. As a result, moderate peak plantar pressures occur, with higher pressures at the heel than at the forefoot [3]. Although moderate, these pressures are sufficient to occlude capillary blood flow [4]. Quiet standing involves a certain amount of body sway [5], so there are variations in the amount of pressure that each part of the foot will experience, but this effect may be too small to be beneficial for capillary blood flow.
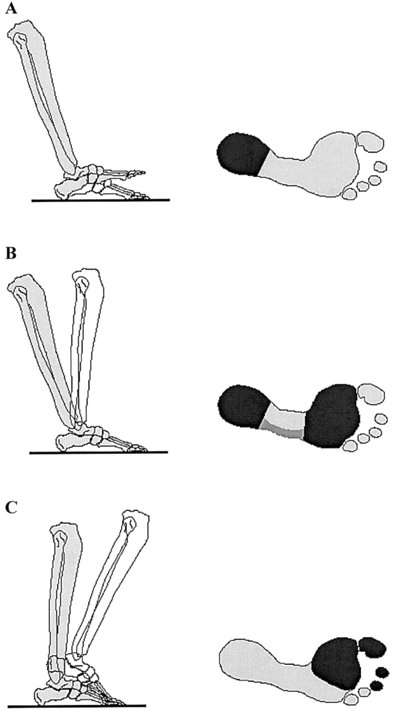
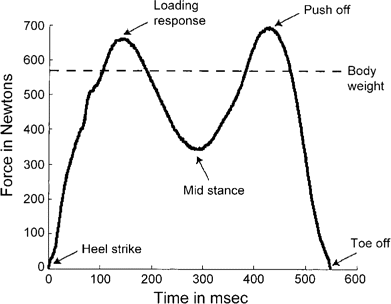
When a person is walking, the stresses applied to the feet are much higher than when standing, for a number of reasons. First, weight is borne on one foot for a substantial amount of time, because both feet are in contact with the floor for only 22% of the gait cycle [6]. Second, the stance phase of gait is characterized by a rollover of the foot [7]. Normally, the foot first rotates around the heel (heel rocker), followed by the ankle joint (ankle rocker) and the metatarsal heads and hallux (forefoot rocker; see figure 3). Different parts of the foot make contact with the floor during the different phases of stance. As a result, the plantar support surface changes in size and location while the GRFs progress anteriorly from heel to hallux. The heel is in contact with the floor during the first ∼64% of the stance phase. The forefoot and toes are in contact with the floor for the last 59% of the stance phase. Therefore, the period that both the heel and the forefoot are in contact with the floor (foot flat) occurs only during the middle 23% of the stance phase [6]. Third, the GRFs vary in magnitude. The vertical force component is characterized by a double-hump curve (see figure 4); the first peak is related to landing on the heel, and the second peak is related to pushing off with the forefoot at the end of stance. At a self-selected walking speed, these vertical peaks are ∼1.2 times body weight, but this increases with fast walking to 1.5 times body weight [8]. The heel and the forefoot therefore experience much higher peak pressures than the midfoot. The highest peak pressures normally occur over the medial metatarsophalangeal region and over the great toe.
Rollover of the foot during gait and changes in the size and location of the plantar contact surface. The foot first rotates around the heel (heel rocker; A), then the ankle (ankle rocker; B), and then the metatarsal heads and toes (forefoot rocker; C). The plantar contact surface is shown at right (dark).
The vertical force component of the ground reaction forces during gait, characterized by a double-hump shape. The first peak occurs during heel strike, followed by the loading response, and the second peak occurs during push-off. The trough in between occurs during midstance.
Besides the double-hump pattern of the vertical force, there are also horizontal (shear) forces at work during gait. The magnitude of the anteriorly or posteriorly directed force can be ∼25% of body weight. This shear force is directed posteriorly at the heel and anteriorly at the forefoot. It appears that these shear stresses are also distributed unequally over the support surface, so that localized peaks occur [9].
Adult walking at a self-selected speed occurs at ∼1.4 m/s and at a cadence of 113 steps/min [7]. The foot is therefore exposed very frequently to the stresses described for a single step. There is limited information about the number of steps taken on a daily or yearly basis. In a small sample of 6 healthy subjects and 6 subjects with diabetes, measured over 1 week, the average numbers of steps per day with the right leg were 5202 and 4395, respectively [10]. About 5000 steps per day would be >2 million steps per year. The mechanical loading of the feet is therefore substantial.
Mechanical Loading of The Diabetic Foot
In diabetes, several factors can affect the stresses applied to the feet. Loss of protective sensation can be dramatic [11], with the effect that patients cannot feel pain or discomfort when the plantar surface is injured or overloaded. Ulcers and lesions can remain undetected for some time, providing opportunities for an initial injury to become worse. Additional problems of diabetic vascular pathology and dryness of the skin make the plantar surface even more vulnerable to the imposed stresses and strains.
Because overweight affects the magnitude of the GRFs during gait and standing, an increase in mechanical loading of the foot can be expected. Increased plantar pressures in obese adults have been reported, in particular on the forefoot, but increased areas of contact between foot and ground have also been reported [12, 13]. Apparently the feet become wider in the presence of obesity. These changes in plantar support area might explain why peak plantar pressure and body mass were only mildly related to each other in patients with diabetes [14, 15].
Generalized limitations in joint mobility have been demonstrated in diabetes [16, 17]. Reduced mobility at the ankle and first metatarsophalangeal joints interferes with normal rollover of the foot during gait [18]. This can lead to higher plantar pressures [19] and a higher risk of ulceration [20]. Limited dorsiflexion of the ankle results in an earlier heel rise in the gait cycle and an earlier loading of the forefoot. Limited dorsiflexion of the great toe results in an earlier loading of this toe during the push-off phase. Structural foot changes related to motor neuropathy include intrinsic muscle wasting, associated with narrowing of the foot, and hammer and claw toes. Other deformities, such as hallux valgus, lesser toe joint dislocations, and alterations in arch height, also seem to be more prevalent in diabetes [21]. Such changes contribute to an increase in plantar pressure by reducing the support surface or by increasing the prominence of bony points (metatarsal heads and bunions). Midfoot (Charcot) fractures and partial foot amputations have similar effects and therefore result in higher plantar pressures [22, 23].
The plantar soft tissues were found to be stiffer and thinner in elderly subjects with diabetes than in healthy young subjects [24, 25]. The increase in stiffness seems particularly to occur in the soft tissue under the first metatarsal head. The reduced shock absorption characteristics of these tissues results in increased peak pressures under dynamic conditions, such as the heel strike and push-off phases of gait. Decreased plantar tissue thickness has been shown to relate to increased peak plantar pressure [26]. The buildup of callus under the forefoot has also been associated with increased plantar pressures and increased risk of ulceration [27].
Balance in standing and walking are affected by diabetic neuropathy. During quiet standing, patients with diabetic neuropathy demonstrate substantially increased body sway [28]. During walking, a “conservative” gait pattern seems to be adopted, with slower walking speed and cadence and with increased double support time [29, 30].
Mechanical Off-Loading of The Diabetic Foot
Mechanical loading of the diabetic foot is clearly part of the etiology of foot ulceration and is subsequently a major factor in delaying wound healing. Therefore, off-loading the affected plantar areas is an important component of prevention and treatment. A number of off-loading mechanisms are available, but not all of them are evidently practical. Complete bed rest and confinement to a wheelchair would work in specific cases but will be too restrictive for most patients. In the case of obesity, reduction of body weight would be appropriate, but since this takes time, it can only realistically be used for prevention and not to treat ulcers in the acute stage. The effects of walking aids to reduce the GRFs applied to the feet have not been thoroughly researched. It is conceivable that there would be an effect, but walking with a cane does not seem to reduce plantar pressures [31]. Patients might benefit from crutches but would need sufficient upper-body strength to manage them and would have to put up with the inconvenience that these walking aids impose. A change in walking style as a therapeutic intervention has been proposed. It has been demonstrated that plantar pressures, in particular in the forefoot, are considerably reduced during a shuffling gait [32] or a “step-to” gait [31], but this requires tremendous discipline from the patient. Winter and Seiko [33] have shown that normally the ankle push-off can generate up to 80% of the power required for walking. “Therapeutic walking” has the effect of limiting ankle push-off, dramatically reducing walking speed to ∼0.5 m/s. At this walking speed, the double-hump pattern of the vertical GRF (figure 4) will be much flatter and the vertical peaks will be equal to body weight, rather than higher [8]. Rosenbaum et al. [34] demonstrated that when walking speed is reduced from an average of 1.19 m/s (normal) to 0.83 m/s (slow), peak plantar pressures are reduced at the heel (5%–18%), at the medial forefoot (9%–11%), and at the hallux (11%).
A reduction in the number of steps taken per day will be beneficial, depending on the ulceration mechanism. For example, high plantar pressure related to a foot deformity or an object in the shoe is thought not to need many steps to produce a lesion; in other cases, a threshold for overloading in terms of steps per day may exist, warranting restrictions on the daily distance walked. However, more research on this issue is required.
Alteration of walking speed may be doubtful as a reliable voluntary intervention, but it may be a welcome “side-effect” of footwear used for treatment of plantar ulcers. Besides slowing down gait, resulting in reduced peak plantar pressures, footwear can be used in multiple ways for transferring load from plantar areas at risk of ulceration to other areas. Load transfer means that the total amount of loading by the GRF is not reduced but is distributed differently than it would be normally. Useful mechanisms include alteration of foot rollover during gait, transfer of forefoot load to midfoot and/or heel, transfer of plantar load to the normally non–weight-bearing parts of the foot, and transfer of plantar load to the lower leg.
A rigid rocker sole limits dorsiflexion of the hallux and toes and, therefore, the involvement of the forefoot rocker mechanism. In one study, plantar peak pressures in the medial forefoot and hallux were reduced by ∼30% with the use of rocker-bottom shoes [35]. This reduction was independent of the effect of walking speed, which was kept constant in this study. However, the average walking speed was 0.83 m/s, which has a general reducing effect on plantar pressures.
Insoles can influence plantar pressures on the basis of their material properties and their design. Pliable materials will help to reduce instantaneous peak pressures under dynamic conditions and can be expected to make increased contact with the foot (increasing the support surface) compared with hard materials. However, under static conditions, these effects may be limited as soon as the material is fully compressed. Custom-molded insoles can further help transfer load. The medial arch (provided it exists) and the area around the heel are normally non–weight-bearing areas of the foot. With a molded support surface, these areas can be involved in weight bearing. This effect is rather small with custom-molded insoles [36] but can be larger in molded-cast shoes [37].
Load transfer to the lower leg is achieved by making use of the conical shape of the leg. A close-fitting cast or brace can provide support, thereby reducing the plantar load. The total contact cast has been shown to achieve 31% load transfer to the cast wall [38]. With the total contact cast, forefoot loading was reduced to only 5% of that with control shoes that used the conventional total contact technique [38].
It is clear that different mechanisms are used to achieve the desired effect of off-loading the ulcerated area. An understanding of the underlying biomechanical principles by which plantar off-loading can be achieved should result in an optimization of available off-loading devices. However, equally important is that clinical effectiveness is demonstrated.





Comments