Abstract
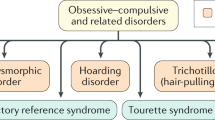
DSM-5 recognizes hoarding disorder as distinct from obsessive–compulsive disorder (OCD), codifying a new consensus. Hoarding disorder was previously classified as a symptom of OCD and patients received treatments designed for OCD. We conducted a meta-analysis to determine whether OCD patients with hoarding symptoms responded differently to traditional OCD treatments compared with OCD patients without hoarding symptoms. An electronic search was conducted for eligible studies in PubMed. A trial was eligible for inclusion if it (1) was a randomized controlled trial, cohort or case–control study; (2) compared treatment response between OCD patients with and those without hoarding symptoms, or examined response to treatment between OCD symptom dimensions (which typically include hoarding) and (3) examined treatment response to pharmacotherapy, behavioral therapy or their combination. Our primary outcome was differential treatment response between OCD patients with and those without hoarding symptoms, expressed as an odds ratio (OR). Twenty-one studies involving 3039 total participants including 304 with hoarding symptoms were included. Patients with OCD and hoarding symptoms were significantly less likely to respond to traditional OCD treatments than OCD patients without hoarding symptoms (OR=0.50 (95% confidence interval 0.42–0.60), z=−7.5, P<0.0001). This finding was consistent across treatment modalities. OCD patients with hoarding symptoms represent a population in need of further treatment research. OCD patients with hoarding symptoms may benefit more from interventions specifically targeting their hoarding symptoms.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout


Similar content being viewed by others
References
American Psychiatric Association. Diagnostic and Statistical Manual of Mental Disorders (Fifth edn). American Psychiatric Publishing: Arlington, VA, 2013.
Nordsletten AE, Reichenberg A, Hatch SL, de la Cruz LF, Pertusa A, Hotopf M et al. Epidemiology of hoarding disorder. Br J Psychiatry 2013; 203: 445–452.
Diagnostic and statistical manual of mental disorders: DSM-IV-TR. American Psychiatric Association: Washington DC, 2000.
Samuels JF, Bienvenu OJ, Grados MA, Cullen B, Riddle MA, Liang KY et al. Prevalence and correlates of hoarding behavior in a community-based sample. Behav Res Ther 2008; 46: 836–844.
Frost RO, Steketee G, Tolin DF . Comorbidity in hoarding disorder. Depression Anxiety 2011; 28: 876–884.
Pertusa A, Fullana MA, Singh S, Alonso P, Menchon JM, Mataix-Cols D . Compulsive hoarding: OCD symptom, distinct clinical syndrome, or both? Am J Psychiatry 2008; 165: 1289–1298.
Pertusa A, Frost RO, Fullana MA, Samuels J, Steketee G, Tolin D et al. Refining the diagnostic boundaries of compulsive hoarding: a critical review. Clin Psychol Rev 2010; 30: 371–386.
Frost RO, Hartl TL, Christian R, Williams N . The value of possessions in compulsive hoarding: patterns of use and attachment. Behav Res Ther 1995; 33: 897–902.
Mataix-Cols D, Frost RO, Pertusa A, Clark LA, Saxena S, Leckman JF et al. Hoarding disorder: a new diagnosis for DSM-V? Depression Anxiety 2010; 27: 556–572.
Saxena S . Neurobiology and treatment of compulsive hoarding. CNS Spectrums 2008; 13: 29–36.
Tolin DF, Kiehl KA, Worhunsky P, Book GA, Maltby N . An exploratory study of the neural mechanisms of decision making in compulsive hoarding. Psychol Med 2009; 39: 325–336.
Tolin DF, Stevens MC, Villavicencio AL, Norberg MM, Calhoun VD, Frost RO et al. Neural mechanisms of decision making in hoarding disorder. Arch Gen Psychiatry 2012; 69: 832–841.
Mataix-Cols D, Pertusa A . Snowdon J. Neuropsychological and neural correlates of hoarding: a practice-friendly review. J Clin Psychol 2011; 67: 467–476.
Lochner C, Kinnear CJ, Hemmings SM, Seller C, Niehaus DJ, Knowles JA et al. Hoarding in obsessive-compulsive disorder: clinical and genetic correlates. J Clin Psychiatry 2005; 66: 1155–1160.
Samuels J, Shugart YY, Grados MA, Willour VL, Bienvenu OJ, Greenberg BD et al. Significant linkage to compulsive hoarding on chromosome 14 in families with obsessive-compulsive disorder: results from the OCD Collaborative Genetics Study. Am J Psychiatry 2007; 164: 493–499.
Iervolino AC, Perroud N, Fullana MA, Guipponi M, Cherkas L, Collier DA et al. Prevalence and heritability of compulsive hoarding: a twin study. Am J Psychiatry 2009; 166: 1156–1161.
Sorrell JM . Understanding hoarding in older adults. J Psychosoc Nurs Ment Health Serv 2012; 50: 17–21.
Frost RO, Ruby D, Shuer LJ . The Buried in Treasures Workshop: waitlist control trial of facilitated support groups for hoarding. Behav Res Ther 2012; 50: 661–667.
Steketee G, Frost RO, Tolin DF, Rasmussen J, Brown TA . Waitlist-controlled trial of cognitive behavior therapy for hoarding disorder. Depression Anxiety 2010; 27: 476–484.
Bloch MH, Landeros-Weisenberger A, Rosario MC, Pittenger C, Leckman JF . Meta-analysis of the symptom structure of obsessive-compulsive disorder. Am J Psychiatry 2008; 165: 1532–1542.
Mataix-Cols D, Rauch SL, Manzo PA, Jenike MA, Baer L . Use of factor-analyzed symptom dimensions to predict outcome with serotonin reuptake inhibitors and placebo in the treatment of obsessive-compulsive disorder. Am j Psychiatry 1999; 156: 1409–1416.
Goodman WK, Price LH, Rasmussen SA, Mazure C, Delgado P, Heninger GR et al. The Yale-Brown Obsessive Compulsive Scale. II. Validity. Arch Gen Psychiatry 1989; 46: 1012–1016.
Goodman WK, Price LH, Rasmussen SA, Mazure C, Fleischmann RL, Hill CL et al. The Yale-Brown Obsessive Compulsive Scale. I. Development, use, and reliability. Arch Gen Psychiatry 1989; 46: 1006–1011.
Rosario-Campos MC, Miguel EC, Quatrano S, Chacon P, Ferrao Y, Findley D et al. The Dimensional Yale-Brown Obsessive-Compulsive Scale (DY-BOCS): an instrument for assessing obsessive-compulsive symptom dimensions. Mol Psychiatry 2006; 11: 495–504.
Egger M, Davey Smith G, Schneider M, Minder C . Bias in meta-analysis detected by a simple, graphical test. Br Med j 1997; 315: 629–634.
Masi G, Millepiedi S, Perugi G, Pfanner C, Berloffa S, Pari C et al. Pharmacotherapy in paediatric obsessive-compulsive disorder: a naturalistic, retrospective study. CNS Drugs 2009; 23: 241–252.
Ferrao YA, Shavitt RG, Bedin NR, de Mathis ME, Carlos Lopes A, Fontenelle LF et al. Clinical features associated to refractory obsessive-compulsive disorder. J Affective Dis 2006; 94: 199–209.
Stein DJ, Carey PD, Lochner C, Seedat S, Fineberg N, Andersen EW . Escitalopram in obsessive-compulsive disorder: response of symptom dimensions to pharmacotherapy. CNS Spectrums 2008; 13: 492–498.
Stein DJ, Andersen EW, Overo KF . Response of symptom dimensions in obsessive-compulsive disorder to treatment with citalopram or placebo. Rev Bras Psiquiatr 2007; 29: 303–307.
Matsunaga H, Maebayashi K, Hayashida K, Okino K, Matsui T, Iketani T et al. Symptom structure in Japanese patients with obsessive-compulsive disorder. Am J Psychiatry 2008; 165: 251–253.
Erzegovesi S, Cavallini MC, Cavedini P, Diaferia G, Locatelli M, Bellodi L . Clinical predictors of drug response in obsessive-compulsive disorder. J Clin Psychopharmacol 2001; 21: 488–492.
Landeros-Weisenberger A, Bloch MH, Kelmendi B, Wegner R, Nudel J, Dombrowski P et al. Dimensional predictors of response to SRI pharmacotherapy in obsessive-compulsive disorder. J Affective Dis 2010; 121: 175–179.
Storch EA, Merlo LJ, Larson MJ, Marien WE, Geffken GR, Jacob ML et al. Clinical features associated with treatment-resistant pediatric obsessive-compulsive disorder. Compr Psychiatry 2008; 49: 35–42.
Storch EA, Merlo LJ, Larson MJ, Bloss CS, Geffken GR, Jacob ML et al. Symptom dimensions and cognitive-behavioural therapy outcome for pediatric obsessive-compulsive disorder. Acta Psychiatr Scand 2008; 117: 67–75.
Shetti CN, Reddy YC, Kandavel T, Kashyap K, Singisetti S, Hiremath AS et al. Clinical predictors of drug nonresponse in obsessive-compulsive disorder. J Clin Psychiatry 2005; 66: 1517–1523.
Saxena S, Maidment KM, Vapnik T, Golden G, Rishwain T, Rosen RM et al. Obsessive-compulsive hoarding: symptom severity and response to multimodal treatment. J Clin Psychiatry 2002; 63: 21–27.
Salomoni G, Grassi M, Mosini P, Riva P, Cavedini P, Bellodi L . Artificial neural network model for the prediction of obsessive-compulsive disorder treatment response. J Clin Psychopharmacol 2009; 29: 343–349.
Rufer M, Fricke S, Moritz S, Kloss M, Hand I . Symptom dimensions in obsessive-compulsive disorder: prediction of cognitive-behavior therapy outcome. Acta Psychiatr Scand 2006; 113: 440–446.
Raffin AL, Guimaraes Fachel JM, Ferrao YA, Pasquoto de Souza F, Cordioli AV . Predictors of response to group cognitive-behavioral therapy in the treatment of obsessive-compulsive disorder. Eur Psychiatry 2009; 24: 297–306.
Olino TM, Gillo S, Rowe D, Palermo S, Nuhfer EC, Birmaher B et al. Evidence for successful implementation of exposure and response prevention in a naturalistic group format for pediatric OCD. Depression Anxiety 2011; 28: 342–348.
Meyer E, Shavitt RG, Leukefeld C, Heldt E, Souza FP, Knapp P et al. Adding motivational interviewing and thought mapping to cognitive-behavioral group therapy: results from a randomized clinical trial. Rev Bras Psiquiatr 2010; 32: 20–29.
Mataix-Cols D, Marks IM, Greist JH, Kobak KA, Baer L . Obsessive-compulsive symptom dimensions as predictors of compliance with and response to behaviour therapy: results from a controlled trial. Psychother Psychosom 2002; 71: 255–262.
Maher MJ, Huppert JD, Chen H, Duan N, Foa EB, Liebowitz MR et al. Moderators and predictors of response to cognitive-behavioral therapy augmentation of pharmacotherapy in obsessive-compulsive disorder. Psychol Medi 2010; 40: 2013–2023.
Black DW, Monahan P, Gable J, Blum N, Clancy G, Baker P . Hoarding and treatment response in 38 nondepressed subjects with obsessive-compulsive disorder. J Clin Psychiatry 1998; 59: 420–425.
Abramowitz JS, Franklin ME, Schwartz SA, Furr JM . Symptom presentation and outcome of cognitive-behavioral therapy for obsessive-compulsive disorder. J ConsultiClin Psychol 2003; 71: 1049–1057.
Storch EA, Lack CW, Merlo LJ, Geffken GR, Jacob ML, Murphy TK et al. Clinical features of children and adolescents with obsessive-compulsive disorder and hoarding symptoms. Compr Psychiatry 2007; 48: 313–318.
Timpano KR, Exner C, Glaesmer H, Rief W, Keshaviah A, Brahler E et al. The epidemiology of the proposed DSM-5 hoarding disorder: exploration of the acquisition specifier, associated features, and distress. J Clin Psychiatry 2011; 72: 780–786, quiz 878-789.
Torres AR, Fontenelle LF, Ferrao YA, do Rosario MC, Torresan RC, Miguel EC et al. Clinical features of obsessive-compulsive disorder with hoarding symptoms: a multicenter study. J Psychiatric Res 2012; 46: 724–732.
Iervolino AC, Rijsdijk FV, Cherkas L, Fullana MA, Mataix-Cols D . A multivariate twin study of obsessive-compulsive symptom dimensions. Arch Gen Psychiatry 2011; 68: 637–644.
Frost RO, Steketee G, Tolin DF . Diagnosis and assessment of hoarding disorder. Annu Rev Clin Psychol 2012; 8: 219–242.
Frost RO . Treatment of hoarding. Expert Rev Neurother 2010; 10: 251–261.
Saxena S . Pharmacotherapy of compulsive hoarding. J Clin Psychol 2011; 67: 477–484.
Ayers CR, Wetherell JL, Golshan S, Saxena S . Cognitive-behavioral therapy for geriatric compulsive hoarding. Behav Res Ther 2011; 49: 689–694.
Tolin DF, Frost RO, Steketee G . A brief interview for assessing compulsive hoarding: the Hoarding Rating Scale-Interview. Psychiatry Res 2010; 178: 147–152.
Frost RO, Hristova V, Steketee G, Tolin DF . Activities of Daily Living Scale in Hoarding Disorder. J Obsessive Compuls Relat Dis 2013; 2: 85–90.
Acknowledgements
We acknowledge the National Institute of Mental Health's support of the Yale Child Study Center Research Training Program (MHB), the National Institutes of Health (K23MH091240 (MHB), T32MH018268-26 (JFL), R25 MH077823 (JFL) and K08MH081190) (CP), the APIRE/Eli Lilly Psychiatric Research Fellowship (MHB), the AACAP/ Eli Lilly Junior Investigator Award (MHB), the Trichotillomania Learning Center (MHB), the Doris Duke Charitable Foundation (CP), NARSAD (MHB), the Rembrandt Foundation (MHB) and UL1 RR024139 from the National Center for Research Resources, a component of the National Institutes of Health, and NIH roadmap for Medical Research (MHB and CP).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no conflict of interest.
PowerPoint slides
Rights and permissions
About this article
Cite this article
Bloch, M., Bartley, C., Zipperer, L. et al. Meta-analysis: hoarding symptoms associated with poor treatment outcome in obsessive–compulsive disorder. Mol Psychiatry 19, 1025–1030 (2014). https://doi.org/10.1038/mp.2014.50
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/mp.2014.50
This article is cited by
-
Possible actions of cannabidiol in obsessive-compulsive disorder by targeting the WNT/β-catenin pathway
Molecular Psychiatry (2022)
-
The prefrontal cortex and OCD
Neuropsychopharmacology (2022)
-
Lithium: a potential therapeutic strategy in obsessive–compulsive disorder by targeting the canonical WNT/β pathway
Translational Psychiatry (2021)
-
An Overview of Anxiety, Trauma-Related and Obsessive-Compulsive Disorders
Current Geriatrics Reports (2021)