Abstract
Objective:
To determine whether the Bishop-score upon admission effects mode of delivery, maternal or neonatal outcomes of labor induction in multiparous women.
Study Design:
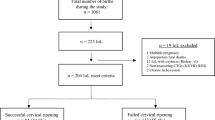
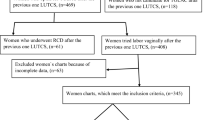
A retrospective study including 600 multiparous women with a singleton pregnancy, 34 gestational weeks and above who underwent labor induction for maternal, fetal or combined indications. Induction was performed with one of three methods— oxytocin, a slow release vaginal prostaglandin E2 insert (10 mg dinoprostone) or a transcervical double balloon catheter. The women were divided into two groups—Bishop-score <6 and Bishop-score ⩾6. We evaluated labor course, maternal complications (postpartum hemorrhage, manual lysis, uterine revision, perineal tear grade 3–4, need for blood transfusions, relaparotomy, prolonged hospitalization) and neonatal outcomes (Apgar score, cord pH, hospitalization in the neonatal intensive care unit, prolonged hospitalization).
Results:
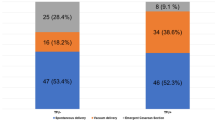
Both groups had a high rate of vaginal deliveries—93.7% and 94.9%, respectively. There was no difference between the two groups in terms of maternal or neonatal outcomes.
Conclusion:
Labor induction in multiparous women is safe and successful regardless of the initial Bishop-score. In multiparous women the Bishop-score is not a good predictor for the success of labor induction, nor is it a predictor for maternal of neonatal adverse outcomes and complications.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout
Similar content being viewed by others
References
ACOG Committee on Practice Bulletins-Obstetrics.. ACOG Practice Bulletin No. 107: induction of labor. Obstet Gynecol 2009; 114 (2, Part 1):386–397.
National Collaborating Centre for Women’s and Children’s HealthInduction of Labor—Clinical Guideline for NICE by NHS, July 2008.
Bishop EH . Pelvic scoring for elective induction. Obstet Gynecol 1964; 24: 266.
Seyb ST, Berka RJ, Socol ML, Dooley SL . Risk of cesarean delivery with elective induction of labor at term in nulliparous women. Obstet Gynecol 1999; 94 (4): 600–607.
Vrouenraets FPJM, Roumen FJME, Dehing CJG, Van Den Akker ESA, Aarts MJB, Scheve EJT . Bishop score and risk of cesarean delivery after induction of labor in nulliparous women. Obstet Gynecol 2005; 105 (4): 690–697.
Luthy DA, Malmgren JA, Zingheim RW . Cesarean delivery after elective induction in nulliparous women: the physician effect. Am J Obstet Gynecol 2004; 191 (5): 1511–1515.
Vahratian A, Zhang J, Troendle JF, Sciscione AC, Hoffman MK . Labor progression and risk of cesarean delivery in electively induced nulliparas. Obstet Gynecol 2005; 105 (4): 698–704.
Maslow AS, Sweeny AL . Elective induction of labor as a risk factor for cesarean delivery among low-risk women at term. Obstet Gynecol 2000; 95 (6, Part 1): 917–922.
Hoffman MK, Vahratian A, Sciscione AC, Troendle JF, Zhang J . Comparison of labor progression between induced and noninduced multiparous women. Obstet Gynecol 2006; 107 (5): 1029–1034.
Yeast JD, Jones A, Poskin M . Induction of labor and the relationship to cesarean delivery: a review of 7001 consecutive inductions. Am J Obstet Gynecol 1999; 180 (3): 628–633.
Macer JA, Macer CL, Chan LS . Elective induction versus spontaneous labor: a retrospective study of complications and outcome. Am J Obstet Gynecol 1992; 166: 1690–1697.
Dublin S, Lydon-Rochelle M, Kaplan RC, Watts D, Critchlow CW . Maternal and neonatal outcomes after induction of labor without an identified indication. Am J Obstet Gynecol 2000; 183 (4): 986–994.
Heinberg EM, Wood RA, Chambers RB . Elective induction of labor in multiparous women. Does it increase the risk of cesarean section? J Reprod Med 2002; 47: 399–403.
Declercq E, Barger M, Cabral HJ, Evans SR, Kotelchuck M, Simon C et al. Maternal outcomes associated with planned primary cesarean births compared with planned vaginal births. Obstet Gynecol 2007; 109 (3): 669–677.
Thorsell M, Lyrenäs S, Andolf E, Kaijser M . Induction of labor and the risk for emergency cesarean section in nulliparous and multiparous women. Acta Obstet Gynecol Scand 2011; 90 (10): 1094–1099.
Levine LD, Hirshberg A, Srinivas SK . Term induction of labor and risk of cesarean delivery by parity. J Matern-Fetal Neonat Med 2013; 27 (12):1232–1236.
Lee HR, Kim M-N, You JY, Choi S-J, Oh S-Y, Roh C-R et al. Risk of cesarean section after induced versus spontaneous labor at term gestation. Obstet Gynecol Sci 2015; 58 (5): 346.
Gaudet L, Wen SW, Walker M . The combined effect of maternal obesity and fetal macrosomia on pregnancy outcomes. J Obstet Gynaecol Can 2014; 36 (9): 776–784.
Ivars J, Garabedian C, Devos P, Therby D, Carlier S, Deruelle P et al. Simplified Bishop score including parity predicts successful induction of labor. Eur J Obstet Gynecol Reprod Biol 2016; 203: 309–314.
Lange AP, Secher NJ, Westergaard JG, Skovgård I . Prelabor evaluation of inducibility. Obstet Gynecol 1982; 60 (2): 137–147.
Laughon SK, Zhang J, Troendle J, Sun L, Reddy UM . Using a simplified Bishop score to predict vaginal delivery. Obstet Gynecol 2011; 117 (4): 805–811.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no conflict of interest.
Rights and permissions
About this article
Cite this article
Navve, D., Orenstein, N., Ribak, R. et al. Is the Bishop-score significant in predicting the success of labor induction in multiparous women?. J Perinatol 37, 480–483 (2017). https://doi.org/10.1038/jp.2016.260
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/jp.2016.260
This article is cited by
-
Prediction of successful trial of labor after cesarean among grand-multiparous women
Archives of Gynecology and Obstetrics (2022)
-
Prediction of mode of delivery by an ultrasound score similar to Bishop score and performance of independent predictors
Journal of Ultrasound (2022)