Abstract
Background:
Physical activity is essential for chronic disease prevention, yet <40% of overweight/obese adults meet the national activity recommendations. For time-efficient counseling, clinicians need a brief, easy-to-use tool that reliably and validly assesses a full range of activity levels, and, most importantly, is sensitive to clinically meaningful changes in activity. The Stanford Leisure-Time Activity Categorical Item (L-Cat) is a single item comprising six descriptive categories ranging from inactive to very active. This novel methodological approach assesses national activity recommendations as well as multiple clinically relevant categories below and above the recommendations, and incorporates critical methodological principles that enhance psychometrics (reliability, validity and sensitivity to change).
Methods:
We evaluated the L-Cat’s psychometrics among 267 overweight/obese women who were asked to meet the national activity recommendations in a randomized behavioral weight-loss trial.
Results:
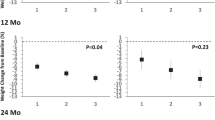
The L-Cat had excellent test–retest reliability (κ=0.64, P<0.001) and adequate concurrent criterion validity; each L-Cat category at 6 months was associated with 1059 more daily pedometer steps (95% CI 712–1407, β=0.38, P<0.001) and 1.9% greater initial weight loss at 6 months (95% CI −2.4 to −1.3, β=−0.38, P<0.001). Of interest, L-Cat categories differentiated from each other in a dose-response gradient for steps and weight loss (Ps<0.05) with excellent face validity. The L-Cat was sensitive to change in response to the trial’s activity component. Women increased one L-Cat category at 6 months (M=1.0±1.4, P<0.001); 55.8% met the recommendations at 6 months whereas 20.6% did at baseline (P<0.001). Even among women not meeting the recommendations at both baseline and 6 months (n=106), women who moved ⩾1 L-Cat categories at 6 months lost more weight than those who did not (M=−4.6%, 95% CI −6.7 to −2.5, P<0.001).
Conclusions:
Given strong psychometrics, the L-Cat has timely potential for clinical use such as tracking activity changes via electronic medical records, especially among overweight/obese populations who are unable or unlikely to reach national recommendations.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout

Similar content being viewed by others
References
Physical Activity Guidelines Advisory Committee. Physical Activity Guidelines Advisory Committee Report.. United States Department of Health and Human Services: Washington DC, 2008.
Haskell WL, Lee I, Pate RR, Powell KE, Blair SN, Franklin BA et al. Physical activity and public health: updated recommendation for adults from the American College of Sports Medicine and the American Heart Association. Med Sci Sports Exerc 2007; 39: 1423–1434.
Centers for Disease Control and Prevention. Prevalence of regular physical activity among adults - United States, 2001 and 2005. MMWR Morb Mortal Wkly Rep 2007; 56: 1209–1212.
Spees CK, Scott JM, Taylor CA . Differences in amounts and types of physical activity by obesity status in US adults. Am J Health Behav 2012; 36: 56–65.
Sallis R . Developing health care systems to support exercise: exercise as the fifth vital sign. Br J Sports Med 2011; 45: 473–474.
Sudman S, Bradburn NM . Asking Questions: A Practical Guide To Questionnaire Design. Jossey-Bass Publishers: San Francisco, 1983.
Burton S, Blair E . Task conditions, response formulation proceses, and response accuracy for behavioral frequency questions in surveys. Public Opinion Q 1991; 55: 50–79.
Ainsworth BE, Macera CA, Jones DA, Reis JP, Addy CL, Bowles HR et al. Comparison of the 2001 BRFSS and the IPAQ physical activity questionnaires. Med Sci Sports Exerc 2006; 38: 1584–1592.
van Poppel MNM, Chinapaw MJM, Mokkink LB, van Mechelen W, Terwee CB . Physical activity questionniares for adults: a systematic review of measurement properties. Sports Med 2010; 40: 565–600.
Pate RR, Pratt M, Blair SN, Haskell WL, Macera CA, Bouchard C et al. Physical activity and public health: a recommendation from the Centers for Disease Control and Prevention and the American College of Sports Medicine. JAMA 1995; 273: 402–407.
Stecker T, Sparks S . Prevalence of obese patients in a primary care setting. Obesity 2006; 14: 373–376.
Finkelstein EA, Trogdon JG, Cohen JW, Dietz W . Annual medical spending attributable to obesity: payer- and service-specific estimates. Health Affairs 2009; 28: w822–w831.
Kiernan M, Brown SD, Schoffman DE, Lee K, King AC, Taylor CB et al. Promoting healthy weight with 'Stability Skills First': a randomized trial. J Consult Clin Psychol 2012. e-pub ahead of print 29 October 2012.
Taylor-Piliae RE, Norton LC, Haskell WL, Mahbouda MH, Fair JM, Iribarren C et al. Validation of a new brief physical activity survey among men and women aged 60-69 years. Am J Epidemiol 2006; 164: 598–606.
Pate RR, O'Neill JR, Lobelo F . The evolving definition of 'sedentary'. Exerc Sport Sci Rev 2008; 36: 173–178.
Ainsworth BE, Haskell WL, Herrmann SD, Meckes N, Bassett DR Jr, Tudor-Locke C et al2011 Compendium of physical activities: a second update of codes and MET values. Med Sci Sports Exerc 2011; 43: 1575–1581.
Kozey SL, Lyden K, Howe CA, Staudenmayer JW, Freedson PS . Accelerometer output and MET values of common physical activities. Med Sci Sports Exerc 2010; 42: 1776–1784.
Matthews CE, Ainsworth BE, Thompson RW, Bassett DR Jr . Sources of variance in daily physical activity levels as measured by an accelerometer. Med Sci Sports Exerc 2002; 34: 1376–1381.
Trost SG, Mciver KL, Pate RR . Conducting accelerometer-based activity assessments in field-based research. Med Sci Sports Exerc 2005; 37: S531–S543.
Levin S, Jacobs DR Jr, Ainsworth BE, Richardson MT, Leon AS . Intra-individual variation and estimates of usual physical activity. Ann Epidemiol 1999; 9: 481–488.
Landis JR, Koch GG . The measurement of observer agreement for categorical data. Biometrics 1977; 33: 159–174.
Glasgow RE, Kaplan RM, Ockene JK, Fisher EB, Emmons KM . Patient-reported measures of psychosocial issues and health behavior should be added to electronic health records. Health Affairs 2012; 31: 497–504.
American College of Sports Medicine and American Medical Association. ACSM and AMA launch "Exercise is Medicine" program: Calls for physicians to prescribe exercise to patients. http://exerciseismedicine.org/images/PressReleaseNov07.pdf 2007.
Society for Behavioral Medicine and the National Institutes of Health. Identifying core behavioral and psychosocial data elements for the electronic health record: Executive Summary. http://www.sbm.org/UserFiles/file/EHR_Meeting_May_2-3-2011--Executive_Summary.pdf 2011.
Bacon L, Aphramor L . Weight science: evaluating the evidence for a paradigm shift. Nutr J 2011; 10: 9.
Acknowledgements
We gratefully thank the trial participants and research staff. We also thank the following for significant contributions to data analysis (Alex McMillan, PhD and Ann Varady MS, Stanford University School of Medicine), data interpretation (Matt Buman, PhD and Erik Hekler, PhD, Arizona State University, and Mary Rosenberger, PhD, Stanford University School of Medicine), and the L-Cat 2.2 version (Catherine Cubbin, PhD, University of Texas at Austin and Paul Estabrooks, PhD, VirginiaTech). The research was supported by Public Health Service Grant R01 CA112594 to Michaela Kiernan, PhD from the National Institutes of Health.
Disclaimer
The funding source did not participate in the design and conduct of the study; collection, management, analysis, and interpretation of the data; or preparation, review, or approval of the manuscript.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no conflicts of interest.
Rights and permissions
About this article
Cite this article
Kiernan, M., Schoffman, D., Lee, K. et al. The Stanford Leisure-Time Activity Categorical Item (L-Cat): a single categorical item sensitive to physical activity changes in overweight/obese women. Int J Obes 37, 1597–1602 (2013). https://doi.org/10.1038/ijo.2013.36
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/ijo.2013.36
Keywords
This article is cited by
-
Acute Effects of Ad Libitum Use of Commercially Available Cannabis Products on the Subjective Experience of Aerobic Exercise: A Crossover Study
Sports Medicine (2023)
-
Relative reinforcement from physical activity in real-world environments: a novel application of behavioral economics
Journal of Behavioral Medicine (2022)
-
Using a consumer-based wearable activity tracker for physical activity goal setting and measuring steps in pregnant women with gestational diabetes mellitus: exploring acceptance and validity
BMC Pregnancy and Childbirth (2021)
-
Weight stigma and health behaviors: evidence from the Eating in America Study
International Journal of Obesity (2021)
-
Effects of Aerobic Exercise Training on Daily Psychological Processes in Family Caregivers: Secondary Analyses of a Randomized Controlled Trial
Affective Science (2021)