Abstract
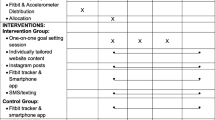
Scalable and convenient programs for family obesity prevention have proven difficult to design/implement. Mobile technology could be helpful tools to engage busy families. The Motivating Families with Interactive Technology (mFIT) study tested the feasibility, acceptability, and effectiveness of two remotely delivered family-based programs targeting physical activity (PA) and healthy eating (HE). Parent–child dyads were randomized to one of two 12-week mobile interventions delivered via weekly email newsletters; programs differed in focus of content (individual vs. family) and method of tracking (paper vs. mobile website). At baseline and 12 weeks, height and weight were objectively measured and participants completed questionnaires. Multivariable models were used to examine changes from baseline to 12 weeks by parent/child, group, and time; Cohen’s d was used to calculate effect sizes. Of the 33 randomized dyads (parents 43 ± 5.8 years, 87.9% female, 69.7% white, BMI 31.1 ± 8.3 kg/m2; children 11 ± 0.9 years, 63.6% female, 66.7% white, BMI 77.6 ± 27.8 percentile), 31 (94.0%) had follow-up data. Baseline means for all measures of parent–child communication and engagement were high. There were no group by time differences for PA or HE. However, combining groups and parents/children, there was a significant increase in average daily steps (1397 steps, p = 0.04, d = 0.4) and servings of fruit (0.3 servings, p = 0.02, d = 0.2), a marginally significant decrease in children’s daily servings of sugar-sweetened beverages (− 0.1 servings, p = 0.05, d = −0.1), and good adherence to self-monitoring protocols. The mFIT program showed excellent feasibility and acceptability as a low-cost, remotely delivered family intervention for PA and HE promotion.


Similar content being viewed by others
References
Bandura, A. (1989). Regulation of cognitive processes through perceived self-efficacy. Developmental Psychology, 25(5), 729–735. https://doi.org/10.1037/0012-1649.25.5.729.
Barlow, S. E., & the Expert Committee. (2007). Expert Committee recommendations regarding the prevention, assessment, and treatment of child and adolescent overweight and obesity: summary report. Pediatrics, 120(Supplement 4), S164–S192. https://doi.org/10.1542/peds.2007-2329C.
Boushey, C. J., Kerr, D. A., Wright, J., Lutes, K. D., Ebert, D. S., & Delp, E. J. (2009). Use of technology in children’s dietary assessment. European Journal of Clinical Nutrition, 63(Suppl 1), S50–S57. https://doi.org/10.1038/ejcn.2008.65.
Broderick, C. B. (1993). Understanding family process: basics of family systems theory. Thousand Oaks: SAGE Publications.
Catenacci, V. A., Barrett, C., Odgen, L., Browning, R., Schaefer, C. A., Hill, J., et al. (2014). Changes in physical activity and sedentary behavior in a randomized trial of an internet-based versus workbook-based family intervention study. Journal of Physical Activity & Health, 11(2), 348–358. https://doi.org/10.1123/jpah.2012-0043.
Centers for Disease Control and Prevention (2011a). Youth risk behavior surveillance system questionnaires. https://www.cdc.gov/healthyyouth/data/yrbs/questionnaires.htm. Accessed 2 Jan 2018.
Centers for Disease Control and Prevention (2011b). The health educator’s social media toolkit. https://www.cdc.gov/healthcommunication/toolstemplates/socialmediatoolkit_bm.pdf. Accessed 7 Jan 2018.
Centers for Disease Control and Prevention (2013a). Behavioral risk factor surveillance system questionnaire. http://www.cdc.gov/brfss/questionnaires/pdf-ques/2013%20BRFSS_English.pdf. Accessed 2 Jan 2018.
Centers for Disease Control and Prevention (2013b). State indicator report on fruits and vegetables. https://www.cdc.gov/nutrition/downloads/state-indicator-report-fruits-vegetables-2013.pdf. Accessed 4 Jan 2018.
Centers for Disease Control and Prevention (2014). Nutrition, physical activity, & obesity: adolescent and school health. http://www.cdc.gov/healthyyouth/npao/index.htm. Accessed 2 Jan 2018.
Cohen, J. (1988). Statistical power analysis for the behavioral sciences. Mahwah: L Erlbaum Associates.
Epstein, L. H., & Wrotniak, B. H. (2010). Future directions for pediatric obesity treatment. Obesity (Silver Spring), 18(Suppl 1), S8–12. https://doi.org/10.1038/oby.2009.425.
Epstein, L. H., Wing, R. R., & Valoski, A. (1985). Childhood obesity. Pediatric Clinics of North America, 32(2), 363–379. https://doi.org/10.1016/S0031-3955(16)34792-7.
Epstein, L. H., Gordy, C. C., Raynor, H. A., Beddome, M., Kilanowski, C. K., & Paluch, R. (2001). Increasing fruit and vegetable intake and decreasing fat and sugar intake in families at risk for childhood obesity. Obesity Research, 9(3), 171–178. https://doi.org/10.1038/oby.2001.18.
Epstein, L. H., Paluch, R. A., Roemmich, J. N., & Beecher, M. D. (2007). Family-based obesity treatment, then and now: twenty-five years of pediatric obesity treatment. Health Psychology, 26(4), 381–391. https://doi.org/10.1037/0278-6133.26.4.381.
Evenson, K. R., Catellier, D. J., Gill, K., Ondrak, K. S., & McMurray, R. G. (2008). Calibration of two objective measures of physical activity for children. Journal of Sports Sciences, 26(14), 1557–1565. https://doi.org/10.1080/02640410802334196.
Freedman, D. S., Mei, Z., Srinivasan, S. R., Berenson, G. S., & Dietz, W. H. (2007). Cardiovascular risk factors and excess adiposity among overweight children and adolescents: the Bogalusa Heart Study. The Journal of Pediatrics, 150(1), 12–17 e12. https://doi.org/10.1016/j.jpeds.2006.08.042.
Goldberg, J. H., & Kiernan, M. (2005). Innovative techniques to address retention in a behavioral weight-loss trial. Health Education Research, 20(4), 439–447. https://doi.org/10.1093/her/cyg139.
Guilamo-Ramos, V., Jaccard, J., Turrisi, R., & Johansson, M. (2005). Parental and school correlates of binge drinking among middle school students. American Journal of Public Health, 95(5), 894–899. https://doi.org/10.2105/AJPH.2003.018952.
Haskell, W. L., Lee, I. M., Pate, R. R., Powell, K. E., Blair, S. N., Franklin, B. A., et al. (2007). Physical activity and public health: updated recommendation for adults from the American College of Sports Medicine and the American Heart Association. Medicine & Science in Sports and Exercise, 39(8), 1423–1434. https://doi.org/10.1249/mss.0b013e3180616b27.
Icek, A. (1991). The theory of planned behavior. Organizational Behavior and Human Decision Processes, 50(2), 179–211. https://doi.org/10.1016/0749-5978(91)90020-t.
Kelsey, M. M., Zaepfel, A., Bjornstad, P., & Nadeau, K. J. (2014). Age-related consequences of childhood obesity. Gerontology, 60(3), 222–228. https://doi.org/10.1159/000356023.
Kiernan, M., Brown, S. D., Schoffman, D. E., Lee, K., King, A. C., Taylor, C. B., Schleicher, N. C., & Perri, M. G. (2013). Promoting healthy weight with “stability skills first”: a randomized trial. Journal of Consulting and Clinical Psychology, 81(2), 336–346. https://doi.org/10.1037/a0030544.
Kim, Y., Beets, M. W., & Welk, G. J. (2012). Everything you wanted to know about selecting the “right” actigraph accelerometer cut-points for youth, but …: a systematic review. Journal of Science and Medicine in Sport, 15(4), 311–321. https://doi.org/10.1016/j.jsams.2011.12.001.
Kim, S. A., Moore, L. V., Galuska, D., Wright, A. P., Harris, D., Grummer-Strawn, L. M., Merlo, C. L., Nihiser, A. J., Rhodes, D. G., & Division of Nutrition, Physical Activity, and Obesity, National Center for Chronic Disease Prevention and Health Promotion, CDC. (2014). Vital signs: fruit and vegetable intake among children—United States, 2003–2010. MMWR. Morbidity and Mortality Weekly Report, 63(31), 671–676.
Let's Move (2012). Learn the facts. https://letsmove.obamawhitehouse.archives.gov/learn-facts/epidemic-childhood-obesity. Accessed 5 Jan 2018.
Lee, I. M., & Buchner, D. M. (2008). The importance of walking to public health. Medicine and Science in Sports & Exercise, 40(7 Suppl), S512–S518. https://doi.org/10.1249/mss.0b013e31817c65d0.
Lee, R. E., Medina, A. V., Mama, S. K., Reese-Smith, J. Y., O’Connor, D. P., Brosnan, M., Cubbin, C., McMillan, T., & Estabrooks, P. A. (2011). Health is power: an ecological, theory-based health intervention for women of color. Contemporary Clinical Trials, 32(6), 916–923. https://doi.org/10.1016/j.cct.2011.07.008.
Loulis, S., & Kuczynski, L. (1997). Beyond one hand clapping: seeing bidirectionality in parent–child relations. Journal of Social and Personal Relationships, 14(4), 441–461. https://doi.org/10.1177/0265407597144002.
Moos, R. H. (1990). Conceptual and empirical approaches to developing family-based assessment procedures: resolving the case of the family environment scale. Family Process, 29(2), 199–208. https://doi.org/10.1111/j.1545-5300.1990.00199.x.
Morrison, R., Reilly, J. J., Penpraze, V., Westgarth, C., Ward, D. S., Mutrie, N., Hutchison, P., Young, D., McNicol, L., Calvert, M., & Yam, P. S. (2013). Children, parents and pets exercising together (CPET): exploratory randomised controlled trial. BMC Public Health, 13(1), 1096. https://doi.org/10.1186/1471-2458-13-1096.
National Heart, Lung, and Blood Institute (2013). We Can!. http://www.nhlbi.nih.gov/health/educational/wecan/. Accessed 13 Dec 2017.
Ornelas, I. J., Perreira, K. M., & Ayala, G. X. (2007). Parental influences on adolescent physical activity: a longitudinal study. International Journal of Behavioral Nutrition and Physical Activity, 4, 3. https://doi.org/10.1186/1479-5868-4-3.
Pearson, J., Muller, C., & Frisco, M. L. (2006). Parental involvement, family structure, and adolescent sexual decision making. Sociological Perspectives, 49(1), 67–90. https://doi.org/10.1525/sop.2006.49.1.67.
Rhee, K. E., Jelalian, E., Boutelle, K., Dickstein, S., Seifer, R., & Wing, R. (2016). Warm parenting associated with decreasing or stable child BMI during treatment. Childhood Obesity, 12(2), 94–102. https://doi.org/10.1089/chi.2015.0127.
Schoffman, D. E., Turner-McGrievy, G., Jones, S. J., & Wilcox, S. (2013). Mobile apps for pediatric obesity prevention and treatment, healthy eating, and physical activity promotion: just fun and games? Translational Behavioral Medicine, 3(3), 320–325. https://doi.org/10.1007/s13142-013-0206-3.
Singh, A. S., Mulder, C., Twisk, J. W., van Mechelen, W., & Chinapaw, M. J. (2008). Tracking of childhood overweight into adulthood: a systematic review of the literature. Obesity Reviews, 9(5), 474–488. https://doi.org/10.1111/j.1467-789X.2008.00475.x.
Sze, Y. Y., Daniel, T. O., Kilanowski, C. K., Collins, R. L., & Epstein, L. H. (2015). Web-based and mobile delivery of an episodic future thinking intervention for overweight and obese families: a feasibility study. JMIR Mhealth Uhealth, 3(4), e97. https://doi.org/10.2196/mhealth.4603.
The Diabetes Prevention Program Research Group. (2002). The Diabetes Prevention Program (DPP): description of lifestyle intervention. Diabetes Care, 25(12), 2165–2171. https://doi.org/10.2337/diacare.25.12.2165.
Thomas, H. (2006). Obesity prevention programs for children and youth: why are their results so modest? Health Education Research, 21(6), 783–795. https://doi.org/10.1093/her/cyl143.
Troiano, R. P., Berrigan, D., Dodd, K. W., Mâsse, L. C., Tilert, T., & McDowell, M. (2008). Physical activity in the United States measured by accelerometer. Medicine & Science in Sports & Exercise, 40(1), 181–188. https://doi.org/10.1249/mss.1240b1013e31815a31851b31813.
Trost, S. G., Pate, R. R., Freedson, P. S., Sallis, J. F., & Taylor, W. C. (2000). Using objective physical activity measures with youth: how many days of monitoring are needed? Medicine and Science in Sports & Exercise, 32(2), 426–431.
Turner-McGrievy, G. M., Hales, S. B., Schoffman, D. E., Valafar, H., Brazendale, K., Weaver, R. G., et al. (2016). Choosing between responsive-design websites versus mobile apps for your mobile behavioral intervention: presenting four case studies. Translational Behavioral Medicine, 7(2), 224–232. https://doi.org/10.1007/s13142-016-0448-y.
Acknowledgements
We would like to thank the research participants and staff volunteers for their contributions to the study, especially Klara Milojkovic for her dedication to the study and assistance with the research process.
Funding
This study was partially funded by Provost’s grants from the Department of Health Promotion, Education, and Behavior in the Arnold School of Public Health, University of South Carolina.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of Interest
The authors declare that they have no competing interests.
Research Involving Human Participants
All procedures performed in this study were approved by the institutional review board at the University of South Carolina. All procedures performed in this study involving human participants were in accordance with the ethical standards of the institutional review board and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Informed Consent
Informed consent (parents) and assent (children) were obtained from all individual participants included in the study.
Electronic supplementary material
ESM 1
(DOCX 19 kb)
Rights and permissions
About this article
Cite this article
Jake-Schoffman, D.E., Turner-McGrievy, G., Wilcox, S. et al. The mFIT (Motivating Families with Interactive Technology) Study: a Randomized Pilot to Promote Physical Activity and Healthy Eating Through Mobile Technology. J. technol. behav. sci. 3, 179–189 (2018). https://doi.org/10.1007/s41347-018-0052-8
Published:
Issue Date:
DOI: https://doi.org/10.1007/s41347-018-0052-8