Abstract
Aim
This systematic review was conducted to explore the associations between sarcopenia, hospitalization and length of stay in the old people.
Methods
Pubmed, Embase, Medline and Cochrane Central Register of Controlled Trails from January 2009 to October 2017 were searched in this review. We included prospective studies, which had the clear definition of sarcopenia and reported the hospitalization or length of stay as one of outcomes. Adjusted Odd ratios (aORs), hazard ratios (aHRs) or relative risks (aRRs) extracted from the studies were combined to synthesize pooled effect measures. Heterogeneity, and methodological quality were assessed using I² statistic and Newcastle–Ottawa scale, respectively.
Results
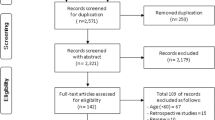
Nine studies were included in this review. Of these, 8 studies with 4174 individuals reported results for hospitalization, 3 studies involving 6276 old people in the community reported results for length of stay. Sarcopenia was significantly associated with future hospitalization (RR 1.40, 95% CI 1.04–1.89, p = 0.029; data from 8 studies). A subgroup analysis showed the associations between sarcopenia and readmission in hospitalized old patients that were statistically significant (RR 1.75, 95% CI 1.01–3.03, p = 0.044; data from 8 studies). However, this association were not found in the community-dwelling older subjects (RR 1.08, 95% CI 0.74–1.57, p = 0.688; data from 8 studies), uncertain in nursing home residents. The association of sarcopenia and length of stay was not statistically significant (OR 1.21, 95% CI 0.90–1.63, p = 0.20; data from 8 studies) in community-dwelling residents.
Conclusions
This systematic review demonstrates that sarcopenia is a significant predictor of readmission in old inpatients, but not associated with hospitalization or length of stay in community-dwelling old adults.




Similar content being viewed by others
References
Cruz-Jentoft AJ, Landi F, Topinková E, Michel JP (2010) Understanding sarcopenia as a geriatric syndrome. Curr Opin Clin Nutr Metab Care 13:1–7. https://doi.org/10.1097/MCO.0b013e328333c1c1
Cao L, Morley JE (2016) Sarcopenia is recognized as an independent condition by an international classification of disease, tenth revision, Clinical MODIFICATION (ICD-10-CM) Code. J Am Med Dir Assoc 17:675–677. https://doi.org/10.1016/j.jamda.2016.06.001
Baumgartner RN, Koehler KM, Gallagher D et al (1998) Epidemiology of sarcopenia among the elderly in New Mexico. Am J Epidemiol 147:755–763
Newman AB, Kupelian V, Visser M et al (2003) Sarcopenia: alternative definitions and associations with lower extremity function. J Am Geriatr Soc 51:1602–1609
Fielding RA, Vellas B, Evans WJ et al (2011) Sarcopenia: an undiagnosed condition in older adults. Current consensus definition: prevalence, etiology, and consequences. International working group on sarcopenia. J Am Med Dir Assoc 12:249–256. https://doi.org/10.1016/j.jamda.2011.01.003
Cruz-Jentoft AJ, Baeyens JP, Bauer JM et al (2010) Sarcopenia: European consensus on definition and diagnosis: report of the European working group on sarcopenia in older people. Age Ageing 39:412–423. https://doi.org/10.1093/ageing/afq034
Studenski SA, Peters KW, Alley DE et al (2014) The FNIH Sarcopenia Project: rationale, study description, conference recommendations and final estimates. J Gerontol A Biol Sci Med Sci 69:547–558. https://doi.org/10.1093/gerona/glu010
Chen LK, Liu LK, Woo J, Assantachai P et al (2014) Sarcopenia in Asia: consensus report of the asian working group for sarcopenia. J Am Med Dir Assoc 15:95–101. https://doi.org/10.1016/j.jamda.2013.11.025
Yoshimura N, Oka H, Muraki S et al (2011) Reference values for hand grip strength, muscle mass, walking time, and one-leg standing time as indices for locomotive syndrome and associated disability: the second survey of the ROAD study. J Orthop Sci 16:768–777. https://doi.org/10.1007/s00776-011-0160-1
Cruz-Jentoft AJ, Landi F, Schneider SM et al (2014) Prevalence of and interventions for sarcopenia in ageing adults: A systematic review. Report of the International Sarcopenia Initiative(EWGSOP and IWGS). Age Ageing 43:748–759. https://doi.org/10.1093/ageing/afu115
Levant S, Chari K, DeFrances CJ (2015) Hospitalizations for patients aged 85 and over in the United States, 2000–2010. NCHS Data Brief 182:1–8
Gariballa S, Alessa A (2013) Sarcopenia: prevalence and prognostic significance in hospitalized patients. Clin Nutr 32:772–776. https://doi.org/10.1016/j.clnu.2013.01.010
Woo J, Leung J, Morley JE (2015) Defining sarcopenia in terms of incident adverse outcomes. J Am Med Dir Assoc 16:247–252. https://doi.org/10.1016/j.jamda.2014.11.013
Bianchi L, Ferrucci L, Cherubini A et al (2016) The predictive value of the EWGSOP definition of sarcopenia: results from the InCHIANTI study. J Gerontol A Biol Sci Med Sci 71:259–264. https://doi.org/10.1093/gerona/glv129
Wang Rong,HuYixin,Fan, Li et al (2016) Effect of sarcopenia on the rate of rehospitalization in elderly male patients. Chin J Health Care Med 02:106–109
Henwood T, Hassan B, Swinton P, Senior H, Keogh J (2017) Consequences of sarcopenia among nursing home residents at long-term follow-up. Geriatr Nurs 38:406–411. https://doi.org/10.1016/j.gerinurse
Yang M, Hu X, Wang H, Zhang L, Hao Q, Dong B (2017) Sarcopenia predicts readmission and mortality in elderly patients in acute care wards: a prospective study. J Cachexia Sarcopenia Muscle 8:251–258. https://doi.org/10.1002/jcsm.12163
Cawthon PM, Lui LY, McCulloch CE et al (2017) Sarcopenia and health care utilization in older women. J Gerontol A Biol Sci Med Sci 72:95–101. https://doi.org/10.1093/gerona/glw118
Cawthon PM, Lui LY, Taylor BC et al (2017) Clinical definitions of sarcopenia and risk of hospitalization in community-dwelling older men: the osteoporotic fractures in men study. J Gerontol A Biol Sci Med Sci 72:1383–1389. https://doi.org/10.1093/gerona/glw327
Beaudart C, Zaaria M, Pasleau F et al (2017) Health outcomes of sarcopenia: a systematic review and meta-analysis. PLoS One 12:e0169548. https://doi.org/10.1371/journal.pone.0169548
Wells GA, Shea B, O’Connell D et al. The Newcastle–Ottawa Scale (NOS) for assessing the quality of nonrandomised studies in meta-analyses. http://www.ohri.ca/programs/clinical_epidemiology/oxford.asp. Accessed 18 Dec 2017
Zhang J, Yu KF (1998) What’s the relative risk? A method of correcting the odds ratio in cohort studies of common outcomes. JAMA 280:1690–1691
Pérez-Zepeda MU, Sgaravatti A, Dent E (2017) Sarcopenia and post-hospital outcomes in older adults: a longitudinal study. Arch Gerontol Geriatr 69:105–109. https://doi.org/10.1016/j.archger.2016.10.013
Henwood T, Hassan B, Swinton P, Senior H, Keogh J (2017) Consequences of sarcopenia among nursing home residents at long-term follow-up. Geriatr Nurs Sep–Oct 38(5):406–411. https://doi.org/10.1016/j.gerinurse.2017.02.003
Huang DD, Zhou CJ, Wang SL et al (2017) Impact of different sarcopenia stages on the postoperative outcomes after radical gastrectomy for gastric cancer. Surgery 161:680–693. https://doi.org/10.1016/j.surg.2016.08.030
Hsu YH, Liang CK, Chou MY et al (2014) Association of cognitive impairment, depressive symptoms and sarcopenia among healthy older men in the veterans retirement community in southern Taiwan: a cross-sectional study. Geriatr Gerontol Int 14 (Suppl 1):102–108. https://doi.org/10.1111/ggi.12221
Springer J, Anker SD (2016) Publication trends in cachexia and sarcopenia in elderly heart failure patients. Wien Klin Wochenschr 128:446–454. https://doi.org/10.1007/s00508-016-1126-2
Bone AE, Hepgul N, Kon S, Maddocks M (2017) Sarcopenia and frailty in chronic respiratory disease. Chron Respir Dis 14:85–99. https://doi.org/10.1177/1479972316679664
Sinclair M, Gow PJ, Grossmann M, Angus PW (2016) Review article: sarcopenia in cirrhosis–aetiology, implications and potential therapeutic interventions. Aliment Pharmacol Ther 43:765–777. https://doi.org/10.1111/apt.13549
Jang HC (2016) Sarcopenia, frailty, and diabetes in older adults. Diabetes Metab J 40:182–189. https://doi.org/10.4093/dmj.2016.40.3.182
Collins J, Noble S, Chester J, Coles B, Byrne A (2014) The assessment and impact of sarcopenia in lung cancer: a systematic literature review. BMJ Open 4:e003697. https://doi.org/10.1136/bmjopen-2013-003697
Martone AM, Bianchi L, Abete P et al (2017) The incidence of sarcopenia among hospitalized older patients: results from the Glisten study. J Cachexia Sarcopenia Muscle 8:907–914. https://doi.org/10.1002/jcsm.12224
Ali S, Garcia JM (2014) Sarcopenia, cachexia and aging: diagnosis, mechanisms and therapeutic options—a mini-review. Gerontology 60:294–305. https://doi.org/10.1159/000356760
Liu CJ, Latham NK (2009) Progressive resistance strength training for improving physical function in older adults. Cochrane Database Syst Rev (3):CD002759. https://doi.org/10.1002/14651858
Calvani R, Miccheli A, Landi F et al (2013) Current nutritional recommendations and novel dietary strategies to manage sarcopenia. J Frailty Aging 2:38–53
Morley JE, Argiles JM, Evans WJ et al (2010) Nutritional recommendations for the management of sarcopenia. J Am Med Dir Assoc 11:391–396. https://doi.org/10.1016/j.jamda
Emmelot-Vonk MH, Verhaar HJ, Nakhai Pour HR et al (2008) Effect of testosterone supplementation on functional mobility, cognition, and other parameters in older men: a randomized controlled trial. JAMA 299:39–52. https://doi.org/10.1001/jama.2007.51
Cappola AR (2013) Testosterone therapy and risk of cardiovascular disease in men. JAMA 310:1805–1806. https://doi.org/10.1001/jama.2013.280387
Morley JE, Kaiser FE, Perry HM et al (1997) Longitudinal changes in testosterone, luteinizing hormone, and follicle-stimulating hormone in healthy older men. Metabolism 46:410–413
Prado CM, Lieffers JR, McCargar LJ et al (2008) Prevalence and clinical implications of sarcopenic obesity in patients with solid tumours of the respiratory and gastrointestinal tracts: a population-based study. Lancet Oncol 9:629–635. https://doi.org/10.1016/S1470-2045(08)70153-0
Shen W, Punyanitya M, Wang Z et al (2004) Total body skeletal muscle and adipose tissue volumes: estimation from a single abdominal cross-sectional image. J Appl Physiol (1985) 97:2333–2338. https://doi.org/10.1152/japplphysiol.00744.2004
Peterson SJ, Braunschweig CA (2016) Prevalence of sarcopenia and associated outcomes in the clinical setting. Nutr Clin Pract 31:40–48. https://doi.org/10.1177/0884533615622537
Funding
The authors declare that they have received no funding for the study
Author information
Authors and Affiliations
Contributions
YL formulated the research question, designed the study and screened the articles, collected the data, and drafted the manuscript. YX designed the study and screened the articles. QK collected the data. ML analyzed the data.BD assisted with formulating the research question and supervising the quality of the paper.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest
Ethical approval
For this type of study, formal consent is not required.
Human and animal rights
This article does not contain any studies with human participants or animals performed by any of the authors.
Informed consent
This type of study is based on aggregated data of already published studies. Informed consent can not be obtained from patients.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Zhao, Y., Zhang, Y., Hao, Q. et al. Sarcopenia and hospital-related outcomes in the old people: a systematic review and meta-analysis. Aging Clin Exp Res 31, 5–14 (2019). https://doi.org/10.1007/s40520-018-0931-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40520-018-0931-z