Abstract
Purpose
To provide 5-year time trends in prevalence and demographic, substance use, and mental health correlates of compulsive exercise among a national sample of college men and women.
Methods
We analyzed 4 academic survey years (2016–2020; N = 8251) of the national (USA) Healthy Minds Study. Compulsive exercise was measured by self-report of any occurrence of “compulsive” exercise in the past 4 weeks. Unadjusted prevalence of compulsive exercise in the past 4 weeks was estimated across the 4 survey years by sex. Multiple logistic regression analyses were conducted among the pooled sample and stratified by sex to estimate the associations between compulsive exercise in the past 4 weeks and demographic, substance use, and mental health correlates.
Results
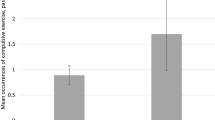
Among the pooled sample, 11% (95% confidence interval [CI] 9.60–12.42%) of men and 17% (95% CI 15.86–18.24%) of women reported compulsive exercise in the past 4 weeks. Prevalence across the 4 survey years remained stable among men and women. Higher body mass index was associated with greater odds of any compulsive exercise in the past 4 weeks among men, while any sports participation was associated with greater odds of any compulsive exercise in the past 4 weeks among women. Compulsive exercise in the past 4 weeks was associated with greater odds of all mental health symptoms and illicit drug use among men and women, and higher odds of alcohol use among women.
Conclusion
Compulsive exercise is relatively common among college men and women and is associated with substance use behaviors and poor mental health symptoms.
Level of Evidence
V, cross-sectional descriptive study

Similar content being viewed by others
Availability of data and material
The Healthy Minds Study is available to researchers. Please visit http://healthymindsnetwork.org for more information.
References
Obert J, Pearlman M, Obert L, Chapin S (2017) Popular weight loss strategies: a review of four weight loss techniques. Curr Gastroenterol Rep 19:17–20. https://doi.org/10.1007/s11894-017-0603-8
Petridou A, Siopi A, Mougios V (2019) Exercise in the management of obesity. Metabolism 92:163–169. https://doi.org/10.1016/j.metabol.2018.10.009
Cooney G, Dwan K, Mead G (2014) Exercise for depression. JAMA J Am Med Assoc 311:2432–2433. https://doi.org/10.1001/jama.2014.4930
Da Silva MA, Singh-Manoux A, Brunner EJ et al (2012) Bidirectional association between physical activity and symptoms of anxiety and depression: the whitehall II study. Eur J Epidemiol 27:537–546. https://doi.org/10.1007/s10654-012-9692-8
De Moor MHM, Beem AL, Stubbe JH et al (2006) Regular exercise, anxiety, depression and personality: a population-based study. Prev Med (Baltim) 42:273–279. https://doi.org/10.1016/j.ypmed.2005.12.002
Lynch WJ, Robinson AM, Abel J, Smith MA (2017) Exercise as a prevention for substance use disorder: a review of sex differences and neurobiological mechanisms. Curr Addict Reports 4:455–466. https://doi.org/10.1007/s40429-017-0178-3
Chekroud SR, Gueorguieva R, Zheutlin AB et al (2018) Association between physical exercise and mental health in 1·2 million individuals in the USA between 2011 and 2015: a cross-sectional study. Lancet Psychiatry 5:739–746. https://doi.org/10.1016/S2215-0366(18)30227-X
Meyer C, Taranis L (2011) Exercise in the eating disorders: terms and definitions. Eur Eat Disord Rev 19:169–173. https://doi.org/10.1002/erv.1121
Mond J, Gorrell S (2021) “Excessive exercise” in eating disorders research: problems of definition and perspective. Eat Weight Disord Stud Anorexia Bulim Obes. https://doi.org/10.1007/s40519-020-01075-3
Dittmer N, Jacobi C, Voderholzer U (2018) Compulsive exercise in eating disorders : proposal for a definition and a clinical assessment. J Eat Disord 6:1–9
Bratland-Sanda S, Mathisen TF, Sundgot-Borgen J, Rosenvinge JH (2019) Defining compulsive exercise in eating disorders: Acknowledging the exercise paradox and exercise obsessions. J Eat Disord 7:8–10. https://doi.org/10.1186/s40337-019-0238-2
Fairburn CG, Beglin S (2008) Eating Disorder Examination Questionnaire. In: Fairburn CG (ed) Cognitive behavior therapy and eating disorders. Guilford Press, New York, pp 309–313
Lavender JM, De Young KP, Anderson DA (2010) Eating Disorder Examination Questionnaire (EDE-Q): norms for undergraduate men. Eat Behav 11:119–121. https://doi.org/10.1016/j.eatbeh.2009.09.005
Luce KH, Crowther JH, Pole M (2008) Eating Disorder Examination Questionnaire (EDE-Q): norms for undergraduate women. Int J Eat Disord 41:273–276. https://doi.org/10.1002/eat.20504
Schaumberg K, Anderson LM, Reilly E, Anderson DA (2014) Patterns of compensatory behaviors and disordered eating in college students. J Am Coll Heal 62:526–533. https://doi.org/10.1080/07448481.2014.930468
Young S, Touyz S, Meyer C et al (2017) Validity of exercise measures in adults with anorexia nervosa: the EDE, compulsive exercise test and other self-report scales. Int J Eat Disord 50:533–541. https://doi.org/10.1002/eat.22633
Rizk M, Mattar L, Kern L et al (2020) Physical activity in eating disorders: a systematic review. Nutrients 12:1–33. https://doi.org/10.3390/nu12010183
Monell E, Levallius J, Forsén Mantilla E, Birgegård A (2018) Running on empty—a nationwide large-scale examination of compulsive exercise in eating disorders. J Eat Disord 6:1–10. https://doi.org/10.1186/s40337-018-0197-z
Fietz M, Touyz S, Hay P (2014) A risk profile of compulsive exercise in adolescents with an eating disorder: a systematic review. Adv Eat Disord 2:241–263. https://doi.org/10.1080/21662630.2014.894470
Lichtenstein MB, Hinze CJ, Emborg B et al (2017) Compulsive exercise: links, risks and challenges faced. Psychol Res Behav Manag 10:85–95. https://doi.org/10.2147/prbm.s113093
Nagata JM, Carlson JL, Kao JM et al (2017) Characterization and correlates of exercise among adolescents with anorexia nervosa and bulimia nervosa. Int J Eat Disord 50:1394–1403. https://doi.org/10.1016/j.physbeh.2017.03.040
Smith AR, Fink EL, Anestis MD et al (2013) Exercise caution: over-exercise is associated with suicidality among individuals with disordered eating. Psychiatry Res 206:246–255. https://doi.org/10.1016/j.psychres.2012.11.004
Sawyer SM, Azzopardi PS, Wickremarathne D, Patton GC (2018) The age of adolescence. Lancet Child Adolesc Heal 2:223–228. https://doi.org/10.1016/S2352-4642(18)30022-1
Bucchianeri MM, Arikian AJ, Hannan PJ et al (2013) Body dissatisfaction from adolescence to young adulthood: findings from a 10-year longitudinal study. Body Image 10:1–7. https://doi.org/10.1016/j.bodyim.2012.09.001
Ward ZJ, Rodriguez P, Wright DR et al (2019) Estimation of eating disorders prevalence by age and associations with mortality in a simulated nationally representative US Cohort. JAMA Netw Open 2:e1912925. https://doi.org/10.1001/jamanetworkopen.2019.12925
Neumark-Sztainer D, Wall M, Larson NI et al (2011) Dieting and disordered eating behaviors from adolescence to young adulthood: Findings from a 10-year longitudinal study. J Am Diet Assoc 111:1004–1011. https://doi.org/10.1016/j.jada.2011.04.012
Eisenberg D, Hunt J, Speer N (2013) Mental health in american colleges and universities: variation across student subgroups and across campuses. J Nerv Ment Dis 201:60–67. https://doi.org/10.1097/NMD.0b013e31827ab077
Arria AM, Caldeira KM, Allen HK et al (2017) Prevalence and incidence of drug use among college students: an 8-year longitudinal analysis. Am J Drug Alcohol Abuse 43:711–718
Schulenberg JE, Johnston LD, O’Malley PM, Bachman JG, Miech RA, Patrick ME (2020) Monitoring the future national survey results on drug use, 1975–2019: Volume II, College students and adults ages 19–60. Ann Arbor: Institute for Social Research, The University of Michigan. Available at http://monitoringthefuture.org/pubs.html#monographs
Eisenberg D, Lipson SK (2020) Healthy Minds Network. https://healthymindsnetwork.org
Lipson SK, Sonneville KR (2017) Eating disorder symptoms among undergraduate and graduate students at 12 U.S. colleges and universities. Eat Behav 24:81–88. https://doi.org/10.1016/j.eatbeh.2016.12.003
Nagata JM, Murray SB, Compte EJ et al (2020) Community norms for the eating disorder examination questionnaire (EDE-Q) among cisgender bisexual plus women and men. Eat Weight Disord Stud Anorexia Bulim Obes. https://doi.org/10.1007/s40519-020-01070-8
Nagata JM, Murray SB, Compte EJ et al (2020) Community norms for the Eating Disorder Examination Questionnaire (EDE-Q) among transgender men and women. Eat Behav 37:101381. https://doi.org/10.1016/j.eatbeh.2020.101381
Gollust SE, Eisenberg D, Golberstein E (2008) Prevalence and correlates of self-injury among university students. J Am Coll Heal 56:491–498
Serras A, Saules KK, Cranford JA, Eisenberg D (2010) Self-injury, substance use, and associated risk factors in a multi-campus probability sample of college students. Psychol Addict Behav 24:119–128. https://doi.org/10.1037/a0017210
Ganson KT, Rodgers RF, Lipson SK et al (2020) Sexual assault victimization and eating disorders among college-enrolled men. J Interpers Violence. https://doi.org/10.1177/0886260520958634
Ganson KT, Murray SB, Nagata JM (2021) Associations between eating disorders and illicit drug use among college students. Int J Eat Disord. https://doi.org/10.1002/eat.23493
Kroenke K, Spitzer RL, Williams JBW (2001) The PHQ-9: validity of a brief depression severity measure. J Gen Intern Med 16:606–613
Spitzer RL, Kroenke K, Williams JBW, Group PHQPCS (1999) Validation and utility of a self-report version of PRIME-MD: the PHQ Primary Care Study. JAMA 282:1737–1744. https://doi.org/10.1001/jama.282.18.1737
Levis B, Benedetti A, Thombs BD (2019) Accuracy of Patient Health Questionnaire-9 (PHQ-9) for screening to detect major depression: Individual participant data meta-analysis. BMJ. https://doi.org/10.1136/bmj.l1476
Spitzer RL, Kroenke K, Williams JBW, Löwe B (2006) A brief measure for assessing generalized anxiety disorder: the GAD-7. Arch Intern Med 166:1092–1097. https://doi.org/10.1001/archinte.166.10.1092
Byrd-Bredbenner C, Eck K, Quick V (2021) GAD-7, GAD-2, and GAD-mini: psychometric properties and norms of university students in the United States. Gen Hosp Psychiatry 69:61–66. https://doi.org/10.1016/j.genhosppsych.2021.01.002
Morgan JF, Reid F, Lacey JH (1999) The SCOFF questionnaire: assessment of a new screening tool for eating disorders. Br Med J 319:1467–1468. https://doi.org/10.1136/bmj.319.7223.1467
Luck AJ, Morgan JF, Reid F et al (2002) The SCOFF questionnaire and clinical interview for eating disorders in general practice: comparative study. Br Med J 325:755–756. https://doi.org/10.1136/bmj.325.7367.755
Maguen S, Hebenstreit C, Li Y et al (2018) Screen for disordered eating: improving the accuracy of eating disorder screening in primary care. Gen Hosp Psychiatry 50:20–25. https://doi.org/10.1016/j.genhosppsych.2017.09.004
Lipson SK, Kern A, Eisenberg D, Breland-Noble AM (2018) Mental health disparities among college students of color. J Adolesc Heal 63:348–356. https://doi.org/10.1016/j.jadohealth.2018.04.014
Murray SB, Nagata JM, Griffiths S et al (2017) The enigma of male eating disorders: a critical review and synthesis. Clin Psychol Rev 57:1–11. https://doi.org/10.1016/j.cpr.2017.08.001
Mitchison D, Mond J (2015) Epidemiology of eating disorders, eating disordered behaviour, and body image disturbance in males: a narrative review. J Eat Disord 3:1–9. https://doi.org/10.1186/s40337-015-0058-y
Nagata JM, Ganson KT, Griffiths S et al (2020) Prevalence and correlates of muscle-enhancing behaviors among adolescents and young adults in the United States. Int J Adolesc Med Health. https://doi.org/10.1515/ijamh-2020-0001
Murray SB, Brown TA, Lavender JM et al (2020) The evolving nature of weight dissatisfaction and eating behaviors among men: secular trends among college men across four decades. J Abnorm Psychol 129:824–830. https://doi.org/10.1037/abn0000587
Benjamini Y, Hochberg Y (1995) Controlling the false discovery rate: a practical and powerful approach to multiple testing. J R Stat Soc 57:289–300
Goodwin H, Haycraft E, Meyer C (2011) Sociocultural correlates of compulsive exercise: Is the environment important in fostering a compulsivity towards exercise among adolescents? Body Image 8:390–395. https://doi.org/10.1016/j.bodyim.2011.05.006
Tylka TL (2011) Refinement of the tripartite influence model for men: dual body image pathways to body change behaviors. Body Image 8:199–207. https://doi.org/10.1016/j.bodyim.2011.04.008
Neumark-Sztainer D, Wall M, Story M, Standish AR (2012) Dieting and unhealthy weight control behaviors during adolescence: associations with 10-year changes in body mass index. J Adolesc Heal 50:80–86. https://doi.org/10.1016/j.jadohealth.2011.05.010
Bratland-Sanda S, Sundgot-Borgen J (2013) Eating disorders in athletes: overview of prevalence, risk factors and recommendations for prevention and treatment. Eur J Sport Sci 13:499–508. https://doi.org/10.1080/17461391.2012.740504
Joy E, Kussman A, Nattiv A (2016) 2016 update on eating disorders in athletes: a comprehensive narrative review with a focus on clinical assessment and management. Br J Sports Med 50:154–162. https://doi.org/10.1136/bjsports-2015-095735
Gorrell S, Scharmer C, Kinasz K, Anderson D (2020) Compulsive exercise and weight suppression: associations with eating pathology in distance runners. Eat Behav 36:101358. https://doi.org/10.1016/j.eatbeh.2019.101358
Di Lodovico L, Dubertret C, Ameller A (2018) Vulnerability to exercise addiction, socio-demographic, behavioral and psychological characteristics of runners at risk for eating disorders. Compr Psychiatry 81:48–52. https://doi.org/10.1016/j.comppsych.2017.11.006
Tarnopolsky MA (2011) Caffeine and creatine use in sport. Ann Nutr Metab 57:1–8. https://doi.org/10.1159/000322696
Udo T, Grilo CM (2019) Psychiatric and medical correlates of DSM-5 eating disorders in a nationally representative sample of adults in the United States. Int J Eat Disord. https://doi.org/10.1002/eat.23004
Nutley SK, Mathews CA, Striley CW (2020) Disordered eating is associated with non-medical use of prescription stimulants among college students. Drug Alcohol Depend 209:107907. https://doi.org/10.1016/j.drugalcdep.2020.107907
Wong CF, Silva K, Kecojevic A et al (2013) Coping and emotion regulation profiles as predictors of nonmedical prescription drug and illicit drug use among high-risk young adults. Drug Alcohol Depend 132:165–171. https://doi.org/10.1016/j.drugalcdep.2013.01.024
Horvath SA, Shorey RC, Racine SE (2020) Emotion dysregulation as a correlate of food and alcohol disturbance in undergraduate students. Eat Behav 38:101409. https://doi.org/10.1016/j.eatbeh.2020.101409
Rancourt D, Ahlich E, Choquette EM et al (2020) A comparison of food and alcohol disturbance (FAD) in sorority and non-sorority women. J Am Coll Heal. https://doi.org/10.1080/07448481.2020.1740233
Lupi M, Martinotti G, Di Giannantonio M (2017) Drunkorexia: an emerging trend in young adults. Eat Weight Disord 22:619–622. https://doi.org/10.1007/s40519-017-0429-2
Kondo T, Nakano Y, Adachi S, Murohara T (2019) Effects of tobacco smoking on cardiovascular disease. Circ J 83:1980–1985. https://doi.org/10.1253/circj.CJ-19-0323
Rice F, Riglin L, Lomax T et al (2019) Adolescent and adult differences in major depression symptom profiles. J Affect Disord 243:175–181. https://doi.org/10.1016/j.jad.2018.09.015
Gratz KL (2003) Risk factors for and functions of deliberate self-harm: an empirical and conceptual review. Clin Psychol Sci Pract 10:192–205. https://doi.org/10.1093/clipsy/bpg022
Nock MK (2010) Self-injury. Annu Rev Clin Psychol 6:339–363. https://doi.org/10.1146/annurev.clinpsy.121208.131258
Gümmer R, Giel KE, Schag K et al (2015) High levels of physical activity in anorexia nervosa: a systematic review. Eur Eat Disord Rev 23:333–344. https://doi.org/10.1002/erv.2377
Taranis L, Meyer C (2011) Associations between specific components of compulsive exercise and eating-disordered cognitions and behaviors among young women. Int J Eat Disord 44:452–458. https://doi.org/10.1002/eat.20838
Oberle CD, Watkins RS, Burkot AJ (2018) Orthorexic eating behaviors related to exercise addiction and internal motivations in a sample of university students. Eat Weight Disord 23:67–74. https://doi.org/10.1007/s40519-017-0470-1
Meyer C, Taranis L, Goodwin H, Haycraft E (2011) Compulsive exercise and eating disorders. Eur Eat Disord Rev 19:174–189. https://doi.org/10.1002/erv.1122
Davern M (2013) Nonresponse rates are a problematic indicator of nonresponse bias in survey research. Health Serv Res 48:905–912. https://doi.org/10.1111/1475-6773.12070
Fosnacht K, Sarraf S, Howe E, Peck LK (2017) How important are high response rates for college surveys? Rev High Educ 40:245–265. https://doi.org/10.1353/rhe.2017.0003
Murray SB, Griffiths S, Mond JM (2016) Evolving eating disorder psychopathology: conceptualising muscularity-oriented disordered eating. Br J Psychiatry 208:414–415. https://doi.org/10.1192/bjp.bp.115.168427
Acknowledgements
We would like to thank Nicole Lisi for providing research assistance and Samuel Benabou for providing editorial assistance.
Funding
No funding was used to support this research.
Author information
Authors and Affiliations
Contributions
KTG and JMN conceptualized the study aims and statistical analysis plan. KTG conducted the statistical analysis and wrote a first draft of the manuscript. All authors provided edits and comments on previous versions of the manuscript. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Conflict of interest
All authors declare that they have no conflict of interest.
Research involving human participants
Healthy Minds Study was approved by the Health Sciences and Behavioral Sciences Institutional Review Board at the University of Michigan and all participating institutions. This study is exempt from research ethics approval given the data are publicly available and unidentifiable.
Informed consent
Informed consent was obtained from all individual participants included in the study.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Ganson, K.T., Mitchison, D., Rodgers, R.F. et al. Compulsive exercise among college students: 5-year time trends in prevalence and demographic, substance use, and mental health correlates. Eat Weight Disord 27, 717–728 (2022). https://doi.org/10.1007/s40519-021-01210-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40519-021-01210-8