Abstract
Aim
To assess dental caries experience and periodontal treatment needs among Libyan children diagnosed with autistic spectrum disorder (ASD).
Materials and methods
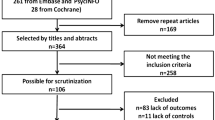
A cross-sectional, comparative case–control study was used, in which dental caries experience of 50 children with ASD was compared with that of 50 controls. The children with ASD were recruited from Benghazi Centre of Children with ASD, Libya. Controls were recruited from school children and matched for age, gender and socioeconomic status. DMFT, dmft for dental caries experience and CPITN for periodontal treatment needs were calculated according to WHO criteria by a calibrated examiner. Scores for DMFT as well as CPITN indices were compared using bivariate analysis.
Results
The data analysed for this study comprised observations from a group of children (cases = 50) diagnosed with ASD matched with healthy children (controls = 50). Consequently, each group consisted of 40 males and 10 females aged between 3 and 14 years (mean 7.29 ± 3.11). The ASD children showed significantly lower means for DMFT and dmft teeth as well as higher periodontal treatment needs (p > 0.05).
Conclusion
Children with ASD were found to be more likely caries-free and have lower DMFT scores and higher unmet periodontal treatment needs than did the unaffected control children.
Similar content being viewed by others
References
Barry S, O’Sullivan EA, Toumba KJ. Barriers to dental care for children with autism spectrum disorder. Eur Arch Paediatr Dent. 2014;15:127–34.
Bassoukou IH, Nicolau J, dos Santos MT. Saliva flow rate, buffer capacity, and pH of autistic individuals. Clin Oral Investig. 2009;13:23–7.
CDC. Facts about ASDs [Online]. Atlanta, USA. Centers for Disease Control and Prevention. http://www.cdc.gov/ncbddd/autism/facts.html (2014). Accessed 15 Feb 2014.
Dao LP, Zwetchkenbaum S, Inglehart MR. General dentists and special needs patients: does dental education matter? J Dent Educ. 2005;69:1107–15.
DeMattei R, Cuvo A, Maurizio S. Oral assessment of children with an autism spectrum disorder. J Dent Hyg. 2007;81:65.
Dias GG, Prado EF, Vadasz E, Siqueira JT. Evaluation of the efficacy of a dental plaque control program in autistic patients. J Autism Dev Disord. 2010;40:704–8.
El Khatib AA, El Tekeya MM, El Tantawi MA, Omar T. Oral health status and behaviours of children with autism spectrum disorder: a case-control study. Int J Paediatr Dent. 2014;24:314–23.
Fahlvik-Planefeldt C, Herrstrom P. Dental care of autistic children within the non-specialized Public Dental Service. Swed Dent J. 2001;25:113–8.
Harris R, Nicoll AD, Adair PM, Pine CM. Risk factors for dental caries in young children: a systematic review of the literature. Community Dent Health. 2004;21:71–85.
Huew R, Waterhouse PJ, Moynihan PJ, Maguire A. Prevalence and severity of dental caries in Libyan school children. Int Dent J. 2011;61:217–23.
Inglehart M, Ramaswami N, Feigal R. Pediatric dentists and autistic patients—who treats how. J Dent Res. 2004;83:1497.
Jaber MA. Dental caries experience, oral health status and treatment needs of dental patients with autism. J Appl Oral Sci. 2011;19:212–7.
Klein U, Nowak AJ. Autistic disorder: a review for the pediatric dentist. Pediatr Dent. 1998;20:312–7.
Loo CY, Graham RM, Hughes CV. The caries experience and behavior of dental patients with autism spectrum disorder. J Am Dent Assoc. 2008;139:1518–24.
Loo CY, Graham RM, Hughes CV. Behaviour guidance in dental treatment of patients with autism spectrum disorder. Int J Paediatr Dent. 2009;19:390–8.
Lord C, Risi S, Dilavore PS, et al. Autism from 2 to 9 years of age. Arch Gen Psychiatry. 2006;63:694–701.
Lowe O, Lindemann R. Assessment of the autistic patient’s dental needs and ability to undergo dental examination. ASDC J Dent Child. 1984;52:29–35.
Marshall CR, Noor A, Vincent JB, et al. Structural variation of chromosomes in autism spectrum disorder. Am J Hum Genet. 2008;82:477–88.
Marshall J, Sheller B, Mancl L. Caries-risk assessment and caries status of children with autism. Pediatr Dent. 2010;32:69–75.
Newbrun E. Preventing dental caries: current and prospective strategies. J Am Dent Assoc. 1992;123:68–73.
Rekha CV, Arangannal P, Shahed H. Oral health status of children with autistic disorder in Chennai. Eur Arch Paediatr Dent. 2012;13:126–31.
Shapira J, Mann J, Tamari I, et al. Oral health status and dental needs of an autistic population of children and young adults. Spec Care Dent. 1989;9:38–41.
Stein LI, Polido JC, Cermak SA. Oral care and sensory over-responsivity in children with autism spectrum disorders. Pediatr Dent. 2013;35:230–5.
Stein LI, Polido JC, Mailloux Z, Coleman GG, Cermak SA. Oral care and sensory sensitivities in children with autism spectrum disorders. Spec Care Dent: Off Publ Am Assoc Hosp Dent Acad Dent Handicap Am Soc Geriatr Dent. 2011;31:102–10.
Udhya J, Varadharaja M, Parthiban J. Autism disorder (AD): an updated review for paediatric dentists. J Clin Diagn Res. 2014;8:275.
Vajawat M, Deepika PC. Comparative evaluation of oral hygiene practices and oral health status in autistic and normal individuals. J Int Soc Prev Community Dent. 2012;2:58–63.
Weil TN, Bagramian RA, Inglehart MR. Treating patients with autism spectrum disorder—SCDA members’ attitudes and behavior. Spec Care Dent. 2011;31:8–17.
Weil TN, Inglehart MR. Dental education and dentists’ attitudes and behavior concerning patients with autism. J Dent Educ. 2010;74:1294–307.
WHO. Oral health surveys: basic methods. Geneva: World Health Organization; 1997.
Wolff AJ, Waldman HB, Milano M, Perlman SP. Dental students’ experiences with and attitudes toward people with mental retardation. J Am Dent Assoc. 2004;135:353–7.
Zeglam AM, Maound AJ. Prevalence of autistic spectrum disorders in Tripoli, Libya: the need for more research and planned services. East Mediterr Health J. 2012;18:184–8.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Fakroon, S., Arheiam, A. & Omar, S. Dental caries experience and periodontal treatment needs of children with autistic spectrum disorder. Eur Arch Paediatr Dent 16, 205–209 (2015). https://doi.org/10.1007/s40368-014-0156-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40368-014-0156-6