Abstract
Objectives
The primary objective of this study was to estimate the health utility values for hypoglycaemia events according to their severity and frequency. The secondary objective was to compare the health utilities between those with Type 2 Diabetes Mellitus and the general population.
Method
The health utilities of hypoglycaemia event were measured using Visual Analogue Scale (VAS) and Time Trade-Off (TTO) methods among conveniently sampled consenting adults (>18 years and literate in either English or Malay language), which were then divided into two groups: those in the general population (GP) and those with Type 2 Diabetes Mellitus (T2DM). Each respondent was required to value 13 different health states, including frequencies of daytime hypoglycaemia and nocturnal hypoglycaemia, each depending on its severity (non-severe or severe).
Results
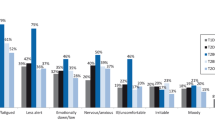
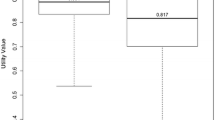
256 respondents from the GP and 99 respondents with T2DM completed the survey. The T2DM group gave higher VAS-values compared to the GP group. The highest mean VAS-utility value for non-severe nocturnal hypoglycaemia occurring once monthly was 0.543 (SD 0.161), and for severe daytime hypoglycaemia occurring once quarterly was 0.293 (SD 0.162) which was the lowest utility value compared to other health states. However, non-severe nocturnal hypoglycaemia occurring once quarterly was 0.537 (SD 0.284) and has the highest TTO-utility value. Severe nocturnal hypoglycaemia occurring once quarterly has the lowest utility value which was −0.104 (SD 0.380). Daytime hypoglycaemia has lower utility value compared to nocturnal hypoglycaemia. Severe hypoglycaemia has a greater disutility compared with the non-severe hypoglycaemia in both studied groups.
Conclusion
The findings show that as a health utility, hypoglycaemia has a substantial impact on utility with severe hypoglycaemia having a greater negative impact compared to non-severe events across the board. This highlights the importance of preventing development of severe hypoglycaemia in patients with Type 2 Diabetes Mellitus at any time of the day.


Similar content being viewed by others
References
Diagnosis ADA. Classification of diabetes mellitus. Diabetes Care. 2010;33(Suppl 1):S62–S9.
Shafiee G, Mohajeri-Tehrani M, Pajouhi M, Larijani B. The importance of hypoglycemia in diabetic patients. Journal of Diabetes & Metabolic Disorders. 2012;11(1):17.
Green AJ, Fox KM, Grandy S. Self-reported hypoglycemia and impact on quality of life and depression among adults with type 2 diabetes mellitus. Diabetes Res Clin Pract. 2012;96(3):313–8.
Amiel SA, Dixon T, Mann R, Jameson K. Hypoglycaemia in type 2 diabetes. Diabet Med. 2008;25(3):245–54.
Krinsley JS, Keegan MT. Hypoglycemia in the critically ill: how low is too low? Mayo Clin Proc. 2010;85(3):215–6.
Shafie AA, Ng CH, Tan YP, Chaiyakunapruk N. Systematic review of the cost effectiveness of insulin analogues in type 1 and type 2 diabetes mellitus. PharmacoEconomics. 2017;35(2):141–62.
Torrance GW, Furlong W, Feeny D. Health utility estimation. Expert Review of Pharmacoeconomics & Outcomes Research. 2002;2(2):99–108.
Whitehead SJ, Ali S. Health outcomes in economic evaluation: the QALY and utilities. Br Med Bull. 2010;96(1):5–21.
Burstrom K, Johannesson M, Diderichsen F. A comparison of individual and social time trade-off values for health states in the general population. Health Policy. 2006;76(3):359–70.
Evans M, Khunti K, Mamdani M, Galbo-Jorgensen CB, Gundgaard J, Bogelund M, et al. Health-related quality of life associated with daytime and nocturnal hypoglycaemic events: a time trade-off survey in five countries. Health Qual Life Outcomes. 2013;11:90.
Harris S, Mamdani M, Galbo-Jorgensen CB, Bogelund M, Gundgaard J, Groleau D. The effect of hypoglycemia on health-related quality of life: Canadian results from a multinational time trade-off survey. Can J Diabetes. 2014;38(1):45–52.
Zhang P, Brown MB, Bilik D, Ackermann RT, Li R, Herman WH. Health utility scores for people with type 2 diabetes in U.S. managed care health plans: results from translating research into action for diabetes (TRIAD). Diabetes Care. 2012;35(11):2250–6.
Aziz AMA, Manan MM, Bahri S, Yusof FABM, Kamarruddin ZB. Said Sb, et al. In: Drug utilization in the treatment of diabetes mellitus in the Ministry of Health facilities.: pharmaceutical services division Ministry of Health Malaysia; 2013.
Garcia AA, Villagomez ET, Brown SA, Kouzekanani K, Hanis CL. The Starr County diabetes education study: development of the Spanish-language diabetes knowledge questionnaire. Diabetes Care. 2001;24(1):16–21.
Arora S, Marzec K, Gates C, Menchine M. Diabetes knowledge in predominantly Latino patients and family caregivers in an urban emergency department. Ethnicity & disease. 2011;21(1):1–6.
Shrestha N, Yadav SB, Joshi AM, Patel BDP, Shrestha J, Diabetes Knowledge DLB. Associated factors among diabetes patients in Central Nepal. International Journal of Collaborative Research on Internal Medicine & Public Health. 2015;7(5):82–91.
Bahia L, Kupfer R, Momesso D, Cabral DAP, Tschiedel B, Puñales M, et al. Health-related quality of life and utility values associated to hypoglycemia in patients with type 1 diabetes mellitus treated in the Brazilian public health system: a multicenter study. Diabetology & Metabolic Syndrome. 2017;9:9.
Johnson JA, Luo N, Shaw JW, Kind P, Coons SJ. Valuations of EQ-5D health states: are the United States and United Kingdom different? Med Care. 2005;43(3):221–8.
Allen KV, Frier BM. Nocturnal hypoglycemia: clinical manifestations and therapeutic strategies toward prevention. Endocrine practice : official journal of the American College of Endocrinology and the American Association of Clinical Endocrinologists. 2003;9(6):530–43.
Sackett DL, Torrance GW. The utility of different health states as perceived by the general public. J Chronic Dis. 1978;31(11):697–704.
Najman JM, Levine S. Evaluating the impact of medical care and technologies on the quality of life: a review and a critique. Social science & medicine (1982). 1981;15f(2–3):107–15.
Acknowledgements
We would like to thank the Director General of Health, Malaysia for his permission to publish this article and Annushiah Vasan who have helped in the mock interview and as the supervisor assessing the interviewers. Concurrently, we would like to thank Wilsom Darius, Nurfila Sharifud-Din Fatin Nabilah, Thesigan A/L Balakrishnan, Tham Shu Ni, Low Xian Wei, Nurul Ainatul Liyana Hj Mohtadzar, Ceciwani Sagathevan, Kalai Divvya A/P Ramasamy, Lee Mei Siew, Najihah Mohd Nasir, Liew Jin Sian, Looi Yi Chien, Nadia Najiha, Muhammad Arif, Nurlisya Rafiha, Low Khai Hang, Nur Adlina, Syazlin Syahira, Nuru Ain, Norfarahani, Siti Nur Najihah, Nur Adila, Sorfina, and Muhammad Hafiz from the School of Pharmaceutical Sciences, Universiti Sains Malaysia Penang who were involved in the process of completing this research.
Declaration of funding
This study was supported by an unrestricted grant from Ministry of Health Malaysia Research Grant (00794).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
Asrul A Shafie has previously provided writing assistance to Novo Nordisk. However, this study did not receive any sponsorship from Novo Nordisk. Chin Hui Ng, Subramaniam Thanimalai, Norliza Haron, and Anita Bhajan Manocha declared no conflict of interest.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Shafie, A.A., Ng, C.H., Thanimalai, S. et al. Estimating the utility value of hypoglycaemia according to severity and frequency using the visual analogue scale (VAS) and time trade-off (TTO) survey. J Diabetes Metab Disord 17, 269–275 (2018). https://doi.org/10.1007/s40200-018-0369-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40200-018-0369-z