Abstract
Purpose
Heart rate variability biofeedback (HRV-BF) is an effective psychophysiological intervention, with short-term effects of increased autonomic nervous system homeostasis, strengthened baroreflex sensitivity, and decreased hostility in patients with coronary artery disease (CAD). The study examined the 1-year HRV-BF effect on cardiovascular prognosis of these patients.
Methods
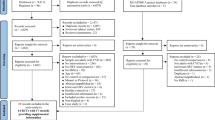
Of 222 patients with CAD referred by cardiologists, 210 were screened and randomly assigned to the HRV-BF and control groups. All patients received psychophysiological assessment and completed psychological questionnaires at pre- and post-interventions and 1-year follow-up. The cardiovascular prognosis primary endpoints included hospital readmission, emergency revisits, and mortality.
Results
The HRV-BF group had fewer all-cause readmissions (12.00 vs. 25.42%) and all-cause emergency visits (13.33 vs. 35.59%) than the control group. The low-frequency HRV in the HRV-BF group increased at post-intervention and 1-year follow-up compared with that at pre-intervention. Although no significant interaction effect was found in the standard deviation of the normal-to-normal intervals (F = 2.96, p = 0.055), it increased by 26.68% from pre- to post-intervention and 15.77% from pre-intervention to follow-up in the HRV-BF group. However, it decreased by 3.60% from pre- to post-intervention and increased by 1.99% from pre-intervention to follow-up in the control group. Depression and hostility scores decreased significantly at post-intervention and 1-year follow-up only in the HRV-BF group.
Conclusions
The long-term HRV-BF effect was confirmed by improved cardiovascular prognosis, increased cardiac autonomic homeostasis and baroreflex sensitivity, and decreased depression and hostility. HRV-BF is an effective psychophysiological intervention with short- and long-term effects in cardiac rehabilitation programs.


Similar content being viewed by others
References
Cowan MJ, Pike KC, Budzynski HK. Psychosocial nursing therapy following sudden cardiac arrest: impact on two-year survival. Nurs Res. 2001;50(2):68–76. https://doi.org/10.1097/00006199-200103000-00002.
Del Pozo JM, Gevirtz RN, Scher B, Guarneri E. Biofeedback treatment increases heart rate variability in patients with known coronary artery disease. Am Heart J. 2004;147(3):545 G1–6. https://doi.org/10.1016/j.ahj.2003.08.013.
Lin IM, Fan SY, HC L, Lin TH, Chu CS, Kuo HF, et al. Randomized controlled trial of heart rate variability biofeedback in cardiac autonomic and hostility among patients with coronary artery disease. Behav Res Ther. 2015;70:38–46. https://doi.org/10.1016/j.brat.2015.05.001.
Cossette S, Frasure-Smith N, Lespérance F. Clinical implications of a reduction in psychological distress on cardiac prognosis in patients participating in a psychosocial intervention program. Psychosom Med. 2001;63(2):257–66. https://doi.org/10.1097/00006842-200103000-00009.
Linden W, Phillips MJ, Leclerc J. Psychological treatment of cardiac patients: a meta-analysis. Eur Heart J. 2007;28(24):2972–84. https://doi.org/10.1093/eurheartj/ehm504.
Roncella A, Pristipino C, Cianfrocca C, Scorza S, Pasceri V, Pelliccia F, et al. One-year results of the randomized, controlled, short-term psychotherapy in acute myocardial infarction (STEP-IN-AMI) trial. Int J Cardiol. 2013;170(2):132–9. https://doi.org/10.1016/j.ijcard.2013.08.094.
Whalley B, Rees K, Davies P, Bennett P, Ebrahim S, Liu Z, et al. Psychological interventions for coronary heart disease. Cochrane Database Syst Rev. 2011;8:CD002902. https://doi.org/10.1002/14651858.
Lehrer P, Vaschillo E, Vaschillo B. Resonant frequency biofeedback training to increase cardiac variability: rationale and manual for training. Appl Psychophysiol Biofeedback. 2000;25(3):177–91. https://doi.org/10.1023/A:1009554825745.
Wheat A, Larkin K. Biofeedback of heart rate variability and related physiology: a critical review. Appl Psychophysiol Biofeedback. 2010;35(3):229–42. https://doi.org/10.1007/s10484-010-9133-y.
Swanson K, Gevirtz R, Brown M, Spira J, Guarneri E, Stoletniy L. The effect of biofeedback on function in patients with heart failure. Appl Psychophysiol Biofeedback. 2009;34(2):71–91. https://doi.org/10.1007/s10484-009-9077-2.
Lehrer P, Vaschillo E, Vaschillo B, Lu SE, Scardella A, Siddique M, et al. Biofeedback treatment for asthma. Chest. 2004;126(2):352–61. https://doi.org/10.1378/chest.126.2.352.
Karavidas MK, Lehrer P, Vaschillo E, Vaschillo B, Marin H, Buyske S, et al. Preliminary results of an open label study of heart rate variability biofeedback for the treatment of major depression. Appl Psychophysiol Biofeedback. 2007;32(1):19–30. https://doi.org/10.1007/s10484-006-9029-z.
Zucker TL, Samuelson KW, Muench F, Greenberg MA, Gevirtz RN. The effects of respiratory sinus arrhythmia biofeedback on heart rate variability and posttraumatic stress disorder symptoms: a pilot study. Appl Psychophysiol Biofeedback. 2009;34(2):135–43. https://doi.org/10.1007/s10484-009-9085-2.
Lehrer P, Vaschillo E, Vaschillo B, Lu SE, Eckberg DL, Edelberg R, et al. Heart rate variability biofeedback increases baroreflex gain and peak expiratory flow. Psychosom Med. 2003;65(5):796–805. https://doi.org/10.1097/01.PSY.0000089200.81962.19.
Lehrer P, Gevirtz R. Heart rate variability biofeedback: how and why does it work? Front Psychol. 2014;5(756):1–9. https://doi.org/10.3389/fpsyg.2014.00756.
Faul F, Erdfelder E, Lang A, Buchner A. G*Power 3: a flexible statistical power analysis program for the social, behavioral, and biomedical sciences. Behav Res Methods. 2007;39(2):175–91. https://doi.org/10.3758/BF03193146.
Beck AT, Steer RA, Brown GK. Beck Depression Inventory manual. 2nd ed. San Antonio, TX: Psychological Corporation; 1996.
Weng C-Y, Lin IM, Lue BH, Chen HJ, Wu YC, Cheng YR. Development and psychometric properties of the Chinese Hostility Inventory-short form. Psychological Testing. 2008;55(3):463–86.
Huikuri H, Stein P. Heart rate variability in risk stratification of cardiac patients. Prog Cardiovasc Dis. 2013;56(2):153–9. https://doi.org/10.1016/j.pcad.2013.07.003.
Carney RM, Blumenthal JA, Stein PK, Watkins L, Catellier D, Berkman LF, et al. Depression, heart rate variability, and acute myocardial infarction. Circulation. 2001;104(17):2024–8. https://doi.org/10.1161/hc4201.097834.
Frasure-Smith N, Lespérance F, Gravel G, Masson A, Juneau M, Talajic M, et al. Social support, depression, and mortality during the first year after myocardial infarction. Circulation. 2000;101(16):1919–24. https://doi.org/10.1161/01.CIR.101.16.1919.
Sloan RP, Shapiro PA, Gorenstein EE, Tager FA, Monk CE, McKinley PS, et al. Cardiac autonomic control and treatment of hostility: a randomized controlled trial. Psychosom Med. 2010;72(1):1–8. https://doi.org/10.1097/PSY.0b013e3181c8a529.
Hajjari P, Mattsson S, McIntyre K, McKinley P, Shapiro P, EE G, et al. The effect of hostility reduction on autonomic control of the heart and vasculature: a randomized controlled trial. Psychosom Med. 2016;78(4):481–91. https://doi.org/10.1097/PSY.0000000000000296.
Laborde S, Mosley E, Thayer JF. Heart rate variability and cardiac vagal tone in psychophysiological research–recommendations for experiment planning, data analysis, and data reporting. Front Psychol. 2017;8:213. https://doi.org/10.3389/fpsyg.2017.00213.
Draghici A, Taylor A. The physiological basis and measurement of heart rate variability in humans. J Physiol Anthropol. 2016;35(1):22. https://doi.org/10.1186/s40101-016-0113-7.
Thayer JF, Lane RD. A model of neurovisceral integration in emotion regulation and dysregulation. J Affect Disord. 2000;61(3):201–16. https://doi.org/10.1016/S0165-0327(00)00338-4.
Lehrer P, Vaschillo B, Zucker T, Graves J, Katsamanis M, Aviles M, et al. Protocol for heart rate variability biofeedback training. Biofeedback. 2013;41(3):98–109. https://doi.org/10.5298/1081-5937-41.3.08.
Thayer JF, Åhs F, Fredrikson MA, Sollers JJ, Wager TD. A meta-analysis of heart rate variability and neuroimaging studies: implications for heart rate variability as a marker of stress and health. Neurosci Biobehav Rev. 2012;36(2):747–56. https://doi.org/10.1016/j.neubiorev.2011.11.009.
Shaffer F, McCraty R, Zerr CL. A healthy heart is not a metronome: an integrative review of the heart’s anatomy and heart rate variability. Front Psychol. 2014;5:1–19. https://doi.org/10.3389/fpsyg.2014.01040.
Moss D, Shaffer F. The application of heart rate variability biofeedback to medical and mental health disorders. Biofeedback. 2017;45(1):2–8. https://doi.org/10.5298/1081-5937-45.1.03.
Acknowledgements
This research was supported by Ministry of Science and Technology, Taiwan (grant number: MOST 103-2410-H-037-005). We would like to thank Professor Pei-Shian Ho for statistical consultations, and cardiologists Dr. Chee-Siong Lee, Dr. Ye-Hsu Lu, Dr. Chih-Sheng Chu, and Dr. Hsuan-Fu Kuo for referring patients to participate this study. We would especially thank student assistants Hsiang-Tzu Huang and Pei-Yun Lin for data collection, and Editage (https://www.editage.com.tw/) for English language editing.
Funding
This study was funded by the Ministry of Science and Technology, Taiwan (grant number: MOST 103-2410-H-037-005).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of Interest
I-Mei Lin has received research grant from the Ministry of Science and Technology. The authors declare that they have no conflict of interest.
Human and Animals Rights and Informed Consent
All procedures followed were in accordance with ethical standards of the responsible committee on human experimentation (intuitional and national) and with the Helsinki Declaration of 1975, as revised in 2000. Informed consent was obtained from all patients for being included in the study.
Rights and permissions
About this article
Cite this article
Yu, LC., Lin, IM., Fan, SY. et al. One-Year Cardiovascular Prognosis of the Randomized, Controlled, Short-Term Heart Rate Variability Biofeedback Among Patients with Coronary Artery Disease. Int.J. Behav. Med. 25, 271–282 (2018). https://doi.org/10.1007/s12529-017-9707-7
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12529-017-9707-7