Abstract
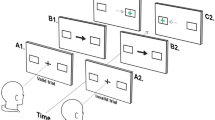
Friedreich ataxia (FRDA) is the most common genetic cause of ataxia with a prevalence of approximately 1 in 29,000. Ocular motor abnormalities are common in FRDA and include fixation instability, saccadic dysmetria, and vestibular dysfunction. It has not yet been determined whether aspects of spatial attention, which are closely coupled to eye movements, are similarly compromised in FRDA. This study examined attentional engagement and disengagement of eye movements in FRDA using a gap overlap task. Thirteen individuals with genetically confirmed FRDA and 12 age-matched unaffected controls participated in the experiment. The gap overlap paradigm was used to examine the effect of early (gap condition), simultaneous (null condition), or late (overlap condition) removal of a central fixation on saccadic latency to a peripheral target stimulus. Although the FRDA group showed a larger gap effect (i.e., difference in saccadic latencies between the overlap and gap condition), these participants demonstrated a greater difference in latencies in the overlap relative to the null condition, suggestive of deficits within the disengagement process of attentional orienting. We propose a role for the cerebellum in these deficits in the disengagement of spatial attention based on evidence of cerebellar connectivity with regions involved in exogenous shifts of attention. The significant correlations between saccadic latency and disease severity as measured by the Friedreich Ataxia Rating Scale further support the proposal that saccadic latency might be useful as a surrogate marker of disease severity and progression in future clinical trials in FRDA.

Similar content being viewed by others
References
Delatycki M, Williamson R, Forrest S. Friedreich ataxia: an overview. J Med Genet. 2000;37:1–8.
Voncken M, Ionnou P, Delatycki M. Friedreich ataxia: update on pathogenesis and possible therapies. Neurogenetics. 2004;5:1–8.
Campuzano V, Montermini L, Moltò MD, Pianese L, Cossée M, Cavalcanti F, et al. Friedreich's ataxia: autosomal recessive disease caused by an intronic GAA triplet repeat expansion. Science. 1996;271:1374–5.
Lynch DR, Farmer JM, Balcer LJ, Wilson RB. Friedreich ataxia: effects of genetic understanding on clinical evaluation and therapy. Arch Neurol. 2002;59(5):743–7.
Pandolfo M. Friedreich ataxia. Semin Pediatr Neurol. 2003;10:163–72.
Della Nave R, Ginestroni A, Giannelli M, Tessa C, Salvatore E, Salvi F, et al. Brain structural damage in Friedreich's ataxia. J Neurol Neurosurg Psychiatry. 2008;79(1):82–5.
Delatycki MB. Evaluating the progression of Friedreich ataxia and its treatment. J Neurol. 2009;256 Suppl 1:36–41.
Furman J, Perlman S, Baloh R. Eye movements in Friedreich's ataxia. Arch Neurol. 1983;40:434–6.
Klockgether T, Zuhlke C, Schulz JB, Burk K, Fetter M, Dittmann H, et al. Friedreich's ataxia with retained tendon reflexes: molecular genetics, clinical neurophysiology, and magnetic resonance imaging. Neurology. 1996;46:118–21.
Spieker S, Schulz JB, Petersen D, Fetter M, Klockgether T, Dichgans J. Fixation instability and oculomotor abnormalities in Friedreich's ataxia. J Neurol. 1995;242:517–21.
Fahey MC, Cremer PD, Aw ST, Millist L, Todd MJ, White OB, et al. Vestibular, saccadic and fixation abnormalities in genetically confirmed Friedreich ataxia. Brain. 2008;131(Pt 4):1035–45.
Corben LA, Georgiou-Karistianis N, Fahey M, Storey E, Churchyard A, Horne M, et al. Towards an understanding of cognitive function in Friedreich Ataxia. Brain Res Bull. 2006;70(3):197–202.
Fielding J, Corben L, Cremer P, Millist L, White O, Delatycki M. Disruption to higher order processes in Friedreich ataxia. Neuropsychologia. 2010;48(1):235–42.
Botez-Marquard T, Botez M. Cognitive behavior in heredodegenerative ataxias. Eur Neurol. 1993;33:351–7.
Botez-Marquard T, Botez M. Olivopontocerebellar atrophy and Friedreich's ataxia: neuropsychological consequences of bilateral versus unilateral cerebellar lesions. Int Rev Neurobiol. 1997;41:387–410.
Hart R, Henry G, Kwentus J, Leshner R. Information processing speed of children with Friedreich’s ataxia. Dev Med Child Neurol. 1986;28:310–3.
Hart R, Kwentus J, Leshner R, Frazier R. Information processing speed in Friedreich’s ataxia. Ann Neurol. 1985;17:612–4.
White, Lalonde R, Botez-Marquard T. Neuropsychologic and neuropsychiatric characteristics of patients with Friedreich's ataxia. J Clin Exp Neuropsychol. 2000;24:677–86.
Wollmann T, Barroso J, Monton F, Nieto A. Neuropsychological test performance of patients with Friedreich's ataxia. J Clin Exp Neuropsychol. 2002;24:677–86.
Mantovan M, Martinuzzi A, Squarzanti F, Bolla A, Silvestri I, Liessi G, et al. Exploring mental status in Friedreich's ataxia: a combined neuropsychological, behavioral and neuroimaging study. Eur J Neurol. 2006;13:827–35.
Corben LA, Delatycki MB, Bradshaw JL, Horne MK, Fahey MC, Churchyard AC, et al. Impairment in motor reprogramming in Friedreich ataxia reflecting possible cerebellar dysfunction. J Neurol. 2009. doi:10.1007/s00415-009-5410-1.
Strick PL, Dum RP, Fiez JA. Cerebellum and nonmotor function. Annu Rev Neurosci. 2009;32:413–34.
Baillieux H, De Smet H, Paquier F, De Deyn P, Marien P. Cerebellar neurocognition: insights into the bottom of the brain. Clin Neurol Neurosurg. 2008;110:763–73.
Botez-Marquard T, Bard C, Leveille J, Botez M. A severe frontal-parietal lobe syndrome following cerebellar damage. Eur J Neurol. 2001;8:347–53.
Grafman J, Litvan I, Massaquoi SG, Stewart M, Sirigu A, Hallet M. Cognitive planning deficit in patients with cerebellar atrophy. Neurology. 1992;42:1493–6.
Schmahmann J. An emerging concept. The cerebellar contribution to higher function. Arch Neurol. 1991;48:1178–87.
Schmahmann J, Pandya D. Prefrontal cortex projections to the basilar pons in rhesus monkey: implications for the cerebellar contribution to higher function. Neurosci Lett. 1995;199:175–8.
Schmahmann J, Pandya D. The cerebrocerebellar system. Int Rev Neurobiol. 1997;41:31–60.
Schmahmann J, Sherman J. The cerebellar cognitive affective syndrome. Brain. 1998;121:561–79.
Akshoomoff NA, Courchesne E. A new role for the cerebellum in cognitive operations. Behav Neurosci. 1992;106(5):731–8.
Courchesne E, Townsend J, Akshoomoff NA, Saitoh O, Yeung-Courchesne R, Lincoln AJ, et al. Impairment in shifting attention in autistic and cerebellar patients. Behav Neurosci. 1994;108(5):848–65.
Prevosto V, Graf W, Ugolini G. Cerebellar inputs to intraparietal cortex areas LIP and MIP: functional frameworks for adaptive control of eye movements, reaching, and arm/eye/head movement coordination. Cereb Cortex. 2010;20(1):214–28.
May PJ, Hartwich-Young R, Nelson J, Porter JD. Cerebellotectal pathways in the macaque: implications for collicular generation of saccades. Neuroscience. 1990;36:305–24.
Kustov AA, Robinson DL. Shared neural control of attentional shifts and eye movements. Nature. 1996;384(6604):74–7.
Munoz DP, Fecteau JH. Vying for dominance: dynamic interactions control visual fixation and saccadic initiation in the superior colliculus. Prog Brain Res. 2002;140:3–19.
Fischer B, Weber H. Express saccades and visual attention. Behav Brain Sci. 1993;16:553–610.
Aw ST, Haslwanter T, Halmagyi GM, Curthoys IS, Yavor RA, Todd MJ. Three-dimensional vector analysis of the human vestibulo-ocular reflex in response to high-acceleration head rotations. I. Responses in normal subjects. J Neurophysiol. 1996;76:4009–20.
Cremer PD, Halmagyi GM, Aw ST, Curthoys IS, McGarvie LA, Todd MJ, et al. Semicircular canal plane head impulses detect absent function of individual semicircular canals. Brain. 1998;121:699–716.
Robinson DA. A method of measuring eye movement using a scleral coil in a magnetic field. IEEE Trans Biomed Electron. 1963;10:137–45.
Subramony S, May W, Lynch D, Gomez C, Fischbeck K, Hallet M, et al. Measuring Friedreich ataxia: interrater reliability of a neurologic rating scale. Neurology. 2005;64:1261–2.
Lynch D, Farmer J, Tsou A, Perlman S, Subramony S, Gomez C, et al. Measuring Friedreich ataxia: complementary features of examination and performance measures. Neurology. 2006;66:1711–6.
Courchesne E. Prediction and preparation, fundamental functions of the cerebellum. Learn Mem. 1997;4:1–35.
Ghajar J, Ivry I. The predictive brain state: asynchrony in disorders of attention? Neuroscientist. 2009;15(3):232–42.
Akshoomoff NA, Courchesne E, Townsend J. Attention coordination and anticipatory control. Int Rev Neurobiol. 1997;41:575–98.
Dum R, Strick P. An unfolded map of the cerebellar dentate nucleus and its projections to the cerebral cortex. J Neurophysiol. 2003;89:634–9.
Goldberg ME, Bisley JW, Powell KD, Gottlieb J. Saccades, salience and attention: the role of the lateral intraparietal area in visual behavior. Prog Brain Res. 2006;155:157–75.
Ferraina S, Paré M, Wurtz RH. Comparison of cortico-cortical and cortico-collicular signals for the generation of saccadic eye movements. J Neurophysiol. 2002;87(2):845–58.
Rizzolatti G, Riggio L, Dascola I, Umiltá C. Reorienting attention across the horizontal and vertical meridians: evidence in favor of a premotor theory of attention. Neuropsychologia. 1987;25(1A):31–40.
Acknowledgements
We thank the participants, who willingly gave their time and continue to support our research. This research was supported by the National Health and Medical Research Council Australia (JF #454811, MBD #546452), the Friedreich Ataxia Research Association, Australasia, and the Friedreich Ataxia Research Alliance, USA.
Conflict of interest
The authors declare no conflict of interest with respect to this article.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Hocking, D.R., Fielding, J., Corben, L.A. et al. Ocular Motor Fixation Deficits in Friedreich Ataxia. Cerebellum 9, 411–418 (2010). https://doi.org/10.1007/s12311-010-0178-5
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12311-010-0178-5