Abstract
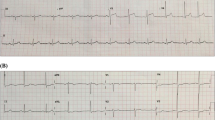
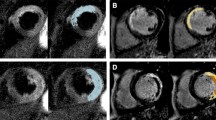
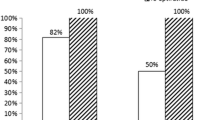
Patients with chest pain and a prehospital ST-segment elevation myocardial infarction (STEMI) are preferably treated with immediate percutaneous coronary intervention (PCI). However, patients with normalization of symptoms and ST-segment elevation upon hospital arrival (transient STEMI) received inconsistent therapy due to logistic reasons and the absence of evidence or explicit guidelines. In this trial, the optimal timing of coronary angiography and subsequent revascularisation is investigated in patients presenting with transient STEMI. In this prospective, multicentre, randomized controlled clinical trial, 142 consecutive patients with initially acute chest pain and STEMI, whose symptoms and ST-segment elevation resolve upon admission, are randomized to immediate intervention or a delayed intervention. Primary outcome is infarct size measured at 4 days determined by cardiovascular magnetic resonance. Secondary outcomes are left ventricular function and volumes, myocardial salvage and microvascular injury at baseline; the change in left ventricular function, volumes and infarct size at 4 months; and major adverse cardiac events at 4 and 12 months. The TRANSIENT Trial evaluates whether a delayed invasive strategy (according to NSTEMI-guidelines) is superior to an immediate invasive strategy (according to STEMI-guidelines) in patients with a transient STEMI.


Similar content being viewed by others
References
Keeley, E. C., Boura, J. A., & Grines, C. L. (2003). Primary angioplasty versus intravenous thrombolytic therapy for acute myocardial infarction: a quantitative review of 23 randomised trials. Lancet, 361, 13–20.
Nallamothu, B. K., Bradley, E. H., & Krumholz, H. M. (2007). Time to treatment in primary percutaneous coronary intervention. New England Journal of Medicine, 357, 1631–1638.
O’Gara, P. T., Kushner, F. G., Ascheim, D. D., et al. (2013). 2013 ACCF/AHA guideline for the management of ST-elevation myocardial infarction: a report of the American College of Cardiology Foundation/American Heart Association Task Force on Practice Guidelines. Journal of the American College of Cardiology, 61, e78–e140.
Steg, P. G., James, S. K., Atar, D., et al. (2012). ESC Guidelines for the management of acute myocardial infarction in patients presenting with ST-segment elevation. European Heart Journal, 33, 2569–2619.
Meisel, S. R., Dagan, Y., Blondheim, D. S., et al. (2008). Transient ST-elevation myocardial infarction: clinical course with intense medical therapy and early invasive approach, and comparison with persistent ST-elevation myocardial infarction. American Heart Journal, 155, 848–854.
Chin, C. T., Chen, A. Y., Wang, T. Y., et al. (2011). Risk adjustment for in-hospital mortality of contemporary patients with acute myocardial infarction: the Acute Coronary Treatment and Intervention Outcomes Network (ACTION) Registry®–Get With The Guidelines (GWTG)™ acute myocardial infarction mortality model and risk score. American Heart Journal, 161, 113–122.
Montalescot, G., Cayla, G., Collet, J. P., et al. (2009). Immediate vs delayed intervention for acute coronary syndromes: a randomized clinical trial. JAMA, 302, 947–954.
Mehta, S. R., Granger, C. B., Boden, W. E., et al. (2009). Early versus delayed invasive intervention in acute coronary syndromes. New England Journal of Medicine, 360, 2165–2175.
Damman, P., van, G. N., Wallentin, L., et al. (2012). Timing of angiography with a routine invasive strategy and long-term outcomes in non-ST-segment elevation acute coronary syndrome: a collaborative analysis of individual patient data from the FRISC II (Fragmin and Fast Revascularization During Instability in Coronary Artery Disease), ICTUS (Invasive Versus Conservative Treatment in Unstable Coronary Syndromes), and RITA-3 (Intervention Versus Conservative Treatment Strategy in Patients With Unstable Angina or Non-ST Elevation Myocardial Infarction) Trials. JACC. Cardiovascular Interventions, 5, 191–199.
Meneveau, N., Seronde, M. F., Descotes-Genon, V., et al. (2009). Immediate versus delayed angioplasty in infarct-related arteries with TIMI III flow and ST segment recovery: a matched comparison in acute myocardial infarction patients. Clinical Research in Cardiology, 98, 257–264.
Hamm, C. W., Bassand, J. P., Agewall, S., et al. (2011). ESC Guidelines for the management of acute coronary syndromes in patients presenting without persistent ST-segment elevation: the Task Force for the management of acute coronary syndromes (ACS) in patients presenting without persistent ST-segment elevation of the European Society of Cardiology (ESC). European Heart Journal, 32, 2999–3054.
Jneid, H., Anderson, J. L., Wright, R. S., et al. (2012). 2012 ACCF/AHA focused update of the guideline for the management of patients with unstable angina/Non-ST-elevation myocardial infarction (updating the 2007 guideline and replacing the 2011 focused update): a report of the American College of Cardiology Foundation/American Heart Association Task Force on Practice Guidelines. Circulation, 126, 875–910.
Dall’Armellina, E., Piechnik, S. K., Ferreira, V. M., et al. (2012). Cardiovascular magnetic resonance by non contrast T1-mapping allows assessment of severity of injury in acute myocardial infarction. Journal of Cardiovascular Magnetic Resonance, 14, 15.
Giri, S., Chung, Y. C., Merchant, A., et al. (2009). T2 quantification for improved detection of myocardial edema. Journal of Cardiovascular Magnetic Resonance, 11, 56.
Nijveldt, R., Beek, A. M., Hirsch, A., et al. (2008). Functional recovery after acute myocardial infarction: comparison between angiography, electrocardiography, and cardiovascular magnetic resonance measures of microvascular injury. Journal of the American College of Cardiology, 52, 181–189.
Ortiz-Perez, J. T., Meyers, S. N., Lee, D. C., et al. (2007). Angiographic estimates of myocardium at risk during acute myocardial infarction: validation study using cardiac magnetic resonance imaging. European Heart Journal, 28, 1750–1758.
Rao, A. K., Pratt, C., Berke, A., et al. (1988). Thrombolysis in Myocardial Infarction (TIMI) Trial—phase I: hemorrhagic manifestations and changes in plasma fibrinogen and the fibrinolytic system in patients treated with recombinant tissue plasminogen activator and streptokinase. Journal of the American College of Cardiology, 11, 1–11.
Thygesen, K., Alpert, J. S., Jaffe, A. S., et al. (2012). Third universal definition of myocardial infarction. European Heart Journal, 33, 2551–2567.
Moussa, I. D., Klein, L. W., Shah, B., et al. (2013). Consideration of a new definition of clinically relevant myocardial infarction after coronary revascularization: an expert consensus document from the Society for Cardiovascular Angiography and Interventions (SCAI). Journal of the American College of Cardiology, 62, 1563–1570.
Xu, J., Song, Y. B., Hahn, J. Y., et al. (2012). Comparison of magnetic resonance imaging findings in non-ST-segment elevation versus ST-segment elevation myocardial infarction patients undergoing early invasive intervention. International Journal of Cardiovascular Imaging, 28, 1487–1497.
Lindsell, C. J., Anantharaman, V., Diercks, D., et al. (2006). The Internet Tracking Registry of Acute Coronary Syndromes (i*trACS): a multicenter registry of patients with suspicion of acute coronary syndromes reported using the standardized reporting guidelines for emergency department chest pain studies. Annals of Emergency Medicine, 48, 666–677. 677.
Stone, G. W., Cox, D., Garcia, E., et al. (2001). Normal flow (TIMI-3) before mechanical reperfusion therapy is an independent determinant of survival in acute myocardial infarction: analysis from the primary angioplasty in myocardial infarction trials. Circulation, 104, 636–641.
Riezebos, R. K., Ronner, E., Ter Bals, E., et al. (2009). Immediate versus deferred coronary angioplasty in non-ST-segment elevation acute coronary syndromes. Heart, 95, 807–812.
Gersh, B. J., & Anderson, J. L. (1993). Thrombolysis and myocardial salvage. Results of clinical trials and the animal paradigm—paradoxic or predictable? Circulation, 88, 296–306.
Grines, C. L., Browne, K. F., Marco, J., et al. (1993). A comparison of immediate angioplasty with thrombolytic therapy for acute myocardial infarction. The Primary Angioplasty in Myocardial Infarction Study Group. New England Journal of Medicine, 328, 673–679.
Kim, R. J., Chen, E. L., Lima, J. A., & Judd, R. M. (1996). Myocardial Gd-DTPA kinetics determine MRI contrast enhancement and reflect the extent and severity of myocardial injury after acute reperfused infarction. Circulation, 94, 3318–3326.
Kim, R. J., Fieno, D. S., Parrish, T. B., et al. (1999). Relationship of MRI delayed contrast enhancement to irreversible injury, infarct age, and contractile function. Circulation, 100, 1992–2002.
Pennell, D. J., Sechtem, U. P., Higgins, C. B., et al. (2004). Clinical indications for cardiovascular magnetic resonance (CMR): Consensus Panel report. European Heart Journal, 25, 1940–1965.
Ferreira, V. M., Piechnik, S. K., Dall’Armellina, E., et al. (2012). Non-contrast T1-mapping detects acute myocardial edema with high diagnostic accuracy: a comparison to T2-weighted cardiovascular magnetic resonance. Journal of Cardiovascular Magnetic Resonance, 14, 42.
Robbers, L. F., Eerenberg, E. S., Teunissen, P. F., et al. (2013). Magnetic resonance imaging-defined areas of microvascular obstruction after acute myocardial infarction represent microvascular destruction and haemorrhage. European Heart Journal, 34, 2346–2353.
Financial Support
The study is financially supported by unrestricted grants from Astra-Zeneca and Biotronik.
Trial Registration Number
NTR4156 (www.trialregister.nl)
Author information
Authors and Affiliations
Corresponding author
Additional information
Associate Editor Emanuele Barbato oversaw the review of this article.
Rights and permissions
About this article
Cite this article
Lemkes, J., Nijveldt, R., Beek, A.M. et al. Evaluating the Optimal Timing of Revascularisation in Patients with Transient ST-Segment Elevation Myocardial Infarction: Rationale and Design of the TRANSIENT Trial. J. of Cardiovasc. Trans. Res. 7, 590–596 (2014). https://doi.org/10.1007/s12265-014-9572-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12265-014-9572-6