Abstract
Despite ample evidence for transdiagnostic interventions in clinical populations and in universal prevention approaches, there are only a few controlled trials examining their role for indicated prevention. This study is the first randomized controlled trial to assess the effectiveness of a brief, 8-session group version of the Unified Protocol for Transdiagnostic Treatment of Emotional Disorders in Adolescents (UP-A), called PROCARE-I (Preventive Transdiagnostic Intervention for Adolescents at Risk for Emotional Disorders-Indicated), delivered online, and including a booster session, in reducing symptoms of anxiety and depression in adolescents compared to an active control condition. Sixty-four adolescents (53% identifying as female) with elevated levels of anxiety and/or depression were randomly assigned to either the 8-week PROCARE-I or the active control condition. Self-report, parent, and clinician measures were collected before and after the interventions, at the 6-month follow-up, and 1 month after the booster session. After the intervention, participants in the PROCARE-I group showed improved scores on 9 of the 13 primary and secondary outcome measures, including reduction of anxiety and mood symptomatology, level of risk of developing emotional disorders, resilience, as well as increase of psychological flexibility, and emotional regulation. In contrast, those in the control group showed improvements in only 2 of the 13 outcome measures. After the booster session, significant differences were found between the PROCARE-I and control condition on measures of overall anxiety and depression symptoms, emotional risk, resilience, and quality of life. Low dropout rates and limited incidence of emotional disorders were observed at follow-ups. The interventions were well-accepted, with high satisfaction rates.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Anxiety and depression are common, chronic, and impairing disorders with a first onset often occurring during adolescence and affecting close to a quarter of all adults during their lifetime (Canals-Sans et al., 2018; Polanczyk et al., 2015). An increased number of adolescents suffering from symptoms of anxiety or depression that are just below the clinical threshold has been observed in the wake of the COVID-19 pandemic and its aftermath (e.g., Racine et al., 2021). Both clinical and subclinical levels of anxiety or depression, with a high tendency for co-occurrence, are negatively related to social and family functioning, are associated with poor academic performance, and can even lead to suicide (Balázs et al., 2013; Lewinsohn et al., 2000; Verboom et al., 2014). All of this, together with the rise in depression and anxiety risk during this developmental period, suggests that adolescence seems to be an appropriate age to implement prevention (Solmi et al., 2022).
Early prevention of anxiety and depression in adolescents is a public health priority (Bennett et al., 2015; Garcia-Lopez, 2023; Makover et al., 2019). Indicated prevention programs are developed to target adolescents who already have elevated symptoms of anxiety and/or depression, but the symptoms do not qualify for a clinical diagnosis. Addressing elevated symptoms at an early age is crucial to improve functioning and well-being, and potentially preventing new cases of a clinical disorder (Beardslee et al., 2013). Therefore, indicated prevention may be the key to mitigating adolescents’ high levels of emotional problems before full symptoms evolve (van Starrenburg et al., 2017).
Meta-analytic and review data of indicated prevention programs for emotional problems have shown them to be more promising than universal prevention, i.e., interventions targeting the general population (Bennett et al., 2015; Hugh-Jones et al., 2021; Lawrence et al., 2017; Teubert & Pinquart, 2011). It has also been argued that indicated prevention programs may have the potential to be effective, given the greater potential scope of the change in symptoms (Dodge, 2020; Jiménez-Vázquez et al., in press). However, most of the studies have found relatively small or modest effects in the short term, with many findings dissipating over the long term, which suggests the need for booster sessions to maintain the effects of such indicated programs over time (Rasing et al., 2017; Stockings et al., 2016).
To date, most indicated preventive interventions have focused on either anxiety or depression, despite the high comorbidity of these conditions (Yapan et al., 2022). Interest in transdiagnostic approaches not only for clinical conditions but for the prevention of emotional problems in adolescents has increased in recent years (Vivas-Fernandez, Garcia-Lopez & Jimenez-Vazquez, in press). Transdiagnostic approaches address emotion regulation to reduce emotional symptomatology in anxiety and depression through cognitive behavioral therapy (CBT) strategies (Peris-Baquero et al., 2022). However, data from a meta-analytic review of both depression and anxiety prevention based on CBT for at-risk adolescents suggests that current randomized control trials (RCT) of such indicated prevention programs are scarce and suffer from methodological limitations, with only 16% of the studies including any active control condition (ACC) at all (Bennett et al., 2015; van Doorn et al., 2021). As the use of waitlist control conditions (WLCs) in RCT may overestimate treatment effects and thus artificially inflate the effect sizes of therapies, the inclusion of ACC in RCT is recommended (Faltinsen et al., 2019; Furukawa et al., 2014).
A transdiagnostic treatment with a strong evidence base is the Unified Protocol for Transdiagnostic Treatment of Emotional Disorders in Adolescents (UP-A; Ehrenreich-May et al., 2018). UP-A has the potential to meet all requirements for indicated prevention and has already been proven effective as an intervention treatment program for adolescents with clinical emotional disorders in several studies (for a review, please see Ehrenreich-May & Kennedy, 2021). It has been tested for universal prevention in an open trial and compared to a wait-list control group (García-Escalera et al., 2019, 2020), for selective prevention in a RCT compared to an active control group at 6-month (Vivas-Fernandez et al., 2023) and 12-month follow-up (Vivas-Fernandez et al., in press), as well as for indicated preventive purposes in an initial cluster randomized wait-list-controlled trial (Schmitt et al., 2022). However, this intervention has not been tested in adolescents with elevated anxiety and/or depression compared to an active control condition, an abbreviated 8-week adaptation of Utalk preventive intervention (La Greca et al., 2016). Further, there is an absence of information about the potential benefits of including booster sessions.
There is a critical need for adapting evidence-based interventions for clinically disturbed adolescents to reach out to those at high risk and examine its efficacy in an RCT, using ACC. To cover this gap, under Prf. Ehrenreich-May’s permission and supervision, UP-A was adapted as PROCARE-I to be used in a group and telepsychology format with a reduced number of sessions along with a booster session conducted 6 months after the intervention. This study is aimed at evaluating the efficacy of an abbreviated, indicated transdiagnostic preventive intervention for anxiety and depression symptomatology in adolescents, named PROCARE-I, compared to an ACC based on emotional psychoeducation. The RCT is to measure the impact of interventions on improving the quality of life of young people, resilience, and psychological flexibility by increasing emotional literacy, self-awareness, self-regulation, motivation, empathy, and social skills. It was hypothesized that PROCARE-I would be more effective than the ACC using between-group comparisons across time assessments. In addition, within-group comparisons PROCARE-I would demonstrate greater improvements in emotion regulation, psychological flexibility, quality of life, and a decrease in anxiety and depressive symptomatology and level of emotional risk, with small to medium effect sizes.
Methods
Design
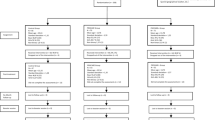
The present study follows a two-arm double-blind RCT (Arm 1 = Active control condition; Arm 2 = PROCARE-I) in Spanish adolescent population. To test the efficacy and efficiency of PROCARE-I, we followed the Consolidated Standards of Reporting Trials (CONSORT: http://www.consort-statement.org) and the SPIRIT guidelines (Standard Protocol Items: Recommendations for Intervention Trials). The study was registered at the ClinicalTrial.gov database: ClinicalTrials.gov Identifier: NCT05252026. Assessment periods included a baseline, a post-test, a 6-month follow-up, and a 1-month follow-up after the booster session (7 months after core intervention) (see Fig. 1). Both groups received a group and online intervention using telepsychology (Google Meet) because of social distancing measures due to the COVID-19 pandemic. PROCARE-I received the institutional review board (IRB) approval, and all evaluations were conducted in an online format through a secure platform. This research was authorized by the bioethics committee of the University of Jaen (ID: GEN-3461-aab8-41a3-85c2-ca28-5102-cdda-8d53). The trial was planned according to internationally adopted guidelines (ICH-E6, E8, and E9), being also considered other guidelines, e.g., from the European Medicine Agency (EMA). PROCARE-I adhered to current data protection legislation (Regulation (EU) 2016/679).
Participants
The screening included 309 adolescents between 12 and 18 years of age (M = 14.57; SD = 1.74). Specifically, 211 self-reported their gender as female (68.29%), 96 as male (31.06%), and 2 as non-binary (0.65%). Out of 309 participants, 100 evidenced emotional symptomatology and were eligible to enter the trial. The selected sample of this study consisted of 64 youths (53% female and 47% male) who decided to enroll in the RCT, ranging from 12 to 18 years old (M = 13.69; SD = 1.56). As can be seen in Table 1, age, gender, and nationality distribution were homogeneous for both conditions and there was no relation of interdependence between the experimental conditions and any of the sociodemographic variables tested (p > 0.05).
The inclusion criteria were: 1) informed consent by the legal guardian and the adolescent; 2) technological means to attend the online sessions; 3) measurements above the limit on the emotional problems scale of the Spanish version of self-reported Strength and Difficulties Questionnaire (SDQ) for adolescents or for parents-reported version (Barriuso-Lapresa et al., 2014; Ortuño-Sierra et al., 2014); 4) scores above the normative data for overall symptomatology or any of the subscales (depression, panic, social phobia, separation, generalized anxiety and obsessive compulsive disorder) measured with the Revised Children’s Anxiety and Depression Scale (RCADS-30; Piqueras et al., 2017); 5) absence of a diagnosis of anxiety and/or mood disorders on the basis of the semi-structured interview of the Anxiety and Related Disorders Interview Schedule for DSM-5 (ADIS-5-C/P; Albano & Silverman, in press) administered to the child and the parents; 6) not receiving psychological/psychiatric treatment, 7) no presence of acute suicidality; and 8) no presence of autism spectrum disorder diagnosis. Participants were randomly allocated to either ACC (N = 31) or PROCARE-I (N = 37) (See Fig. 1).
Measures
The assessment of primary and secondary outcomes included the following self-reported measures via a survey supported by Limesurvey©. The clinical diagnostic interview was administered online via videoconference.
Primary outcome measures
The Strengths and Difficulties Questionnaire (SDQ, Goodman, 1997) (www.sdqinfo.org) is a 25-item questionnaire to assess emotional and behavioral problems, hyperactivity/inattention, peer relationship problems, and prosocial behavior in children and adolescents. It has been translated into several languages, including Spanish, and has a broad cross-cultural validity. It has a 3-point Likert scale from 0 to 2 ("not true", "somewhat true" and "certainly true"). Both the self-report and the parent version had shown adequate psychometric properties and cut-off scores for screening purposes (Barriuso-Lapresa et al., 2014; Ortuño-Sierra et al., 2014). Due to the nature of our study, the 5-item emotional subscale of the parent and self-report SDQ were administered. In this study, the reliability (Cronbach’s alpha; α) was 0.82 and 0.78 for self-reported and parent versions, respectively.
The Revised Child Anxiety and Depression Scale, 30-item version, RCADS-30 (Sandín et al., 2010) consists of 30 items with a Likert-type scale from 0 to 3 ("never", "sometimes", "often" and "always"). It assesses anxiety and depression symptoms in children and adolescents through different subscales: panic disorder (PD), social phobia (SP), separation anxiety disorder (SAD), generalized anxiety disorder (GAD), obsessive–compulsive disorder (OCD), and major depressive disorder (MDD). The RCADS-30 has excellent psychometric properties and cut-off points for Spanish populations (Piqueras et al., 2017). In our study, the RCADS-30 total score was found to have excellent mean reliability (α = 0.90). Acceptable to good reliability was also found for the subscales, with values ranging from 0.65 to 0.78.
The Anxiety Disorders Interview Schedule for DSM-5 – Child and Parent Versions (ADIS-5-C/P; Albano & Silverman, in press) assesses anxiety disorders in 6- to 17-year-olds and is organized according to the anxiety disorders listed in the 5th Edition of the Diagnostic and Statistical Manual of Mental Disorders (DSM-5; American Psychological Association, 2013). The ADIS-5-C/P consists of comparable but separate child and parent interviews. Although designed specifically to diagnose anxiety disorders, the children's version (ADIS-5-C) also assesses affective disorders and ADHD and includes screening for other conditions (substance abuse, schizophrenia, eating disorders, somatoform disorders, etc.). The parent version (ADIS-5-P) also assesses conduct disorders and includes screening for other conditions (such as enuresis, pervasive developmental disorders, and learning disorders). This interview was used to diagnose or rule out a diagnosis at baseline. The presence of any disorder was considered based on information provided by both adolescents and parents. A composite severity score (CSR) was also obtained by the clinician on a scale from 0 to 8, clinically significant at 4 points and above. A Spanish translation was administered after obtaining Oxford University Press’ approval for the ADIS-5- C/P to be used for research purposes. The interviews were administered, through Google Meet, separately to the adolescent and the parents, taking an average duration of 90 min.
Secondary outcome measures
The 10-Item Connor-Davidson Resilience Scale (CD-RISC-10; Campbell-Sills & Stein, 2007) is a self-report shortened version of the original Connor & Davidson, (2003) scale. It assesses resilience through 10 items with a 5-point Likert-type response format. The internal consistency of the Spanish version is α = 0.85 and is considered a reliable and valid instrument to measure this construct (Notario-Pacheco et al., 2011). In this study, we found excellent reliability (α = 0.92).
The KIDSCREEN-10 Index (Ravens-Sieberer et al., 2001). A questionnaire developed from the KIDSCREEN-27 which assesses the overall health-related quality of life of children and adolescents concerning physical, mental, and social health status. This instrument contains 10 items with a Likert-type response format ranging from 0 to 5 (“not at all”, “a little”, “moderately”, “a lot” and “very much”). The psychometric properties are adequate (Ravens-Sieberer et al., 2010). In this study, Cronbach’s alpha value was 0.85.
The Willingness & Action Measure for Children and Adolescents (WAM-C/A; Greco et al., 2004; Larson, 2008) is a measure of psychological flexibility assessing the willingness to accept and be in contact with emotions, thoughts, feelings, or emotional experiences which generate discomfort (acceptance subscale), as well as the tendency to act in line with important life values and goals (action subscale). It has 14 items with a Likert-type response format scored from 0 to 4 ("not true at all", "a little true", "quite true", "true" and "very true"). The Spanish adaptation of Cobos-Sánchez et al., (2020) has shown a Cronbach's alpha of 0.87 for the total score. In this study, Cronbach’s alpha value was 0.72.
The Difficulties in Emotion Regulation Scale (DERS; Gratz & Roemer, 2004). The Spanish adaptation was applied, which has shown adequate psychometric properties in Spanish adolescents (Hervás & y Jódar, 2008). It assesses emotional regulation through 36 items with a Likert-type response format ranging from 0 to 4 (“Almost never”, “sometimes”, “half the time”, “most of the time”, “almost always”) grouped into six dimensions: (1) non-acceptance of emotional responses, (2) difficulties in directing behavior towards goals when upset, (3) difficulties in controlling impulsive behaviors when upset, (4) effective emotional regulation strategies, (5) lack of emotional awareness and emotional clarity. In this study, Cronbach’s alpha value was 0.82.
Other measures
The Client Satisfaction Questionnaire (CSQ-8, Larsen et al., 1979). The CSQ-8 is a self-report questionnaire assessing the general level of satisfaction with the service received. It is comprised of eight items which are scored on a scale, ranging from 1 to 4. The total score varies from 8 to 32, where a higher score indicates greater satisfaction with the service received. Good psychometric properties for the Spanish-speaking population have also been found by Vázquez et al., (2019). In this study, Cronbach’s alpha value was 0.82.
Procedure
This trial was divided into several phases: screening, pre-test assessment, and allocation to treatment conditions, 8-sessions of a 60-min length intervention, a post-test assessment, a 6-month-follow-up followed by a 60-min booster session, and a 1-month follow-up after the booster session. The sample was recruited through secondary education centers, social media, and mass press, as well as local, regional, and national administrations of the Spanish state organization related to education and youth. Informed consent was obtained from legal guardians and the adolescents themselves. The SDQ, CD-RISC, and RCADS-30 were administered online and used for screening purposes. The presence of a clinical diagnosis was determined using ADIS-5-C/P to rule out the diagnosis. All participants received written or oral feedback on the results.
Those adolescents who met the previously described inclusion and exclusion criteria were assigned to PROCARE-I and ACC groups. All participants were randomly assigned to one of the conditions and had no knowledge of which intervention they were receiving. Assessors were also blind to treatment allocation. Adolescents with scores indicative of the presence of emotional risk but the absence of emotional symptomatology (i.e., selective scores) were offered the possibility to participate in a selective prevention program. In addition, adolescents with a clinical disorder were referred to public mental health services. To encourage maximum fidelity to the protocol, online training was used to train therapists in both PROCARE-I and ACC. The high standards supervision of the UP-A techniques was performed under the supervision of Prof. Jill Ehrenreich-May. All therapists passed all treatment competency checks following training. Additional measures of protocol adherence and treatment integrity were developed during the RCT for both treatment conditions. Fidelity sheets were filled in by therapists after each session and were supervised by the University of Miami’s team as independent evaluators to maintain the maximum possible fidelity to treatment content and manual directions.
Before the first session, 12 adolescents enrolled in the ACC declined to enter the trial claiming that it would interfere with academic assignments and perception of lack of usefulness. As for the PROCARE-I condition, another 12 adolescents were unable to commit to a treatment schedule.
An intention-to-treat (ITT) analysis revealed no significant differences (p > 0.05) between the sample assigned to the initial treatment (N = 100) and the one which benefited from experimental treatment conditions (N = 68). As a result, adolescents were allocated to either the control condition (n = 31) or the PROCARE-I (n = 37) group. During trial, three and one adolescents dropped out of the ACC and PROCARE-I conditions, respectively. As a result, 28 (90.4% of the sample retained) and 36 (97.3% of the sample retained) adolescents completed the control and PROCARE-I conditions, respectively.
During the post-treatment and follow-up assessment periods, all parents and adolescents were reassessed. Following the recommendations of the EU Clinical Trial Directive (2001/20/EC) and Regulation (536/2014), compensation to research participants was not a benefit and was not listed in the benefits section of the protocol. Recruitment techniques (e.g., advertising) did not focus on compensation as a means of enticing potential participants. Those participants who enrolled in the RCT and post-test assessment did not receive any compensation. Only adolescents and parents participating in the booster session and follow-up assessments were eligible to be compensated for their time.
Experimental conditions
The two experimental conditions (PROCARE-I and ACC) included a 15-min initial informational and individual session with the adolescent and their family (session 0). The following sessions were group-based (6–8 adolescents) and run by a therapist and a co-therapist certified by the University of Miami and held via Google Meet. Both conditions included a booster session (60-min-length) six months after the intervention to maintain the effects of interventions over time. Details of each treatment strand are provided below:
The PROCARE-I intervention was an abbreviated adaptation of the Unified Protocol for Transdiagnostic Treatment of Emotional Disorders in Adolescents (UP-A, Ehrenreich-May et al., 2018). The UP-A uses evidence-based CBT strategies for the treatment of emotional disorders such as emotion education, cognitive reappraisal, behavioral activation, and a range of exposure techniques; along with others such as motivation enhancement and mindfulness techniques. It aims to promote change through improvements in emotional reactivity and regulation skills, enhancing tolerance to distress associated with negative emotions and reducing or eliminating maladaptive emotional behaviors that reinforce the intensity of emotional distress in the long term. The following modules were delivered: education about emotions and emotional behaviors, introduction to emotion-focused behavioral experiments, awareness of physical sensations, flexible thinking, emotional awareness, and situation-based exposures to emotion. PROCARE-I did not include UP-A’s parent-directed materials but parents were informed of adolescent’s session contents at end of each session.
The ACC active control condition was an abbreviated 8-week adaptation of the 12-week UTalk preventive intervention for adolescents who are at risk for problems with social anxiety and/or depression developed by La Greca et al., (2016). UTalk is based on emotional psychoeducation in a group format, emphasizing discussion of thoughts, feelings, and behavior as parts of emotion, and providing support around generally distressing events. No explicit coping strategies for dealing with strong emotions or CBT strategies beyond psychoeducation were provided as part of this program. ACC was a youth-focused intervention but parents were informed of adolescent’s session contents at end of each session.
Data analysis
Data were coded and analyzed with the statistical package IBM SPSS Statistics 28.0 (IBM Corp Released, 2021). First, analyses were carried out to ensure the equivalence of the experimental conditions in the pretest. Comparisons between sociodemographic variables between control and PROCARE-I were calculated using Z (Mann Whitney's U for nonparametric comparisons with a quantitative variable; χ2 (Chi-square) for comparisons with a nominal variable). As no differences were found according to any of the sociodemographic variables (p > 0.05), subsequent analyses were performed without controlling for gender, age, or any other variables. Between-group analyses were examined using the Student's t-test and the Mann Whitney’s U test (for nonparametric comparisons) at the pretest, post-test, 6-month follow-up, and 1-month after the booster session. Within-group comparisons were calculated for each condition. Descriptive analyses (means and standard deviations) of the different experimental groups were carried out to examine differences between pre-test and post-tests using either ANOVA for paired samples or the Friedman test for nonparametric comparisons. Finally, should significant comparisons between pre-test and post-test (post-interventions, follow-up, and post-booster sessions) be evident, either Student's t-test paired-samples or the Wilcoxon signed-rank test (for nonparametric comparisons) were computed. Effect sizes were analyzed using Cohen’s d (typified mean difference) (Cohen, 1988) and Pearson’s r (Coolican, 2009). For parametric comparisons, Cohen’s d: small (a1) = 0.2, medium (a2) = 0.5, large (a3) = 0.8 was used; for nonparametric comparisons Pearson’ r: small (b1) = 0.1, medium (b2) = 0.3, large (b3) = 0.5.
Results
Between-group analyses
No statistically significant differences between the conditions were found regarding age, gender, ethnicity nor attendance to sessions (Table 1). As can be seen in Table 2, results revealed no statistically significant differences among the conditions at the baseline or pretest.
At the post-test (Table 2), statistically significant differences were observed in the psychological flexibility between ACC and PROCARE-I, with a medium effect size. At follow-up, significant differences in favor of PROCARE-I were found in the self-reported level of emotional risk and emotion regulation, with low effect sizes. At 1-month following the booster session, data showed significant statistical differences on primary outcome measures, revealing that PROCARE-I was significantly superior to ACC in the reduction of overall mood and anxiety symptomatology, specific panic and separation anxiety symptomatology and decrease of the level of emotional risk as reported by both adolescents and parents, with medium effect sizes. Further, PROCARE-I increased significantly secondary measures such as quality of life, resilience and psychological flexibility compared to ACC, with low to medium effect sizes.
Within-group analyses
For the ACC condition, significant differences on primary outcome measures at post-test were limited to the level of emotional risk measured by parents and obsessive–compulsive symptomatology, with medium effect sizes (Table 3). Compared to the pretest, at the 6-month follow-up participants evidenced a decrease in panic symptomatology, obsessive–compulsive symptomatology, overall anxiety and mood symptomatology and level of emotional risk measured by parents. In addition, an increase in levels of resilience and emotion regulation were found. Effect sizes were medium with the exception of obsessive–compulsive symptomatology, which was high. These differences were maintained at follow-up following booster, except for overall anxiety and mood symptomatology. Finally, emotional regulation reached unique significance between post and follow-ups, with medium effect sizes.
As far as the PROCARE-I condition is concerned, comparisons between the pretest and post-test or follow-ups revealed significant differences for most of the primary and secondary outcome measures (see Table 4). Youth in the PROCARE-I condition evidenced statistically significant improvement after intervention in overall anxiety and mood symptomatology and a specific decrease in generalized anxiety, obsessive–compulsive and depressive symptomatology, with low and medium effect sizes. In addition, there was evident a significant reduction in the level of emotional risk reported by parents and adolescents, with medium and large effect sizes. Gains were also observed in secondary outcome measures at post-test: an increase in the level of resilience, emotion regulation, and psychological flexibility, with medium effect sizes. Compared to the pretest, at the 6-month follow-up, participants also evidenced improvements in their panic and separation anxiety symptomatology in addition to gains at the post-test. Most of the effect sizes at the 6-month follow-up were large. Further, comparisons between the pretest and 1-month follow-up after the booster session revealed a significant unique decrease in social anxiety symptomatology and an increase of effect sizes in all treatment outcome measures, mostly in the large range. Statistical testing of secondary outcomes revealed significant differences in the levels of resilience, psychological flexibility, and emotion regulation between pretreatment and follow-ups with medium to large effect sizes. Only separation anxiety symptomatology and emotion regulation were significant between the post-test and 6-month follow-up, with medium and high effect sizes, respectively. There was a positive effect of the booster session when compared to the post-test on primary outcome measures: statistically significant improvement in emotional risk as reported by both adolescents and parents, in overall anxiety and mood symptomatology, and a specific decrease in generalized anxiety, panic, separation anxiety, and depressive symptomatology, ranging from low to large effect sizes. Additional gains were also observed on secondary treatment measures: an increase in levels of resilience and emotion regulation, with large effect sizes. Finally, a specific effect of the booster session was observed in the decrease of overall anxiety and mood symptomatology and level of emotional risk as reported by parents as well as an increase of levels of resilience, mostly with medium effects sizes.
At 6-month follow-up after the intervention, 3 participants in the ACC (10.7%) and 2 in PROCARE-I (5.6%) evidenced a clinical emotional disorder. Specifically, one girl was diagnosed with MDD, another with social phobia, and a third one with social phobia and comorbid MDD in the control condition. At PROCARE-I, two girls developed a social anxiety disorder. There were no differences between conditions in preventing the onset of clinical disorders (p > 0.05).
Attendance, feasibility, fidelity, and acceptability rates
The attendance of participants to sessions (range: 0–8) was high for the ACC (M = 7.68; SD = 0.72) and PROCARE-I (M = 7.58; SD = 0.65), with no statistical differences between conditions, (Z = -107, p = 0.28). Participation of adolescents was also high (0–16) in ACC (M = 10.78; SD = 4.00) and PROCARE-I (M = 10.11; SD = 3.44) with no statistical differences between conditions, Z = -0.88, p = 0.37. Fidelity of therapists to manualized interventions data revealed that 98.7% and 97.8% were fully compliant with the checklist for ACC and PROCARE-I, respectively. Participant’s satisfaction levels, as measured by the Client Satisfaction Questionnaire (CSQ-8, range 0–32), were medium–high for ACC (M = 24.7; SD = 3.74) and PROCARE-I participants (M = 25.34; SD = 4.19), with no statistical differences between conditions (p = 0.40).
Discussion
This paper presents the results of an RCT that examined the efficacy of PROCARE-I, an abbreviated group-based adaptation of UP-A, delivered via telepsychology with a 60-min booster session for indicated prevention, as compared to an emotion education and support condition. The results showed that PROCARE-I, as an indicated preventive transdiagnostic intervention, significantly reduced adolescents’ anxiety and depression symptoms and the risk of developing anxiety and/or depressive disorders in adolescents while improving resilience, psychological flexibility, and emotional regulation at both the post-test and the 6-month follow-up. These data suggest that the PROCARE-I preventive intervention is not only effective in reducing emotional symptomatology and emotional risk, but it also impacts on another transdiagnostic variables, such as resilience, emotion regulation, and psychological flexibility, with medium to high effect sizes.
Compared to the ACC, PROCARE-I showed significant improvements in primary measures assessing overall anxiety and depressive symptomatology, panic, separation anxiety, and emotional risk reported by both adolescents and parents, as well as in the secondary measures of resilience, quality of life, and psychological flexibility, one month after the booster session. The presence of between-group differences at follow-up following the booster session is consistent with recent study conducted by Schmitt et al., (2022) with a at 3-month follow-up but contrast with other studies revealing no differences over the long term (Hugh-Jones et al., 2021; Rasing et al., 2017; Stockings et al., 2016; Teubert & Pinquart, 2011).
Differences in these particular variables in the PROCARE-I rather than ACC suggest transdiagnostic measures may be more sensitive to capture treatment changes in evidence-based transdiagnostic protocols. These findings are in line with other transdiagnostic interventions showing an increase in client cognitive flexibility (Milgram et al., 2022; Morris & Mansell, 2018, Sighvatsson et al., 2020). This suggests that the PROCARE-I intervention may exert preventive effects on anxiety or depression symptomatology through improved emotion management and psychological flexibility. However, at post-treatment, the differences between both interventions were only significant for psychological flexibility, which was maintained after the booster session. Indeed, the booster session contributed to maintaining long-term effects, highlighting the relevant role of the booster session for the transdiagnostic treatment in the maintenance of effects over time, which is consistent with reports from other studies (Loevaas et al., 2020; Rasing et al., 2017; Stockings et al., 2016).
The acceptability of both interventions was found to be good with a limited number of dropouts and good participant satisfaction in both conditions. Thus, participants who attended a large number of sessions in both conditions and drop-outs during the intervention were limited to 9.6% and 2.7% for ACC and PROCARE-I, respectively. This suggests that both interventions were well-received by participants, in line with other transdiagnostic internet-delivered prevention programs for adolescents (Schmitt et al., 2022).
After the interventions, only 5.6% of adolescents who enrolled in the PROCARE-I condition developed a full anxiety or mood disorder, consistent with studies suggesting that indicated preventive interventions can contribute to the prevention of the development of a clinical disorder (Rasing et al., 2017). PROCARE-I showed to be more successful in preventing the onset of anxiety and/or depression disorders, although not statistically significant. It may be plausible that the inclusion of an ACC may have contributed to this finding. Future studies should examine the effect of other control conditions (e.g., waiting-list, placebo, etc.) to monitor the potential effect of the ACC. Another explanation is that booster sessions may have reduced the likelihood of the onset of clinical disorders in both conditions, as authors have argued that booster sessions could maintain the effects of interventions over time (Rasing et al., 2017; Stockings et al., 2016). One of the strengths of this study is the inclusion of an ACC and use of a multi-informant approach (parents and children), and the administration of diagnostic assessments for clinical diagnoses.
Some limitations should be noted. First, the limited sample size may have limited the ability to detect significant differences between the conditions at post-test. Second, the study did not examine differences between completers and non-completers due to low drop-out rates. Third, future studies should analyze potential mediators or moderators of the treatment. Fourth, the study found that participants reported high satisfaction levels, but some participants expressed a preference for attending sessions in person, indicating a need to examine the effectiveness of PROCARE-I in a face-to-face format. Fifth, the study did not evaluate the cost-effectiveness of PROCARE-I, and cost-effectiveness methods should be applied in future studies to determine the value of conducting indicated interventions. Finally, the study only assessed the effects at medium term, so future research should evaluate the potential of this indicated transdiagnostic preventive intervention in the longer term.
Despite these limitations, the results of this randomized controlled trial suggest the efficacy of an acceptable, brief group-based transdiagnostic intervention delivered using telepsychology compared to the active control condition for adolescents at high-risk for developing emotional disorders. Although meta-analytic reviews have found that differences in indicated interventions are more evident at post-test and smaller at follow-ups (e.g., Hugh-Jones et al., 2021; Teubert & Pinquart, 2011), our data reveal that indicated, brief transdiagnostic programs may produce significant effects, which persist at follow-up and after a booster session.
Conclusions
The results of this study reveal that PROCARE-I, an adapted 8-week UP-A intervention delivered via telepsychology in a group format, was not sufficient to reduce emotional symptoms until a booster session was implemented. The data revealed in the post-booster proved that participants in the PROCARE-I condition showed significant improvements in resilience, quality of life, psychological flexibility together with reductions in anxiety, depression and risk of emotional problems. The intervention was well-accepted, with a low drop-out rate of less than 3%, and only a small proportion of participants (less than 6%) developed an emotional disorder at follow-up. If the 8-week treatment is the only option due to time or financial constraints, future research lines should examine if a more personalized intervention may be the key to achieve significant outcomes at postest. Providing adolescents additional tailor-made sessions which aim at their specific risk factors may be a promising path to explore. In summary, ensuring that adolescents benefit from a booster session, 8-week PROCARE-I may be an effective online indicated primary prevention approach for high-risk adolescents.
Data Availability
Data sets generated and/or analyzed during this study are not publicly available due to organizational limitations, but are available from the corresponding author upon reasonable request.
References
Albano, A. M. & Silverman, W.K. (in press) The anxiety disorders interview schedule for children for DSM-5, Child and Parent Versions. New York, NY: Oxford University Press.
American Psychological Association. (2013). Diagnostic and statistical manual of mental disorders (5th ed.). American Psychiatric Publishing.
Balázs, J., Miklósi, M., Keresztény, A., Hoven, C. W., Carli, V., Wasserman, C., Apter, A., Bobes, J., Brunner, R., Cosman, D., Cotter, P., Haring, C., Iosue, M., Kaess, M., Kahn, J. P., Keeley, H., Marusic, D., Postuvan, V., Resch, F., … Wasserman, D. (2013). Adolescent subthreshold depression and anxiety: psychopathology, functional impairment, and increased suicide risk. Journal of Child Psychology and Psychiatry, and aAllied Disciplines, 54(6), 670–677. https://doi.org/10.1111/jcpp.12016.
Barriuso-Lapresa, L. M., Hernando-Arizaleta, L., & Rajmil, L. (2014). Reference values of the strengths and difficulties questionnaire (SDQ) version for parents in the Spanish population, 2006. Actas Españolas De Psiquiatria, 42(2), 43–48.
Beardslee, W. R., Brent, D. A., Weersing, V. R., Clarke, G. N., Porta, G., Hollon, S. D., Gladstone, T. R., Gallop, R., Lynch, F. L., Iyengar, S., DeBar, L., & Garber, J. (2013). Prevention of depression in at-risk adolescents: Longer-term effects. JAMA Psychiatry, 70(11), 1161–1170. https://doi.org/10.1001/jamapsychiatry.2013.295
Bennett, K., Manassis, K., Duda, S., Bagnell, A., Bernstein, G. A., Garland, E. J., Miller, L. D., Newton, A., Thabane, L., & Wilansky, P. (2015). Preventing child and adolescent anxiety disorders: An overview of systematic reviews. Depression and Anxiety, 32(12), 909–918. https://doi.org/10.1002/da.22400
Campbell-Sills, L., & Stein, M. B. (2007). Psychometric analysis and refinement of the Connor-Davidson Resilience Scale (CD-RISC): Validation of a 10-item measure of resilience. Journal of Traumatic Stress, 20(6), 1019–1028. https://doi.org/10.1002/jts.20271
Canals-Sans, J., Hernández-Martínez, C., Sáez-Carles, M., & Arija-Val, V. (2018). Prevalence of DSM-5 depressive disorders and comorbidity in Spanish early adolescents: Has there been an increase in the last 20 years? Psychiatry Research, 268, 328–334. https://doi.org/10.1016/j.psychres.2018.07.023
Cobos-Sánchez, L., Flujas-Contreras, J. M., & Gómez, I. (2020). Willingness and action measure for adolescents: Psychometric validation in Spanish adolescents. Journal of Contextual Behavioral Science, 15, 46–51. https://doi.org/10.1016/j.jcbs.2019.11.006
Cohen, J. (1988). Statistical power analysis for the behavioral sciences (2nd ed.). Lawrence Erlbaum Associates, Publishers.
Connor, K. M., & Davidson, J. R. (2003). Development of a new resilience scale: The Connor-Davidson Resilience Scale (CD-RISC). Depression and Anxiety, 18(2), 76–82. https://doi.org/10.1002/da.10113
Coolican, H. (2009). Research methods and statistics in psychology (5th ed.). Hodder Education Group.
Dodge, K. A. (2020). Annual Research Review: Universal and targeted strategies for assigning interventions to achieve population impact. Journal of Child Psychology and Psychiatry, and Allied Disciplines, 61(3), 255–267. https://doi.org/10.1111/jcpp.13141
Ehrenreich-May, J., & Kennedy, S. M. (2021). Applications of the Unified Protocols for Transdiagnostic Treatment of Emotional Disorders in Children and Adolescents. Oxford University Press.
Ehrenreich-May, J., Kennedy, S. M., Sherman, J. A., Bilek, E. L., Buzzella, B. A., Bennett, S. M., & Barlow, D. H. (2018). The Unified Protocol for Transdiagnostic Treatment of Emotional Disorders in Adolescents (UP-A; in Unified protocols for transdiagnostic treatment of emotional disorders in children and adolescents). Oxford University Press.
Faltinsen, E., Todorovac, A., Hróbjartsson, A., Gluud, C., Kongerslev, M. T., Simonsen, E., & Storebø, O. J. (2019). (2019) Placebo, usual care and wait-list interventions for all mental health disorders. Cochrane Database of Systematic Reviews, 1, 1–26. https://doi.org/10.1002/14651858.MR000050
Furukawa, T. A., Noma, H., Caldwell, D. M., Honyashiki, M., Shinohara, K., Imai, H., Chen, P., Hunot, V., & Churchill, R. (2014). Waiting list may be a nocebo condition in psychotherapy trials: A contribution from network meta-analysis. Acta Psychiatrica Scandinavica, 130(3), 181–192. https://doi.org/10.1111/acps.12275
García-Escalera, J., Chorot, P., Sandín, B., Ehrenreich-May, J., Prieto, A., & Valiente, R. M. (2019). An open trial applying the Unified Protocol for Transdiagnostic Treatment of Emotional Disorders in Adolescents (UP-A) adapted as a school-based prevention program. Child & Youth Care Forum, 48(1), 29–53. https://doi.org/10.1007/s10566-018-9471-0
García-Escalera, J., Valiente, R. M., Sandín, B., Ehrenreich-May, J., Prieto, A., & Chorot, P. (2020). The Unified Protocol for Transdiagnostic Treatment of Emotional Disorders in Adolescents (UP-A) Adapted as a School-Based Anxiety and Depression Prevention Program: An Initial Cluster Randomized Wait-List-Controlled Trial. Behavior Therapy, 51(3), 461–473. https://doi.org/10.1016/j.beth.2019.08.003
Garcia-Lopez L. J. (2023). Novel approaches for the prevention of emotional problems in young people. Journal of anxiety disorders, 100, 102797. https://doi.org/10.1016/j.janxdis.2023.102797
Goodman, R. (1997). The Strengths and Difficulties Questionnaire: A research note. Journal of Child Psychology and Psychiatry, and Allied Disciplines, 38(5), 581–586. https://doi.org/10.1111/j.1469-7610.1997.tb01545.x
Gratz, K. L., & Roemer, L. (2004). Multidimensional assessment of emotion regulation and dysregulation: Development, factor structure, and initial validation of the difficulties in emotion regulation scale. Journal of Psychopathology and Behavioral Assessment, 26, 41–54. https://doi.org/10.1023/B:JOBA.0000007455.08539.94
Greco, L. A., Murrell, A.M., & Coyne, L.W. (2004).Willingness and acceptance measure for children and adolescents (WAM-C/A). Available from Laurie Greco, Division of Adolescent Medicine and Behavioral Science, Vanderbilt University Medical Center, Nashville, TN.
Hervás, G., & y Jódar, R. (2008). Adaptación al castellano de la Escala de dificultades en la regulación emocional. Clínica y salud: Investigación Empírica en Psicología, 19(2), 139–56.
Hugh-Jones, S., Beckett, S., Tumelty, E., & Mallikarjun, P. (2021). Indicated prevention interventions for anxiety in children and adolescents: A review and meta-analysis of school-based programs. European Child & Adolescent Psychiatry, 30(6), 849–860. https://doi.org/10.1007/s00787-020-01564-x
IBM Corp. Released (2021). IBM SPSS statistics for windows, version 28.0. Armonk, NY: IBM Corp.
Jiménez-Vázquez, D., Garcia-Lopez, L.J., & Vivas, M. (in press). Indicated preventive interventions for high-risk adolescents of emotional disorders: a systematic review. Revista de Psicología Clínica con Niños y Adolescentes [The Journal of Clinical Psychology with Children and Adolescents].
La Greca, A. M., Ehrenreich-May, J., Mufson, L., & Chan, S. (2016). Preventing adolescent social anxiety and depression and reducing peer victimization: Intervention development and open trial. Child & Youth Care Forum, 45(6), 905–926. https://doi.org/10.1007/s10566-016-9363-0
Larsen, D. L., Attkisson, C. C., Hargreaves, W. A., & Nguyen, T. D. (1979). Assessment of client/patient satisfaction: Development of a general scale. Evaluation and Program Planning, 2(3), 197–207. https://doi.org/10.1016/0149-7189(79)90094-6
Larson, C.M. (2008) Stories: A revision of the willingness & action measure for children and adolescents (WAM-C/a). [Doctoral dissertation, University of North Texas] University of North Texas Research Repository . https://digital.library.unt.edu/ark:/67531/metadc9761/m2/1/high_res_d/thesis.pdf
Lawrence, P. J., Rooke, S. M., & Creswell, C. (2017). Review: Prevention of anxiety among at-risk children and adolescents - a systematic review and meta-analysis. Child and Adolescent Mental Health, 22(3), 118–130. https://doi.org/10.1111/camh.12226
Lewinsohn, P. M., Solomon, A., Seeley, J. R., & Zeiss, A. (2000). Clinical implications of “subthreshold” depressive symptoms. Journal of Abnormal Psychology, 109(2), 345–351. https://doi.org/10.1037/0021-843X.109.2.345
Loevaas, M., Lydersen, S., Sund, A. M., Neumer, S. P., Martinsen, K. D., Holen, S., Patras, J., Adolfsen, F., Rasmussen, L. P., & Reinfjell, T. (2020). A 12-month follow-up of a transdiagnostic indicated prevention of internalizing symptoms in school-aged children: The results from the EMOTION study. Child and Adolescent Ppsychiatry and Mental Health, 14, 15. https://doi.org/10.1186/s13034-020-00322-w
Makover, H., Adrian, M., Wilks, C., et al. (2019). Indicated prevention for depression at the transition to high school: Outcomes for depression and anxiety. Prevention Science, 20, 499–509. https://doi.org/10.1007/s11121-019-01005-5
Milgram, L., Tonarely, N. A., & Ehrenreich-May, J. (2022). Youth Top Problems and Early Treatment Response to the Unified Protocols for Transdiagnostic Treatment of Emotional Disorders in Children and Adolescents. Child Psychiatry and Human Development, 53(3), 582–598. https://doi.org/10.1007/s10578-021-01151-4
Morris, L., & Mansell, W. (2018). A systematic review of the relationship between rigidity/flexibility and transdiagnostic cognitive and behavioral processes that maintain psychopathology. Journal of Experimental Psychopathology, 9(3), Article 2043808718779431. https://doi.org/10.1177/2043808718779431
Notario-Pacheco, B., Solera-Martínez, M., Serrano-Parra, M. D., Bartolomé-Gutiérrez, R., García-Campayo, J., & Martínez-Vizcaíno, V. (2011). Reliability and validity of the Spanish version of the 10-item Connor-Davidson Resilience Scale (10-item CD-RISC) in young adults. Health and Quality of Life Outcomes, 9, 63. https://doi.org/10.1186/1477-7525-9-63
Ortuño-Sierra, J., Fonseca-Pedrero, E., Paíno, M., & Aritio-Solana, R. (2014). Prevalence of emotional and behavioral symptomatology in Spanish adolescents. Revista De Psiquiatria y Salud Mental, 7(3), 121–130. https://doi.org/10.1016/j.rpsm.2013.12.003
Peris-Baquero, Ó., Moreno, J. D., & Osma, J. (2022). Long-term cost-effectiveness of group unified protocol in the Spanish public mental health system. Current Psychology. https://doi.org/10.1007/s12144-022-03365-8
Piqueras, J. A., Pineda, D., Martin-Vivar, M., & Sandín, B. (2017). Confirmatory factor analysis and psychometric properties of the Revised Child Anxiety and Depression Scale−30 (RCADS-30) in clinical and non-clinical samples. Revista De Psicopatología y Psicología Clínica, 22(3), 183–196. https://doi.org/10.5944/rppc.vol.22.num.3.2017.19332
Polanczyk, G. V., Salum, G. A., Sugaya, L. S., Caye, A., & Rohde, L. A. (2015). Annual research review: A meta-analysis of the worldwide prevalence of mental disorders in children and adolescents. Journal of Child Psychology and Psychiatry, and Allied Disciplines, 56(3), 345–365. https://doi.org/10.1111/jcpp.12381
Racine, N., McArthur, B. A., Cooke, J. E., Eirich, R., Zhu, J., & Madigan, S. (2021). global prevalence of depressive and anxiety symptoms in children and adolescents during COVID-19: A meta-analysis. JAMA Pediatrics, 175(11), 1142–1150. https://doi.org/10.1001/jamapediatrics.2021.2482
Rasing, S., Creemers, D., Janssens, J., & Scholte, R. (2017). Depression and anxiety prevention based on cognitive behavioral therapy for at-risk adolescents: A meta-analytic review. Frontiers in Psychology, 8, 1066. https://doi.org/10.3389/fpsyg.2017.01066
Ravens-Sieberer, U., Erhart, M., Rajmil, L., Herdman, M., Auquier, P., Bruil, J., Power, M., Duer, W., Abel, T., Czemy, L., Mazur, J., Czimbalmos, A., Tountas, Y., Hagquist, C., Kilroe, J., European KIDSCREEN Group. (2010). Reliability, construct and criterion validity of the KIDSCREEN-10 score: a short measure for children and adolescents’ well-being and health-related quality of life. Quality of Life Research: an International Journal of Quality of Life aspects of Treatment, Care and Rehabilitation, 19(10), 1487–1500. https://doi.org/10.1007/s11136-010-9706-5
Ravens-Sieberer, U., Gosch, A., Abel, T., Auquier, P., Bellach, B. M., Bruil, J., Dür, W., Power, M., Rajmil, L., European KIDSCREEN Group. (2001). Quality of life in children and adolescents: a European public health perspective. Sozial- und Praventivmedizin, 46(5), 294–302. https://doi.org/10.1007/BF01321080
Schmitt, J. C., Valiente, R. M., García-Escalera, J., Arnáez, S., Espinosa, V., Sandín, B., & Chorot, P. (2022). Prevention of Depression and Anxiety in Subclinical Adolescents: Effects of a Transdiagnostic Internet-Delivered CBT Program. International Journal of Environmental Research and Public Health, 19(9), 5365. https://doi.org/10.3390/ijerph19095365
Sandín, B., Chorot, P., Valiente, R. M., & Chorpita, B. F. (2010). Development of a 30-item version of the Revised Child Anxiety and Depression Scale. Revista De Psicopatología Y Psicología Clínica, 15(3), 165–178. https://doi.org/10.5944/rppc.vol.15.num.3.2010.4095
Sighvatsson, M. B., Salkovskis, P. M., Sigurdsson, E., Valdimarsdottir, H. B., Thorsdottir, F., & Sigurdsson, J. F. (2020). ‘You should always look at the washing machine without actually being in it!’ thematic framework analysis of patients’ understanding of transdiagnostic cognitive behaviour therapy and its mechanisms. Psychology and Psychotherapy: Theory, Research and Practice, 93(2), 258–275. https://doi.org/10.1111/papt.12220
Solmi, M., Radua, J., Olivola, M., Croce, E., Soardo, L., de Pablo, G. S., Il Shin, J., Kirkbride, J. B., Jones, P., Kim, J. H., Kim, J. Y., Carvalho, A. F., Seeman, M. V., Correll, C. U., & Fusar-Poli, P. (2022). Age at onset of mental disorders worldwide: Large-scale meta-analysis of 192 epidemiological studies. Molecular Psychiatry, 27(1), 281–295. https://doi.org/10.1038/s41380-021-01161-7
Stockings, E. A., Degenhardt, L., Dobbins, T., Lee, Y. Y., Erskine, H. E., Whiteford, H. A., & Patton, G. (2016). Preventing depression and anxiety in young people: A review of the joint efficacy of universal, selective and indicated prevention. Psychological Medicine, 46(1), 11–26. https://doi.org/10.1017/S0033291715001725
Teubert, D., & Pinquart, M. (2011). A meta-analytic review on the prevention of symptoms of anxiety in children and adolescents. Journal of Anxiety Disorders, 25(8), 1046–1059. https://doi.org/10.1016/j.janxdis.2011.07.001
van Doorn, M., Nijhuis, L. A., Egeler, M. D., Daams, J. G., Popma, A., van Amelsvoort, T., McEnery, C., Gleeson, J. F., Ory, F. G., Avis, K. A., Ruigt, E., Jaspers, M. W. M., Alvarez-Jimenez, M., & Nieman, D. H. (2021). Online Indicated Preventive Mental Health Interventions for Youth: A Scoping Review. Frontiers in Psychiatry, 12, Article 580843. https://doi.org/10.3389/fpsyt.2021.580843
van Starrenburg, M. L., Kuijpers, R. C., Kleinjan, M., Hutschemaekers, G. J., & Engels, R. C. (2017). Effectiveness of a cognitive behavioral therapy-based indicated prevention program for children with elevated anxiety levels: a randomized controlled trial. Prevention Science, 18, 31–39. https://doi.org/10.1007/s11121-016-0725-5
Vázquez, F. L., Torres, Á., Otero, P., Blanco, V., & Attkisson, C. C. (2019). Psychometric properties of the Castilian Spanish Version of the Client Satisfaction Questionnaire (CSQ-8). Current Psychology, 38(3), 829–835. https://doi.org/10.1007/s12144-017-9659-8
Verboom, C. E., Sijtsema, J. J., Verhulst, F. C., Penninx, B. W., & Ormel, J. (2014). Longitudinal associations between depressive problems, academic performance, and social functioning in adolescent boys and girls. Developmental Psychology, 50(1), 247–257. https://doi.org/10.1037/a0032547
Vivas-Fernandez, M. Garcia-Lopez, L.J. & Jimenez-Vazquez, D. (in press). Interventions for selective prevention of emotional problems in adolescents: a systematic review. Revista de Psicología Clínica con ni˜nos y adolescentes [The Journal of Clinical Psychology with Children and Adolescents].
Vivas-Fernandez, M., Garcia-Lopez, L. J., Piqueras, J. A., Muela-Martinez, J. A., Canals-Sans, J., Espinosa-Fernandez, L., Jimenez-Vazquez, D., Diaz-Castela, M. D. M., Morales-Hidalgo, P., Rivera, M., & Ehrenreich-May, J. (2023). Randomized controlled trial for selective preventive transdiagnostic intervention for adolescents at risk for emotional disorders. Child and adolescent psychiatry and mental health, 17(1), 77. https://doi.org/10.1186/s13034-023-00616-9
Vivas-Fernandez, M., Garcia-Lopez, L. J., Piqueras, Espinosa-Fernandez, L., J. A., Muela-Martinez, J. A., Jimenez-Vazquez, D., Diaz-Castela M. D. M. & Ehrenreich-May, J. (in press). A 12-month follow-up of a selective, transdiagnostic prevention intervention for adolescents at-risk for emotional disorders: results from the PROCARE+ study. Child Psychiatry & Human Development. https://doi.org/10.1007/s10578-023-01638-2
Yapan, S., Türkçapar, M. H., & Boysan, M. (2022). Rumination, automatic thoughts, dysfunctional attitudes, and thought suppression as transdiagnostic factors in depression and anxiety. Current Psychology, 41, 5896–5912. https://doi.org/10.1007/s12144-020-01086-4
Funding
This work was partially supported by the State Research Agency [PID2019-111138RB-I00/AEI/10.13039/501100011033] and the RED2022-134247-T Network for the PROmotion of EMOtional Health and Wellbeing of Adolescents (PROEMO) and the Research Network on Chronicity, Primary Care and Prevention and Health Promotion (RICAPPS).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Ethics approval
In order to test the efficacy and efficiency of PROCARE-I, we followed the Consolidated Standards of Reporting Trials (CONSORT: http://www.consort-statement.org) and the SPIRIT guidelines (Standard Protocol Items: Recommendations for Intervention Trials). The study was registered at the ClinicalTrial.gov database: ClinicalTrials.gov Identifier: NCT05252026. PROCARE-I received IRB approval and research was authorized by the bioethics committee of the University of Jaen (ID: GEN-3461-aab8-41a3-85c2-ca28-5102-cdda-8d53). The trial was planned according to internationally adopted guidelines (ICH-E6, E8 and E9), being also considered other guidelines, e.g., from the European Medicine Agency (EMA). PROCARE-I adhered to current data protection legislation (Regulation (EU) 2016/679).
Consent to participate
Informed consent was obtained from all individual participants included in the study. In addition, written informed consent was obtained from the parents of the underage participants.
Disclosure
The authors have no conflicts of interest to declare that are relevant to the content of this article.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Garcia-Lopez, LJ., Jimenez-Vazquez, D., Muela-Martinez, JA. et al. Effectiveness of a transdiagnostic indicated preventive intervention for adolescents at high risk for anxiety and depressive disorders. Curr Psychol 43, 15484–15498 (2024). https://doi.org/10.1007/s12144-023-05421-3
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12144-023-05421-3