Abstract
Purpose of Review
Medication adherence is critical for effective management of hypertension, yet half of patients with hypertension are non-adherent to medications. In this review, we describe and critically evaluate medication adherence interventions published in the past 3 years for patients with hypertension.
Recent Findings
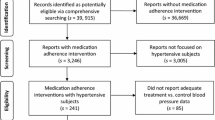
We identified 1593 articles and 163 underwent full review, of which 42 studies met the inclusion criteria. Studies were classified into eight categories: simplification of medication regimen (e.g., fixed dose combination pills); electronic Health (eHealth) tools (e.g., text messaging reminders); behavioral counseling (e.g., motivational interviewing); healthcare system changes (e.g., patient-centered medical home); patient education; multicomponent chronic disease management program; home blood pressure monitoring; and financial incentives. Studies utilizing strategies to simplify medication regimens, eHealth tools, patient education, and behavioral counseling were most likely to report positive findings.
Summary
Interventions targeting patient behavior were more likely to be associated with improvements in medication adherence compared to those targeting providers or the healthcare system. eHealth tools show promise for augmenting behavioral interventions. A major limitation of included trials was short study duration and use of self-report measures of medication adherence. Future research should explore how complex interventions that utilize a combination of evidence-based strategies and target multiple adherence behaviors (e.g., both day-to-day medication taking and long-term persistence) may be efficacious in improving medication adherence.
Similar content being viewed by others
References
Papers of particular interest, published recently, have been highlighted as: • Of importance •• Of major importance
GBD 2017 Causes of Death Collaborators. Global, regional, and national age-sex-specific mortality for 282 causes of death in 195 countries and territories, 1980–2017: a systematic analysis for the global burden of disease study 2017. Lancet. 2018;392(10159):1736–88. https://doi.org/10.1016/S0140-6736(18)32203-7
Chobanian AV, Bakris GL, Black HR, Cushman WC, Green LA, Izzo JL Jr, et al. Seventh report of the joint National Committee on prevention, detection, evaluation, and treatment of high blood pressure. Hypertension. 2003;42(6):1206–52.
Muntner P, Hardy ST, Fine LJ, Jaeger BC, Wozniak G, Levitan EB, et al. Trends in blood pressure control among US adults with hypertension, 1999-2000 to 2017-2018. JAMA. 2020;324(12):1190–200. https://doi.org/10.1001/jama.2020.14545.
Bramley TJ, et al. Relationship of blood pressure control to adherence with antihypertensive monotherapy in 13 managed care organizations. J Manag Care Pharm. 2006;12(3):239–45.
Sokol MC, McGuigan KA, Verbrugge RR, Epstein RS. Impact of medication adherence on hospitalization risk and healthcare cost. Med Care. 2005;43(6):521–30.
Chowdhury R, Khan H, Heydon E, Shroufi A, Fahimi S, Moore C, et al. Adherence to cardiovascular therapy: a meta-analysis of prevalence and clinical consequences. Eur Heart J. 2013;34(38):2940–8.
Dragomir A, Côté R, Roy L, Blais L, Lalonde L, Bérard A, et al. Impact of adherence to antihypertensive agents on clinical outcomes and hospitalization costs. Med Care. 2010;48(5):418–25.
Sabate E. Adherence to long-term therapies: evidence for action. Geneva: World Health Organization; 2003.
• Kronish IM, Thorpe CT, Voils CI. Measuring the multiple domains of medication nonadherence: findings from a Delphi survey of adherence experts. Transl Behav Med. 2019;ibz133. https://doi.org/10.1093/tbm/ibz133. This paper describes the three phases of medication adherence that should be applied in clinical research.
Cramer JA, Roy A, Burrell A, Fairchild CJ, Fuldeore MJ, Ollendorf DA, et al. Medication compliance and persistence: terminology and definitions. Value Health. 2008;11(1):44–7.
Burnier M, Egan BM. Adherence in hypertension. Circ Res. 2019;124(7):1124–40.
Nieuwlaat R, Wilczynski N, Navarro T, Hobson N, Jeffery R, Keepanasseril A, Agoritsas T, Mistry N, Iorio A, Jack S, Sivaramalingam B, Iserman E, Mustafa RA, Jedraszewski D, Cotoi C, Haynes RB. Interventions for enhancing medication adherence. Cochrane Database Syst Rev. 2014;2014(11):CD000011. https://doi.org/10.1002/14651858.CD000011.pub4.
Crilly P, Kayyali R. A systematic review of randomized controlled trials of telehealth and digital technology use by community pharmacists to improve public health. Pharmacy (Basel). 2020;8(3):E137.
Morawski K, Ghazinouri R, Krumme A, Lauffenburger JC, Lu Z, Durfee E, et al. Association of a Smartphone application with medication adherence and blood pressure control: the MedISAFE-BP randomized clinical trial. JAMA Intern Med. 2018;178(6):802–9.
Sartori AC, Rodrigues Lucena TF, Takáo Lopes C, Picinin Bernuci M, Yamaguchi MU. Educational Intervention Using WhatsApp on Medication Adherence in Hypertension and Diabetes Patients: A Randomized Clinical Trial. Telemed J E Health. 2020. https://doi.org/10.1089/tmj.2019.0305.
Turner BJ, Hollenbeak CS, Liang Y, Pandit K, Joseph S, Weiner MG. A randomized trial of peer coach and office staff support to reduce coronary heart disease risk in African-Americans with uncontrolled hypertension. J Gen Intern Med. 2012;27(10):1258–64.
Zhai P, Hayat K, Ji W, Li Q, Shi L, Atif N, et al. Efficacy of text messaging and personal consultation by pharmacy students among adults with hypertension: randomized controlled trial. J Med Internet Res. 2020;22(5):e16019.
Harvin LA, Winter DM, Hoover EL, Lewis LM. A faith-based intervention to improve hypertension management among African Americans. J Christ Nurs. 2020;37(1):38–45.
Kini V, Ho PM. Interventions to improve medication adherence: a review. Jama. 2018;320(23):2461–73.
Persell SD, Karmali KN, Lazar D, Friesema EM, Lee JY, Rademaker A, et al. Effect of electronic health record-based medication support and nurse-led medication therapy management on hypertension and medication self-management: a randomized clinical trial. JAMA Intern Med. 2018;178(8):1069–77.
Persell SD, Peprah YA, Lipiszko D, Lee JY, Li JJ, Ciolino JD, et al. Effect of home blood pressure monitoring via a smartphone hypertension coaching application or tracking application on adults with uncontrolled hypertension: a randomized clinical trial. JAMA Netw Open. 2020;3(3):e200255.
Abughosh S, Wang X, Serna O, Esse T, Mann A, Masilamani S, et al. A motivational interviewing intervention by pharmacy students to improve medication adherence. J Manag Care Special Pharm. 2017;23(5):549–60.
Bolarinwa O, Juni MH, Nor Afiah MZ, Salmiah MS, Akande TM. Mid-term impact of home-based follow-up care on health-related quality of life of hypertensive patients at a teaching hospital in Ilorin, Nigeria. Niger J Clin Pract. 2019;22(1):69–78.
Sheilini M, Hande HM, Prabhu MM, Pai MS, George A. Impact of multimodal interventions on medication nonadherence among elderly hypertensives: a randomized controlled study. Patient Prefer Adherence. 2019;13:549–59.
van der Laan DM, et al. Effectiveness of a patient-tailored, Pharmacist-Led Intervention Program to Enhance Adherence to Antihypertensive Medication: The CATI Study. Front Pharmacol. 2018;9:1057.
Mirniam AA, Habibi Z, Khosravi A, Sadeghi M, Eghbali-Babadi M. A clinical trial on the effect of a multifaceted intervention on blood pressure control and medication adherence in patients with uncontrolled hypertension. ARYA Atheroscler. 2019;15(6):267–74.
Amer M, et al. Impact of pharmacist's intervention on disease related knowledge, medication adherence, HRQoL and control of blood pressure among hypertensive patients. Pak J Pharm Sci. 2018;31(6 (Supplementary):2607–16.
Delavar F, Pashaeypoor S, Negarandeh R. The effects of self-management education tailored to health literacy on medication adherence and blood pressure control among elderly people with primary hypertension: a randomized controlled trial. Patient Educ Couns. 2020;103(2):336–42.
Yazdanpanah Y. Effect of an educational program based on health belief model on medication adherence in elderly patients with hypertension. Evid Based Care J. 2019;9(1):12.
•• Shen Y, et al. Effectiveness of low-cost reminder package combined with case-based health education to improve hypertensive patients' medication adherence: a clustered randomized controlled trial. Patient Prefer Adherence. 2019;13:1083–92. This study demonstrated the importance of using multicomponent strategies that include family members to improve medication adherence in patients with hypertension.
Tan BY, et al. Assessment of medication adherence and the costs associated with a calendar blister pack intervention among hypertensive patients in Malaysia: a randomized controlled trial. SAGE Open Med. 2017;5:2050312117709189.
•• Sarfo FS, et al. Phone-based intervention for blood pressure control among Ghanaian stroke survivors: a pilot randomized controlled trial. Int J Stroke. 2019;14(6):630–8. This study demonstrates the efficacy of a multicomponent intervention that combines innovative tools (Smartphone app) with traditional methods (nurse case management) to improve medication adherence.
Márquez Contreras E, Márquez Rivero S, Rodríguez García E, López-García-Ramos L, Carlos Pastoriza Vilas J, Baldonedo Suárez A, et al. Specific hypertension smartphone application to improve medication adherence in hypertension: a cluster-randomized trial. Curr Med Res Opin. 2019;35(1):167–73.
Varleta P, Acevedo M, Akel C, Salinas C, Navarrete C, García A, et al. Mobile phone text messaging improves antihypertensive drug adherence in the community. J Clin Hypertens. 2017;19(12):1276–84.
Buis L, Hirzel L, Dawood RM, Dawood KL, Nichols LP, Artinian NT, et al. Text messaging to improve hypertension medication adherence in African Americans from primary care and emergency department settings: results from two randomized feasibility studies. JMIR Mhealth Uhealth. 2017;5(2):e9.
Chandler J, et al. Impact of a culturally tailored mHealth medication regimen self-management program upon blood pressure among hypertensive Hispanic adults. Int J Environ Res Public Health. 2019;16(7):1226.
Joshi R, Agrawal T, Fathima F, Usha T, Thomas T, Misquith D, et al. Cardiovascular risk factor reduction by community health workers in rural India: a cluster randomized trial. Am Heart J. 2019;216:9–19.
Kim M. Effects of customized long-message service and phone-based health-coaching on elderly people with hypertension. Iran J Public Health. 2019;48(4):655–63.
Tamblyn R, Winslade N, Qian CJ, Moraga T, Huang A. What is in your wallet? A cluster randomized trial of the effects of showing comparative patient out-of-pocket costs on primary care prescribing for uncomplicated hypertension. Implement Sci. 2018;13(1):7.
Schoenthaler A, de la Calle F, Pitaro M, Lum A, Chaplin W, Mogavero J, et al. A systems-level approach to improving medication adherence in hypertensive Latinos: a randomized control trial. J Gen Intern Med. 2020;35(1):182–9.
Shen Y, Peng X, Wang M, Zheng X, Xu G, Lü L, et al. Family member-based supervision of patients with hypertension: a cluster randomized trial in rural China. J Hum Hypertens. 2017;31(1):29–36.
Ozpancar N, Pakyuz SC, Topcu B. Hypertension management: what is the role of case management? Rev Esc Enferm USP. 2017;51:e03291.
Muhammad J, Jamial MM, Ishak A. Home blood pressure monitoring has similar effects on office blood pressure and medication compliance as usual care. Korean J Fam Med. 2019;40(5):335–43.
da Silva Mattei ÂT, et al. Nursing case management for people with hypertension in primary health care: a randomized controlled trial. Res Nurs Health. 2020;43(1):68–78.
Cuffee YL, Sciamanna C, Gerin W, Lehman E, Cover L, Johnson AA, et al. The effectiveness of home blood pressure on 24-hour blood pressure control: a randomized controlled trial. Am J Hypertens. 2019;32(2):186–92.
Aghakhani N, Parizad N, Soltani B, Khademvatan K, Rahimi Z. The effect of the blended education program on treatment concordance of patients with hypertension: a single-blind randomized, controlled trial. J Vasc Nurs. 2019;37(4):250–6.
Lauffenburger JC, Shrank WH, Bitton A, Franklin JM, Glynn RJ, Krumme AA, et al. Association between patient-centered medical homes and adherence to chronic disease medications: a cohort study. Ann Intern Med. 2017;166(2):81–8.
McWilliams JM, Najafzadeh M, Shrank WH, Polinski JM. Association of changes in medication use and adherence with accountable care organization exposure in patients with cardiovascular disease or diabetes. JAMA Cardiol. 2017;2(9):1019–23.
Kim J-A, Kim E-S, Lee E-K. Evaluation of the chronic disease management program for appropriateness of medication adherence and persistence in hypertension and type-2 diabetes patients in Korea. Medicine. 2017;96(14):e6577.
Bartlett LE, Pratt N, Roughead EE. Does a fixed-dose combination of amlodipine and atorvastatin improve persistence with therapy in the Australian population? Curr Med Res Opin. 2018;34(2):305–11.
Ho CT, Tung YC, Chou SH, Hsiao FC, Lin YS, Chang CJ, et al. Clinical outcomes in hypertensive patients treated with a single-pill fixed-dose combination of renin-angiotensin system inhibitor and thiazide diuretic. J Clin Hypertens (Greenwich). 2018;20(12):1731–8.
Fleig SV, Weger B, Haller H, Limbourg FP. Effectiveness of a fixed-dose, single-pill combination of perindopril and amlodipine in patients with hypertension: a non-interventional study. Adv Ther. 2018;35(3):353–66.
Kim SJ, Kwon OD, Cho BL, Oh SW, Lee CM, Choi HC. Effects of combination drugs on antihypertensive medication adherence in a real-world setting: a Korean Nationwide study. BMJ Open. 2019;9(6):e029862.
Verma AA, Khuu W, Tadrous M, Gomes T, Mamdani MM. Fixed-dose combination antihypertensive medications, adherence, and clinical outcomes: a population-based retrospective cohort study. PLoS Med. 2018;15(6):e1002584.
Doshi JA, et al. Synchronized prescription refills and medication adherence: a retrospective claims analysis. Am J Manag Care. 2017;23(2):98–104.
Moorhead P, et al. Efficacy and safety of a medication dose reminder feature in a digital health offering with the use of sensor-enabled medicines. J Am Pharm Assoc (2003). 2017;57(2):155–161.e1.
Yeung K, Basu A, Marcum ZA, Watkins JB, Sullivan SD. Impact of a value-based formulary in three chronic disease cohorts. Am J Manag Care. 2017;23(3 Suppl):S46–s53.
Tan BY, Shafie AA, Hassali MAA, Saleem F, Muneswarao J. Improving medication adherence through calendar packaging: results of a randomized controlled trial among hypertensive patients. J Pharm Health Serv Res. 2017;8(2):115–22.
Zare S, Rezaee R, Aslani A, Shirdeli M, Kojuri J. Moving toward community based telehealth services using mHealth for hypertensive patients. Int J Technol Assess Health Care. 2019;35(5):379–83.
•• Son K-J, et al. A community-based intervention for improving medication adherence for elderly patients with hypertension in Korea. Int J Environ Res Public Health. 2019;16(5):721. This study describes a multilevel intervention strategy that combines approaches at the level of the health system with that of the community to make an impact on patient medication adherence.
Vrijens B, et al. Current situation of medication adherence in hypertension. Front Pharmacol. 2017;8:100.
Salam A, et al. Efficacy and safety of dual combination therapy of blood pressure-lowering drugs as initial treatment for hypertension: a systematic review and meta-analysis of randomized controlled trials. J Hypertens. 2019;37(9):1768–74.
Hong SH, Wang J, Tang J. Dynamic view on affordability of fixed-dose combination antihypertensive drug therapy. Am J Hypertens. 2013;26(7):879–87.
DiPette DJ, et al. Fixed-dose combination pharmacologic therapy to improve hypertension control worldwide: clinical perspective and policy implications. J Clin Hypertens. 2019;21(1):4–15.
Conn VS, Ruppar TM, Chase JAD, Enriquez M, Cooper PS. Interventions to improve medication adherence in hypertensive patients: systematic review and meta-analysis. Curr Hypertens Rep. 2015;17(12):94.
Conn VS, Ruppar TM. Medication adherence outcomes of 771 intervention trials: systematic review and meta-analysis. Prev Med. 2017;99:269–76.
Schroeder K, Fahey T, Ebrahim S, Peters TJ. Adherence to long-term therapies: recent WHO report provides some answers but poses even more questions. J Clin Epidemiol. 2004;57(1):2–3.
•• De Geest S, et al. ESPACOMP Medication Adherence Reporting Guideline (EMERGE). Ann Intern Med. 2018;169(1):30–5. This paper outlines the reporting guidelines all researcher should employ when conducting research and publishing findings related to medication adherence.
Rose AJ, et al. Effects of daily adherence to antihypertensive medication on blood pressure control. J Clin Hypertens (Greenwich, Conn). 2011;13(6):416–21.
van der Kleij R, Kasteleyn MJ, Meijer E, Bonten TN, Houwink EJF, Teichert M, et al. SERIES: eHealth in primary care. Part 1: concepts, conditions and challenges. Eur J Gen Pract. 2019;25(4):179–89.
Acknowledgments
We would like to acknowledge Mr. Timothy Roberts for his assistance in developing the search strategy for this review.
Funding
Preparation of this article was supported in part by the National Institutes of Health grant T32HL129953 - Mentoring URM Scientists in Behavioral and Cardiovascular Health to Increase Academic Workforce Diversity and American Heart Association grant 19POST34380633. The sponsors had no role in the study design, in the collection, analysis, or interpretation of the findings, in writing the present report, or in the decision to submit the manuscript for publication.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of Interest
The authors declare no conflicts of interest relevant to this manuscript.
Human and Animal Rights and Informed Consent
This article does not contain any studies with human or animal subjects performed by any of the authors.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
This article is part of the Topical Collection on Implementation to Increase Blood Pressure Control: What Works?
Appendix A. Review Search Strategy
Appendix A. Review Search Strategy
((("hypertension"[MeSH Terms] OR hypertension[Text Word]) OR blood pressure[Text Word]) OR ("blood pressure"[MeSH Terms] OR "blood pressure determination"[MeSH Terms] OR "arterial pressure"[MeSH Terms])) AND ("Medication Adherence"[Mesh] OR "medication adherence"[tw] OR "medication nonadherence"[tw]) AND (((clinical[Title/Abstract] AND trial[Title/Abstract]) OR clinical trials as topic[MeSH Terms] OR clinical trial[Publication Type] OR random*[Title/Abstract] OR random allocation[MeSH Terms] OR therapeutic use[MeSH Subheading]))
“Medication Adherence” [Mesh] OR adherence[tw] OR nonadherence[tw] OR … adherence, adherent, compliance, compliant, noncompliant, noncompliance, nonadherence, nonadherent
AND ((((((((((hypertension[MeSH Terms]) OR hypertension[Text Word]) OR blood pressure[Text Word]) OR blood pressure[MeSH Terms])
AND (((((Prospective Studies[MeSH Terms]) OR Cohort Studies[MeSH Terms]) OR Followup Studies[MeSH Terms]) OR Longitudinal Studies[MeSH Terms]) AND Cross Sectional Studies[MeSH Terms])
Rights and permissions
About this article
Cite this article
Izeogu, C., Kalinowski, J. & Schoenthaler, A. Strategies to Improve Adherence to Anti-Hypertensive Medications: a Narrative Review. Curr Hypertens Rep 22, 105 (2020). https://doi.org/10.1007/s11906-020-01115-4
Accepted:
Published:
DOI: https://doi.org/10.1007/s11906-020-01115-4