Abstract
Background
Fecal urgency is classically associated with diarrhea, but is also common in individuals with normal bowel habits or constipation. Its etiology, particularly in non-diarrhea individuals, is unclear.
Methods
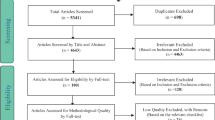
We examined data from 368 individuals with and without diarrhea who underwent three-dimensional high-resolution anorectal manometry and balloon expulsion test. All patients completed the Rome III constipation module and the pelvic floor distress inventory (PDFI-20) survey. Patients were considered to have fecal urgency if they reported being bothered “moderately” or “quite a bit” by it in the past 3 months.
Results
A total of 103 patients (28.0%) met our definition of fecal urgency. These patients were significantly more likely to meet criteria for irritable bowel syndrome and to report fecal incontinence, urinary incontinence, and diarrhea. Fecal urgency was associated with rectal hypersensitivity in those with diarrhea, but not in those without diarrhea. Fecal urgency was associated with urinary urge incontinence in those without diarrhea, but not those with diarrhea.
Conclusions
In patients with diarrhea, fecal urgency is associated with rectal hypersensitivity, whereas in patients without diarrhea, fecal urgency is associated with urinary urge incontinence. This suggests that fecal urgency has different pathophysiological mechanisms in patients with different underlying bowel habits.

Similar content being viewed by others
References
Drossman DA, Sandler RS, Broom CM, McKee DC. Urgency and fecal soiling in people with bowel dysfunction. Dig Dis Sci. 1986;31:1221–1225.
Heaton KW, Ghosh S, Braddon FE. How bad are the symptoms and bowel dysfunction of patients with the irritable bowel syndrome? A prospective, controlled study with emphasis on stool form. Gut. 1991;32:73–79.
Talley NJ, Weaver AL, Zinsmeister AR, Melton LJ. Self-reported diarrhea: what does it mean? Am J Gastroenterol. 1994;89:1160–1164.
Rangan V, Mitsuhashi S, Singh P, et al. Risk factors for fecal urgency among individuals with and without diarrhea, based on data from the national health and nutrition examination survey. Clin Gastroenterol Hepatol. 2018;16:1450–1458.e2.
Mangel AW, Wang J, Sherrill B, Gnanasakthy A, Ervin C, Fehnel SE. Urgency as an endpoint in irritable bowel syndrome. Gastroenterol Res. 2011;4:9–12.
Shin A, Lembo A. IBS in America: Survey Summary Findings [Internet]. American Gastroenterology Association; 2015 [cited 2018 Oct 1]. Available from http://www.multivu.com/players/English/7634451-aga-ibs-in-america-survey/docs/survey-findings-pdf-635473172.pdf.
Bharucha AE, Zinsmeister AR, Locke GR, et al. Risk factors for fecal incontinence: a population-based study in women. Am J Gastroenterol. 2006;101:1305–1312.
Bharucha AE, Seide BM, Zinsmeister AR, Melton LJ. Relation of bowel habits to fecal incontinence in women. Am J Gastroenterol. 2008;103:1470–1475.
Bharucha AE, Fletcher JG, Melton LJ, Zinsmeister AR. Obstetric trauma, pelvic floor injury and fecal incontinence: a population-based case-control study. Am J Gastroenterol. 2012;107:902–911.
Bharucha AE, Zinsmeister AR, Schleck CD, Melton LJ. Bowel disturbances are the most important risk factors for late onset fecal incontinence: a population-based case-control study in women. Gastroenterology. 2010;139:1559–1566.
Staller K, Song M, Grodstein F, et al. Increased long-term dietary fiber intake is associated with a decreased risk of fecal incontinence in older women. Gastroenterology. 2018;155:661–667.e1.
Schiller LR, Pardi DS, Sellin JH. Chronic diarrhea: diagnosis and management. Clin Gastroenterol Hepatol. 2017;15:182–193.e3.
Basilisco G, De Marco E, Tomba C, Cesana BM. Bowel urgency in patients with irritable bowel syndrome. Gastroenterology. 2007;132:38–44.
Naliboff BD, Munakata J, Fullerton S, et al. Evidence for two distinct perceptual alterations in irritable bowel syndrome. Gut. 1997;41:505–512.
Slater BJ, Plusa SM, Smith AN, Varma JS. Rectal hypersensitivity in the irritable bowel syndrome. Int J Colorectal Dis. 1997;12:29–32.
Grinsvall C, Törnblom H, Tack J, Van Oudenhove L, Simrén M. Psychological factors selectively upregulate rectal pain perception in hypersensitive patients with irritable bowel syndrome. Neurogastroenterol Motil. 2015;27:1772–1782.
Chan CLH, Scott SM, Williams NS, Lunniss PJ. Rectal hypersensitivity worsens stool frequency, urgency, and lifestyle in patients with urge fecal incontinence. Dis Colon Rectum. 2005;48:134–140.
Bharucha AE, Fletcher JG, Harper CM, et al. Relationship between symptoms and disordered continence mechanisms in women with idiopathic faecal incontinence. Gut. 2005;54:546–555.
Siproudhis L, El Abkari M, El Alaoui M, Juguet F, Bretagne JF. Low rectal volumes in patients suffering from fecal incontinence: what does it mean? Aliment Pharmacol Ther. 2005;22:989–996.
Caetano AC, Santa-Cruz A, Rolanda C. Digital Rectal examination and balloon expulsion test in the study of defecatory disorders: Are they suitable as screening or excluding tests? Can J Gastroenterol Hepatol. 2016;2016:8654314.
Chiarioni G, Kim SM, Vantini I, Whitehead WE. Validation of the balloon evacuation test: reproducibility and agreement with findings from anorectal manometry and electromyography. Clin Gastroenterol Hepatol. 2014;12:2049–2054.
Zar S, Benson MJ, Kumar D. Rectal afferent hypersensitivity and compliance in irritable bowel syndrome: differences between diarrhoea-predominant and constipation-predominant subgroups. Eur J Gastroenterol Hepatol. 2006;18:151–158.
Qin C, Malykhina AP, Akbarali HI, Foreman RD. Cross-organ sensitization of lumbosacral spinal neurons receiving urinary bladder input in rats with inflamed colon. Gastroenterology. 2005;129:1967–1978.
Christianson JA, Liang R, Ustinova EE, Davis BM, Fraser MO, Pezzone MA. Convergence of bladder and colon sensory innervation occurs at the primary afferent level. Pain. 2007;128:235–243.
Matsumoto S, Hashizume K, Wada N, et al. Relationship between overactive bladder and irritable bowel syndrome: a large-scale internet survey in Japan using the overactive bladder symptom score and Rome III criteria. BJU Int. 2013;111:647–652.
Cukier JM, Cortina-Borja M, Brading AF. A case-control study to examine any association between idiopathic detrusor instability and gastrointestinal tract disorder, and between irritable bowel syndrome and urinary tract disorder. Br J Urol. 1997;79:865–878.
Carter D, Beer-Gabel M. Lower urinary tract symptoms in chronically constipated women. Int Urogynecology J. 2012;23:1785–1789.
Kim KS, Kim H-J, Lee SH, Cho ST, Moon HS. Association between irritable bowel syndrome and overactive bladder: a research survey. Urology. 2017;109:88–93.
Prather CM, Ortiz-Camacho CP. Evaluation and treatment of constipation and fecal impaction in adults. Mayo Clin Proc. 1998;73:881–886. (quiz 887).
Gladman MA, Lunniss PJ, Scott SM, Swash M. Rectal hyposensitivity. Am J Gastroenterol. 2006;101:1140–1151.
Nordenstam JF, Altman DH, Mellgren AF, Rothenberger DA, Zetterström JP. Impaired rectal sensation at anal manometry is associated with anal incontinence one year after primary sphincter repair in primiparous women. Dis Colon Rectum. 2010;53:1409–1414.
Loganathan A, Schloithe AC, Hakendorf P, Liyanage CM, Costa M, Wattchow D. Prolonged pudendal nerve terminal motor latency is associated with decreased resting and squeeze pressures in the intact anal sphincter. Colorectal Dis. 2013;15:1410–1415.
Boyle DJ, Knowles CH, Murphy J, et al. The effects of age and childbirth on anal sphincter function and morphology in 999 symptomatic female patients with colorectal dysfunction. Dis Colon Rectum. 2012;55:286–293.
Mion F, Garros A, Brochard C, Vitton V, Ropert A, Bouvier M, et al. 3D High-definition anorectal manometry: Values obtained in asymptomatic volunteers, fecal incontinence and chronic constipation. Results of a prospective multicenter study (NOMAD). Neurogastroenterol Motil Off J Eur Gastrointest Motil Soc. 2017;29(8).
Rao SS, Hatfield R, Soffer E, Rao S, Beaty J, Conklin JL. Manometric tests of anorectal function in healthy adults. Am J Gastroenterol. 1999;94:773–783.
Noelting J, Ratuapli SK, Bharucha AE, Harvey DM, Ravi K, Zinsmeister AR. Normal values for high-resolution anorectal manometry in healthy women: effects of age and significance of rectoanal gradient. Am J Gastroenterol. 2012;107:1530–1536.
Wickramasinghe DP, Perera CS, Senanayake H, Samarasekera DN. Three-dimensional anorectal manometry findings in primigravida. Dig Dis Sci. 2015;60:3764–3770.
Coss-Adame E, Rao SSC, Valestin J, Ali-Azamar A, Remes-Troche JM. Accuracy and reproducibility of high-definition anorectal manometry and pressure topography analyses in healthy subjects. Clin Gastroenterol Hepatol. 2015;13:1143–1150.e1.
Lee HJ, Jung KW, Han S, et al. Normal values for high-resolution anorectal manometry/topography in a healthy Korean population and the effects of gender and body mass index. Neurogastroenterol Motil. 2014;26:529–537.
Li Y, Yang X, Xu C, Zhang Y, Zhang X. Normal values and pressure morphology for three-dimensional high-resolution anorectal manometry of asymptomatic adults: a study in 110 subjects. Int J Colorectal Dis. 2013;28:1161–1168.
Verkuijl SJ, Trzpis M, Broens PMA. Normal rectal filling sensations in patients with an enlarged rectum. Dig Dis Sci. 2019;64:1312–1319.
Funding
Research reported in this publication was supported by the National Institutes of Health under Award Number R01AT00857303 and T32DK007760
Author information
Authors and Affiliations
Contributions
AL and VR designed the research study. VR, PS, and WH analyzed the data. VR, JN, and PS wrote the paper. JN, PS, JI, SB, and AL provided key editorial input into the paper
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Rangan, V., Nee, J., Singh, P. et al. Fecal Urgency: Clinical and Manometric Characteristics in Patients With and Without Diarrhea. Dig Dis Sci 65, 3679–3687 (2020). https://doi.org/10.1007/s10620-020-06349-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10620-020-06349-5