Abstract
Background
Little attention has been paid to family-wide repercussions of a child’s celiac disease diagnosis and concomitant gluten-free diet management.
Aims
We quantitatively and qualitatively describe positive and negative family-wide effects of a child’s celiac disease diagnosis and disease management.
Methods
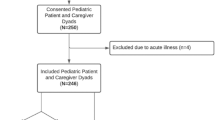
We interviewed 16 families with at least one child currently following a gluten-free diet, with a biopsy-confirmed celiac disease diagnosis ≥ 1 year prior. Mothers and fathers independently rated child’s dietary adherence, concern about child’s health status, burden in caring for child’s dietary needs, and level of change in various aspects of life post- diagnosis. Children rated their own celiac-specific quality of life through a validated scale. Seventy-one in-depth semi-structured interviews were conducted with 16 children with celiac disease, 31 parents, and 24 siblings.
Results
Mothers and fathers rated the effects of their child’s celiac disease differently, with mothers reporting more lifestyle changes and heavier burden. Negative and positive themes emerged from the interviews. Mothers felt the burden of managing a gluten-free diet. Fathers felt guilty for carrying a celiac disease-associated gene and both fathers and siblings regretted limited food choices at restaurants and home. The need to be a more creative cook was seen as a positive effect by mothers. Fathers appreciated new family traditions. Siblings felt they had developed empathy for others. A framework is proposed to illustrate these family-wide interactions.
Conclusions
A child’s celiac disease diagnosis and disease management affects the entire family. Our results will inform family-centered interventions that maximize quality of life for families.


Similar content being viewed by others
References
Lebwohl B, Sanders DS, Green PHR. Coeliac disease. Lancet. 2018;391:70–81.
Ludvigsson JF, Murray JA. Epidemiology of celiac disease. Gastroenterol Clin North Am. 2019;48:1–18.
Singh P, Arora S, Lal S, Strand TA, Makharia GK. Risk of celiac disease in the first- and second-degree relatives of patients with celiac disease: a systematic review and meta-analysis. Am J Gastroenterol. 2015;110:1539–1548.
Ludvigsson JF. Mortality and malignancy in celiac disease. Gastro Endosc Clin N Am. 2012;22:705–722.
Myléus A, Reilly NR, Green PHR. Rate, risk factors and outcomes of nonadherence in pediatric patients with celiac disease: a systematic review. Clin Gastroenterol Hepatol. 2020;18:562–573.
Lebwohl B, Michaëlsson K, Green PH, Ludvigsson JF. Persistent mucosal damage and risk of fracture in celiac disease. J Clin Endocrinol Metab. 2014;99:609–616.
De Lorenzo CM, Xikota JC, Wayhs MC, Nassar SM, de Souza Pires MM. Evaluation of the quality of life of children with celiac disease and their parents: a case-control study. Qual Life Res. 2012;1:77–85.
Lee AR, Ng DL, Zivin J, Green PH. Economic burden of a gluten-free diet. J Hum Nutr Diet. 2007;20:423–430.
Meyer S, Rosenblum S. Activities, participation and quality of life concepts in children and adolescents with celiac disease: a scoping review. Nutrients. 2017;9:929.
Wolf RL, Lebwohl B, Lee AR, et al. Hypervigilance to a gluten-free diet and decreased quality of life in teenagers and adults with celiac disease. Dig Dis Sci. 2018;63:1438–1448.
Bacigalupe G, Plocha A. Celiac is a social disease: family challenges and strategies. Fam Syst Health. 2015;33:46–54.
Erickson K, Freeborn D, Roper SO, Mandleco B, Anderson A, Dyches T. Parent experiences raising young people with type 1 diabetes and celiac disease. J Pediatr Nurs. 2015;30:353–363.
Errichiello S, Esposito O, Di Mase R, et al. Celiac disease: predictors of compliance with a gluten-free diet in adolescents and young adults. J Pediatr Gastroenterol Nutr. 2010;50:54–60.
Lee AR, Wolf R, Contento I, Verdeli H, Green PH. Coeliac disease: the association between quality of life and social support network participation. J Hum Nutr Diet. 2015;29:383–390.
Olsson C, Lyon P, Hörnell A, Ivarsson A, Sydner YM. Food that makes you different: the stigma experienced by adolescents with celiac disease. Qual Health Res. 2009;19:976–984.
Roy A, Minaya M, Monegro M, et al. Partner burden: a common entity in celiac disease. Dig Dis Sci. 2016;61:3451–3459.
Sverker A, Hensing G, Hallert C. ‘Controlled by food’-lived experiences of coeliac disease. J Hum Nutr Diet. 2005;18:171–180.
Sverker A, Ostlund G, Hallert C, Hensing G. Sharing life with a gluten-intolerant person—the perspective of close relatives. J Hum Nutr Diet. 2007;20:412–422.
Smith JA, Flowers P, Larkin M. Interpretative Phenomenological Analysis: Theory, Method and Research. London: Sage; 2009.
Fade SA, Swift JA. Qualitative research in nutrition and dietetics: data analysis issues. J Hum Nutr Diet. 2011;24:106–114.
Green J, Willis K, Hughes E, et al. Generating best evidence from qualitative research: the role of data analysis. Aust N Z J Public Health. 2007;31:545–550.
Pilnick A, Swift JA. Qualitative research in nutrition and dietetics: assessing quality. J Hum Nutr Diet. 2011;24:209–214.
Power EM. De-centering the text: exploring the potential for visual methods in the sociology of food. J Study Food Soc. 2003;6:9–20.
Kendall H, Brennan M, Seal C, Ladha C, Kuznesof S. Behind the kitchen door: a novel mixed method approach for exploring the food previsioning practices of the older consumer. Food Qual Prefer. 2016;53:105–116.
Wills WJ, Dickinson AM, Meah A, Short F. Reflections of the use of visual methods in a qualitative study of domestic kitchen practices. Sociology. 2016;50:470–485.
Leffler DA, Dennis M, Edwards George JB, et al. A simple validated gluten-free diet adherence survey for adults with celiac disease. Clin Gastroenterol Hepatol. 2009;7:530–536.
Biagi F, Bianchi PI, Marchese A, et al. A score that verifies adherence to a gluten-free diet: a cross-sectional, multicentre validation in real clinical life. Br J Nutr. 2012;108:1884–1888.
Della Vida FL, Lacorte D, Retetangos C, Selarno A, Grondona A, Molinazzi D. Gluten free diet in coeliac children: are there any factors affecting adherence? Dig Liver Dis. 2017;49:266–267.
Jordan NE, Li Y, Magrini D, et al. Development and validation of a celiac disease quality of life instrument for North American children. J Pediatr Gastroenterol Nutr. 2013;57:477–486.
Ferretti F, Branchi F, Dell’Osso B, Conte D, Elli L. Coping with celiac disease: how heavy is the burden for caregivers? Rev Esp Enferm Dig. 2017;109:250–255.
IBM SPSS Statistics for Windows, version 23 (IBM Corp., Armonk, N.Y., USA)’ [6].Apr 17, 2015.
Gerstle JF, Varenne H, Contento I. Post-diagnosis family adaptation influences glycemic control in women with type 2 diabetes meillitus. J Am Diet Assoc. 2001;101:918–922.
Weisbrod VM, Silvester JA, Raber C, McMahon J, Coburn SS, Kerzner B. Preparation of gluten-free foods alongside gluten-containing food may not always be as risky for celiac patients as diet guides suggest. Gastroenterology. 2019;19:1340–1341.
Ludvigsson JF, Lebwohl B, Chen Q, et al. Anxiety after coeliac disease diagnosis predicts mucosal healing: a population-based study. Aliment Pharmacol Ther. 2018;48:1091–1098.
Acknowledgments
This study was funded by the Provost Investment Fund at Teachers College Columbia University and in part by Columbia University’s CTSA grant No. UL1 TR000040 from NCATS/NIH. BL is supported by The Louis and Gloria Flanzer Philanthropic Trust. Dr. Anne Lee receives grant support from Dr. Schar.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflicts of interest
CR, HL, RW, PZ, NR declare they have no conflicts of interest. AL is on the Medical Advisory Boards for Dr Schar Foods and the University of Monash Low FODMAP Diet. BL serves as a consultant for Takeda, Innovate, and Anokion. PG consultant to Janssen/J&J, Innovate, ImmunogenX. Speakers bureau—Abbvie.
Ethnical approval
All procedures performed in this study involving human participants were in accordance with ethical standards of the institutional review boards at both Columbia University Medical Center and Teachers College, Columbia University and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Informed consent
Written informed consent was obtained from all individual participants included in the study.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Russo, C., Wolf, R.L., Leichter, H.J. et al. Impact of a Child’s Celiac Disease Diagnosis and Management on the Family. Dig Dis Sci 65, 2959–2969 (2020). https://doi.org/10.1007/s10620-020-06316-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10620-020-06316-0