Abstract
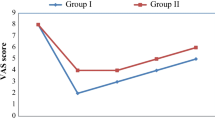
The efficacy of neurolytic coeliac plexus block (NCPB) guided by computerized tomography (CT) was compared with pharmacological therapy in the treatment of pain due to pancreatic cancer. The study involved 56 patients who were placed randomly in either a NCPB group and pharmacological therapy group. At day 1, 7, and 14, the visual analogue scale (VAS) pain scores of the NCPB group were significantly lower than those of the pharmacological therapy group (P < 0.01), with values of 1.3 ± 0.8 versus 4.1 ± 0.9, 1.7 ± 1.1 versus 3.1 ± 1.1, and 2.0 ± 1.1 versus 2.9 ± 0.6, respectively. However, the differences in the improvement of quality of life (QOL) between two groups were not statistically significant. Moreover, the dose of opioid was significantly lower in the patients of group 1 than those of group 2, while the complications related to NCPB were transient. We therefore concludes that CT-guided NCPB with alcohol is an effective and safe modality in the management of intractable pancreatic cancer pain.

Similar content being viewed by others
References
Carr DB, Goudas LC, Balk EM, Bloch R, Ioannidis JP, Lau J (2004) Evidence report on the treatment of pain in cancer patients. J Natl Cancer Inst Monogr 32:23–31
Fallon M, McConnell S (2006) The principles of cancer pain management. Clin Med 6:136–139
Caraceni A, Portenoy RK (1996) Pain management in patients with pancreatic carcinoma. Cancer 78:639–653
Alter CL (1996) Palliative and supportive care of patients with pancreatic cancer. Semin Oncol 23:229–240
Cariati M, De Martini G, Pretolesi F, Roy MT (2002) CT-guided superior hypogastric plexus block. J Comput Assist Tomogr 26:428–431
McNicol E, Horowicz-Mehler N, Fisk RA, Bennett K, Gialeli-Goudas M, Chew PW, Lau J, Carr D (2003) Management of opioid side effects in cancer-related and chronic noncancer pain: a systematic review. J Pain 4:231–256
Brown DL, Bulley CK, Quiel EL (1987) Neurolytic celiac plexus block for pancreatic cancer pain. Anesth Analg 66:869–873
Regan JM, Peng P (2000) Neurophysiology of cancer pain. Cancer Control 7:111–119
Lieberman RP, Nance PN, Cuka DJ (1988) Anterior approach to celiac plexus block during interventional biliary procedures. Radiology 167:562–564
Romanelli DF, Beckmann CF, Heiss FW (1993) Celiac plexus block: efficacy and safety of the anterior approach. Am J Roentgenol 160:497–500
Mercadante S, Catala E, Arcuri E, Casuccio A (2003) Celiac plexus block for pancreatic cancer pain: factors influencing pain, symptoms and quality of life. J Pain Symptom Manage 26:1140–1147
de Leon-Casasola OA (2000) Critical evaluation of chemical neurolysis of the sympathetic axis for cancer pain. Cancer Control 7:142–148
Mercadante S, Fulfaro F, Casuccio A (2002) Pain mechanisms involved and outcome in advanced cancer patients with possible indications for celiac plexus block and superior hypogastric plexus block. Tumori 88:243–245
Vranken JH, Zuurmond WW, de Lange JJ (2001) Increasing the efficacy of a celiac plexus block in patients with severe pancreatic cancer pain. J Pain Symptom Manage 22:966–977
Hegedus V (1979) Relief of pancreatic pain by radiography-guided block. Am J Roentgenol 133:1101–1103
Moore DC (1996) Neurolytic celiac plexus block: can paraplegia and death after neurolytic celiac plexus block be eliminated? Anesthesiology 84:1522–1523
Busch EH, Kay D, Branting SB (2003) Low volume neurolytic celiac plexus block with computed tomography guidance. Anesthesiology 9:1243–1244
Goroszeniuk T, di Vadi P (2000) Use of contrast before percutaneous neurolytic block. Reg Anesth Pain Med 25:437–438
Mercadante S, Nicosia F (1998) Celiac plexus block: a reappraisal. Reg Anesth Pain Med 23:37–48
Wong GY, Brown DL (1995) Transient paraplegia following alcohol celiac plexus block. Reg Anesth 20:352–355
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Zhang, CL., Zhang, TJ., Guo, YN. et al. Effect of Neurolytic Celiac Plexus Block Guided by Computerized Tomography on Pancreatic Cancer Pain. Dig Dis Sci 53, 856–860 (2008). https://doi.org/10.1007/s10620-007-9905-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10620-007-9905-2