Abstract
Background
Pharmacotherapy is considered an evidenced-based treatment for anxious youth. There is a need to better understand the relation between medication adherence and child outcomes.
Objective
This study prospectively examined: (1) baseline predictors of adherence and (2) the relation between medication adherence and clinical outcomes in children and adolescents with anxiety disorders.
Method
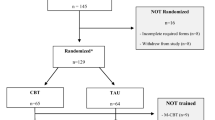
Participants were 349 youth randomized to sertraline, pill placebo, or sertraline plus cognitive behavioral therapy in the Child/Adolescent Anxiety Multimodal Study and followed over 12 weeks. The measure of pharmacotherapy adherence used was pharmacotherapist (PT) ratings of adherence at each session. Four domains of baseline predictors were examined (demographics, child clinical variables, family/parent variables, and treatment variables).
Results
Multiple regression analyses revealed few significant predictors of adherence. The most robust predictors of greater adherence were living with two parents and parents’ positive expectations that medication would lead to better outcomes. PTs ratings of higher adherence predicted higher global functioning at post treatment and treatment responder status.
Conclusions
In order to increase adherence, improving expectations and instilling hope for positive outcomes and problem solving ways to overcome pragmatic barriers associated with single parent families is recommended.
ClinicalTrials.gov Number
NCT00052078.
Similar content being viewed by others
References
Adler, L. D., & Nierenberg, A. A. (2010). Review of medication adherence in children and adults with ADHD. Postgraduate Medicine, 122(1), 184–191.
American Psychiatric Association. (2000). Diagnostic and statistical manual of mental disorders: DSM-IV-TR. Washington, DC: Author.
Bartlett, S. J., Krishnan, J. A., Riekert, K. A., Butz, A. M., Malveaux, F. J., & Rand, C. S. (2004). Maternal depressive symptoms and adherence to therapy in inner-city children with asthma. Pediatrics, 113(2), 229–237.
Brinkman, W. B., Sherman, S. N., Zmitrovich, A. R., Visscher, M. O., Crosby, L. E., Phelan, K. J., et al. (2012). In their own words: Adolescent views on ADHD and their evolving role managing medication. Academic Pediatrics, 12(1), 53–61.
Bussing, R., Koro-Ljungberg, M., Noguchi, K., Mason, D., Mayerson, G., & Garvan, C. W. (2012). Willingness to use ADHD treatments: A mixed methods study of perception by adolescents, parents, health professionals and teachers. Social Science and Medicine, 74(1), 92–100.
Charach, A., & Gajaria, A. (2008). Improving psychostimulant adherence in children with ADHD. Expert Review of Neurotherapeutics, 8, 1563–1571.
Charch, A., Yeung, E., Volpe, T., Goodale, T., & dosReis, S. (2014). Exploring stimulant treatment in ADHD: Narratives of young adolescents and their parents. BMC Psychiatry, 14, 110.
Comer, J. S., Olfson, M., & Mojtabai, R. (2010). National trends in child and adolescent psychotropic polypharmacy in office-based practice, 1996–2007. American Academy of Child & Adolescent Psychiatry, 49, 1001–1010.
Compton, S. N., Walkup, J. T., Albano, A. M., Piacentini, J. C., Birmaher, B., Sherrill, J. T., et al. (2010). Child/Adolescent Anxiety Multimodal Study (CAMS): Rationale, design, and methods. Child and Adolescent Psychiatry and Mental Health, 4, 1–15.
Derogatis, L. R. (1993). Brief Symptom Inventory: Administration, scoring, and procedures manual. Minneapolis, MN: National Computer Systems.
Graham, J. W., Olchowski, A. E., & Gilreath, T. D. (2007). How many imputations are really needed? Some practical clarifications of multiple imputation theory. Prevention Science, 8(3), 206–213.
Guy, W. (1976). The Clinical Global Impressions. In W. Guy (Ed.), ECDEU assessment manual for psychopharmacology—Revised (pp. 218–222). Rockville, MD: NIMH.
Hamrin, V., McCarthy, E. M., & Tyson, V. (2010). Pediatric psychotropic medication initiation and adherence: A literature review based on social exchange theory. Journal of Child and Adolescent Psychiatric Nursing, 23(3), 151–172.
Hollingshead, A. B. (1971). Commentary on the indiscriminate state of social class measurement. Social Forces, 49, 563–567.
Lee, P., Zehgeer, A., Ginsburg, G. S., McCracken, J., Keeton, C., Kendall, P. C., et al. (2017). Child and adolescent adherence with cognitive behavioral therapy for anxiety: Predictors and associations with outcomes. Journal of Clinical Child and Adolescent Psychology. https://doi.org/10.1080/15374416.2017.1310046.
Pappadopulos, E., Jensen, P. S., Chait, A. R., Arnold, L. E., Swanson, J. M., Greenhill, L. L., et al. (2009). Medication adherence in the MTA: Saliva methylphenidate samples versus parent report and mediating effect of concomitant behavioral treatment. Journal of the American Academy of Child and Adolescent Psychiatry, 48(5), 501–510.
Reinhard, S. C., Gubman, G. D., Horwitz, A. V., & Minsky, S. (1994). Burden Assessment Scale for families of the seriously mentally ill. Evaluation & Program Planning, 17, 261–269.
Research Units on Pediatric Psychopharmacology Anxiety Study Group. (2002). The Pediatric Anxiety Rating Scale (PARS): Development and psychometric properties. Journal of the American Academy of Child and Adolescent Psychiatry, 41, 1061–1069.
Sabate, E. (2001). Adherence to long-term therapies: Policy for action. Geneva: World Health Organization.
Shaffer, D., Gould, M., Brasic, J., Ambrosini, P., Fisher, P., Bird, H., et al. (1983). A Children’s Global Assessment Scale. Archives of General Psychiatry, 40, 1228–1231.
Silverman, W., & Albano, A. M. (1996). The anxiety disorders interview schedule for DSM-IV: Child and parent versions. San Antonio, TX: The Psychological Corporation.
Skinner, H., Steinhauer, P., & Santa-Barbara, J. (1995). Family Assessment Measure III (FAM-III). North Tonawanda, NY: Multi-Health Systems.
Walkup, J. T., Albano, A. M., Piacentini, J., Birmaher, B., Compton, S. N., Sherrill, J. T., et al. (2008). Cognitive behavioral therapy, sertraline, or a combination in childhood anxiety. New England Journal of Medicine, 359(26), 2753–2766.
Walkup, J. T., Labellarte, M. J., Riddle, M. A., Pine, D., Greenhill, L., Klein, R., et al. (2003). Searching for moderators and mediators of pharmacological treatment effects in children and adolescents with anxiety disorders. Journal of the American Academy of Child and Adolescent Psychiatry, 42, 13–21.
Woldu, H., Porta, G., Goldstein, T., Sakolsky, D., Perel, J., Emslie, G., et al. (2011). Pharmacokinetically and clinician-determined adherence to an antidepressant regimen and clinical outcome in the TORDIA trial. Journal of the American Academy of Child and Adolescent Psychiatry, 50, 490–498.
Yang, J., Yoon, B. M., Lee, M. S., Joe, S. H., Jung, I. K., & Kim, S. H. (2012). Adherence with electronic monitoring and symptoms in children with attention deficit hyperactivity disorder. Psychiatry Investigation, 9, 263–268.
Acknowledgements
This research was supported the National Institute of Mental Health Grants U01MH64089, U01MH64107, U01MH64003, U01MH63747, U01MH064092, and U01MH64088 awarded to the PIs of the Child/Adolescent Anxiety Multimodal Study.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
None of the authors have potential conflicts of interest to report.
Ethical Approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards. This article does not contain any studies with animals performed by any of the authors.
Informed Consent
Informed consent was obtained from all individual participants included in the study.
Rights and permissions
About this article
Cite this article
Zehgeer, A., Ginsburg, G.S., Lee, P. et al. Pharmacotherapy Adherence for Pediatric Anxiety Disorders: Predictors and Relation to Child Outcomes. Child Youth Care Forum 47, 633–644 (2018). https://doi.org/10.1007/s10566-018-9459-9
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10566-018-9459-9