Abstract
Purpose
Breast, cervical, and colorectal cancers are cancers that can be detected early through screening. Despite organized cancer screening programs in Ontario, Canada participation remains low among marginalized populations. Although extensive research has been done about factors contributing to under-screening by cancer site, the predictors of under/never screened conjointly for all three types of cancer remain unknown.
Methods
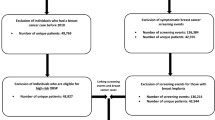
Using provincial-level linked administrative data sets, we examined Ontario women who were screen-eligible for all three types of cancer over a 36-month period (i.e., April 2014–March 2017) and determined how many were up to date on 0, 1, 2, and all three types of screenings. Multivariate logistic regression was utilized to examine individual and structural predictors of screening with the group overdue for all screening being the reference group.
Results
Of the 1,204,551 screen-eligible women, 15% were overdue for all. Living in the lowest income neighborhoods (AOR 0.46 [95% CI 0.45–0.47]), being recent immigrants (AOR 0.54 [95% CI 0.53–0.55]), having no primary care provider (AOR 0.17 [95% CI 0.16–0.17]), and having no contact with health care services (AOR 0.09 [95% CI 0.09–0.09]) significantly increased the likelihood of being overdue for all versus no screening type.
Conclusions
Considering that more than 15% of screen-eligible women in Ontario were overdue for all types of cancer screening, it is imperative to address structural barriers such as lack of a primary care provider. Innovative interventions like “one-stop shopping” where screening for different cancers can be offered at the same time could promote screening uptake.

Similar content being viewed by others
Data availability
All data generated or analyzed during this study are included in this published article [and its supplementary information files].
References
Canadian Cancer Statistics Advisory Committee (2018) Canadian Cancer Statistics 2018. Toronto, ON: Canadian Cancer Society. http://cancer.ca/Canadian-Cancer-Statistics-2018-EN. Accessed June 2019
Schoen RE, Pinsky PF, Weissfeld JL, Yokochi LA, Church T, Laiyemo AO et al (2012) Colorectal-cancer incidence and mortality with screening flexible sigmoidoscopy. N Engl J Med 366(25):2345–2357
Hewitson P, Glasziou P, Watson E, Towler B, Irwig L (2008) Cochrane systematic review of colorectal cancer screening using the fecal occult blood test (hemoccult): an update. Am J Gastroenterol 103(6):1541–1549
Tonelli M, Connor Gorber S, Joffres M, Dickinson J, Singh H, Lewin G et al (2011) Recommendations on screening for breast cancer in average-risk women aged 40–74 years. Can Med Assoc J 183(17):1991–2001
Cervical Screening – CCO (2012) Cancer Care Ontario. https://www.cancercare.on.ca/pcs/screening/cervscreening/. Accessed 10 Mar 2020
Cancer Care Ontario (2016) ColonCancerCheck (CCC) Screening recommendations summary—April 2016. CCC screening recommendations summary
Cancer Care Ontario (2012) Ontario cervical screening guidelines summary revised October 2016—based on current screening guidelines. Ontario cervical screening guidelines summary
Cancer Care Ontario. Ontario Breast Screening Program (OBSP) (2015) Guidelines Summary. https://www.cancercareontario.ca/sites/ccocancercare/files/assets/OBSPGuidelinesSummary.pdf. Accessed 10 Mar 2020
Borkhoff CM, Saskin R, Rabeneck L, Baxter NN, Liu Y, Tinmouth J, Paszat LF (2013) Disparities in receipt of screening tests for cancer, diabetes and high cholesterol in Ontario, Canada: a population-based study using area-based methods. Can J Public Health 104(4):e284–e290
Vahabi M, Lofters A, Kumar M, Glazier RH (2015a) Breast cancer screening disparities among urban immigrants: a population-based study in Ontario, Canada. BMC Public Health 15:679
Vahabi M, Lofters A, Kumar M, Glazier RH (2016) Breast cancer screening disparities among immigrant women by world region of origin: a population-based study in Ontario, Canada. Cancer Med 5:1670–1686
Ferdous M, Lee S, Goopy S, Yang H, Nahid Rumana N, Abedin T, Turin TC (2018) Barriers to cervical cancer screening faced by immigrant women in Canada: a systematic scoping review. BMC Women’s Health 18:165. https://doi.org/10.1186/s12905-018-0654-5
Vahabi M, Lofters A, Kumar M, Glazier R (2015b) Breast cancer screening disparities in Ontario, Canada. BMC Public Health 15:679–691. https://doi.org/10.1186/s12889-015-2050-5
Lofters A, Vahabi M, Kim E, Ellison L, Graves E, Glazier RH (2017) Cervical cancer screening among women from Muslim majority countries in Ontario, Canada. Cancer Epidemiol Biomark Prev 26(10):1493–1499. https://doi.org/10.1158/1055-9965.EPI-17-0323
Vahabi M, Lofters A, Wong J, Ellison L, Graves E, Damba C, Glazier RH (2019) Fecal occult blood test screening uptake among immigrants from Muslim majority countries: a retrospective cohort study in Ontario, Canada. Cancer Med. https://doi.org/10.1002/cam4.2541
Poole B, Black C, Gelmon K, Kan L (2010) Is Canadian women’s breast cancer screening behaviour associated with having a family doctor? Can Fam Physician 56(4):e150-157
Ogedegbe G, Cassells AN, Robinson CM, DuHamel K, Tobin JN, Sox CH et al (2005) Perception of barriers and facilitator of cancer early detection among low-income minority women in community health centers. J Natl Med Assoc 97(2):162–170
Thomas V, Saleem T, Abraham R (2005) Barriers to effective uptake of cancer screening among black and minority ethnic groups. Int J Palliat Nurs 11(11):562–571
Kiran T, Glazier RH, Moineddin R, Gu S, Wilton AS, Paszat L (2017) The impact of a population-based screening program on income- and immigration-related disparities in colorectal cancer screening. Cancer Epidemiol Biomark Prev 26(9):1401–1410. https://doi.org/10.1158/1055-9965.EPI-17-0301
Ontario's LHINs (2019) Local health integration network. http://www.lhins.on.ca. Accessed 26 Mar 2020
Kralj B (2015) Measuring "rurality" for purposes of health-care planning: an empirical measure for Ontario Toronto: Ontario Medical Association. http://www.oma.org/Shortage/Data/00rurality.asp. Accessed 26 Mar 2020
Marchildon GP, Hutchison B (2016) Primary care in Ontario, Canada: new proposals after 15 years of reform. Health Policy 120(7):732–738
Johns Hopkins ACG System (2017) The Johns Hopkins University. https://www.hopkinsacg.org. Accessed 26 Mar 2020
Wilkins R (2004) PPCF+ version 4E user’s guide. In: Health Analysis Measurement Group (ed) Automated geographic coding based on the statistics canada postal code conversion FIles, including postal codes to December 2003. Statistics Canada, Ottawa
Davis MM, Renfro S, Pham R, Hassmiller Lich K, Shannon J, Coronado GD, Wheeler SB (2017) Geographic and population-level disparities in colorectal cancer testing: a multilevel analysis of medicaid and commercial claims data. Prev Med 101:44–52. https://doi.org/10.1016/j.ypmed.2017.05.001
Honein-AbouHaidar GN, Kastner M, Vuong V, Perrier L, Daly C, Rabeneck L et al (2016) Systematic review and meta-study synthesis of qualitative studies evaluating facilitators and barriers to participation in colorectal cancer screening. Cancer Epidemiol Biomark Prev 25(6):907–917
Khan AM, Urquia M, Kornas K et al (2017) Socioeconomic gradients in all-cause, premature and avoidable mortality among immigrants and long-term residents using linked death records in Ontario. Canada J Epidemiol Community Health 71:625–632
Vahabi M, Lofters A, Kim E, Wong JP, Ellison L, Graves E et al (2017) Breast cancer screening utilization among women from Muslim majority countries in Ontario. Canada Prev Med 105:176–183
Health Care Connect Program. Ontario Ministry of Health and Long Term Care. https://www.ontario.ca/page/find-family-doctor-or-nurse-practitioner?_ga=2.203698130.31479681.1562023907-1347006204.1552083749. Accessed 5 Apr 2020
Leyva B, Allen JD, Ospino H, Tom LS, Negrón R, Buesa R, Torres MI (2017) Enhancing capacity among faith-based organizations to implement evidence-based cancer control programs: a community-engaged approach. Transl Behav Med 7(3):517–528
Lobb R, Pinto AD, Lofters A (2013) Using concept mapping in the knowledge-to action process to compare stakeholder opinions on barriers to use of cancer screening among south Asians. Implement Sci 8:37
Lofters AK, Moineddin R, Hwang SW, Glazier RH (2011) Predictors of low cervical cancer screening among immigrant women in Ontario. Canada BMC Womens Health 11:20
Bobridge A, Price K, Gill TK, Taylor AW (2017) Influencing cancer screening participation rates—providing a combined cancer screening program (a ‘one stop’ shop) could be a potential answer. Front Oncol 7:308. https://doi.org/10.3389/fonc.2017.00308
Dhanji Z, Randall A (2016) Cervical screening reminder calls pilot: utilizing EMRs to improve cancer screening. J Clin Oncol 34(7_suppl):163–163
Feldman J, Davie S, Kiran T (2017) Measuring and improving cervical, breast, and colorectal cancer screening rates in a multi-site urban practice in Toronto, Canada. BMJ Qual Improv Rep 6(u213991):w5531. https://doi.org/10.1136/bmjquality.u213991.w5531
Acknowledgments
This study was supported by funding from the Toronto Central Local Health Integration Network. Additional support was provided through the Ontario Ministry of Health and Long-Term Care, St. Michael’s Hospital, and the MAP Centre for Urban Health Solutions at St. Michael's Hospital. This study was also supported by ICES, which is funded by an annual grant from the Ontario Ministry of Health and Long-Term Care (MOHLTC). The opinions, results, and conclusions reported in this paper are those of the authors and are independent from the funding sources. No endorsement by ICES or the Ontario MOHLTC is intended or should be inferred. Parts of this material are based on data and information compiled and provided by the Canadian Institute for Health Information (CIHI). However, the analyses, conclusions, opinions, and statements expressed herein are those of the authors, and not necessarily those of CIHI. Parts of this material are based on data and information provided by Cancer Care Ontario (CCO). The opinions, results, view, and conclusions reported in this paper are those of the authors and do not necessarily reflect those of CCO. No endorsement by CCO is intended or should be inferred. Dr. Aisha Lofters is supported by a New Investigator Award from CIHR. Dr. Aisha Lofters and Dr. Richard Glazier are supported as Clinician Scientists in the Department of Family and Community Medicine at the University of Toronto, and Dr. Glazier is supported as a Clinician Scientist in the Department of Family and Community Medicine at St. Michael's Hospital. Dr. Aisha Lofters is supported by a Chair in Implementation Science at the Peter Gilgan Centre for Women’s Cancers at Women’s College Hospital in Partnership with the Canadian Cancer Society.
Funding
Ontario Ministry of Health and Long-Term Care (MOHLTC).
Author information
Authors and Affiliations
Contributions
AK extracted the data based on specification provided by MV, AL, and RG. MV processed and analyzed the data and drafted the article. AL and RG reviewed the article critically for intellectual content. All the authors gave final approval of the version to be published and agreed to serve as guarantors of the work.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no competing interests.
Ethical approval
The Research Ethics Board of St. Michael’s Hospital in Ontario provided ethics approval for the study.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Vahabi, M., Lofters, A.K., Kopp, A. et al. Correlates of non-adherence to breast, cervical, and colorectal cancer screening among screen-eligible women: a population-based cohort study in Ontario, Canada. Cancer Causes Control 32, 147–155 (2021). https://doi.org/10.1007/s10552-020-01369-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10552-020-01369-y