Abstract
Purpose
Identifying correlates of colorectal cancer screening (CRCS) is critical for cancer control and prevention. Classification tree analysis (CTA) is a potentially powerful analytic tool that can identify distinct population subgroups for which CRCS is influenced by any number of multivariable interactions. This study used CTA to identify correlates of CRCS for exclusive population subgroups.
Methods
Data were obtained from the 2007 Health Information National Trends Survey (HINTS) and analyzed in 2014. CTA was employed to determine the association between demographic (n = 11), psychosocial (n = 6), and numeracy (n = 3) variables and CRCS status of adults ≥50 years (n = 3,769).
Results
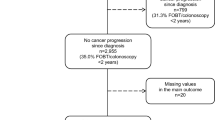
Overall CRCS rate was 66.9 %. Level of doctor avoidance (three categories) was the initial splitting variable, leading to a total of 21 terminal node subgroups of CRCS utilization: (1) avoid doctor, not for fear of illness/death [n = 625 (16.5 %), four subgroups]; (2) avoid doctor, fear illness/death [n = 366 (9.7 %), two subgroups]; (3) do not avoid doctor [n = 2,778 (73.7 %), 15 subgroups].
Conclusions
Doctor avoidance was an important behavioral influence on CRCS adherence. Use of CTA to identify unique characteristics within population subgroups has merit for tailoring future intervention strategies. Community-based approaches may be effective for reaching individuals who avoid routine doctor visits.

Similar content being viewed by others
References
National Cancer Institute (2010) A snapshot of colorectal cancer. Incidence and mortality. http://www.cancer.gov/researchandfunding/snapshots/colorectal. Accessed 15 June 2014
American Cancer Society (2014) Cancer facts and figures, 2014. http://www.cancer.org/research/cancerfactsstatistics/cancerfactsfigures2014/. Accessed 15 June 2014
Walsh JME, Terdiman JP (2003) Colorectal cancer screening: scientific review. JAMA 289(10):1288–1296
Smith RA, Cokkinides V, Eyre HJ (2007) Cancer screening in the United States, 2007: a review of current guidelines, practices, and prospects. CA Cancer J Clin 57:90–104
National Cancer Institute (2014) Cancer trends progress report: 2011–2012 update. http://progressreport.cancer.gov/doc_detail.asp?pid=1&did=2011&chid=102&coid=1018&mid. Accessed 20 June 2014
Rakowski W, Clark MA (1998) Do groups of women aged 50 to 75 match the national average mammography rate? Am J Prev Med 15(3):187–197
Vernon SW (1997) Participation in colorectal cancer screening: a review. J Natl Cancer Inst 89(19):1406–1422
Beydoun HA, Beydoun MA (2008) Predictors of colorectal cancer screening behaviors among average-risk older adults in the United States. Cancer Cause Control 19(4):339–359
Consedine NS, Magai C, Krivoshekova YS, Ryzewicz L, Neugut AI (2004) Fear, anxiety, worry, and breast cancer screening behavior: a critical review. Cancer Epidemiol Biomarkers Prev 13(4):501–510
Davids S, Schapira M, McAuliffe T, Nattinger A (2004) Predictors of pessimistic breast cancer risk perceptions in a primary care population. J Gen Intern Med 19(4):310–315
Kiviniemi M, Bennett A, Zaiter M, Marshall J (2011) Individual-level factors in colorectal cancer screening: a review of the literature on the relation of individual level health behavior constructs and screening behavior. Psycho Oncology 20:1023–1033
Gimeno Garcia A, Hernandez Alvarez Buylla N, Nicolas-Perez D, Quintero E (2014) Public awareness of colorectal cancer screening: knowledge, attitudes, and interventions for increasing screening uptake. Oncology. doi:10.1155/2014/425787
Davis TC, Williams MV, Marin E, Parker RM, Glass J (2002) Health literacy and cancer communication. CA Cancer J Clin 52(3):134–149
Schwartzberg JG, VanGeest J, Wang CC (eds) (2005) Understanding health literacy: implications for medicine and public health. American Medical Association Press, Chicago, IL
United States Department of Health and Human Services (2014) Health literacy. http://www.health.gov/communication/literacy/. Accessed 21 May 2014
Miller DP Jr, Brownlee CD, McCoy TP, Pignone MP (2007) The effect of health literacy on knowledge and receipt of colorectal cancer screening: a survey study. BMC Fam Pract. doi:10.1186/1471-2296-8-16
United States Department of Health and Human Services (2010) Quick guide to health literacy. (2010). http://www.health.gov/communication/literacy/quickguide/. Accessed 24 May 2014
Ciampa PJ, White RO, Perrin EM et al (2013) The association of acculturation and health literacy, numeracy and health-related skills in Spanish-speaking caregivers of young children. J Immigr Minor Health 15(3):492–498
Keller C, Siegrist M (2009) Effect of risk communication formats on risk perception depending on numeracy. Med Decis Mak 29(4):483–490
Golbeck AL, Ahlers-Schmidt CR, Paschal AM, Dismuke SE (2005) A definition and operational framework for health numeracy. Am J Prev Med 29(4):375–376
Lipkus IM, Samsa G, Rimer BK (2001) General performance on a numeracy scale among highly educated samples. Med Decis Mak 21(1):37–44
Reyna VF, Brainerd CJ (2007) The importance of mathematics in health and human judgement: numeracy, risk communication, and medical decision making. Learn Individ Differ 17:147–159
Rothman RL, Montori VM, Cherrington A, Pignone MP (2008) Perspective: the role of numeracy in health care. J Health Commun 13:583–595
Schapira MM, Neuner J, Fletcher KE, Gilligan MA, Hayes E, Laud P (2011) The relationship of health numeracy to cancer screening. J Cancer Educ 26(1):103–110
Schwartz LM, Woloshin S, Black WC, Welch HG (1997) The role of numeracy in understanding the benefit of screening mammography. Ann Intern Med 127(11):966–972
Kutner M, Greenberg BD, Jin Y, Paulsen C (2006) The Health literacy of America’s adults: results from the 2003 National Assessment of Adult Literacy. National Center for Education Statistics, United States Department of Education, Washington
Rothman RL, Housam R, Weiss H et al (2006) Patient understanding of food labels: the role of literacy and numeracy. Am J Prev Med 31(5):391–398
Ciampa PJ, Osborn CY, Peterson NB, Rothman RL (2010) Patient numeracy, perceptions of provider communication, and colorectal cancer screening utilization. J Health Commun 15(Suppl 3):157–168
Breiman L (2001) Statistical modeling: the two cultures. Stat Sci 16(3):199–231
Camp NJ, Slattery ML (2002) Classification tree analysis: a statistical tool to investigate risk factor interactions with an example for colon cancer. Cancer Causes Control 13(9):813–823
Zhang H, Bonney G (2000) Use of classification trees for association studies. Genet Epidemiol 19:323–332
Kitsantas P, Moore TW, Sly DF (2007) Using classification trees to profile adolescent smoking behaviors. Addict Behav 32(1):9–23
McKenzie DM, McFarlane AC, Creamer M, Ikin JF, Forbes AB, Kelsall HL et al (2006) Hazardous or harmful alcohol use in Royal Australian Navy veterans of the 1991 Gulf War: identification of high risk subgroups. Addict Behav 31(9):1683–1694
Welte JW, Barnes GM, Wieczorek WF, Tidwell MC (2004) Gambling participation and pathology in the United States—a sociodemographic analysis using classification trees. Addict Behav 29(5):983–989
Calvocoressi L, Stolar M, Kasl SV, Claus EB, Jones BA (2005) Applying recursive partitioning to a prospective study of factors associated with adherence to mammography screening guidelines. Am J Epidemiol 162(12):1215–1224
Gjelsvik A, Rogers ML, Clark MA, Ombao HC, Rakowski W (2014) Continuum of mammography use among US women: classification tree analysis. Am J Health Behav 38(4):492–500
Ishikawa Y, Zheng YF, Nishiuchi H, Suda T, Hasumi T, Saito H (2013) Classification tree analysis to enhance targeting for follow-up exam of colorectal cancer screening. BMC Cancer 13:470. doi:10.1186/1471-2407-13-470
Nelson DE, Kreps GL, Hesse BW, Croyle RT, Willis G, Arora NK et al (2004) The Health Information National Trends Survey (HINTS): development, design, and dissemination. J Health Commun 9(5):443–460 discussion 481–444
Subramanian S, Klosterman M, Amonkar MM, Hunt TL (2004) Adherence with colorectal cancer screening guidelines: a review. Prev Med 38(5):536–550
Janz NK, Champion VL, Strecher VJ (2002) The health belief model. In: Glanz KM, Rimer BK, Lewis FM (eds) Health behavior and health education: theory, research, and practice, 3rd edn. Wiley, San Fransisco, pp 45–66
Messina CR, Lane DS, Grimson R (2005) Colorectal cancer screening attitudes and practices preferences for decision making. Am J Prev Med 28(5):439–446
SPSS. AnswerTree(r) (2002) 3.1 user’s guide. SPSS, Inc, Chicago
Biggs D, De Ville B, Suen E (1991) A method of choosing multiway partitions for classification and decision trees. J Appl Stat 18(1):49–62
Lemon SC, Roy J, Clark MA, Friedmann PD, Rakowski W (2003) Classification and regression tree analysis in public health: methodological review and comparison with logistic regression. Ann Behav Med 26(3):172–181
Coups EJ, Manne SL, Meropol NJ, Weinberg DS (2007) Multiple behavioral risk factors for colorectal cancer and colorectal cancer screening status. Cancer Epidemiol Biomarkers Prev 16(3):510–516
Pruitt SL, McQueen A, Tiro JA, Rakowski W, Diclemente CC, Vernon SW (2010) Construct validity of a mammography processes of change scale and invariance by stage of change. J Health Psychol 15(1):64–74
Tiro JA, Diamond PM, Perz CA, Fernandez M, Rakowski W, DiClemente CC et al (2005) Validation of scales measuring attitudes and norms related to mammography screening in women veterans. Health Psychol 24(6):555–566
Spleen A, Lengerich E, Camacho F, Vanderpool R (2014) Health care avoidance among rural populations: results from a nationally representative survey. Rural Health 30:79–88
American Cancer Society (2014) Colorectal cancer facts and figures: 2014–2016. http://www.cancer.org/acs/groups/content/documents/document/acspc-042280.pdf. Accessed 30 Dec 2014
Peroskie A, Ferrer RA, Klein WMP (2013) Association of cancer worry and perceived risk with doctor avoidance: an analysis of information avoidance in a nationally representative US sample. J Behav Med. doi:10.1007/s10865-013-9537-2
Kannan VD, Veazie PJ (2014) Predictors of avoiding medical care and reasons for avoidance behavior. Med Care 52(4):336–345
Byrne SK (2008) Healthcare avoidance: a critical review. Holist Nurs Pract 22(5):280–292
Mcqueen A, Vernon SW, Meissner HI, Rakowski W (2008) Risk perceptions and worry about cancer: does gender make a difference? J Health Commun 13(1):56–79
Moser RP, Arndt J, Han PK, Waters EA, Amsellem M, Hesse BW (2014) Perceptions of cancer as a death sentence: prevalence and consequences. J Health Psychol 19(12):1518–1524
Reynolds LM, Consedine NS, Pizarro DA, Bissett IP (2013) Disgust and behavioral avoidance in colorectal cancer screening and treatment: a systematic review and research agenda. Cancer Nurs 36(2):122–130
Acknowledgments
This research was internally supported by the University of Delaware.
Conflict of interest
The authors declare no conflict of interests.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Dominick, G.M., Papas, M.A., Rogers, M.L. et al. Classification tree analysis to examine influences on colorectal cancer screening. Cancer Causes Control 26, 443–454 (2015). https://doi.org/10.1007/s10552-015-0523-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10552-015-0523-6