Abstract
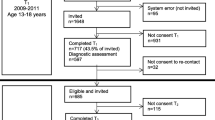
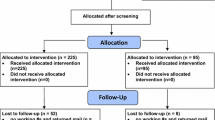
This study examined research attrition in clinical service settings by comparing psychotherapy research completers and dropouts in a private therapy practice. Seventy-seven children 7–12 years old enrolled in the Resilience Builder Program® (RBP), a manualized group therapy created and administered in a private practice. Children had social impairments, and most were diagnosed with Attention Deficit Hyperactivity Disorder (ADHD) and/or anxiety disorders. Results found that compared to completers, research dropouts had significantly greater social deficits, disruptive behavior problems, affective problems, medication use, and were more likely to be ethnic minorities. We discuss implications for research recruitment and retention in clinical service settings.



Similar content being viewed by others
References
Alvord, M. K., & Rich, B. A. (2012). Resilience Builder groups for youth: practice and research in a private clinical setting. Independent Practitioner, 32, 18–20.
Alvord, M. K., Zucker, B., & Grados, J. J. (2011). Resilience Builder Program for children and adolescents: Enhancing social competence and self-regulation—A cognitive-behavioral group approach. Champaign: Research Press.
Barrett, P. M., Farrell, L., Pina, A. A., Peris, T. S., & Piacentini, J. (2008). Evidence-based psychosocial treatments for child and adolescent obsessive-compulsive disorder. Journal of Clinical Child & Adolescent Psychology, 37, 131–155.
Barrington, J., Prior, M., Richardson, M., & Allen, K. (2005). Effectiveness of CBT versus standard treatment for childhood anxiety disorders in a community clinic setting. Behaviour Change, 22, 29–43.
Bierman, K. L., & Welsh, J. A. (2000). Assessing social dysfunction: the contributions of laboratory and performance-based measures. Journal of Clinical Child Psychology, 29, 526–539.
Clarke, G. N., Hornbrook, M., Lynch, F., Polen, M., Gale, J., O’Connor, E., et al. (2002). Group cognitive-behavioral treatment for depressed adolescent offspring of depressed parents in a health maintenance organization. Journal of the American Academy of Child and Adolescent Psychiatry, 41, 305–313.
Clarke, G., Debar, L., Lynch, F., Powell, J., Gale, J., O’Connor, E., et al. (2005). A randomized effectiveness trial of brief cognitive-behavioral therapy for depressed adolescents receiving antidepressant medication. Journal of the American Academy of Child and Adolescent Psychiatry, 44, 888–898.
Coplan, R. J., & Armer, M. (2007). A “multitude” of solitude: A closer look at social withdrawal and non-social play in early childhood. Child Development Perspectives, 1, 26–32.
Counts, C. A., Nigg, J. T., Stawicki, J. A., Rappley, M. D., & von, E. A. (2005). Family adversity in DSM-IV ADHD combined and inattentive subtypes and associated disruptive behavior problems. Journal of the American Academy of Child and Adolescent Psychiatry, 44, 690–698.
Cribbie, R. A., & Keselman, H. J. (2003). Pairwise multiple comparisons: A model comparison approach versus stepwise procedures. British Journal of Mathematical and Statistical Psychology, 56, 167–182.
De Los Reyes, A., & Kazdin, A. E. (2005). Informant discrepancies in the assessment of childhood psychopathology: A critical review, theoretical framework, and recommendations for further study. Psychological Bulletin, 131, 483–509.
Derogatis, L. R., & Melisaratos, N. (1983). The Brief Symptom Inventory: An introductory report. Psychological Medicine, 13, 595–605.
Dishion, T. J., Bullock, B. M., & Granic, I. (2002). Pragmatism in modeling peer influence: Dynamics, outcomes, and change processes. Development and Psychopathology, 14, 969–981.
Dwight-Johnson, M., Sherbourne, C. D., Liao, D., & Wells, K. B. (2000). Treatment preferences among depressed primary care patients. Journal of General Internal Medicine, 15, 527–534.
Farrell, L. J., Schlup, B., & Boschen, M. J. (2010). Cognitive-behavioral treatment of childhood obsessive-compulsive disorder in community-based clinical practice: Clinical significance and benchmarking against efficacy. Behaviour Research and Therapy, 48, 409–417.
Flick, S. N. (1988). Managing attrition in clinical research. Clinical Psychology Review, 8, 499–515.
Foley, M. (2011). A comparison of family adversity and family dysfunction in families of children with attention deficit hyperactivity disorder (ADHD) and families of children without ADHD. Journal for Specialists in Pediatric Nursing, 16, 39–49.
Gonzalez, A., Weersing, V. R., Warnick, E. M., Scahill, L. D., & Woolston, J. L. (2011). Predictors of treatment attrition among an outpatient clinic sample of youths with clinically significant anxiety. Administration and Policy In Mental Health, 38, 356–367.
Hunt, C., & Andrews, G. (1992). Drop-out rate as a performance indicator in psychotherapy. Acta Psychiatrica Scandinavica, 85, 275–278.
Kazdin, A. E. (2008). Evidence-based treatment and practice: New opportunities to bridge clinical research and practice, enhance the knowledge base, and improve patient care. American Psychologist, 63, 146–159.
Kupersmidt, J. B., & Coie, J. D. (1990). Preadolescent peer status, aggression, and school adjustment as predictors of externalizing problems in adolescence. Child Development, 61, 1350–1362.
La Greca, A. M., Silverman, W. K., & Lochman, J. E. (2009). Moving beyond efficacy and effectiveness in child and adolescent intervention research. Journal of Consulting and Clinical Psychology, 77, 373–382.
Marchand, E., Stice, E., Rohde, P., & Becker, C. B. (2011). Moving from efficacy to effectiveness trials in prevention research. Behaviour Research and Therapy, 49, 32–41.
Merikangas, K. R., He, J. P., Burstein, M., Swanson, S. A., Avenevoli, S., Cui, L., et al. (2010). Lifetime prevalence of mental disorders in U.S. adolescents: Results from the National Comorbidity Survey Replication–Adolescent Supplement (NCS-A). Journal of the American Academy of Child and Adolescent Psychiatry, 49, 980–989.
Miller, L. M., Southam-Gerow, M. A., & Allin, R. B. (2008). Who stays in treatment? Child and family predictors of youth client retention in a public mental health agency. Child & Youth Care Forum, 37, 153–170.
National Advisory Mental Health Council’s Workgroup on Child and Adolescent Mental Health Intervention Development and Deployment. (2001). (Rep. No. NIH 01-4985). Rockville: NIMH.
Norcross, J. C., Beutler, L. E., & Levant, R. F. (2006). Evidence-based practices in mental health: Debate and dialogue on the fundamental questions. Washington, DC: American Psychological Association.
Owens, J. S., Goldfine, M. E., Evangelista, N. M., Hoza, B., & Kaiser, N. M. (2007). A critical review of self-perceptions and the positive illusory bias in children with ADHD. Clinical Child and Family Psychology Review, 10, 335–351.
Patterson, G. R., Crosby, L., & Vuchinich, S. (1992). Predicting risk for early police arrest. Journal of Quantitative Criminology, 8, 335–355.
Pelham, W. E., Jr, & Fabiano, G. A. (2008). Evidence-based psychosocial treatments for attention-deficit/hyperactivity disorder. Journal of Clinical Child & Adolescent Psychology, 37, 184–214.
Pellerin, K. A., Costa, N. M., Weems, C. F., & Dalton, R. F. (2010). An examination of treatment completers and non-completers at a child and adolescent community mental health clinic. Community Mental Health Journal, 46, 273–281.
Pina, A. A., & Silverman, W. K. (2004). Somatic symptoms, and distress in hispanic/latino and European American youths with anxiety disorders. Clinical Phenomenology, 33, 227–236.
Pina, A. A., Silverman, W. K., Weems, C. F., Kurtines, W. M., & Goldman, M. L. (2003). A comparison of completers and non-completers of exposure-based cognitive and behavioral treatment for phobic and anxiety disorders in youth. Journal of Consulting and Clinical Psychology, 71, 701–705.
President’s New Freedom Commission on Mental Health. (2003). Achieving the promise: Transforming mental health care in American: Final report (Rep. No. SMA-03-3832). Rockville: DHHS.
Prior, M., Smart, D., Sanson, A., & Oberklaid, F. (2000). Does shy-inhibited temperament in childhood lead to anxiety problems in adolescence? Journal of the American Academy of Child and Adolescent Psychiatry, 39, 461–468.
Reynolds, C. R., & Kamphaus, R. W. (2004). Behavior assessment system for children. Atlascocita: American Guidance Service.
Rubin, K. H., Coplan, R. J., Chen, X., Buskirk, A., & Wojslawowicz, A. (2005). Peer relationships in childhood. In M. H. Bornstein & M. E. Lamb (Eds.), Developmental science: An advanced textbook (5th ed.). Mahwah: Lawrence Erlbaum.
Sim, L., Whiteside, S. P., Dittner, C. A., & Mellon, M. (2006). Effectiveness of a social skills training program with school age children: Transition to a clinical setting. Journal of Child and Family Studies, 15, 409–418.
Sledge, W. H., Moras, K., Hartley, D., & Levine, M. (1990). Effect of time-limited psychotherapy on patient dropout rates. American Journal of Psychiatry, 147, 1341–1347.
Smith-Boydson, J. M., & Nelson, T. D. (2008). Adoption of evidence-based treatments in community settings: Obstacles and opportunities. In R. G. Steele, T. D. Elkin, & M. C. Roberts (Eds.), Handbook of evidence-based therapies for Children and Adolescents: Bridging science and practice. New York: Springer.
Southam-Gerow, M. A., Weisz, J. R., & Kendall, P. C. (2003). Youth with anxiety disorders in research and service clinics: Examining client differences and similarities. Journal of Clinical Child & Adolescent Psychology, 32, 375–385.
Southam-Gerow, M. A., Silverman, W. K., & Kendall, P. C. (2006). Client similarities and differences in two childhood anxiety disorders research clinics. J. Clin. Child Adolesc. Psychol., 35, 528–538.
Spoth, R., Goldberg, C., & Redmond, C. (1999). Engaging families in longitudinal preventive intervention research: Discrete-time survival analysis of socioeconomic and social-emotional risk factors. Journal of Consulting and Clinical Psychology, 67, 157–163.
Stevens, J., Kelleher, K. J., Ward-Estes, J., & Hayes, J. (2006). Perceived barriers to treatment and psychotherapy attendance in child community mental health centers. Community Mental Health Journal, 42, 449–458.
Substance Abuse and Mental Health Services Administration. (2012). Mental Health United States 2010. Rockville: Substance Abuse and Mental Health Services Administration.
Weersing, V. R., & Weisz, J. R. (2002). Community clinic treatment of depressed youth: Benchmarking usual care against CBT clinical trials. Journal of Consulting and Clinical Psychology, 70, 299–310.
Weersing, R., Gonzales, A., Campo, J., & Lucas, A. (2008). Brief behavioral therapy for pediatric anxiety and depression: Piloting an integrated treatment approach. Cognitive and Behavioral Practice, 15, 126–139.
Weisz, J. R., Donenberg, G. R., Han, S. S., & Weiss, B. (1995). Bridging the gap between laboratory and clinic in child and adolescent psychotherapy. Journal of Consulting and Clinical Psychology, 63, 688–701.
Weisz, J. R., Jensen Doss, A., & Hawley, K. M. (2005). Youth psychotherapy outcome research: A review and critique of the evidence base. Annual Review of Psychology, 56, 337–363.
Weisz, J. R., Southam-Gerow, M. A., Gordis, E. B., Connor-Smith, J. K., Chu, B. C., Langer, D. A., et al. (2009). Cognitive-behavioral therapy versus usual clinical care for youth depression: An initial test of transportability to community clinics and clinicians. Journal of Consulting and Clinical Psychology, 77, 383–396.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Rich, B.A., Hensler, M., Rosen, H.R. et al. Attrition from Therapy Effectiveness Research Among Youth in a Clinical Service Setting. Adm Policy Ment Health 41, 343–352 (2014). https://doi.org/10.1007/s10488-013-0469-5
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10488-013-0469-5