Abstract
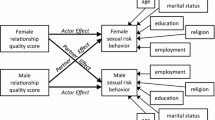
Few studies examine how relationship factors influence sexual risk. We investigated gender differences of the influence of relationship functioning on sexual risk behavior and sexually transmitted infections (STIs) among 296 young pregnant couples. Compared to women, men were twice as likely to have a concurrent partner, were less likely to intend to be monogamous in the future, had less HIV/STI knowledge and more perceived risk for HIV/STI, negative attitudes and efficacy toward condom use (all P < 0.05). For men, poor relationship functioning related to less intentions to be monogamous, more partner concurrency, worse sexual communication, and more condom use. For women, poor relationship functioning related to worse sexual communication and less condom use. In addition, women who had good relationship functioning and women who had partners with poor relationship functioning were more likely to have an STI. These results demonstrate the need to include heterosexual men and relationship factors in HIV prevention.
Similar content being viewed by others
References
Furman W. The emerging field of adolescent romantic relationships. Curr Dir Psychol Sci. 2002;11(5):177–81.
Furman W, Shaffer L. The role of romantic relationships in adolescent development. In: Florsheim P, editor. Adolescent romantic relations and sexual behavior. Mahwah: Lawrence Erlbaum Associates; 2003. p. 3–22.
Misovich SJ, et al. Close relationships and elevated HIV risk behavior: Evidence and possible underlying psychological processes. Rev Gen Psychol. 1997;1(1):72–107.
Malow RM, et al. HIV preventive interventions for adolescents: A look back and ahead. Curr HIV/AIDS Rep. 2007;4(4):173–80.
El-Bassel N, et al. HIV prevention for intimate couples: a relationship-based model. Fam Syst Health. 2001;19(4):379–95.
Kershaw T, et al. Let’s stay together: relationship dissolution among parenting and non-parenting adolescents. J Behav Med. 2010;33(6):454–65.
Kershaw TS, et al. Avoidance, anxiety, and sex: the influence of romantic attachment on HIV-risk among pregnant women. AIDS Behav. 2007;11(2):299–311.
Aalsma MC, et al. Adolescent romantic partnerships and health-risk behaviors: a comparison of dyad members. J Adolesc Health. 2004;34(2):151–2.
Choi KH, et al. Extramarital sex and HIV risk behavior among US adults: results from the national AIDS behavioral survey. Am J Public Health. 1994;84(12):2003–7.
Gee CB, Rhodes JE. Postpartum transitions in adolescent mothers’ romantic and maternal relationships. Merrill-Palmer Q. 1999;45(3):512–32.
Ott MA, et al. Longitudinal associations among relationship factors, partner change, and sexually transmitted infection acquisition in adolescent women. Sex Transm Dis. 2011;38(3):153–7.
Niccolai LM, et al. New sex partner acquisition and sexually transmitted disease risk among adolescent females. J Adolesc Health. 2004;34(3):216–23.
Foxman B, et al. Measures of sexual partnerships: lengths, gaps, overlaps, and sexually transmitted infection. Sex Transm Dis. 2006;33(4):209–14.
Kalichman SC, Grebler T. Reducing numbers of sex partners: do we really need special interventions for sexual concurrency? AIDS Behav. 2010;14(5):987–90.
Kretzschmar M, Dietz K. The effect of pair formation and variable infectivity on the spread of an infection without recovery. Math Biosci. 1998;148(1):83–113.
Wilson SR, et al. Correlates of sexual risk for HIV infection in female members of heterosexual California Latino couples: An application of a Bernoulli process model. AIDS Behav. 2003;7(i):273–90.
Seal DW, Ehrhardt AA. HIV-prevention-related sexual health promotion for heterosexual men in the United States: pitfalls and recommendations. Arch Sex Behav. 2004;33(3):211–22.
Strathdee SA, et al. Sex differences in risk factors for HIV seroconversion among injection drug users: a 10-year perspective. Arch Intern Med. 2001;161(10):1281–8.
CDC. HIV/AIDS surveillance report 2002. Rockville, Maryland: Centers for Disease Control and Prevention, 2002.
Kaiser Family Foundation. What teens know and don’t (but should) about sexually transmitted diseases. Menlo Park: Kaiser Family Foundation, 1998.
Grunbaum J, et al. Youth risk behavior surveillance—United States 2003. Morb Mortal Wkly Rep. 2004;53(SS02):1–96.
Fortenberry JD. Health behaviors and reproductive health risk within adolescent sexual dyads. In: Florsheim P, editor. Adolescent romantic relations and sexual behavior. Mahwah: Lawurence Erlbaum Publishers; 2003. p. 279–96.
Christakis NA, Fowler JH. The spread of obesity in large social networks over 32 years. N Engl J Med. 2007;357(4):370–9.
Christakis NA, Fowler JH. The collective dynamics of smoking in a large social network. N Engl J Med. 2008;358(21):2249–58.
Dulude D, et al. High-risk pregnancies, psychological distress, and dyadic adjustment. J Reprod Infant Psychol. 2002;20(2):101–24.
Cox MJ, et al. The transition to parenthood: marital conflict and withdrawal and parent-infant interactions. In: Cox MJ, Brooks-Gunn J, editors. Conflict and cohesion in families. Mahwah: Laurence Erlbaum Associates; 1999. p. 87–104.
Ketterlinus RD, et al. Development and ecological sources of stress among adolescent parents. Fam Relat Interdiscip J Appl Fam Stud. 1991;40(4):435–41.
Bost KK, et al. Structural and supportive changes in couples’ family and friendship networks across the transition to parenthood. J Marriage Fam. 2002;64(2):517–31.
Florsheim P, et al. The transition to parenthood among young African American and Latino couples: relational predictors of risk for parental dysfunction. J Fam Psychol. 2003;17(1):65–79.
Ventura SJ, Mathews TJ, Hamilton BE, Sutton PD, Abma JC. Adolescent pregnancy and childbirth: United States, 1991–2008. In: CDC, editor. Morbidity and mortality weekly report. Atlanta: CDC; 2011.
Centers for Disease Control and Prevention. HIV/AIDS surveillance in adolescents and young adults (through 2007), 2009.
Centers for Disease Control and Prevention. Fact Sheet: HIV in the United States. Atlanta: US Department of Health and Human Services, CDC; 2010.
Centers for Disease Control and Prevention. Trends in reportable sexually transmitted diseases in the United States, national surveillance data for Chlamydia, Gonorrhea, and Syphilis. Atlanta: CDC; 2009.
Chesson HW, et al. The estimated direct medical cost of sexually transmitted diseases among American youth. Perspect Sex Reprod Health. 2004;36(1):11–9.
Hein K, et al. Comparison of HIV+ and HIV− adolescents: risk factors and psychosocial determinants. Pediatrics. 1995;95(1):96–104.
Laga M et al. Non ulcerative sexually transmitted diseases (STD) as risk factors for HIV infection. In: Sixth international AIDS conference, San Francisco; 1990.
Plummer F. Co-factors in male-female sexual transmission of HIV type I. J Infect Dis. 1991;163(2):233–9.
Wasserheit J. Epidemiological synergy: Interrelationships between human immunodeficiency virus infection and other sexually transmitted diseases. Sex Transm Dis. 1992;19(2):95–102.
Ickovics, et al. High postpartum rates of sexually transmitted infections among teens: Pregnancy as a window of opportunity for prevention. Sex Transm Infect. 2003;79:469–73.
Meade CS, Ickovics JR. Systematic review of sexual risk among pregnant and mothering teens in the USA: pregnancy as an opportunity for integrated prevention of STD and repeat pregnancy. Soc Sci Med. 2005;60(4):661–78.
Donenberg GR, Pao M. Youths and HIV/AIDS: psychiatry’s role in a changing epidemic. J Am Acad Child Adolesc Psychiatry. 2005;44(8):728–47.
Spanier GB. Measuring dyadic adjustment: new scale for assessing the quality of marriage and similar dyads. J Marriage Fam. 1976;38(1):15–28.
Helweg-Larsen M, Collins BE. The UCLA multidimensional condom attitudes scale: documenting the complex determinants of condom use in college students. Health Psychol. 1994;13(3):224–37.
Brafford LJ, Beck KH. Development and validation of a condom self-efficacy scale for college students. J Am Coll Health. 1991;39(5):219–25.
Kershaw TS, et al. Pregnancy as a window of opportunity for HIV prevention: effects of an HIV intervention delivered within prenatal care. Am J Public Health. 2009;99(11):2079–86.
Sikkema KJ, et al. HIV risk behaviors among women living in low-income, inner-city housing developments. Am J Public Health. 1996;86(8):1123–8.
Kenny DA, et al. Dyadic data analysis. New York: The Guilford Press; 2006.
Cohen S. Social relationships and health. Am Psychol. 2004;59(8):676–84.
Hamilton BE et al. Births: preliminary data for 2009. National vital statistics reports. Hyattsville: National Center for Health Statistics; 2010, 59(3).
Bowleg L, et al. What does it take to be a man? What is a real man?: ideologies of masculinity and HIV sexual risk among black heterosexual men. Cult Health Sex. 2011;13(5):545–59.
Coley RL. (In)visible men. Emerging research on low-income, unmarried, and minority fathers. Am Psychol. 2001;56(9):743–53.
Coley RL, Morris JE. Comparing father and mother reports of father involvement among low-income minority families. J Marriage Fam. 2002;64(4):982–97.
Bowleg L. Love, sex, and masculinity in sociocultural context. Men Masc. 2004;7(2):166–86.
Logan TK, et al. Women, sex, and HIV: social and contextual factors, meta-analysis of published interventions, and implications for practice and research. Psychol Bull. 2002;128(6):851–85.
Garnett GP, et al. Fewer partners or more condoms? Modeling the effectiveness of STI prevention interventions. Sex Transm Infect. 2008;84(Suppl 2):4–11.
Pinkerton SD, Abramson PR. Evaluating the risks: a Bernoulli process model of HIV infection and risk reduction. Eval Rev. 1993;17(5):504–28.
Johnson BT, et al. Behavioral interventions for African Americans to reduce sexual risk of HIV: a meta-analysis of randomized controlled trials. J Acquir Immune Defic Syndr. 2009;51(4):492–501.
Noar SM. Behavioral interventions to reduce HIV-related sexual risk behavior: review and synthesis of meta-analytic evidence. AIDS Behav. 2008;12(3):335–53.
El-Bassel N, et al. The efficacy of a relationship-based HIV/STD prevention program for heterosexual couples. Am J Public Health. 2003;93(6):963–9.
El-Bassel N, et al. Long-term effects of an HIV/STI sexual risk reduction intervention for heterosexual couples. AIDS Behav. 2005;9(1):1–13.
Milan S, et al. Prevalence, course, and predictors of emotional distress in pregnant and parenting adolescents. J Consult Clin Psychol. 2004;72(2):328–40.
Frosch CA, et al. Marital behavior and the security of preschooler-parent attachment relationships. J Fam Psychol. 2000;14(1):144–61.
Cutrona CE, et al. Predictors and correlates of continuing involvement with the baby’s father among adolescent mothers. J Fam Psychol. 1998;12(3):369–87.
Coyne JC, et al. Prognostic importance of marital quality for survival of congestive heart failure. Am J Cardiol. 2001;88(5):526–9.
Holt-Lunstad J, et al. Influence of a “warm touch” support enhancement intervention among married couples on ambulatory blood pressure, oxytocin, alpha amylase, and cortisol. Psychosom Med. 2008;70(9):976–85.
Holt-Lunstad J, et al. The influence of close relationships on nocturnal blood pressure dipping. Int J Psychophysiol. 2009;71(3):211–7.
Acknowledgment
This study is supported by a grant from the National Institutes of Mental Health (1R01MH75685).
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Kershaw, T., Arnold, A., Gordon, D. et al. In the Heart or in the Head: Relationship and Cognitive Influences on Sexual Risk Among Young Couples. AIDS Behav 16, 1522–1531 (2012). https://doi.org/10.1007/s10461-011-0049-1
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10461-011-0049-1