Abstract
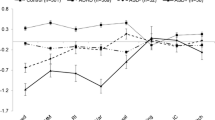
Attention problems are observed in attention-deficit/hyperactivity disorder (ADHD) and autism spectrum disorder (ASD). Most neuropsychological studies that compared both disorders focused on complex executive functions (EF), but missed to contrast basic attention functions, as well as ASD- and ADHD subtypes. The present study compared EF as well as basic attention functioning of children with the combined subtype (ADHD-C), the predominantly inattentive subtype (ADHD-I), and autism spectrum disorder without ADHD (ASD-) with typically developing controls (TD). Basic attention functions and EF profiles were analysed by testing the comprehensive attention function model of van Zomeren and Brouwer using profile analysis. Additionally, neurocognitive impairments in ASD- and ADHD were regressed on dimensional measures of attention- and hyperactive-impulsive symptoms across and within groups. ADHD-C revealed a strong impairment across measures of EF compared to ASD- and TD. The ADHD-C profile furthermore showed disorder specific impairments in interference control, whereas the ASD- profile showed a disorder specific impairment in basic attention component divided attention. Attention- and hyperactive-impulsive symptom severity did not predict neurocognitive impairments across- or within groups. Study findings thus support disorder and subtype specific attention/EF profiles, which refute the idea of a continuum of ADHD-I, ADHD-C, and ASD with increasing neurocognitive impairments.




Similar content being viewed by others
References
Rommelse NNJ, Geurts HM, Franke B, Buitelaar JK, Hartman CA (2011) A review on cognitive and brain endophenotypes that may be common in autism spectrum disorder and attention-deficit/hyperactivity disorder and facilitate the search for pleiotropic genes. Neurosci Biobehav Rev 35:1363–1396. https://doi.org/10.1007/s00787-010-0092-x
Taurines R, Schwenck C, Westerwald E, Sachse M, Siniatchkin M, Freitag C (2012) ADHD and autism: differential diagnosis or overlapping traits? A selective review. ADHD Atten Def Hyp Disord 4:115–139. https://doi.org/10.1007/s12402-012-0086-2
Goldstein S, Schwebach AJ (2004) The comorbidity of pervasive developmental disorder and attention deficit hyperactivity disorder: results of a retrospective chart review. J Autism Dev Disord 34:329–339. https://doi.org/10.1023/B:JADD.0000029554.46570.68
Leyfer OT, Folstein SE, Bacalman S, Davis NO, Dinh E, Morgan J, Tager-Flusberg H, Lainhart JE (2006) Comorbid psychiatric disorders in children with autism: interview development and rates of disorders. J Autism Dev Disord 36:849–861. https://doi.org/10.1007/s10803-006-0123-0
Sinzig J, Walter D, Doepfner M (2009) Attention deficit/hyperactivity disorder in children and adolescents with autism spectrum disorder: symptom or syndrome? J Atten Disord 13:117–126. https://doi.org/10.1177/1087054708326261
van der Meer JM, Oerlemans AM, van Steijn DJ, Lappenschaar MG, de Sonneville LM, Buitelaar JK, Rommelse NN (2012) Are autism spectrum disorder and attention-deficit/hyperactivity disorder different manifestations of one overarching disorder? Cognitive and symptom evidence from a clinical and population-based sample. J Am Acad Child Adolesc Psychiatry 51:1160–1172. https://doi.org/10.1016/j.jaac.2012.08.024
Chhabildas N, Pennington BF, Willcut EG (2001) A comparison of the neuropsychological profiles of the DSM-IV subtypes of ADHD. J Abnorm Child Psychol 29:529–540
Huang-Pollock CL, Mikami AY, Pfiffner L, McBurnett K (2007) ADHD subtype differences in motivational responsivity but not inhibitory control: evidence from a reward-based variation of the stop signal paradigm. J Clin Child Adolesc Psychol 36:127–136. https://doi.org/10.1080/15374410701274124
Nikolas MA, Nigg JT (2013) Neuropsychological performance and attention-deficit hyperactivity disorder subtypes and symptom dimensions. Neuropsychology 27:107–120. https://doi.org/10.1037/a0030685
Corbett BA, Constantine LJ, Hendren R, Rocke D, Ozonoff S (2009) Examining executive functioning in children with autism spectrum disorder, attention deficit hyperactivity disorder and typical development. Psychiatr Res 166:210–222. https://doi.org/10.1016/j.psychres.2008.02.005
Johnson KA, Robertson IH, Kelly SP, Silk TJ, Barry E, Dáibhis A, Watchorn A, Keavy M, Fitzgerald M, Gallagher L, Gill M, Bellgrove MA (2007) Dissociation in performance of children with ADHD and high-functioning autism on a task of sustained attention. Neuropsychologia 45:2234–2245. https://doi.org/10.1016/j.neuropsychologia.2007.02.019
Noterdaeme M, Amorosa H, Mildenberger K, Sitter S, Minow F (2001) Evaluation of attention problems in children with autism and children with a specific language disorder. Eur Child Adolesc Psychiatr 10:58–66. https://doi.org/10.1007/s007870170048
Craig F, Margari F, Legrottaglie AR, Palumbi R, de Giambattista C, Margari L (2016) A review of executive function deficits in autism spectrum disorder and attention-deficit/hyperactivity disorder. Neuropsychiatr Dis Treat 12:1191–1202. https://doi.org/10.2147/NDT.S104620
Lai CLE, Lau Z, Lui SSY, Lok E, Tam V, Chan Q, Cheng KM, Lam SM, Cheung EFC (2017) Meta-analysis of neuropsychological measures of executive functioning in children and adolescents with high-functioning autism spectrum disorder. Autism Res 10:911–939. https://doi.org/10.1002/aur.1723
Miyake A, Friedman NP, Emerson MJ, Witzki AH, Howerter A, Wager TD (2000) The unity and diversity of executive functions and their contributions to complex “Frontal Lobe” tasks: a latent variable analysis. Cogn Psychol 41:49–100. https://doi.org/10.1006/cogp.1999.0734
Alderson RM, Rapport MD, Kofler MJ (2007) Attention-deficit/hyperactivity disorder and behavioral inhibition: a meta-analytic review of the stop-signal paradigm. J Abnorm Child Psychol 35:745–758. https://doi.org/10.1007/s10802-007-9131-6
Geurts HM, Corbett B, Solomon M (2009) The paradox of cognitive flexibility in autism. Trends Cogn Sci 13:74–82. https://doi.org/10.1016/j.tics.2008.11.006
Geurts HM, Grasman PPP, Verté S, Oosterlaan J, Roeyers H, van Kammen SM, Sergeant JA (2008) Intra individual variability in ADHD, autism spectrum disorders and Tourette’s syndrome. Neuropsychologia 46:3030–3041. https://doi.org/10.1016/j.neuropsychologia.2008.06.013
Lijffijt M, Kenemans JL, Verbaten MN, van Engeland H (2005) A meta-analytic review of stopping performance in attention-deficit/hyperactivity disorder: deficient inhibitory motor control? J Abnorm Child Psychol 114:216–222. https://doi.org/10.1037/0021-843X.114.2.216
van Zomeren AH, Brouwer WH (1994) Clinical neuropsychology of attention. Oxford University Press, New York
Posner MI, Walker JA, Friedrich FA, Rafal RD (1987) How do the parietal lobes direct covert attention? Neuropsychologia 25:135–145
Norman DA, Shallice T (1986) Attention to action: willed and automatic control of behaviour. In: Davidson RJ, Schwartz GE, Shapiro D (eds) Consciousness and self-regulation: advances in research and theory. Plenum Press, New York
Tucha L, Tucha O, Walitza S, Sontag TA, Laufkötter R, Linder M, Lange KW (2009) Vigilance and sustained attention in children and adults with ADHD. J Atten Disord 12:410–421. https://doi.org/10.1177/1087054708315065
Tucha O, Walitza S, Mecklinger L, Sontag TA, Kübber S, Linder M, Lange KW (2006) Attentional functioning in children with ADHD - predominantly hyperactive-impulsive type and children with ADHD—combined type. J Neural Transm 113:1943–1953. https://doi.org/10.1007/s00702-006-0496-450
Johnson KA, Robertson IA, Barry E, Mulligan A, Daibhis A, Daly M, Watchorn A, Gill M, Bellgrove MA (2008) Impaired conflict resolution and alerting in children with ADHD: evidence from the Attention Network Task (ANT). J Child Psychol Psychiatr 49:1339–1347. https://doi.org/10.1111/j.1469-7610.2008.01936.x
Samyn V, Roeyers H, Bijttebier P, Wiersema JR (2013) Attentional networks in boys with ADHD or Autism Spectrum Disorder and the relationship with effortful control. J Atten Disord. https://doi.org/10.1177/1087054712473183
Keehn B, Lincoln AJ, Müller RA, Townsend J (2010) Attentional networks in children and adolescents with autism spectrum disorder. J Child Psychol Psychiatr 51:1251–1259. https://doi.org/10.1111/j.1469-7610.2010.02257.x
van den Bergh B, Mennes M, Stevens V, van der Meere J, Börger N, Stiers P, Marcoen A, Lagae L (2006) ADHD deficit as measured in adolescent boys with a continuous performance task is related to antenatal maternal anxiety. Pedriatic Res 59:78–82. https://doi.org/10.1203/01.pdr.0000191143.75673.52
Tucha L, Fuermaier ABM, Koerts J, Buggenthin R, Aschenbrenner S, Weisbrod M, Thome J, Lange KW, Tucha O (2017) Sustained attention in adult ADHD: time-on-task effects of various measures of attention. J Neural Trans 124:39–53. https://doi.org/10.1007/s00702-015-1426-0
Huang-Pollock CL, Karalunas SL, Tam H, Moore AN (2012) Evaluating vigilance deficits in ADHD: a meta-analysis of CPT performance. J Abnorm Psychol 12:360–371. https://doi.org/10.1037/a0027205
Sinzig J, Bruning N, Morsch D, Lehmkuhl G (2008) Attention profiles in autistic children with and without comorbid hyperactivity and attention problems. Acta Neuropsychiatrica 20:207–215. https://doi.org/10.1111/j.1601-5215.2008.00292.x
Frazier TW, Demaree HA, Youngstrom EA (2004) Meta-analysis of intellectual and neuropsychological test performance in attention-deficit/hyperactivity disorder. Neuropsychology 18:543–555. https://doi.org/10.1037/0894-4105.18.3.543
Pasini A, Paloscia C, Alessandrelli R, Porfirio MC, Curatolo P (2007) Attention and executive functions profile in drug naive ADHD subtypes. Brain Dev 29:400–408. https://doi.org/10.1016/j.braindev.2006.11.010
Willcutt EG, Doyle AE, Nigg JT, Faraone SV, Pennington BF (2005) Validity of the executive function theory of attention-deficit/hyperactivity disorder: a meta-analytic review. Biol Psychiat 57:1336–1346. https://doi.org/10.1016/j.biopsych.2005.02.006
Günther T, Knospe EL, Herpertz-Dahlmann B, Konrad K (2015) Sex differences in attentional performance in a clinical sample with ADHD of the combined subtype. J Atten Disord 19:764–770. https://doi.org/10.1177/1087054712461176
Althaus M, de Sonneville LM, Minderaa RB, Hensen LG, Til RB (1996) Information processing and aspects of visual attention in children with the DSM-III-R diagnosis “pervasive developmental disorder not otherwise specified” (PDDNOS): I. Focused and divided attention. Child Neuropsychol 2:7–29. https://doi.org/10.1080/09297049608401347
Albrecht B, Brandeis D, Uebel H, Heinrich H, Mueller UC, Hasselhorn M, Steinhausen H, Rotherberger A, Banaschewski T (2008) Action monitoring in boys with attention-deficit/hyperactivity disorder, their nonaffected siblings, and normal control subjects: evidence for an endophenotype. Biol Psychiat 64:615–625. https://doi.org/10.1016/j.biopsych.2007.12.016
Tye C, Asherson P, Ashwood KL, Azadi B, Bolton P, McLoughlin G (2014) Attention and inhibition in children with ASD, ADHD and co-morbid ASD + ADHD: an event-related potential study. Psychol Med 44:1101–1116. https://doi.org/10.1017/S0033291713001049
Huang-Pollock CL, Nigg JT (2003) Searching for the attention deficit in attention deficit hyperactivity disorder: the case of visuospatial orienting. Clin Psychol Rev 23:801–830. https://doi.org/10.1016/S0272-7358(03)00073-4
Landry O, Parker A (2013) A meta-analysis of visual orienting in autism. Front Hum Neurosci 7:833. https://doi.org/10.3389/fnhum.2013.00833
Semrud-Clikeman M, Walkowiak J, Wilkinson A, Butcher B (2010) Executive functioning in children with Asperger syndrome, ADHD-combined type, ADHD-predominately inattentive type, and controls. J Autism Dev Disord 40:1017–1027. https://doi.org/10.1007/s10803-010-0951-9
Rühl D, Bölte S, Feineis-Matthews S, Poustka F (2004) ADOS. Diagnostische Beobachtungsskala für autistische Störungen. Huber, Bern
Bölte S, Rühl D, Schmötzer GPF (2006) ADI-R. Diagnostisches Interview für Autismus-revidiert. Huber, Bern
American Psychiatric Association (2000) Diagnostic and statistical manual of mental disorders, 4th edition, text revision (DSM-IV-TR). American Psychiatric Association, Washington
Achenbach TM (1991) Manual for the child behavior checklist and 1991 profile. University of Vermont, Department of Psychiatry, Burlington
Schneider S, Unnewehr S, Margraf J (2009) Kinder-DIPS. Diagnostisches Interview bei psychischen Störungen im Kindes- und Jugendalter. Springer, Berlin
Döpfner M, Lehmkuhl G (1998) Diagnostik-System für psychische Störungen im Kindes- und Jugendalter nach ICD-10 und DSM-IV: DISYPS-KJ; klinische Diagnostik—Elternurteil—Erzieher- und Lehrerurteil—Selbsturteil, 1st edn. Huber, Bern
Bölte S, Poustka F (2006) FSK Fragebogen zur Sozialen Kommunikation—Autismus Screening. Huber, Bern
Zimmermann P, Fimm B (2007) Testbatterie zur Aufmerksamkeitsprüfung (TAP), Version 2.1. Psytest, Herzogenrath
Erhart M, Dopfner M, Ravens-Sieberer U (2008) Psychometric properties of two ADHD questionnaires: comparing the Conners’ scale and the FBB-HKS in the general population of German children and adolescents–results of the BELLA study. Eur Child Adolesc Psychiat 17:106–115. https://doi.org/10.1007/s00787-008-1012-1
IBM Corp. Released (2013) IBM SPSS Statistics for Windows, Version 22.0. IBM Corp, Armonk
Benjamini Y, Hochberg Y (1995) Controlling the false discovery rate: a practical and powerful approach to multiple testing. J R Stat Soc Ser B Methodol 57:289–300. https://doi.org/10.2307/2346101
Adams ZW, Derefinko KJ, Milich R, Fillmore MT (2008) Inhibitory functioning across ADHD subtypes: recent findings, clinical implications, and future directions. Dev Disabil Res Rev 14:268–275. https://doi.org/10.1002/ddrr.37
De La Fuente A, Xia S, Branch C, Li X (2013) A review of attention-deficit/hyperactivity disorder from the perspective of brain networks. Front Hum Neurosci 7:192. https://doi.org/10.3389/fnhum.2013.00192
Reed P, McCarthy J (2012) Cross-modal attention-switching is impaired in autism spectrum disorders. J Autism Dev Disord 42:947–953. https://doi.org/10.1007/s10803-011-1324-8
Sachse M, Schlitt S, Hainz D, Ciaramidaro A, Schirman S, Walter H, Poustka F, Bolte S, Freitag CM (2013) Executive and visuo-motor function in adolescents and adults with autism spectrum disorder. J Autism Dev Disord 43:1222–1235
Sacrey LA, Armstrong VL, Bryson SE, Zwaigenbaum L (2014) Impairments to visual disengagement in autism spectrum disorder: a review of experimental studies from infancy to adulthood. Neurosci Biobehav Rev 47:559–577
O’Halloran L, Cao Z, Ruddy K et al (2017) Neural circuitry underlying sustained attention in healthy adolescents and in ADHD symptomatology. Neuroimage 169:395–406. https://doi.org/10.1016/j.neuroimage.2017.12.030
Verté S, Geurts HM, Roeyers H, Oosterlaan J, Sergeant JA (2006) The relationship of working memory, inhibition, and response variability in child psychopathology. J Neurosci Methods 151:5–14. https://doi.org/10.1016/j.jneumeth.2005.08.023
Lukito S, Jones CRG, Pickles A, Baird G, Happé F, Charman T, Simonoff E (2017) Specificity of executive function and theory of mind performance in relation to attention-deficit/hyperactivity symptoms in autism spectrum. Mol Autism 8:60. https://doi.org/10.1186/s13229-017-0177-1
Happé F, Booth R, Charlton R, Hughes C (2006) Executive function deficits in autism spectrum disorders and attention-deficit/hyperactivity disorder: examining profiles across domains and ages. Brain Cogn 61:25–39. https://doi.org/10.1016/j.bandc.2006.03.004
Jepsen JR, Fagerlund B, Mortensen EL (2009) Do attention deficits influence IQ assessment in children and adolescents with ADHD? J Atten Disord 12:551–562
Reiersen AM, Constantino JN, Volk HE, Todd RD (2007) Autistic traits in a population-based ADHD twin sample. J Child Psychol Psychiatry 48:464–472. https://doi.org/10.1111/j.1469-7610.2006.01720.x
Ronald A, Simonoff E, Kuntsi J, Asherson P, Plomin R (2008) Evidence for overlapping genetic influences on autistic and ADHD behaviours in a community twin sample. J Child Psychol Psychiatr 49:535–542. https://doi.org/10.1111/j.1469-76.10.2006.01720.x
Simonoff E, Pickles A, Charman T, Chandler S, Loucas T, Baird G (2008) Psychiatric disorders in children with autism spectrum disorders: prevalence, comorbidity, and associated factors in a population-derived sample. J Am Acad Child Adolesc Psychiatr 47:921–929. https://doi.org/10.1097/CHI.0b013e318179964f
Coghill D, Sonuga-Barke EJS (2012) Annual research review: categories versus dimensions in the classification and conceptualisation of child and adolescent mental disorders–implications of recent empirical study. J Child Psychol Psychiatr 53:469–489. https://doi.org/10.1111/j.1469-7610.2011.02511.x
Acknowledgements
We gratefully thank all children and their families for their participation in our study. Data collection was supported by grants of the German Research Foundation DFG to Christine M. Freitag and Jobst Meyer (Grants ME 1923/5-1, ME 1923/5-3), the German Federal Ministry of Education and Research (BMBF) Grant 01GV0605, and the BMBF/EC ERA-Net Grant 01EW1105 to Christine M. Freitag. Data analysis and writing was supported by the EU funded International Training Network MiND to CMF (Grant Number 82600321). CMF receives royalties for books on Attention-Deficit/Hyperactivity Disorder and Autism Spectrum Disorder. She has served as consultant to Desitin and Roche.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
None of the other authors has to report any conflict of interests.
Rights and permissions
About this article
Cite this article
Boxhoorn, S., Lopez, E., Schmidt, C. et al. Attention profiles in autism spectrum disorder and subtypes of attention-deficit/hyperactivity disorder. Eur Child Adolesc Psychiatry 27, 1433–1447 (2018). https://doi.org/10.1007/s00787-018-1138-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00787-018-1138-8