Abstract
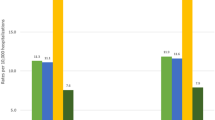
Suicide is one of the leading causes of maternal mortality in many countries, but little is known about the epidemiology of suicide and suicidal behavior among pregnant women in the USA. We sought to examine trends and provide nationally representative estimates for suicidal behavior (including suicidal ideation and suicide and self-inflicted injury) among pregnant women from 2006 to 2012 in the USA. Pregnant women aged 12–55 years were identified through pregnancy- and delivery-related hospitalization records from the National (Nationwide) Inpatient Sample. Suicidal behavior was identified by the International Classification of Diseases, Ninth Revision, Clinical Modification codes. Annual, nationwide estimates and trends were determined using discharge and hospital weights. The prevalence of suicidal ideation more than doubled from 2006 to 2012 (47.5 to 115.0 per 100,000 pregnancy- and delivery-related hospitalizations), whereas the prevalence of suicide and self-inflicted injury remained stable. Nearly 10 % of suicidal behavior occurred in the 12–18-year group, showing the highest prevalence per 100,000 pregnancy- and delivery-related hospitalizations (158.8 in 2006 and 308.7 in 2012) over the study period. For suicidal ideation, blacks had higher prevalence than whites; women in the lowest income quartile had the highest prevalence. Although the prevalence of suicidal behavior was higher among hospitalizations with depression diagnoses, more than 30 % of hospitalizations were for suicidal behavior without depression diagnoses. Our findings highlight the increasing burden and racial differences in suicidal ideation among US pregnant women. Targeted suicide prevention efforts are needed for high-risk pregnant women including teens, blacks, and low-income women.



Similar content being viewed by others
References
Agampodi S, Wickramage K, Agampodi T, Thennakoon U, Jayathilaka N, Karunarathna D, Alagiyawanna S (2014) Maternal mortality revisited: the application of the new ICD-MM classification system in reference to maternal deaths in Sri Lanka. Reprod Health 11:17
Appleby L (1991) Suicide during pregnancy and in the first postnatal year. BMJ 302:137–140
Asad N, Karmaliani R, Sullaiman N, Bann CM, McClure EM, Pasha O, Wright LL, Goldenberg RL (2010) Prevalence of suicidal thoughts and attempts among pregnant Pakistani women. Acta Obstet Gynecol Scand 89:1545–1551
Austin M-P, Kildea S (2007) Maternal mortality and psychiatric morbidity in the perinatal period: challenges and opportunities for prevention in the Australian setting. Med J Aust 186:364–367
Bates DW, Evans RS, Murff H, Stetson PD, Pizziferri L, Hripcsak G (2003) Detecting adverse events using information technology. J Am Med Inform Assoc 10:115–128
Bryant A, Mhyre JM, Leffert LR, Hoban RA, Yakoob MY, Bateman BT (2012) The association of maternal race and ethnicity and the risk of postpartum hemorrhage. Anesth Analg 115:1127–1136
Callahan ST, Fuchs DC, Shelton RC, Balmer LS, Dudley JA, Gideon PS, DeRanieri MM, Stratton SM, Williams CL, Ray WA (2013) Identifying suicidal behavior among adolescents using administrative claims data. Pharmacoepidemiol Drug Saf 22:769–775
Centers for Disease Control and Prevention (2015) Deaths: final data for 2013. http://www.cdc.gov/nchs/data/nvsr/nvsr64/nvsr64_02.pdf. Accessed 18 September 2015
Chang J, Berg CJ, Saltzman LE, Herndon J (2005) Homicide: a leading cause of injury deaths among pregnant and postpartum women in the United States, 1991–1999. Am J Public Health 95:471
Cockburn J, Pawson ME (2007) Psychological challenges in obstetrics and gynecology. Springer, New York
Czeizel AE (2011) Attempted suicide and pregnancy. J Inj Violence 3:45–54
Czeizel AE, Tomcsik M, Tímár L (1997) Teratologic evaluation of 178 infants born to mothers who attempted suicide by drugs during pregnancy. Obstet Gynecol 90:195–201
Doshi A, Boudreaux ED, Wang N, Pelletier AJ, Camargo CA (2005) National study of US emergency department visits for attempted suicide and self-inflicted injury, 1997–2001. Ann Emerg Med 46:369–375
Economou M, Madianos M, Peppou LE, Theleritis C, Patelakis A, Stefanis C (2013) Suicidal ideation and reported suicide attempts in Greece during the economic crisis. World Psychiatry 12:53–59
Federal Reserve Bank of Minneapolis (2015) Consumer price index, 1913. https://www.minneapolisfed.org/community/teaching-aids/cpi-calculator-information/consumer-price-index-and-inflation-rates-1913. Accessed 12 February 2015
Fischer LR, Rush WA, Kluznik JC, O’Connor PJ, Hanson AM (2008) Abstract C-C1-06: identifying depression among diabetes patients using natural language processing of office notes. Clin Med Res 6:125–126
Frautschi S, Cerulli A, Maine D (1994) Suicide during pregnancy and its neglect as a component of maternal mortality. Int J Gynaecol Obstet 47:275–284
Fuhr DC, Calvert C, Ronsmans C, Chandra PS, Sikander S, De Silva MJ, Patel V (2014) Contribution of suicide and injuries to pregnancy-related mortality in low-income and middle-income countries: a systematic review and meta-analysis. Lancet Psychiatry 1:213–225
Gandhi SG, Gilbert WM, McElvy SS, El Kady D, Danielson B, Xing G, Smith LH (2006) Maternal and neonatal outcomes after attempted suicide. Obstet Gynecol 107:984–990
Gavin AR, Tabb KM, Melville JL, Guo Y, Katon W (2011) Prevalence and correlates of suicidal ideation during pregnancy. Arch Womens Ment Health 14:239–246
Gentile S (2011) Suicidal mothers. J Inj Violence research 3:90–97
Gibbs JT (1997) African‐American suicide: a cultural paradox. Suicide Life Threat Behav 27:68–79
Gissler M, Hemminki E, Lonnqvist J (1996) Suicides after pregnancy in Finland, 1987–1994: register linkage study. BMJ 313:1431–1434
Gold KJ, Singh V, Marcus SM, Palladino CL (2012) Mental health, substance use and intimate partner problems among pregnant and postpartum suicide victims in the National Violent Death Reporting System. Gen Hosp Psychistry 34:139–145
Gunnell D, Lopatatzidis A, Dorling D, Wehner H, Southall H, Frankel S (1999) Suicide and unemployment in young people. Analysis of trends in England and Wales, 1921–1995. Br J Psychiatry 175:263–270
Healthcare Cost and Utilization Project (HCUP) (2015a) Introduction to the HCUP National Inpatient Sample (NIS). https://www.hcup-us.ahrq.gov/db/nation/nis/NISIntroduction2012.pdf. Accessed 1 February 2015
Healthcare Cost and Utilization Project (HCUP) (2015b) Introduction to the HCUP Nationwide Inpatient Sample (NIS). https://www.hcup-us.ahrq.gov/db/nation/nis/nisarchive.jsp. Accessed 1 February 2015
Healthcare Cost and Utilization Project (HCUP) (2015c) Nationwide Inpatient Sample (NIS) Redesign Report. http://www.hcup-us.ahrq.gov/db/nation/nis/reports/NISRedesignFinalReport040914.pdf. Accessed 1 February 2015
Healthcare Cost and Utilization Project (HCUP) (2015d) Trend weights for HCUP NIS data. https://www.hcup-us.ahrq.gov/db/nation/nis/trendwghts.jsp. Accessed 1 February 2015
Hornbrook MC, Whitlock EP, Berg CJ, Callaghan WM, Bachman DJ, Gold R, Bruce FC, Dietz PM, Williams SB (2007) Development of an algorithm to identify pregnancy episodes in an integrated health care delivery system. Health Serv Res 42:908–927
Huang H, Faisal-Cury A, Chan Y-F, Tabb K, Katon W, Menezes PR (2012) Suicidal ideation during pregnancy: prevalence and associated factors among low-income women in São Paulo, Brazil. Arch Womens Ment Health 15:135–138
Jha AK (2011) The promise of electronic records: around the corner or down the road? JAMA 306:880–881
Kendell R (1991) Suicide in pregnancy and the puerperium. BMJ 302:126
Kessler RC, Borges G, Walters EE (1999) Prevalence of and risk factors for lifetime suicide attempts in the National Comorbidity Survey. Arch Gen Psychiatry 56:617–626
Kessler RC, Berglund P, Borges G, Nock M, Wang PS (2005) Trends in suicide ideation, plans, gestures, and attempts in the United States, 1990–1992 to 2001–2003. JAMA 293:2487–2495
Kozhimannil KB, Trinacty CM, Busch AB, Huskamp HA, Adams AS (2011) Racial and ethnic disparities in postpartum depression care among low-income women. Psychiatr Serv 62:619–625
Kuklina EV, Whiteman MK, Hillis SD, Jamieson DJ, Meikle SF, Posner SF, Marchbanks PA (2008) An enhanced method for identifying obstetric deliveries: implications for estimating maternal morbidity. Matern Child Health J 12:469–477
Lindahl V, Pearson JL, Colpe L (2005) Prevalence of suicidality during pregnancy and the postpartum. Arch Womens Ment Health 8:77–87
Lorant V, Kunst AE, Huisman M, Costa G, Mackenbach J (2005) Socio-economic inequalities in suicide: a European comparative study. Br J Psychiatry 187:49–54
Lowry R, Crosby AE, Brener ND, Kann L (2014) Suicidal thoughts and attempts among US high school students: trends and associated health-risk behaviors, 1991–2011. J Adolesc Health 54:100–108
Marzuk PM, Tardiff K, Leon AC, Hirsch CS, Portera L, Hartwell N, Iqbal MI (1997) Lower risk of suicide during pregnancy. Am J Psychiatry 154:122–123
Mauri M, Oppo A, Borri C, Banti S (2012) SUICIDALITY in the perinatal period: comparison of two self-report instruments. Results from PND-ReScU. Arch Womens Ment Health 15:39–47
McMillan KA, Enns MW, Asmundson G, Sareen J (2010) The association between income and distress, mental disorders, and suicidal ideation and attempts: findings from the collaborative psychiatric epidemiology surveys. J Clin Psychiatry 71:1168–1175
Mościcki E, O’Carroll P, Rae D, Locke B, Roy A, Regier D (1988) Suicide attempts in the epidemiologic catchment area study. Yale J Biol Med 61:259
Murff HJ, FitzHenry F, Matheny ME, Gentry N, Kotter KL, Crimin K, Dittus RS, Rosen AK, Elkin PL, Brown SH (2011) Automated identification of postoperative complications within an electronic medical record using natural language processing. JAMA 306:848–855
National Cancer Institute (2015) Standard populations—single ages. http://seer.cancer.gov/stdpopulations/stdpop.singleages.html. Accessed 1 February 2015
Nelson AR, Smedley BD, Stith AY (2002) Unequal treatment: confronting racial and ethnic disparities in health care. National Academies Press, Washington
Nock M, Nock MK, Borges G, Ono Y (2012) Suicide: global perspectives from the WHO world mental health surveys. Cambridge University Press, New York
Oates M (2003) Suicide: the leading cause of maternal death. Br J Psychiatry 183:279–281
Orr ST, Blazer DG, James SA (2006) Racial disparities in elevated prenatal depressive symptoms among black and white women in eastern North Carolina. Ann Epidemiol 16:463–468
Pagura J, Cox BJ, Sareen J, Enns MW (2008) Factors associated with multiple versus single episode suicide attempts in the 1990–1992 and 2001–2003 United States national comorbidity surveys. J Nerv Ment Dis 196:806–813
Paris R, Bolton RE, Weinberg MK (2009) Postpartum depression, suicidality, and mother-infant interactions. Arch Womens Ment Health 12:309–321
Perez-Rodriguez MM, Baca-Garcia E, Oquendo MA, Blanco C (2008) Ethnic differences in suicidal ideation and attempts. Prim psychiatry 15:44
Perlis R, Iosifescu D, Castro V, Murphy S, Gainer V, Minnier J, Cai T, Goryachev S, Zeng Q, Gallagher P (2012) Using electronic medical records to enable large-scale studies in psychiatry: treatment resistant depression as a model. Psychol Med 42:41–50
Phillips MR (2014) Pregnancy and suicide: towards a coherent narrative. Lancet Psychiatry 1:168–170
Pinheiro RT, da Cunha Coelho FM, da Silva RA, de Ávila QL, de Mattos Souza LD, Castelli RD, de Matos MB, Pinheiro KAT (2012) Suicidal behavior in pregnant teenagers in southern Brazil: social, obstetric and psychiatric correlates. J Affect Disord 136:520–525
Research Triangle Institute (2014) SUDAAN example manual. Research Triangle Park, NC
Rockett IR, Samora JB, Coben JH (2006) The black–white suicide paradox: possible effects of misclassification. Soc Sci Med 63:2165–2175
Scott LN, Pilkonis PA, Hipwell AE, Keenan K, Stepp SD (2015) Non-suicidal self-injury and suicidal ideation as predictors of suicide attempts in adolescent girls: a multi-wave prospective study. Compr Psychiatry 58:1–10
Shadigian EM, Bauer ST (2005) Pregnancy-associated death: a qualitative systematic review of homicide and suicide. Obstet Gynecol Surv 60:183–190
Shaffer D, Gould M, Hicks RC (1994) Worsening suicide rate in black teenagers. Am J Psychiatry 151:1810–1812
Silverman JG, Raj A, Mucci LA, Hathaway JE (2001) Dating violence against adolescent girls and associated substance use, unhealthy weight control, sexual risk behavior, pregnancy, and suicidality. JAMA 286:572–579
Ting SA, Sullivan AF, Boudreaux ED, Miller I, Camargo CA (2012) Trends in US emergency department visits for attempted suicide and self-inflicted injury, 1993–2008. Gen Hosp Psychistry 34:557–565
World Health Organization, Practice Management Information Corporation (1998) ICD-9-CM: International Classification of Diseases, 9th Revision: Clinical Modification vol 1. Practice Management Information Corporation, Los Angeles, PMIC
Yusuf HR, Akhter HH, Chowdhury ME, Rochat RW (2007) Causes of death among women aged 10–50 years in Bangladesh, 1996–1997. J Health Popul Nutr 25:302
Zhong QY, Gelaye B, Rondon MB, Sánchez SE, Simon GE, Henderson DC, Barrios YV, Sánchez PM, Williams MA (2014) Using the Patient Health Questionnaire (PHQ-9) and the Edinburgh Postnatal Depression Scale (EPDS) to assess suicidal ideation among pregnant women in Lima, Peru. Arch Womens Ment Health 18:783–792
Acknowledgments
This research was supported by awards from the National Institutes of Health (the National Institute on Minority Health and Health Disparities T37-MD001449 and the National Center for Research Resources (NCRR), the National Center for Advancing Translational Sciences (NCATS) 8UL1TR 000170–05). The authors would like to thank Dr. Miguel-Angel Luque Fernandez and Dr. Wenyuan Li for their help with programming. The authors would like to thank Kathy Brenner for the help with editing this manuscript. Special thanks are extended to the Research Computing Group at the Faculty of Art and Sciences of Harvard University, for the continuous support with computational resources.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interests
The authors declare that there are no conflicts of interest.
Additional file
Below is the link to the electronic supplementary material.
Additional file 1
eTable 1 ICD-9-CM diagnosis and procedure codes, DRG codes used to determine pregnancy- and delivery-related hospitalizations. eTable 2 ICD-9-CM diagnosis codes used to identify depression diagnoses. eTable 3a Characteristics of pregnant women with suicidal ideation-related hospitalizations. eTable 3b Characteristics of pregnant women with suicide- and self-inflicted injury-related hospitalizations. eTable 4 Suicidal behavior-related hospitalizations according to age groups among pregnant women. eTable 5 Suicidal behavior-related hospitalizations according to race among pregnant women. eTable 5a Suicidal ideation-related hospitalizations according to race among pregnant women. eTable 5b Suicide- and self-inflicted injury-related hospitalizations according to race among pregnant women. eTable 6 Suicidal behavior-related hospitalizations according to median household income quartiles for patient zip code among pregnant women. eTable 6a Suicidal ideation-related hospitalizations according to median household income quartiles for patient zip code among pregnant women. eTable 6b Suicide- and self-inflicted injury-related hospitalizations according to median household income quartiles for patient zip code among pregnant women. eTable 7 Suicidal behavior-related hospitalizations according to race and median household income quartiles for patient zip code among pregnant women. eTable 7a Suicidal ideation-related hospitalizations according to race and median household income quartiles for patient zip code among pregnant women. eTable 7b Suicide- and self-inflicted injury-related hospitalizations according to race and median household income quartiles for patient zip code among pregnant women. eTable 8 Suicidal behavior-related hospitalizations according to depression diagnoses among pregnant women. eTable 8a Suicidal ideation-related hospitalizations according to depression status among pregnant women. eTable 8b Suicide- and self-inflicted injury-related hospitalizations according to depression status among pregnant women. eFigure 1 National trends in annual numbers of suicidal-behavior related hospitalizations among pregnant women. eFigure 2 Suicidal behavior-related hospitalizations according to median household income quartiles for patient zip code among pregnant women. eFigure 3 Suicidal behavior-related hospitalizations according to depression diagnoses among pregnant women. (DOCX 553 KB)
Rights and permissions
About this article
Cite this article
Zhong, QY., Gelaye, B., Miller, M. et al. Suicidal behavior-related hospitalizations among pregnant women in the USA, 2006–2012. Arch Womens Ment Health 19, 463–472 (2016). https://doi.org/10.1007/s00737-015-0597-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00737-015-0597-x