Abstract
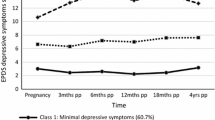
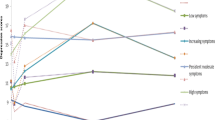
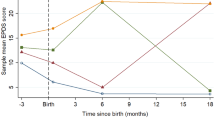
Approximately 14 % of women experience depressive symptoms in the first postnatal year. Few studies have examined the persistence of symptoms beyond this time. This study aims to (a) assess the course of women’s depressive symptoms from the first postnatal year to when their children were aged 6–7 years, (b) identify distinct groups of women defined by their symptom trajectories over time, and (c) identify antenatal and early postnatal risk factors associated with persistent symptoms. Data from 4,879 women participating in the Longitudinal Study of Australian Children were analysed using latent growth modelling and logistic regression to identify risk factors associated with class membership. For the overall sample, depressive symptoms were highest during the first postnatal year and then gradually decreased over 6–7 years. Two distinct classes were identified with the majority of women (84 %) reporting minimal symptoms over time, and 16 % experiencing persistently high symptoms. Risk factors were younger maternal age, being from a non-English speaking background, not completing high school, having a past history of depression, antidepressant use during pregnancy, child development problems, lower parenting self-efficacy, poor relationship quality, and stressful life events. This research identifies risk factors that may predispose mothers to enduring depressive symptoms, offering opportunities for early identification and targeted early intervention.

Similar content being viewed by others
References
Affonso D, Lovett S, Paul S, Sheptak S, Nussbaum R, Newman L, Johnson B (1992) Dysphoric distress in childbearing women. J Perinatol 12(4):325–332
Bandura A (1997) Self-efficacy: the exercise of control. Freeman, New York
Beck CT (1996) Postpartum depressed mothers’ experience interacting with their children. Nurs Res 45(2):98–104
Beeghly M, Weinberg M, Olson K, Kernan H, Riley J, Tronick E (2002) Stability and change in level of maternal depressive symptomatology during the first postpartum year. J Affect Disord 71:169–180
Bentler P (1990) Comparative fit indexes in structural models. Psychol Bull 107(2):238–246
Bryanton J, Gagnon A, Hatem M, Johnston C (2008) Predictors of early parenting self-efficacy: results of a prospective cohort study. Nurs Res 57(4):252–259
Burke L (2003) The impact of maternal depression on familial relationships. Int Rev Psychiatry 15:243–255
Campbell S, Cohn J (1997) The timing and chronicity of postpartum depression. Implications for infant development. In: Copper PJ (ed) Postpartum depression and child development. Guildford, New York, pp 165–197
Chen Y, Subramanian S, Acevedo-Garcia D, Kawachi I (2005) Women’s status and depressive symptoms: a multilevel analysis. Soc Sci Med 60:49–60
Commonwealth Department of Family and Community Services (2004) Parenting information project. Volume 1: Main report. Canberra, Australia
Cooke M, Schmied V, Sheehan A (2007) An exploration of the relationship between postnatal distress and maternal role attainment, breast feeding problems and breast feeding cessation in Australia. Midwifery 23:66–76
Evans J, Heron J, Francomb H, Oke S, Golding J (2001) Cohort study of depressed mood during pregnancy and after childbirth. Br Med J 232:257–260
Giallo R, Cooklin A, Wade C, D’Esposito F, Nicholson J (2014) Maternal postnatal mental health and later emotional-behavioural development of children: the mediating role of parenting behaviour. Child: Care, Health and Development (in press)
Glascoe F (2000) Parents evaluation of developmental status—authorised Australian version. Centre for Community Child Health, Parkville
Goodman J (2004) Paternal postpartum depression, its relationship to maternal postpartum depression, and implications for family health. J Adv Nurs 45(1):26–35
Grace S, Evindar A, Stewart D (2003) The effect of postpartum depression on child cognitive development and behavior: a review and critical analysis of the literature. Arch Womens Ment Health 6:263–273
Halligan S, Murray L, Martins C, Cooper P (2007) Maternal depression and psychiatric outcomes in adolescent offspring: a 13-year longitudinal study. J Affect Disord 97:145–154
Hendrick S (1988) A generic measure of relationship satisfaction. J Marriage Fam 50(1):93–98
Hiscock H, Wake M (2001) Infant sleep problems and postnatal depression: a community-based study. Pediatrics 107(6):1317–1322
Horowitz J, Goodman J (2004) A longitudinal study of maternal postpartum depression symptoms. Res Theory Nurs Pract Int J 18(2/3):149–163
Horowitz J, Damato E, Solon L, von Metzsch G (1996) Identification of symptoms of postpartum depression: linking research to practice. J Perinatol 16(5):360–365
Jones T, Prinz R (2005) Potential roles of parental self-efficacy in parent and child adjustment: a review. Clin Psychol Rev 25(3):341–363
Kessler R, Barker P, Cople L, Epstein J, Gfroerer J, Hiripi E, Howes M, Normand S, Manderscheid R, Walters E, Zaslavsky A (2003) Screening for serious mental illness in the general population. Arch Psychiatry 60:184–189
Klier C, Rosenbaum K, Zeller M, Steinhardt K, Bergemann N, Muzik M (2008) A multirisk approach to predicting chronicity of postpartum depressive symptoms. Depression Anxiety 25:718–724
Kumar R, Robson M (1984) A prospective study of emotional disorders in childbearing women. Br J Psychiatry 144:35–47
Leahy-Warren P, McCarthy G, Corcoran P (2012) First-time mothers: social support, maternal parental self-efficacy and postnatal depression. J Clin Nurs 21(3–4):388–397
Leigh B, Milgrom J (2008) Risk factors for antenatal depression, postnatal depression and parenting stress. BMC Psychiatry 8(24)
Matthey S, Barnett B, Ungerer J, Waters B (2000) Paternal and maternal depressed mood during the transition to parenthood. J Affect Disord 60:75–85. doi:10.1016/S0165-0327(99)00159-7
McCue Horwitz S, Briggs-Gowan M, Storfer-Isser A, Carter A (2007) Prevalence, correlates, and persistence of maternal depression. J Women's Health 16(5):678–691
McLennan J, Kotelchuck M, Cho H (2001) Prevalence, persistence, and correlates of depressive symptoms in a national sample of mothers of toddlers. J Am Acad Child Adolesc Psychiatry 40(11):1316–1323
McMahon CA, Trapolini T, Barnett B (2008) Maternal state of mind regarding attachment predicts persistence of postnatal depression in the preschool years. J Affect Disord 107:199–203. doi:10.1016/j.jad.2007.07.017
Murray L, Sinclair D, Cooper P, Ducournau P, Turner P (1999) The socioemotional development of 5-year-old children of postnatally depressed mothers. J Child Psychol Psychiatry 40(8):1259–1271
Muthen L, Muthen B (1998–2011) Mplus User’s Guide. Muthen & Muthen, Los Angeles
National Center for Education Statistics (2004) Early Childhood Longitudinal Study (ECLS). Department of Education, Washington
O’Hara M, Swain A (1996) Rates and risk of postpartum depression: a meta-analysis. Int Rev Psychiatry 8(1):37–54
Paulson J (2010) Focusing on depression in expectant and new fathers: prenatal and postpartum depression not limited to mothers. Psychiatr Times 27(2):48–52
Post and Antenatal Depression Association (2012) The cost of perinatal depression in Australia. Deloitte Access Economics Pty Ltd, Australia
Ross C (2000) Neighborhood disadvantage and adult depression. J Heal Soc Behav 41:177–187
Small R, Brown S, Lumley J, Astbury J (1994) Missing voices: what women say and do about depression after childbirth. J Reprod Infant Psychol 12(2):89–103
Soloff C, Lawrence D, Johnstone R (2005) Sample design (LSAC Technical Paper, No. 1). Australian Institute of Family Studies, Commonwealth of Australia, Melbourne
Wang L, Wu T, Anderson J, Florence J (2011) Prevalence and risk factors of maternal depression during the first three years of child rearing. J Women's Health 20:711–718
Wilhelm K, Mitchell P, Slade T, Brownhill S, Andrews G (2003) Prevalence and correlates of DSM-IV major depression in an Australian National Survey. Journal of Affective Disorders 75:155–162
Acknowledgments
This paper used data from the Longitudinal Study of Australian Children. The study was conducted in partnership between the Department of Families, Housing, Community Services and Indigenous Affairs (FaHCSIA), the Australian Institute of Family Studies (AIFS), and the Australian Bureau of Statistics (ABS). This research was supported by PRC funding from the Victorian Government. The findings reported in this paper are those of the authors and should not be attributed to FaHCSIA, AIFS, or the ABS.
Conflict of interest
The authors declare that they have no conflict of interest.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Giallo, R., Cooklin, A. & Nicholson, J.M. Risk factors associated with trajectories of mothers’ depressive symptoms across the early parenting period: an Australian population-based longitudinal study. Arch Womens Ment Health 17, 115–125 (2014). https://doi.org/10.1007/s00737-014-0411-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00737-014-0411-1