Abstract
Purpose
The aim of the current study was to examine the incidence of poor sleep quality, medication use, and dysfunction and the association of self-stigma and perceived social constraints (i.e., ambivalence over emotional expression; AEE) on sleep among a sample of Chinese American breast cancer survivors.
Methods
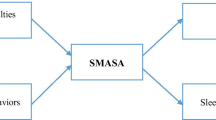
The data were based on self-report baseline data (n = 136) from an expressive writing intervention study for Chinese American breast cancer survivors (MTime since diagnosis = 27.17 months; SD = 19.31). Participants completed self-report questionnaires related to psychological and physical health and health behaviors. Using linear regression and path modeling, our hypotheses were tested using models where (1) self-stigma predicted sleep characteristics (i.e., quality, medication use, and dysfunction) with (2) AEE mediating the relationship between self-stigma and sleep.
Results
Participants frequently reported poor sleep quality (44.9%), use of sleep aids (37.5%), and difficulty staying awake during the day (37.5%). Greater self-stigma was related to greater AEE (b = .48, SE = .09, p < .05), which was related to worse sleep quality (b = − .19, SE = .08, p < .05), greater use of sleep aids (b = .25, SE = .11, p < .05), and greater difficulty staying awake during the day (b = .30, SE = .09, p < .05). Further, the indirect effect of self-stigma on sleep quality (ab = − .09, 95% CI − .19, − .03), use of sleep aids (ab = .12, 95% CI .03, .25), and difficulty staying awake during the day (ab = .15, 95% CI .06, .18) through AEE was significant.
Conclusion
The results of this study highlight significant sleep-related problems among Chinese American breast cancer survivors and the importance of considering cultural beliefs of cancer in counseling.
Implication for cancer survivors
Chinese American breast cancer survivors are at risk for sleep-related difficulties due, in part, to perceived self-stigma and emotional constraints. Greater education and community outreach to Chinese communities may help destigmatize breast cancer and encourage emotional expression around cancer-related topics.


Similar content being viewed by others
References
Palesh O, Aldridge-Gerry A, Ulusakarya A, Ortiz-Tudela E, Capuron L, Innominato PF (2013) Sleep disruption in breast cancer patients and survivors. J Natl Compr Cancer Netw 11(12):1523–1530
Koopman C, Nouriani B, Erickson V, Anupindi R, Butler LD, Bachmann MH, Sephton SE, Spiegel D (2002) Sleep disturbances in women with metastatic breast cancer. Breast J 8(6):362–370
Savard J, Ivers H, Villa J, Caplette-Gingras A, Morin CM (2011) Natural course of insomnia comorbid with cancer: an 18-month longitudinal study. J Clin Oncol 29(26):3580–3586
Phipps AI, Bhatti P, Neuhouser ML, Chen C, Crane TE, Kroenke CH, Ochs-Balcom H, Rissling M, Snively BM, Stefanick ML, Treggiari MM, Watson NF (2016) Pre-diagnostic sleep duration and sleep quality in relation to subsequent cancer survival. J Clin Sleep Med 12(4):495–503
Palesh O, Aldridge-Gerry A, Zeitzer JM, Koopman C, Neri E, Giese-Davis J, Jo B, Kraemer H, Nouriani B, Spiegel D (2014) Actigraphy-measured sleep disruption as a predictor of survival among women with advanced breast cancer. Sleep. 37(5):837–842
Clevenger L, Schrepf A, Degeest K, Bender D, Goodheart M, Ahmed A, Dahmoush L, Penedo F, Lucci J 3rd, Thaker PH, Mendez L, Sood AK, Slavich GM, Lutgendorf SK (2013) Sleep disturbance, distress, and quality of life in ovarian cancer patients during the first year after diagnosis. Cancer. 119(17):3234–3241
Gonzalez BD, Lu Q (2018) Sleep disturbance among Chinese breast cancer survivors living in the USA. Support Care Cancer 26(6):1695–1698
Krueger JM, Takahashi S, Kapas L et al (1995) Cytokines in sleep regulation. Adv Neuroimmunol 5(2):171–188
Opp MR, Krueger JM (2015) Sleep and immunity: a growing field with clinical impact. Brain Behav Immun 47:1–3
Savard J, Morin CM (2001) Insomnia in the context of cancer: a review of a neglected problem. J Clin Oncol 19(3):895–908
López G, Ruiz NG, Patten E (2017) Key facts about Asian Americans, a diverse and growing population. Fact Tank. 2017. http://www.pewresearch.org/fact-tank/2017/09/08/key-facts-about-asian-americans/. Accessed 9/15/18
Gomez SL, Von Behren J, McKinley M et al (2017) Breast cancer in Asian Americans in California, 1988–2013: increasing incidence trends and recent data on breast cancer subtypes. Breast Cancer Res Treat 164(1):139–147
National Comprehensive Cancer Network (2019) Survivorship (Version 1.2019). 2019; https://www.nccn.org/professionals/physician_gls/pdf/survivorship.pdf.
Kabat GC, Xue X, Kamensky V, Zaslavsky O, Stone KL, Johnson KC, Wassertheil-Smoller S, Shadyab AH, Luo J, Hale L, Qi L, Cauley JA, Brunner RL, Manson JE, Rohan TE (2018) The association of sleep duration and quality with all-cause and cause-specific mortality in the Women’s Health Initiative. Sleep Med 50:48–54
Yeung NCY, Ramirez J, Lu Q (2017) Perceived stress as a mediator between social constraints and sleep quality among Chinese American breast cancer survivors. Support Care Cancer 25(7):2249–2257
Otte JL, Carpenter JS (2009) Theories, models, and frameworks related to sleep-wake disturbances in the context of cancer. Cancer Nurs 32(2):90–106
Matthews EE, Hacker ED, Otte JL, Dean GE (2018) Agenda for sleep research in older adults with cancer: a conference report. Cancer Nurs 41(2):109–116
Harvey AG (2002) A cognitive model of insomnia. Behav Res Ther 40(8):869–893
Carlson LE, Campbell TS, Garland SN, Grossman P (2007) Associations among salivary cortisol, melatonin, catecholamines, sleep quality and stress in women with breast cancer and healthy controls. J Behav Med 30(1):45–58
Pachankis JE (2007) The psychological implications of concealing a stigma: a cognitive-affective-behavioral model. Psychol Bull 133(2):328–345
Lepore SJ, Revenson TA (2007) Social constraints on disclosure and adjustment to cancer. Soc Personal Psychol Compass 1(1):313–333
Else-Quest NM, Jackson TL (2014) Cancer stigma. In: Corrigan P (ed) The stigma of disease and disability: understanding causes and overcoming injustices. American Psychological Association, Washington, D.C., pp 165–181
King S (2004) Pink Ribbons Inc: breast cancer activism and the politics of philanthropy. Int J Qual Stud Educ 17(4):473–492
Sulik GA (2010) Pink ribbon blues: how breast cancer culture undermines women’s health. Oxford University Press
Karbani G, Lim JN, Hewison J, Atkin K, Horgan K, Lansdown M, Chu CE (2011) Culture, attitude and knowledge about breast cancer and preventive measures: a qualitative study of South Asian breast cancer patients in the UK. Asian Pac J Cancer Prev 12(6):1619–1626
Wong-Kim E, Sun A, Merighi JR, Chow EA (2005) Understanding quality-of-life issues in Chinese women with breast cncer: a qualitative investigation. Cancer Control 12(4_suppl):6–12
Tang PL, Mayer DK, Chou FH, Hsiao KY (2016) The experience of cancer stigma in Taiwan: a qualitative study of female cancer patients. Arch Psychiatr Nurs 30(2):204–209
Cho J, Choi EK, Kim SY et al (2013) Association between cancer stigma and depression among cancer survivors: a nationwide survey in Korea. Psychooncology. 22(10):2372–2378
Yang LH, Kleinman A, Link BG, Phelan JC, Lee S, Good B (2007) Culture and stigma: adding moral experience to stigma theory. Soc Sci Med 64(7):1524–1535
Wong MG (2014) The Chinese American family. In: Marcelo MS-O, Carola S-O, Desirée Q-H (eds) The new immigrant and the American family: interdisciplinary perspectives on the new immigration, vol 4. Taylor and Francis, London, pp 158–186
Gonzalez BD, Jacobsen PB (2012) Depression in lung cancer patients: the role of perceived stigma. Psychooncology. 21(3):239–246
K. W, C.C.Y. W, S. I, Q. L. The role of acculturation in the relationship between self-stigma and psychological distress among Chinese American breast cancer survivors. . Under review
Ong AD, Cerrada C, Lee RA, Williams DR (2017) Stigma consciousness, racial microaggressions, and sleep disturbance among Asian Americans. Asian Am J Psychol 8(1):72
Ruff RR, Ng J, Jean-Louis G, Elbel B, Chaix B, Duncan DT (2018) Neighborhood stigma and sleep: findings from a pilot study of low-income housing residents in New York City. Behav Med 44(1):48–53
Fekete EM, Williams SL, Skinta MD (2018) Internalised HIV-stigma, loneliness, depressive symptoms and sleep quality in people living with HIV. Psychol Health 33(3):398–415
King LA, Emmons RA (1990) Conflict over emotional expression: psychological and physical correlates. J Pers Soc Psychol 58(5):864–877
Chen SX, Cheung FM, Bond MH, Leung JP (2005) Decomposing the construct of ambivalence over emotional expression in a Chinese cultural context. Eur J Personal 19(3):185–204
Wang C, Wong CC, Lu Q (2018) The pain of ambivalence over emotional expression. Int J Behav Med. 25(2):216–222
Wu IHC, McNeill LH, Lu Q (2019) Ambivalence over emotional expression and physical functioning and limitations: mediating and moderating effects of PTSD symptoms and acculturation among Chinese breast cancer survivors. Supportive care in cancer : official journal of the Multinational Association of Supportive Care in Cancer 27(1):311–319
Tsai W, Lu Q (2018) Perceived social support mediates the longitudinal relations between ambivalence over emotional expression and quality of life among Chinese American breast cancer survivors. Int J Behav Med 25(3):368–373
Wong CCY, Warmoth K, Ivy S, Cheung B, Lu Q (2018) Relation of social constraints on disclosure to adjustment among Chinese American cancer survivors: a multiprocesses approach. Psychooncology. 27(3):977–982
Zoccola PM, Dickerson SS, Lam S (2009) Rumination predicts longer sleep onset latency after an acute psychosocial stressor. Psychosom Med 71(7):771–775
Guastella AJ, Moulds ML (2007) The impact of rumination on sleep quality following a stressful life event. Pers Individ Dif 42(6):1151–1162
Lu Q, Gallagher MW, Loh A, Young L (2018) Expressive writing intervention improves quality of life among Chinese-American breast cancer survivors: a randomized controlled trial. Ann Behav Med 52(11):952–962
Brislin RW (1970) Back-translation for cross-cultural research. J Cross-Cult Psychol 1(3):185–216
Mak WW, Cheung RY (2010) Self-stigma among concealable minorities in Hong Kong: conceptualization and unified measurement. Am J Orthop 80(2):267–281
Buysse DJ, Reynolds CF 3rd, Monk TH, Berman SR, Kupfer DJ (1989) The Pittsburgh Sleep Quality Index: a new instrument for psychiatric practice and research. Psychiatry Res 28(2):193–213
Hayes AF (2017) Introduction to mediation, moderation, and conditional process analysis: a regression-based approach, 2nd edn. The Guilford Press, New York, NY
IBM SPSS Statistics for Windows [computer program]. Version 24. Armonk, NY: IBM Corp; Released 2016
Wu AH, Wang R, Koh W-P, Stanczyk FZ, Lee H-P, Yu MC (2008) Sleep duration, melatonin and breast cancer among Chinese women in Singapore. Carcinogenesis. 29(6):1244–1248
Trudel-Fitzgerald C, Zhou ES, Poole EM, Zhang X, Michels KB, Eliassen AH, Chen WY, Holmes MD, Tworoger SS, Schernhammer ES (2017) Sleep and survival among women with breast cancer: 30 years of follow-up within the Nurses’ Health Study. Br J Cancer 116(9):1239–1246
Bertisch SM, Herzig SJ, Winkelman JW, Buettner C (2014) National use of prescription medications for insomnia: NHANES 1999-2010. Sleep. 37(2):343–349
Clarke TC, Black LI, Stussman BJ, Barnes PM, Nahin RL (2015) Trends in the use of complementary health approaches among adults: United States, 2002-2012. National health statistics reports (79):1–16
Petrov ME, Howard VJ, Kleindorfer D, Grandner MA, Molano JR, Howard G (2014) Over-the-counter and prescription sleep medication and incident stroke: the REasons for Geographic and Racial Differences in Stroke study. Journal of stroke and cerebrovascular diseases : the official journal of National Stroke Association 23(8):2110–2116
Moore TA, Berger AM, Dizona P (2011) Sleep aid use during and following breast cancer adjuvant chemotherapy. Psychooncology. 20(3):321–325
Savard J, Simard S, Blanchet J, Ivers H, Morin CM (2001) Prevalence, clinical characteristics, and risk factors for insomnia in the context of breast cancer. Sleep. 24(5):583–590
Bardwell WA, Profant J, Casden DR, Dimsdale JE, Ancoli-Israel S, Natarajan L, Rock CL, Pierce JP, Women's Healthy Eating & Living (WHEL) Study Group (2008) The relative importance of specific risk factors for insomnia in women treated for early-stage breast cancer. Psychooncology. 17(1):9–18
Fiorentino L, Ancoli-Israel S (2006) Insomnia and its treatment in women with breast cancer. Sleep Med Rev 10(6):419–429
Birtel MD, Wood L, Kempa NJ (2017) Stigma and social support in substance abuse: implications for mental health and well-being. Psychiatry Res 252:1–8
Kapella MC, Berger BE, Vern BA, Vispute S, Prasad B, Carley DW (2015) Health-related stigma as a determinant of functioning in young adults with narcolepsy. PLoS One 10(4):e0122478
Tam Ashing K, Padilla G, Tejero J, Kagawa-Singer M (2003) Understanding the breast cancer experience of Asian American women. Psycho-Oncology. 12(1):38–58
Lam WWT, Fielding R (2003) The evolving experience of illness for Chinese women with breast cancer: a qualitative study. Psycho-Oncology. 12(2):127–140
Lui C-W, Ip D, Chui WH (2009) Ethnic experience of cancer: a qualitative study of Chinese–Australians in Brisbane, Queensland. Soc Work Health Care 48(1):14–37
Kwok C, Sullivan G (2006) Chinese-Australian women’s beliefs about cancer: implications for health promotion. Cancer Nurs 29(5):E14–E21
Tsai W, Wu IHC, Lu Q (2019) Acculturation and quality of life among Chinese American breast cancer survivors: the mediating role of self-stigma, ambivalence over emotion expression, and intrusive thoughts. Psychooncology. 28(5):1063–1070
van Dalfsen JH, Markus CR (2018) The influence of sleep on human hypothalamic–pituitary–adrenal (HPA) axis reactivity: a systematic review. Sleep Med Rev 39:187–194
Patel NP, Grandner MA, Xie D, Branas CC, Gooneratne N (2010) “Sleep disparity” in the population: poor sleep quality is strongly associated with poverty and ethnicity. BMC Public Health 10:475
Lovato N, Lack L (2019) Insomnia and mortality: a meta-analysis. Sleep Med Rev 43:71–83
Yang X, Mak WWS (2017) The differential moderating roles of self-compassion and mindfulness in self-stigma and well-being among people living with mental illness or HIV. Mindfulness. 8(3):595–602
Chan KKS, Lee CWL, Mak WWS (2018) Mindfulness model of stigma resistance among individuals with psychiatric disorders. Mindfulness. 9(5):1433–1442
Haller H, Winkler MM, Klose P, Dobos G, Kummel S, Cramer H (2017) Mindfulness-based interventions for women with breast cancer: an updated systematic review and meta-analysis. Acta Oncol 56(12):1665–1676
Funding
The study was funded by American Cancer Society MRSGT-10-011-01-CPPB (PI: Qian Lu). Trial registration: ClinicalTrials.gov Identifier: NCT02946619. This manuscript was supported in part by a cancer prevention fellowship for Ivan H.C. Wu, Ph.D., by the Cancer Prevention and Research Institute of Texas grant award, RP170259, Shine Chang, PhD, Principal Investigator and by the MD Anderson Cancer Center Support Grant, CA016672, funded by the National Cancer Institute.
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Informed consent
Informed consent was obtained from all individual participants included in the study.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Wu, I.H.C., Tsai, W., McNeill, L.H. et al. The associations of self-stigma, social constraints, and sleep among Chinese American breast cancer survivors. Support Care Cancer 28, 3935–3944 (2020). https://doi.org/10.1007/s00520-019-05233-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00520-019-05233-x