Abstract
Purpose
Financial toxicity is a multidimensional side effect of cancer treatment. Yet, most relevant research has focused on individual-level determinants of financial toxicity and characterized only patient perspectives. This study examined the multilevel determinants of financial toxicity from the perspectives of Latina breast cancer survivors and healthcare professionals.
Methods
We analyzed qualitative data from focus groups with 19 Latina breast cancer survivors and interviews with 10 healthcare professionals recruited through community partners and venues in Chicago.
Results
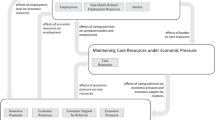
At the individual-level, the lack of knowledge and prioritization regarding financial aspects of care (e.g., costs of treatment, insurance coverage) was identified as important determinants of financial toxicity. However, healthcare professionals emphasized the need for early financial planning, while survivors prioritized survival over financial concerns immediately after diagnosis. At the interpersonal-level, social networks were identified as important platforms for disseminating information on financial resources. At the community-level, community norms and dynamics were identified as important barriers to seeking financial assistance. Access to culturally astute community-based organizations was considered one potential solution to eliminate these barriers. At the organizational/healthcare policy-level, financial assistance programs’ restrictive eligibility criteria, lack of coverage post-treatment, limited availability, and instability were identified as major determinants of financial toxicity.
Conclusion
Our findings suggest that multilevel interventions at the individual-, interpersonal-, community-, and organizational/healthcare policy-levels are needed to adequately address financial toxicity among Latina and other survivors from disadvantaged communities.
Similar content being viewed by others
References
Ashing K, Rosales M, Lai L, Hurria A (2014) Occurrence of comorbidities among African-American and Latina breast cancer survivors. J Cancer Surviv 8:312–318. https://doi.org/10.1007/s11764-014-0342-x
Fu OS, Crew KD, Jacobson JS et al (2009) Ethnicity and persistent symptom burden in breast cancer survivors. J Cancer Surviv 3:241–250. https://doi.org/10.1007/s11764-009-0100-7
Luckett T, Goldstein D, Butow PN et al (2011) Psychological morbidity and quality of life of ethnic minority patients with cancer: a systematic review and meta-analysis. Lancet Oncol 12:1240–1248. https://doi.org/10.1016/S1470-2045(11)70212-1
Yanez B, Thompson EH, Stanton AL (2011) Quality of life among Latina breast cancer patients: a systematic review of the literature. J Cancer Surviv 5:191–207. https://doi.org/10.1007/s11764-011-0171-0
Yanez B, McGinty HL, Buitrago D et al (2016) Cancer outcomes in Hispanics/Latinos in the United States: an integrative review and conceptual model of determinants of health. J Lat Psychol 4:114–129. https://doi.org/10.1037/lat0000055
Advani PS, Ying J, Theriault R et al (2014) Ethnic disparities in adherence to breast cancer survivorship surveillance care. Cancer 120:894–900. https://doi.org/10.1002/cncr.28490
Breslau ES, Jeffery DD, Davis WW et al (2010) Cancer screening practices among racially and ethnically diverse breast cancer survivors: results from the 2001 and 2003 California Health Interview Survey. J Cancer Surviv 4:1–14. https://doi.org/10.1007/s11764-009-0102-5
Fedewa SA, Ward EM, Stewart AK, Edge SB (2010) Delays in adjuvant chemotherapy treatment among patients with breast cancer are more likely in African American and Hispanic populations: a national cohort study 2004-2006. J Clin Oncol 28:4135–4141. https://doi.org/10.1200/JCO.2009.27.2427
Palmer NRA, Kent EE, Forsythe LP et al (2014) Racial and ethnic disparities in patient-provider communication, quality-of-care ratings, and patient activation among long-term cancer survivors. J Clin Oncol 32:4087–4094. https://doi.org/10.1200/JCO.2014.55.5060
White A, Pollack LA, Smith JL et al (2013) Racial and ethnic differences in health status and health behavior among breast cancer survivors—Behavioral Risk Factor Surveillance System, 2009. J Cancer Surviv 7:93–103. https://doi.org/10.1007/s11764-012-0248-4
Kale HP, Carroll NV (2016) Self-reported financial burden of cancer care and its effect on physical and mental health-related quality of life among US cancer survivors. Cancer 122:283–289. https://doi.org/10.1002/cncr.29808
Koskinen J-P, Färkkilä N, Sintonen H et al (2019) The association of financial difficulties and out-of-pocket payments with health-related quality of life among breast, prostate and colorectal cancer patients. Acta Oncol 0:1–7. https://doi.org/10.1080/0284186X.2019.1592218
Lentz R, Benson AB, Kircher S Financial toxicity in cancer care: prevalence, causes, consequences, and reduction strategies. J Surg Oncol 0. https://doi.org/10.1002/jso.25374
Pearce A, Tomalin B, Kaambwa B et al (2019) Financial toxicity is more than costs of care: the relationship between employment and financial toxicity in long-term cancer survivors. J Cancer Surviv 13:10–20. https://doi.org/10.1007/s11764-018-0723-7
Timmons A, Gooberman-Hill R, Sharp L (2013) The multidimensional nature of the financial and economic burden of a cancer diagnosis on patients and their families: qualitative findings from a country with a mixed public–private healthcare system. Support Care Cancer 21:107–117. https://doi.org/10.1007/s00520-012-1498-4
Zafar SY, Peppercorn JM, Schrag D et al (2013) The financial toxicity of cancer treatment: a pilot study assessing out-of-pocket expenses and the insured cancer patient’s experience. Oncologist 18:381–390. https://doi.org/10.1634/theoncologist.2012-0279
Blinder VS, Patil S, Thind A et al (2012) Return to work in low-income Latina and non-Latina white breast cancer survivors: a 3-year longitudinal study. Cancer 118:1664–1674. https://doi.org/10.1002/cncr.26478
Jagsi R, Pottow JAE, Griffith KA et al (2014) Long-term financial burden of breast cancer: experiences of a diverse cohort of survivors identified through population-based registries. J Clin Oncol 32:1269–1276. https://doi.org/10.1200/JCO.2013.53.0956
Jagsi R, Ward KC, Abrahamse PH et al (2018) Unmet need for clinician engagement regarding financial toxicity after diagnosis of breast cancer. Cancer 124:3668–3676. https://doi.org/10.1002/cncr.31532
Lee M, Salloum RG (2016) Racial and ethnic disparities in cost-related medication non-adherence among cancer survivors. J Cancer Surviv 10:534–544. https://doi.org/10.1007/s11764-015-0499-y
Ashing-Giwa KT, Padilla GV, Bohorquez DE et al (2006) Understanding the breast cancer experience of Latina women. J Psychosoc Oncol 24:19–52. https://doi.org/10.1300/J077v24n03_02
Buki LP, Garcés DM, Hinestrosa MC et al (2008) Latina breast cancer survivors’ lived experiences: diagnosis, treatment, and beyond. Cultur Divers Ethnic Minor Psychol 14:163–167. https://doi.org/10.1037/1099-9809.14.2.163
Azzani M, Roslani AC, Su TT (2015) The perceived cancer-related financial hardship among patients and their families: a systematic review. Support Care Cancer 23:889–898. https://doi.org/10.1007/s00520-014-2474-y
Ashing‐Giwa KT, Padilla G, Tejero J et al (2004) Understanding the breast cancer experience of women: a qualitative study of African American, Asian American, Latina and Caucasian cancer survivors. Psychooncology 13:408–428. https://doi.org/10.1002/pon.750
Zapka JG, Taplin SH, Solberg LI, Manos MM (2003) A framework for improving the quality of cancer care: the case of breast and cervical cancer screening. Cancer Epidemiol Biomarkers Prev 12:4–13
Molina Y, Watson KS, San Miguel LG, et al. (2019) Integrating multiple community-based approaches in intervention development. Health Education Research. Health Educ Res
Nevin PE, Blas M, Bayer A et al (2019) Positive cancer care in Peru: patient and provider perspectives. Health Care Women Int 0:1–14. https://doi.org/10.1080/07399332.2019.1608206
Bernard HR, Wutich A, Ryan GW (2016) Analyzing qualitative data: systematic approaches. SAGE Publications, Content Analysis 11: 243–268
Hsieh H-F, Shannon SE (2005) Three approaches to qualitative content analysis. Qual Health Res 15:1277–1288. https://doi.org/10.1177/1049732305276687
Lopez‐Class M, Gomez‐Duarte J, Graves K, Ashing‐Giwa K (2012) A contextual approach to understanding breast cancer survivorship among Latinas. Psychooncology 21:115–124. https://doi.org/10.1002/pon.1998
Warnecke RB, Oh A, Breen N et al (2008) Approaching health disparities from a population perspective: The National Institutes of Health Centers for Population Health and Health Disparities. Am J Public Health 98:1608–1615. https://doi.org/10.2105/AJPH.2006.102525
Blackman DJ, Masi CM (2006) Racial and ethnic disparities in breast cancer mortality: are we doing enough to address the root causes? J Clin Oncol 24:2170–2178. https://doi.org/10.1200/JCO.2005.05.4734
Creswell JW, Miller DL (2000) Determining validity in qualitative inquiry. Theory Pract 39:124–130. https://doi.org/10.1207/s15430421tip3903_2
Morse JM, Barrett M, Mayan M et al (2002) Verification strategies for establishing reliability and validity in qualitative research. Int J Qual Methods 1:13–22. https://doi.org/10.1177/160940690200100202
Suri H (2011) Purposeful sampling in qualitative research synthesis. Qual Res J 11:63–75. https://doi.org/10.3316/QRJ1102063
Sandelowski M (2001) Real qualitative researchers do not count: the use of numbers in qualitative research. Res Nurs Health 24:230–240. https://doi.org/10.1002/nur.1025
Sandelowski M, Barroso J (2003) Classifying the findings in qualitative studies. Qual Health Res 13:905–923. https://doi.org/10.1177/1049732303253488
Carrera PM, Kantarjian HM, Blinder VS (2018) The financial burden and distress of patients with cancer: understanding and stepping-up action on the financial toxicity of cancer treatment. CA Cancer J Clin 68:153–165. https://doi.org/10.3322/caac.21443
Yousuf Zafar S (2016) Financial toxicity of cancer care: it’s time to intervene. J Natl Cancer Inst 108. https://doi.org/10.1093/jnci/djv370
Molina Y, Thompson B, Espinoza N, Ceballos R (2013) Breast cancer interventions serving US-Based Latinas: current approaches and directions. Womens Health (Lond) 9:335–350. https://doi.org/10.2217/WHE.13.30
Galván N, Buki LP, Garcés DM (2009) Suddenly, a carriage appears: social support needs of Latina breast cancer survivors. J Psychosoc Oncol 27:361–382. https://doi.org/10.1080/07347330902979283
Moy B, Polite BN, Halpern MT et al (2011) American Society of Clinical Oncology Policy Statement: opportunities in the patient protection and affordable care act to reduce cancer care disparities. J Clin Oncol 29:3816–3824. https://doi.org/10.1200/JCO.2011.35.8903
Kent EE, Forsythe LP, Yabroff KR et al (2013) Are survivors who report cancer-related financial problems more likely to forgo or delay medical care? Cancer 119:3710–3717. https://doi.org/10.1002/cncr.28262
Pisu M, Kenzik KM, Oster RA et al (2015) Economic hardship of minority and non-minority cancer survivors 1 year after diagnosis: another long-term effect of cancer? Cancer 121:1257–1264. https://doi.org/10.1002/cncr.29206
Licqurish S, Phillipson L, Chiang P et al (2017) Cancer beliefs in ethnic minority populations: a review and meta-synthesis of qualitative studies. Eur J Cancer Care (Engl) 26:e12556. https://doi.org/10.1111/ecc.12556
Acknowledgments
The authors would like to thank study participants for their time, effort, and perspectives. They would also like to thank Mr. Hunter T. Norris for editorial support.
Funding
This work was supported by the University of Illinois at Chicago’s Institute for Race Research and Public Policy under a 2018–2019 Policy & Social Engagement Fellowship as well as by the National Cancer Institute under grant number K01CA154938. YM was also supported by the University of Illinois Cancer Center and Center for Research on Women and Gender.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflicts of interest.
Disclaimer
The opinions or assertions contained herein are the private ones of the authors and are not considered as official or reflecting the views of the National Institutes of Health.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Chebli, P., Lemus, J., Avila, C. et al. Multilevel determinants of financial toxicity in breast cancer care: perspectives of healthcare professionals and Latina survivors. Support Care Cancer 28, 3179–3188 (2020). https://doi.org/10.1007/s00520-019-05119-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00520-019-05119-y