Abstract
Purpose
Breast cancer is the leading cause of cancer mortality in women worldwide. With medical advances, metastatic breast cancer (MBC) patients often live for years with many symptoms that interfere with activities. However, there is a paucity of efficacious interventions to address symptom-related suffering and functional interference. Thus, this study examined the feasibility and preliminary efficacy of telephone-based acceptance and commitment therapy (ACT) for symptom interference with functioning in MBC patients.
Methods
Symptomatic MBC patients (N = 47) were randomly assigned to six telephone sessions of ACT or six telephone sessions of education/support. Patients completed measures of symptom interference and measures assessing the severity of pain, fatigue, sleep disturbance, depressive symptoms, and anxiety.
Results
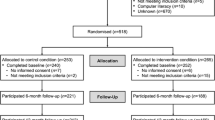
The eligibility screening rate (64%) and high retention (83% at 8 weeks post-baseline) demonstrated feasibility. When examining within-group change, ACT participants showed decreases in symptom interference (i.e., fatigue interference and sleep-related impairment; Cohen’s d range = − 0.23 to − 0.31) at 8 and 12 weeks post-baseline, whereas education/support participants showed minimal change in these outcomes (d range = − 0.03 to 0.07). Additionally, at 12 weeks post-baseline, ACT participants showed moderate decreases in fatigue and sleep disturbance (both ds = − 0.43), whereas education/support participants showed small decreases in these outcomes (ds = − 0.24 and − 0.18 for fatigue and sleep disturbance, respectively). Both the ACT and education/support groups showed reductions in depressive symptoms (ds = − 0.27 and − 0.28) at 12 weeks post-baseline. Group differences in all outcomes were not statistically significant.
Conclusions
ACT shows feasibility and promise in improving fatigue and sleep-related outcomes in MBC patients and warrants further investigation.


Similar content being viewed by others
References
Ferlay J, Soerjomataram I, Dikshit R, Eser S, Mathers C, Rebelo M, Parkin DM, Forman D, Bray F (2015) Cancer incidence and mortality worldwide: sources, methods and major patterns in GLOBOCAN 2012. Int J Cancer 136(5):E359–E386. https://doi.org/10.1002/ijc.29210
Aranda S, Schofield P, Weih L, Yates P, Milne D, Faulkner R, Voudouris N (2005) Mapping the quality of life and unmet needs of urban women with metastatic breast cancer. Eur J Cancer Care (Engl) 14(3):211–222. https://doi.org/10.1111/j.1365-2354.2005.00541.x
Given BA, Given CW, Sikorskii A, Hadar N (2007) Symptom clusters and physical function for patients receiving chemotherapy. Semin Oncol Nurs 23(2):121–126. https://doi.org/10.1016/j.soncn.2007.01.005
Mosher CE, Duhamel KN (2012) An examination of distress, sleep, and fatigue in metastatic breast cancer patients. Psychooncology 21(1):100–107. PMCID: PMC3756885. https://doi.org/10.1002/pon.1873
Cleeland CS, Mayer M, Dreyer NA, Yim YM, Yu E, Su Z, Mun Y, Sloan JA, Kaufman PA (2014) Impact of symptom burden on work-related abilities in patients with locally recurrent or metastatic breast cancer: results from a substudy of the VIRGO observational cohort study. Breast 23(6):763–769. https://doi.org/10.1016/j.breast.2014.08.004
Low CA, Stanton AL (2015) Activity disruption and depressive symptoms in women living with metastatic breast cancer. Health Psychol 34(1):89–92. https://doi.org/10.1037/hea0000052
Willis K, Lewis S, Ng F, Wilson L (2015) The experience of living with metastatic breast cancer—a review of the literature. Health Care Women Int 36(5):514–542. https://doi.org/10.1080/07399332.2014.896364
Lam WWT, Tsang J, Yeo W, Suen J, Ho WM, Yau TK, Soong I, Wong KY, Kwong A, Suen D, Sze WK, Ng AWY, Girgis A, Fielding R (2013) The evolution of supportive care needs trajectories in women with advanced breast cancer during the 12 months following diagnosis. Support Care Cancer 22:635–644
Grabsch B, Clarke DM, Love A, McKenzie DP, Snyder RD, Bloch S, Smith G, Kissane DW (2006) Psychological morbidity and quality of life in women with advanced breast cancer: a cross-sectional survey. Palliat Support Care 4(1):47–56
Kissane DW, Grabsch B, Love A, Clarke DM, Bloch S, Smith GC (2004) Psychiatric disorder in women with early stage and advanced breast cancer: a comparative analysis. Aust N Z J Psychiatry 38(5):320–326. https://doi.org/10.1080/j.1440-1614.2004.01358.x
Koopman C, Nouriani B, Erickson V, Anupindi R, Butler LD, Bachmann MH, Sephton SE, Spiegel D (2002) Sleep disturbances in women with metastatic breast cancer. Breast J 8(6):362–370. https://doi.org/10.1046/j.1524-4741.2002.08606.x
Palesh OG, Collie K, Batiuchok D, Tilston J, Koopman C, Perlis ML, Butler LD, Carlson R, Spiegel D (2007) A longitudinal study of depression, pain, and stress as predictors of sleep disturbance among women with metastatic breast cancer. Biol Psychol 75(1):37–44. https://doi.org/10.1016/j.biopsycho.2006.11.002
McGuire DB, Sheidler VR (1992) Pain. In: Groenwald SL, Frogge MH, Goodman M, Yarbro CH (eds) Manifestations of cancer and cancer treatment. Jones and Bartlett Publishers, Boston, pp 441–985
Mustafa M, Carson-Stevens S, Gillespie D, Edwards AGK (2013) Psychological interventions for women with metastatic breast cancer (review). Cochrane Database Syst Rev 6:CD004253
Beatty L, Kemp E, Butow P, Girgis A, Schofield P, Turner J, Hulbert-Williams NJ, Levesque JV, Koczwara B (2017) A systematic review of psychotherapeutic interventions for women with metastatic breast cancer: context matters. Psychooncology. https://doi.org/10.1002/pon.4445
Hayes SC, Strosahl KD, Wilson KG (2012) Acceptance and commitment therapy, second edition: the process and practice of mindful change. Guilford Press, New York
Edmonds CVI, Lockwood GA, Cunningham AJ (1999) Psychological response to long term group therapy: a randomized trial with metastatic breast cancer patients. Psychooncology 8(1):74–91. https://doi.org/10.1002/(SICI)1099-1611(199901/02)8:1<74::AID-PON339>3.0.CO;2-K
Edelman S, Bell DR, Kidman AD (1999) A group cognitive behaviour therapy programme with metastatic breast cancer patients. Psychooncology 8(4):295–305. https://doi.org/10.1002/(SICI)1099-1611(199907/08)8:4<295::AID-PON386>3.0.CO;2-Y
Feros DL, Lane L, Ciarrochi J, Blackledge JT (2013) Acceptance and commitment therapy (ACT) for improving the lives of cancer patients: a preliminary study. Psychooncology 22(2):459–464. https://doi.org/10.1002/pon.2083
Hayes SC, Luoma JB, Bond FW, Masuda A, Lillis J (2006) Acceptance and commitment therapy: model, processes and outcomes. Behav Res Ther 44(1):1–25. https://doi.org/10.1016/j.brat.2005.06.006
Ciarrochi J, Fisher D, Lane L (2011) The link between value motives, value success, and well-being among people diagnosed with cancer. Psychooncology 20(11):1184–1192. https://doi.org/10.1002/pon.1832
Hulbert-Williams NJ, Storey L (2016) Psychological flexibility correlates with patient-reported outcomes independent of clinical or sociodemographic characteristics. Support Care Cancer 24(6):2513–2521. https://doi.org/10.1007/s00520-015-3050-9
Hann KEJ, McCracken LM (2014) A systematic review of randomized controlled trials of Acceptance and Commitment Therapy for adults with chronic pain: outcome domains, design quality, and efficacy. J Contextual Behav Sci 3(4):217–227. https://doi.org/10.1016/j.jcbs.2014.10.001
Gregg JA, Callaghan GM, Hayes SC, Glenn-Lawson JL (2007) Improving diabetes self-management through acceptance, mindfulness, and values: a randomized controlled trial. J Consult Clin Psychol 75(2):336–343. https://doi.org/10.1037/0022-006X.75.2.336
Hulbert-Williams NJ, Storey L, Wilson KG (2015) Psychological interventions for patients with cancer: psychological flexibility and the potential utility of Acceptance and Commitment Therapy. Eur J Cancer Care (Engl) 24(1):15–27. https://doi.org/10.1111/ecc.12223
Rost AD, Wilson K, Buchanan E, Hildebrandt MJ, Mutch D (2012) Improving psychological adjustment among late-stage ovarian cancer patients: examining the role of avoidance in treatment. Cogn Behav Pract 19(4):508–517. https://doi.org/10.1016/j.cbpra.2012.01.003
Hayes SC, Smith S (2005) Get out of your mind and into your life: the new acceptance and commitment therapy. New Harbinger, Oakland
Cella D, Riley W, Stone A, Rothrock N, Reeve B, Yount S, Amtmann D, Bode R, Buysse D, Choi S, Cook K, Devellis R, DeWalt D, Fries JF, Gershon R, Hahn EA, Lai JS, Pilkonis P, Revicki D, Rose M, Weinfurt K, Hays R (2010) The Patient-Reported Outcomes Measurement Information System (PROMIS) developed and tested its first wave of adult self-reported health outcome item banks: 2005–2008. J Clin Epidemiol 63(11):1179–1194. https://doi.org/10.1016/j.jclinepi.2010.04.011
Cella D, Yount S, Rothrock N, Gershon R, Cook K, Reeve B, Ader D, Fries JF, Bruce B, Rose M (2007) The Patient-Reported Outcomes Measurement Information System (PROMIS): progress of an NIH roadmap cooperative group during its first two years. Med Care 45(Suppl 1):S3–S11. https://doi.org/10.1097/01.mlr.0000258615.42478.55
Callahan CM, Unverzagt FW, Hui SL, Perkins AJ, Hendrie HC (2002) Six-item screener to identify cognitive impairment among potential subjects for clinical research. Med Care 40(9):771–781. https://doi.org/10.1097/00005650-200209000-00007
Bauer J, Capra S, Ferguson M (2002) Use of the scored Patient-Generated Subjective Global Assessment (PG-SGA) as a nutrition assessment tool in patients with cancer. Eur J Clin Nutr 56(8):779–785. https://doi.org/10.1038/sj.ejcn.1601412
Dajczman E, Kasymjanova G, Kreisman H, Swinton N, Pepe C, Small D (2008) Should patient-rated performance status affect treatment decisions in advanced lung cancer? J Thorac Oncol 3(10):1133–1136. https://doi.org/10.1097/JTO.0b013e318186a272
Cardoso F, Harbeck N, Fallowfield L, Kyriakides S, Senkus E (2012) Locally recurrent or metastatic breast cancer: ESMO Clinical Practice Guidelines for diagnosis, treatment and follow-up. Ann Oncol 23:vii11–vii19
Cleeland CS, Mendoza TR, Wang XS, Chou C, Harle MT, Morrissey M, Engstrom MC (2000) Assessing symptom distress in cancer patients: the M.D. Anderson Symptom Inventory. Cancer 89(7):1634–1646. https://doi.org/10.1002/1097-0142(20001001)89:7<1634::AID-CNCR29>3.0.CO;2-V
Amtmann D, Cook KF, Jensen MP, Chen W-H, Choi S, Revicki D, Cella D, Rothrock N, Keefe F, Callahan L, Lai J-S (2010) Development of a PROMIS item bank to measure pain interference. Pain 150(1):173–182. https://doi.org/10.1016/j.pain.2010.04.025
Hann DM, Denniston MM, Baker F (2000) Measurement of fatigue in cancer patients: further validation of the fatigue symptom inventory. Qual Life Res 9(7):847–854. https://doi.org/10.1023/A:1008900413113
Yu L, Buysse DJ, Germain A, Moul DE, Stover A, Dodds NE, Johnston KL, Pilkonis PA (2012) Development of short forms from the PROMIS sleep disturbance and sleep-related impairment item banks. Behav Sleep Med 10(1):6–24. https://doi.org/10.1080/15402002.2012.636266
Pilkonis PA, Choi SW, Reise SP, Stover AM, Riley WT, Cella D (2011) Item banks for measuring emotional distress from the patient-reported outcomes measurement information system (PROMIS(R)): depression, anxiety, and anger. Assessment 18(3):263–283. https://doi.org/10.1177/1073191111411667
Porter LS, Keefe FJ, Baucom DH, Hurwitz H, Moser B, Patterson E, Kim HJ (2009) Partner-assisted emotional disclosure for patients with gastrointestinal cancer: results from a randomized controlled trial. Cancer 115(S18):4326–4338. https://doi.org/10.1002/cncr.24578
Mosher CE, Winger JG, Hanna N, Jalal SI, Einhorn LH, Birdas TJ, Ceppa DP, Kesler KA, Schmitt J, Kashy DA, Champion VL (2016) Randomized pilot trial of a telephone symptom management intervention for symptomatic lung cancer patients and their family caregivers. J Pain Symptom Manag 52:469–482 PMCID: PMC5075493
Bohlmeijer ET, Fledderus M, Rokx TAJJ, Pieterse ME (2011) Efficacy of an early intervention based on acceptance and commitment therapy for adults with depressive symptomatology: evaluation in a randomized controlled trial. Behav Res Ther 49(1):62–67. https://doi.org/10.1016/j.brat.2010.10.003
Fledderus M, Bohlmeijer ET, Pieterse ME, Schreurs KM (2012) Acceptance and commitment therapy as guided self-help for psychological distress and positive mental health: a randomized controlled trial. Psychol Med 42(03):485–495. https://doi.org/10.1017/S0033291711001206
Johns SA, Brown LF, Beck-Coon K, Monahan PO, Tong Y, Kroenke K (2015) Randomized controlled pilot study of mindfulness-based stress reduction for persistently fatigued cancer survivors. Psychooncology 24(8):885–893. https://doi.org/10.1002/pon.3648
Johns SA, Brown LF, Beck-Coon K, Talib TL, Monahan PO, Giesler RB, Tong Y, Wilhelm L, Carpenter JS, Von AD, Wagner CD, de Groot M, Schmidt K, Monceski D, Danh M, Alyea JM, Miller KD, Kroenke K (2016) Randomized controlled pilot trial of mindfulness-based stress reduction compared to psychoeducational support for persistently fatigued breast and colorectal cancer survivors. Support Care Cancer 24(10):4085–4096. https://doi.org/10.1007/s00520-016-3220-4
Faller H, Schuler M, Richard M, Heckl U, Weis J, Küffner R (2013) Effects of psycho-oncologic interventions on emotional distress and quality of life in adult patients with cancer: systematic review and meta-analysis. J Clin Oncol 31(6):782–793. https://doi.org/10.1200/JCO.2011.40.8922
Acknowledgements
The authors thank Susan Daily, B.S., RT (T), Kelly Chinh, B.S., Lauren Hall, LCSW, and Danielle B. Tometich, M.S., for their assistance with this study and the study participants for their time and effort. The content is solely the responsibility of the authors and does not necessarily represent the official views of the National Cancer Institute or Walther Cancer Foundation.
Funding
This study was supported by a grant from the Walther Cancer Foundation. Catherine Mosher was supported by the National Cancer Institute (K07CA168883 and K05CA175048). Shelley Johns was supported by the National Cancer Institute (K05CA175048) and Walther Cancer Foundation (0175.01). Victoria Champion was supported by the National Cancer Institute (K05CA175048).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Informed consent
Informed consent was obtained from all individual participants included in the study.
Rights and permissions
About this article
Cite this article
Mosher, C.E., Secinti, E., Li, R. et al. Acceptance and commitment therapy for symptom interference in metastatic breast cancer patients: a pilot randomized trial. Support Care Cancer 26, 1993–2004 (2018). https://doi.org/10.1007/s00520-018-4045-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00520-018-4045-0