Abstract
Background
We compared two types of visual field index including mean deviation (MD) and the visual field index (VFI) for assessing the relationship between quality of life (QOL) and the loss of visual field in open-angle glaucoma patients.
Methods
We examined 336 eyes of 168 consecutive glaucoma patients. All participants completed the Japanese version of the 25-item National Eye Institute Visual Function Questionnaire (NEI VFQ-25). Visual field testing using the Humphrey Field Analyzer (HFA) was performed to obtain both MD and VFI in the bilateral eyes of each patient. We defined eyes of better MD or VFI as the better eye and the fellow eyes as the worse eye. Visual field data and scores of NEI VFQ-25 were compared between patients with normal tension glaucoma (NTG) and patients with primary open-angle glaucoma (POAG). A single linear regression analysis was applied to assess the significance of the relationship between QOL and visual field, and to compare the strength of correlations between MD and the VFI. An unpaired t test was used for the comparison the data between NTG and POAG.
Results
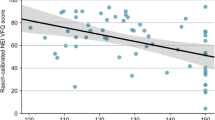
A significant relationship was observed between QOL and visual field in nine subscales and the composite in both the better eye and the worse eye. The relationship was stronger in the better eye than in the worse eye. The correlation coefficients of the VFI were slightly higher than those of MD overall. The highest correlation coefficients were demonstrated in ten subscales and the composite in the better eye of the VFI. Only the score for general vision was significantly higher in NTG patients than POAG patients.
Conclusions
A significant relationship was found between QOL and both the VFI and MD, but the VFI had a marginally better correlation than that of MD. While QOL was better related with visual field loss in the better eye than in the worse eye, the difference was not large. Not much of a difference was found in the status of QOL between NTG patients and POAG patients.





Similar content being viewed by others
References
Mangione CM, Berry S, Spritzer K, Janz NK, Klein R, Owsley C, Lee PP (1998) Identifying the content area for the 51-item National Eye Institute Visual Function Questionnaire: results from focus groups with visually impaired persons. Arch Ophthalmol 116:227–233
Mangione CM, Lee PP, Pitts J, Gutierrez P, Berry S, Hays RD (1998) Psychometric Properties of the National Eye Institute Visual Function Questionnaire (NEI - VFQ). Arch Ophthalmol 116:1496–1504
Mangione CM, Lee PP, Gutierrez PR, Spritzer K, Berry S, Hays RD (2001) Development of the 25-Item National Eye Institute Visual Function Questionnaire. Arch Ophthalmol 119:1050–1058
McKean-Cowdin R, Wang Y, Wu J, Azen SP, Varma R; Los Angeles Latino Eye Study Group (2008) Impact of Visual Field Loss on Health-Related Quality of Life in Glaucoma. The Los Angeles Latino Eye Study. Ophthalmology 115:941–948
Sumi I, Shirato S, Matsumoto S, Araie M (2003) The relationships between visual disability and visual field in patients with glaucoma. Ophthalmology 110:332–339
Parrish RK 2nd, Gedde SJ, Scott IU, Feuer WJ, Schiffman JC, Mangione CM, Montenegro-Piniella A (1997) Visual function and quality of life among patients with glaucoma. Arch Ophthalmol 115:1447–1455
Bengtsson B, Heijl A (2008) A visual field index for calculation of glaucoma rate of progression. Am J Ophthalmol 145:343–353
Suzukamo Y, Oshika T, Yuzawa M, Tokuda Y, Tomidokoro A, Oki K, Mangione CM, Green J, Fukuhara S (2005) Psychometric properties of the 25-item National Eye Institute Visual Function Questionnaire (NFI VFQ-25). Japanese version. Health Qual Life Outcome 3:65
Gutierrez P, Wilson MR, Johnson C, Gordon M, Cioffi GA, Sherwood M, Meng K, Mangione CM (1997) Influence of glaucomatous visual field loss on health-related quality of life. Arch Ophthalmol 115:777–784
Nelson P, Aspinall P, Papasouliotis O, Worton B, O’Brien C (2003) Quality of life in glaucoma and its relationship with visual function. J Glaucoma 12:139–150
Magacho L, Lima FE, Nery AC, Sagawa A, Magacho B, Avila MP (2004) Quality of life in glaucoma patients: regression analysis and correlation with possible modifiers. Ophthalmic Epidemiol 11:263–270
Lam BL, Alward WL, Kolder HE (1991) Effect of cataract on automated perimetry. Ophthalmology 98:1066–1070
Smith SD, Katz J, Quigley HA (1997) Effect of cataract extraction on the results of automated perimetry in glaucoma. Arch Ophthalmol 115:1515–1519
Araie M, Arai M, Koseki N, Suzuki Y (1995) Influence of myopic refraction on visual field defects in normal tension and primary open angle glaucoma. Jpn J Ophthalmol 39:60–64
Caprioli J, Spaeth GL (1984) Comparison of visual field defects in the low-tension glaucoma with those in the high-tension glaucomas. Am J Ophthalmol 97:730–737
Araie M (1995) Pattern of visual field defects in normal-tension and high-tension glaucoma. Curr Opin Ophthalmol 6:36–45
Jampel HD, Schwartz A, Pollack I, Abrams D, Weiss H, Miller R (2002) Glaucoma patients’ assessment of their visual function and quality of life. J Glaucoma 11:154–163
Freeman EE, Munoz B, Turano KA, West SK (2006) Measures of visual function and their association with driving modification in older adults. Invest Ophthalmol Vis Sci 47:514–520
Haymes SA, Leblanc RP, Nicolela MT, Chiasson LA, Chauban BC (2008) Glaucoma and on-road driving performance. Invest Ophthalmol Vis Sci 49:3035–3041
Acknowledgements
We thank Mses. Shizuko Yamada1, Masayo Endo1, Mayumi Saito1, Miwako Yoshihara2, Junko Watanabe2 for the contribution to this study.
1. Minami Hospital 2. Ojiya Hospital
Financial Disclosure
The authors have no propriety or commercial interest in any materials discussed in this article.
Financial support
None.
Conflict of interest
No conflicting relationship exists for any of the authors.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Sawada, H., Fukuchi, T. & Abe, H. Evaluation of the relationship between quality of vision and the visual function index in Japanese glaucoma patients. Graefes Arch Clin Exp Ophthalmol 249, 1721–1727 (2011). https://doi.org/10.1007/s00417-011-1779-5
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00417-011-1779-5