Abstract
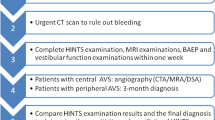
Almost 20 % of cerebral ischaemic strokes occur in the posterior circulation. Estimates are that 20 % of these patients present with isolated vertigo. In approximately one-sixth to one-third of these patients, this symptom is wrongly diagnosed to be peripheral vestibular in origin. As a result, these missed stroke patients are withheld from therapeutic and secondary prophylactic treatment, which may result in unnecessary morbidity and mortality. We therefore propose a diagnostic algorithm concerning the clinical differentiation of acute vestibular syndrome (AVS) patients based on a critical review of the available literature.

Similar content being viewed by others
References
Nouh A, Remke J, Ruland S (2014) Ischemic posterior circulation stroke: a review of anatomy, clinical presentations, diagnosis, and current management. Front Neurol. doi:10.3389/fneur.2014.00030
Venhovens J, Meulstee J, Verhagen WIM (2016) Vestibular evoked myogenic potentials (VEMPs) in central neurological disorders. Clin Neurophysiol 127:40–49. doi:10.1016/j.clinph.2014.12.021
Kim MB, Boo SH, Ban JH (2013) Nystagmus-based approach to vertebrobasilar stroke presenting as vertigo without initial neurologic signs. Eur Neurol 70:322–328. doi:10.1159/000353285
Seemungal BM, Bronstein AM (2008) A practical approach to acute vertigo. Pract Neurol 8:211–221. doi:10.1136/jnnp.2008.154799
Kim JS, Lee H (2013) Vertigo due to posterior circulation stroke. Semin Neurol 33:179–184. doi:10.1055/s-0033-1354600
Grewal K, Austin PC, Kapral MK et al (2015) Missed strokes using computed tomography imaging in patients with vertigo: population-based cohort study. Stroke 46:108–113. doi:10.1161/STROKEAHA.114.007087
Kerber KA, Brown DL, Lisabeth LD et al (2006) Stroke among patients with dizziness, vertigo, and imbalance in the emergency department: a population-based study. Stroke 37:2484–2487. doi:10.1161/01.STR.0000240329.48263.0d
Lee H, Sohn SI, Cho YW et al (2006) Cerebellar infarction presenting isolated vertigo: frequency and vascular topographical patterns. Neurology 67:1178–1183. doi:10.1212/01.wnl.0000238500.02302.b4
Lee H (2014) Isolated vascular vertigo. J Stroke 16:124–130. doi:10.5853/jos.2014.16.3.124
Tehrani ASS, Kattah JC, Mantokoudis G et al (2014) Small strokes causing severe vertigo: frequency of false-negative MRIs and nonlacunar mechanisms. Neurology 83:169–173. doi:10.1212/WNL.0000000000000573
Newman-Toker DE, Kerber KA, Hsieh YH et al (2013) HINTS outperforms ABCD2 to screen for stroke in acute continuous vertigo and dizziness. Acad Emerg Med 20:987–996. doi:10.1111/acem.12223
Newman-Toker DE, Saber Tehrani AS, Mantokoudis G et al (2013) Quantitative video-oculography to help diagnose stroke in acute vertigo and dizziness: toward an ECG for the eyes. Stroke 44:1158–1161. doi:10.1161/STROKEAHA.111.000033
Mantokoudis G, Tehrani ASS, Wozniak A et al (2015) VOR gain by head impulse video-oculography differentiates acute vestibular neuritis from stroke. Otol Neurotol 36:457–465. doi:10.1097/MAO.0000000000000638
Cohn B (2014) Can bedside oculomotor (HINTS) testing differentiate central from peripheral causes of vertigo? Ann Emerg Med 64:265–268. doi:10.1016/j.annemergmed.2014.01.010
Kohn MA (2014) HINTS to identify stroke in ED patients with dizziness. Acad Emerg Med 21:347. doi:10.1111/acem.12339
Edlow JA (2013) Diagnosing dizziness: we are teaching the wrong paradigm! Acad Emerg Med 20:1064–1066. doi:10.1111/acem.12234
Kattah JC, Talkad AV, Wang DZ et al (2009) HINTS to diagnose stroke in the acute vestibular syndrome: three-step bedside oculomotor examination more sensitive than early MRI diffusion-weighted imaging. Stroke 40:3504–3510. doi:10.1161/STROKEAHA.109.551234
Newman-Toker DE, Curthoys IS, Halmagyi GM (2015) Diagnosing stroke in acute vertigo: the HINTS family of eye movement tests and the future of the “Eye ECG”. Semin Neurol 35:506–521. doi:10.1055/s-0035-1564298
Newman-Toker DE (2016) Missed stroke in acute vertigo and dizziness: it is time for action, not debate. Ann Neurol 79:27–31. doi:10.1002/ana.24532
Tarnutzer AA, Berkowitz AL, Robinson KA et al (2011) Does my dizzy patient have a stroke? A systematic review of bedside diagnosis in acute vestibular syndrome. CMAJ 183:E571–E592. doi:10.1503/cmaj.100174
Chen L, Lee W, Chambers BR, Dewey HM (2011) Diagnostic accuracy of acute vestibular syndrome at the bedside in a stroke unit. J Neurol 258:855–861. doi:10.1007/s00415-010-5853-4
Akhtar N, Kamran SI, Deleu D et al (2009) Ischaemic posterior circulation stroke in State of Qatar. Eur J Neurol 16:1004–1009. doi:10.1111/j.1468-1331.2009.02709.x
Searls DE (2012) Symptoms and signs of posterior circulation ischemia in the new England medical center posterior circulation registry. Arch Neurol 69:346. doi:10.1001/archneurol.2011.2083
Brandt T, Dieterich M (1993) Vestibular falls. J Vestib Res 3:3–14
Jeong SH, Kim HJ, Kim JS (2013) Vestibular neuritis. Semin Neurol 33:185–194. doi:10.1055/s-0033-1354598
Lee H, Sohn SI, Jung DK et al (2002) Sudden deafness and anterior inferior cerebellar artery infarction. Stroke 33:2807–2812
Lee H (2012) Audiovestibular loss in anterior inferior cerebellar artery territory infarction: a window to early detection? J Neurol Sci 313:153–159. doi:10.1016/j.jns.2011.08.039
Lee H, Kim JS, Chung EJ et al (2009) Infarction in the territory of anterior inferior cerebellar artery: spectrum of audiovestibular loss. Stroke 40:3745–3751. doi:10.1161/STROKEAHA.109.564682
Venhovens J, Meulstee J, Verhagen WIM (2015) The negative predictive value of the head impulse test, nystagmus, and test of skew deviation bedside oculomotor examination in acute vestibular syndrome. Ann Emerg Med 66:91–92. doi:10.1016/j.annemergmed.2015.03.009
Chen L, Todd M, Halmagyi GM, Aw S (2014) Head impulse gain and saccade analysis in pontine-cerebellar stroke and vestibular neuritis. Neurology 83:1513–1522. doi:10.1212/WNL.0000000000000906
Kerber KA, Meurer WJ, Brown DL et al (2015) Stroke risk stratification in acute dizziness presentations: a prospective imaging-based study. Neurology 85:1869–1878. doi:10.1212/WNL.0000000000002141
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflicts of interest
None to be disclosed.
Rights and permissions
About this article
Cite this article
Venhovens, J., Meulstee, J. & Verhagen, W.I.M. Acute vestibular syndrome: a critical review and diagnostic algorithm concerning the clinical differentiation of peripheral versus central aetiologies in the emergency department. J Neurol 263, 2151–2157 (2016). https://doi.org/10.1007/s00415-016-8081-8
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00415-016-8081-8