Abstract
Background
Physiotherapy is a common treatment option in patients with fecal incontinence. Although physiotherapy may result in relief of symptoms, to what extent improvement is associated with changes in anorectal function is still unclear.
Aim
The aim of the present study was to investigate prospectively how anorectal function changes with physiotherapy and whether these changes are related to changes in fecal incontinence score.
Methods
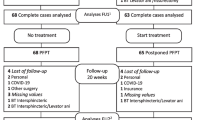
Consenting consecutive patients (n=266) with fecal incontinence (91% women; mean age, 59 years) underwent anorectal manometry, anal and rectal mucosal sensitivity measurements, and rectal capacity measurement at baseline and after nine sessions of standardized pelvic floor physiotherapy. These findings were compared with changes in Vaizey incontinence score.
Results
On follow-up 3 months after physiotherapy, squeeze pressure (p=0.028), as well as urge sensation threshold (p=0.046) and maximum tolerable volume (p=0.018), had increased significantly. The extent of improvement was not related to age, duration of fecal incontinence, menopause, and endosonography findings. All other anorectal functions did not change. An improvement in the Vaizey score was moderately correlated with an increase in incremental squeeze pressure (r=0.14, p=0.04) and a decrease in anal mucosal sensitivity threshold (r=0.20, p=0.01).
Conclusions
Physiotherapy improves squeeze pressure, urge sensation, and maximum tolerable volume. However, improved anorectal function does not always result in a decrease in fecal incontinence complaints.


Similar content being viewed by others
References
Cardozo L, Khoury S, Weiri A (eds) (2001) Proceedings of the second international consultation on incontinence. Health Publication Ltd, Plymouth
Perry S, Shaw C, McGrother C et al (2002) Prevalence of faecal incontinence in adults aged 40 years or more living in the community. Gut 50:480–484
Borrie MJ, Davidson HA (1992) Incontinence in institutions: costs and contributing factors. CMAJ 147:322–328
Johanson JF, Irizarry F, Doughty A (1997) Risk factors for fecal incontinence in a nursing home population. J Clin Gastroenterol 24:156–160
Madoff RD, Parker SC, Varma MG, Lowry AC (2004) Faecal incontinence in adults. Lancet 364(9434):621–632
Mavrantonis C, Wexner SD (1998) A clinical approach to fecal incontinence. J Clin Gastroenterol 27:108–121
Jorge JM, Wexner SD (1993) Etiology and management of fecal incontinence. Dis Colon Rectum 36:77–97
Cheetham MJ, Malouf AJ, Kamm MA (2001) Fecal incontinence. Gastroenterol Clin North Am 30(1):115–130
Kamm MA (1998) Faecal incontinence. BMJ 316:528–532
Norton C, Hosker G, Brazzelli M (2000) Biofeedback and/or sphincter exercises for the treatment of faecal incontinence in adults. Cochrane Database Syst Rev (2):CD002111
Rao SS, Welcher KD, Happel J (1996) Can biofeedback therapy improve anorectal function in fecal incontinence? Am J Gastroenterol 91(11):2360–2366
Ozturk R et al (2004) Long-term outcome and objective changes of anorectal function after biofeedback therapy for faecal incontinence. Aliment Pharmacol Ther 20(6):667–674
Sangwan YP, Coller JA, Barrett RC et al (1995) Can manometric parameters predict response to biofeedback therapy in fecal incontinence? Dis Colon Rectum 38(10):1021–1025
Martinez-Puente Mdel C, Pascual-Montero JA, Garcia-Olmo D (2004) Customized biofeedback therapy improves results in fecal incontinence. Int J Colorectal Dis 19(3):210–214
Chiarioni G, Scattolini C, Bonfante F, Vantini I (1993) Liquid stool incontinence with severe urgency: anorectal function and effective biofeedback treatment. Gut 34(11):1576–1580
Chiarioni G, Bassotti G, Stegagnini S et al (2002) Sensory retraining is key to biofeedback therapy for formed stool fecal incontinence. Am J Gastroenterol 97(1):109–117
Diamant NE, Kamm MA, Wald A, Whitehead WE (1999) AGA technical review on anorectal testing techniques. Gastroenterology 116(3):735–760
Soffer EE, Hull T (2000) Fecal incontinence: a practical approach to evaluation and treatment. Am J Gastroenterol 95(8):1873–1880 (review)
Bharucha AE (2003) Fecal incontinence. Gastroenterology 124:1672–1685
Rao SS, Patel RS (1997) How useful are manometric tests of anorectal function in the management of defecation disorders? Am J Gastroenterol 92(3):469–475
Bharucha AE (2004) Outcome measures for fecal incontinence: anorectal structure and function. Gastroenterology 126(Suppl 1):S90–S98
Vaizey CJ et al (1999) Prospective comparison of faecal incontinence grading systems. Gut 44:77–80
Rao SS, Welcher KD, Leistikow JS (1998) Obstructive defecation: a failure of rectoanal coordination. Am J Gastroenterol 93(7):1042–1050
Isherwood PJ, Rane A (2000) Comparative assessment of pelvic floor strength using a perineometer and digital examination. BJOG 107(8):1007–1011
Laycock J, Jerwood D (2001) Pelvic floor muscle assessment: the perfect scheme. Physiotherapy 87:631–642
Baxter NN, Rothenberger DA, Lowry AC (2003) Measuring fecal incontinence. Dis Colon Rectum 46:1591–1605
Rao SSC (2004) Diagnosis and management of fecal incontinence. American College of Gastroenterology Practice Parameters Committee. Am J Gastroenterol 99(8):1585–1604
Felt-Bersma RJ, Poen AC, Cuesta MA, Meuwissen SG (1997) Anal sensitivity test: what does it measure and do we need it? Cause or derivative of anorectal complaints. Dis Colon Rectum 40(7):811–816
Prather CM (2004) Predictors of outcome in treatment trials. Gastroenterology 126:S135–S140
Acknowledgements
This work was supported by a grant from The Netherlands Organization for Health Research and Development ZON-MW (grant 945-01-013, 2001).
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Dobben, A.C., Terra, M.P., Berghmans, B. et al. Functional changes after physiotherapy in fecal incontinence. Int J Colorectal Dis 21, 515–521 (2006). https://doi.org/10.1007/s00384-005-0049-6
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00384-005-0049-6