Abstract
Objective
To evaluate the health-related quality of life on a very long-term follow-up in patients treated with extracorporeal membrane oxygenation (ECMO) during neonatal and pediatric age.
Design
Prospective follow-up study.
Setting
Pediatric Intensive Care Unit of a tertiary-care University-Hospital.
Patients
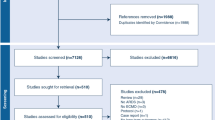
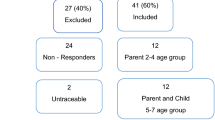
Out of 20 neonates and 21 children treated with ECMO in our center, 24 patients underwent short-term neurological follow-up. Twenty of them underwent long-term neurological follow-up.
Intervention
Short-term follow-up was performed at 18 months and consisted in clinical evaluation, electroencephalography, and neuroimaging. Long-term follow-up was performed in 2017, at the mean period 19.72 years from ECMO (median 20.75, range 11.50–24.08) and consisted in a standardized questionnaires self-evaluation (PedsQL 4.0 Generic Core Scale) of health-related quality of life and an interviewed about the presence of organ morbidity, school level, or work position.
Measurements and main results
Sixty-one percent (25/41) of the patients survived within 30 days after ECMO treatment. Short-term follow-up was performed in 24 patients (1 patient but died before the evaluation): 21 patients (87%) showed a normal neurological status, and 3 developed severe disability. Long-term follow-up was performed in 20 long-term survivors (3 patients were not possible to be contacted and considered lost to follow-up): mean age of patients at long-term follow-up was 21.23 (median 20.96, range 13.33–35.58) years; 90% (18/20) of them have no disability with a complete normal quality of life and 95% have no cognitive impairment.
Conclusions
ECMO represents a life-saving treatment for infants and children with respiratory and/or heart failure; survivors show a good quality of life comparable to healthy peers.

Similar content being viewed by others
References
Bartlett RH, Gazzaniga AB, Jefferies MR, Huxtable RF, Haiduc NJ, Fong SW (1976) Extracorporeal membrane oxygenation (ECMO) cardiopulmonary support in infancy. Trans Am Soc Artif Intern Organs 22:80–93
Bartlett RH, Gazzaniga AB, Toomasian J et al (1986) Extracorporeal membrane oxygenation (ECMO) in neonatal respiratory failure. 100 cases. Ann Surg 204:236–245
Butt W, Mac laren G (2016) Extracorporeal membrane oxygenation 2016: an update. Version 1. F1000Res 5:F1000 Faculty Rev-750
ECLS Registry Report: International Summary July 2016. Available from URL: https://www.elso.org/Registry/Statistics/InternationalSummary.aspx
Cengiz P, Seidel K, Rycus PT, Brogan TV, Roberts JS (2005) Central nervous system complications during pediatric extracorporeal life support: incidence and risk factors. Crit Care Med 33:2817–2824
Hervey-Jumper SL, Annich GM, Yancon AR, Garton HJL, Muraszko KM, Maher CO (2011) Neurological complications of extracorporeal membrane oxygenation in children. J Neurosurg Pediatr 7:338–344
Glass P, Wagner AE, Papero PH, Rajasingham SR, Civitello LA, Kjaer MS, Coffman CE, Getson PR, Short BL (1995 Sep) Neurodevelopmental status at age five years of neonates treated with extracorporeal membrane oxygenation. J Pediatr 127:447–457
Thiagarajan RR, Laussen PC, Rycus PT, Bartlett RH, Bratton SL (2007) Extracorporeal membrane oxygenation to aid cardiopulmonary resuscitation in infants and children. Circulation 116:1693–1700
Sivarajan VB, Best D, Brizard CP, Shekerdemian LS, d’Udekem Y, Butt W (2011) Duration of resuscitation prior to rescue extracorporeal membrane oxygenation impacts outcome in children with heart disease. Intensive Care Med 37:853–860
Amigoni A, Pettenazzo A, Biban P, Suppiej A, Freato F, Zaramella P, Zacchello F (2005) Neurologic outcome in children after extracorporeal membrane oxygenation: prognostic value of diagnostic tests. Pediatr Neurol 32:173–179
Barrett CS, Bratton SL, Salvin JW, Laussen PC, Rycus PT, Thiagarajan RR (2009) Neurological injury after extracorporeal membrane oxygenation use to aid pediatric cardiopulmonary resuscitation. Pediatr Crit Care Med 10:445–451
Huang SC, Wu ET, Wang CC, Chen YS, Chang CI, Chiu IS, Ko WJ, Wang SS (2012) Eleven years of experience with extracorporeal cardiopulmonary resuscitation for paediatric patients with in-hospital cardiac arrest. Resuscitation 83:710–714
Waitzer E, Riley SP, Perreault T, Shevell MI (2009) Neurologic outcome at school entry for newborns treated with extracorporeal membrane oxygenation for noncardiac indications. J Child Neurol 24:801–806
Costello JM, O’Brien MBA, Wypij D et al (2012) Quality of life of pediatric cardiac patients who previously required extracorporeal membrane oxygenation. Pediatr Crit Care Med 13:428–434
Fleck TP, Dangel G, Bächle F et al (2017) Long-term follow-up on health-related quality of life after mechanical circulatory support in children. Pediatr Crit Care Med 18:176–182
Garcia Guerra G, Robertson CM, Alton GY, Joffe AR, Moez EK, Dinu IA, Ross DB, Rebeyka IM, Lequier L, Western Canadian Complex Pediatric Therapies Follow-Up Group (2014) Health-related quality of life in pediatric cardiac extracorporeal life support survivors. Pediatr Crit Care Med 15:720–727
Madderom MJ, Gischler SJ, Duivenvoorden H, Tibboel D, IJsselstijn H (2013) Neonatal extracorporeal membrane oxygenation: impaired health at 5 years of age. Pediatr Crit Care Med 14:183–193
Varni JW, Seid M, Knight TS, Uzark K, Szer IS (2002) The PedsQL 4.0 Generic Core Scales: sensitivity, responsiveness, and impact on clinical decision-making. J Behav Med 25:175–193
Boyle K, Felling R, Yiu A, Battarjee W, Schwartz JME, Salorio C, Bembea MM (2018; Jun 11) Neurologic outcomes after extracorporeal membrane oxygenation-a systematic review. Pediatr Crit Care Med 19:760–766
Pressler R, Bady B, Binnie CD et al (2003) Neurophysiology of the neonatal period. In: Binnie CD, Cooper R, Mauguière F, Osselton J, Prior PF, Tedman BM (eds) Clinical neurophysiology, Vol II: EEG, paediatric neurophysiology, special techniques and applications. Elsevier, Amsterdam, pp 450–601
Bayley N (1993) Bayley scales of infant development, 2nd edn. Psychological Corporation, San Antonio
Thorndike RL, Hagen EP, Stanford-Binet SJM (1986) Intelligence Scale: Fourth Edition. Riverside Publishing, Itasca
Wechsler D (1967) Wechsler preschool and primary scale of intelligence manual. The Psychological Corporation, New York
Wechsler D (1991) Manual for the Wechsler intelligence scale for children III. The Psychological Corporation, New York
Varni JW, Seid M, Kurtin PS (2001) PedsQL 4.0: reliability and validity of the Pediatric Quality of Life Inventory version 4.0 generic core scales in healthy and patient populations. Med Care 39(8):800–812
Varni JW, Burwinkle TM, Seid M, Skarr D (2003) The PedsQL 4.0 as a pediatric population health measure: feasibility, reliability, and validity. Ambul Pediatr 3:329–341
Varni JW, Limbers CA (2009) The PedsQL 4.0 generic core scales young adult version: feasibility, reliability and validity in a university student population. J Health Psychol 14:611–622
Taylor AK, Cousins R, Butt WW (2007) The long-term outcome of children managed with extracorporeal life support: an institutional experience. Crit Care Resusc 9:172–177
Morris MC, Ittenbach RF, Godinez RI, Portnoy JD, Tabbutt S, Hanna BD, Hoffman TM, Gaynor JW, Connelly JT, Helfaer MA, Spray TL, Wernovsky G (2004) Risk factors for mortality in 137 pediatric cardiac intensive care unit patients managed with extracorporeal membrane oxygenation. Crit Care Med 32:1061–1069
Wagner K, Risnes I, Berntsen T, Skarbø AB, Ramberg B, Vandvik IH, Rasmussen M, Nome T, Olsen KB, Svennevig JL (2007) Clinical and psychosocial follow-up study of children treated with extracorporeal membrane oxygenation. Ann Thorac Surg 84:1349–1355
Gupta P, Robertson MJ, Beam B et al (2015) Relationship of ECMO duration with outcomes after pediatric cardiac surgery: a multi-institutional analysis. Minerva Anestesiol 81:619–627
Hamrick SE, Gremmels DB, Keet CA et al (2003) Neurodevelopmental outcome of infants supported with extracorporeal membrane oxygenation after cardiac surgery. Pediatrics 111:671–675
Lequier L, Joffe AR, Robertson CM, Dinu IA, Wongswadiwat Y, Anton NR, Ross DB, Rebeyka IM (2008) Two-year survival, mental, and motor outcomes after cardiac extracorporeal life support at less than five years of age. J Thorac Cardiovasc Surg 136:976–983
Hanekamp MN, Mazer P, van der Cammen-van Zijp MHM, van Kessel-Feddema BJM, Nijhuis-van der Sanden MWG, Knuijt S, Zegers-Verstraeten JLA, Gischler SJ, Tibboel D, Kollée LAA (2006) Follow-up of newborns treated with extracorporeal membrane oxygenation: a nationwide evaluation at 5 years of age. Crit Care 10:R127
Khambekar K, Nichani S, Luyt DK, Peek G, Firmin RK, Field DJ, Pandya HC (2006) Developmental outcome in newborn infants treated for acute respiratory failure with extracorporeal membrane oxygenation: present experience. Arch Dis Child Fetal Neonatal Ed 91:F21–F25
Rais-Bahrami K, Wagner AE, Coffman C, Glass P, Short BL (2000) Neurodevelopmental outcome in ECMO vs Near-Miss ECMO patients at 5 years of age. Clin Pediatr (Phila) 39:145–152
Acknowledgments
The investigators acknowledge all the families of treated patients.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
Authors have no conflict of interest to declare.
Rights and permissions
About this article
Cite this article
Di Leo, V., Biban, P., Mercolini, F. et al. The quality of life in extracorporeal life support survivors: single-center experience of a long-term follow-up. Childs Nerv Syst 35, 227–235 (2019). https://doi.org/10.1007/s00381-018-3999-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00381-018-3999-z