Abstract
Purposes
This paper reports the development and evaluation of a perceived cognitive function (pedsPCF) item bank reported by parents of the pediatric US general population.
Methods
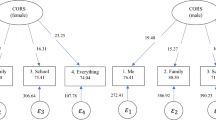
Based on feedback from clinicians, parents, and children, we developed a scale sampling concerns related to children’s cognitive functioning. We administered the scale to 1,409 parents of children aged 7–17 years; of them, 319 had a neurological diagnosis. Dimensionality of the pedsPCF was evaluated via factor analyses and its clinical utility studied by comparing parent ratings in patient groups and symptom cluster defined by the Child Behavior Checklist (CBCL).
Results
Forty-four of 45 items met criteria for unidimensionality. The pedsPCF significantly differentiated samples defined by medication use, repeated grades, special education status, neurologic diagnosis, and relevant symptom clusters with large effect sizes (>0.8). It can predicted children symptoms with the correction rates ranging 79–89%.
Conclusions
We have provided empirical support for the unidimensionality of the pedsPCF item bank and evidence for its potential clinical utility. The pedsPCF is a promising measurement tool to screen children for further comprehensive cognitive tests.

Similar content being viewed by others
References
Mulhern RK, Merchant TE, Gajjar A, Reddick WE, Kun LE (2004) Late neurocognitive sequelae in survivors of brain tumours in childhood. Lancet Oncol 5:399–408
Meador KJ (2002) Cognitive outcomes and predictive factors in epilepsy. Neurology 58:S21–S26
Conway MA (1991) In defense of everyday memory. Am Psychol 46:19–26
Loftus EF (1991) The glitter of everyday memory and the gold. Am Psychol 46:16–18
Chaytor N, Schmitter-Edgecombe M (2003) The ecological validity of neuropsychological tests: a review of the literature on everyday cognitive skills. Neuropsychol Rev 13:181–197
Silver CH (2000) Ecological validity of neuropsychological assessment in childhood traumatic brain injury. J Head Trauma Rehabil 15:973–988
Dufouil C, Fuhrer R, Alperovitch A (2005) Subjective cognitive complaints and cognitive decline: consequence or predictor? The epidemiology of vascular aging study. J Am Geriatr Soc 53:616–621
Zimprich D, Martin M, Kliegel M (2003) Subjective cognitive complaints, memory performance, and depressive affect in old age: a change-oriented approach. Int J Aging Hum Dev 57:339–366
Blazer DG, Hays JC, Fillenbaum GG, Gold DT (1997) Memory complaint as a predictor of cognitive decline: a comparison of African American and white elders. J Aging Health 9:171–184
Jorm AF, Christensen H, Korten AE, Henderson AS, Jacomb PA, MacKinnon A (1997) Do cognitive complaints either predict future cognitive decline or reflect past cognitive decline? A longitudinal study of an elderly community sample. Psychol Med 27:91–98
Christodoulou C, Melville P, Scherl WF, Morgan T, MacAllister WS, Canfora DM, Berry SA, Krupp LB (2005) Perceived cognitive dysfunction and observed neuropsychological performance: longitudinal relation in persons with multiple sclerosis. J Int Neuropsychol Soc 11:614–619
Banos JH, LaGory J, Sawrie S, Faught E, Knowlton R, Prasad A, Kuzniecky R, Martin RC (2004) Self-report of cognitive abilities in temporal lobe epilepsy: cognitive, psychosocial, and emotional factors. Epilepsy Behav 5:575–579
Allen CC, Ruff RM (1990) Self-rating versus neuropsychological performance of moderate versus severe head-injured patients. Brain Inj 4:7–17
Kadis DS, Stollstorff M, Elliott I, Lach L, Smith ML (2004) Cognitive and psychological predictors of everyday memory in children with intractable epilepsy. Epilepsy Behav 5:37–43
de Groot JC, de Leeuw FE, Oudkerk M, Hofman A, Jolles J, Breteler MM (2001) Cerebral white matter lesions and subjective cognitive dysfunction: the Rotterdam Scan Study. Neurology 56:1539–1545
Ferguson RJ, McDonald BC, Saykin AJ, Ahles TA (2007) Brain structure and function differences in monozygotic twins: possible effects of breast cancer chemotherapy. J Clin Oncol 25:3866–3870
Mahone EM, Martin R, Kates WR, Hay T, Horska A (2009) Neuroimaging correlates of parent ratings of working memory in typically developing children. J Int Neuropsychol Soc 15:31–41
Soni MK, Cella D (2002) Quality of life and symptom measures in oncology: an overview. Am J Manage Care 8:S560–S573
Hahn EA, Cella D (2003) Health outcomes assessment in vulnerable populations: measurement challenges and recommendations. Arch Phys Med Rehabil 84:S35–S42
Nathan PC, Patel SK, Dilley K, Goldsby R, Harvey J, Jacobsen C, Kadan-Lottick N, McKinley K, Millham AK, Moore I, Okcu MF, Woodman CL, Brouwers P, Armstrong FD (2007) Guidelines for identification of, advocacy for, and intervention in neurocognitive problems in survivors of childhood cancer: a report from the Children’s Oncology Group. Arch Pediatr Adolesc Med 161:798–806
Achenbach TM (1991) Integrative guide to the 1991 CBCL/4–18, YSR, and TRF profiles. University of Vermont, Department of Psychology, Burlington, VT
McDonald RP (1999) Test Theory: A unified treatment. Lawrence Earlbaum Associates, Inc., Mahwah, NJ
Reise SP, Morizot J, Hays RD (2007) The role of the bifactor model in resolving dimensionality issues in health outcomes measures. Qual Life Res 16(Suppl 1):19–31
Lai JS, Crane PK, Cella D (2006) Factor analysis techniques for assessing sufficient unidimensionality of cancer related fatigue. Qual Life Res 15:1179–1190
Lai JS, Butt Z, Wagner L, Sweet JJ, Beaumont JL, Vardy J, Jacobsen PB, Jacobs SR, Shapiro PJ, Cella D (2009) Evaluating the dimensionality of perceived cognitive function. J Pain Symptom Manage 37:982–995
Cook KF, Kallen MA, Amtmann D (2009) Having a fit: impact of number of items and distribution of data on traditional criteria for assessing IRT’s unidimensionality assumption. Qual Life Res 18:447–460
Czyzewski DI, Mariotto MJ, Bartholomew LK, LeCompte SH, Sockrider MM (1994) Measurement of quality of well being in a child and adolescent cystic fibrosis population. Med Care 32:965–972
Hinds PS, Hockenberry M, Rai SN, Zhang L, Razzouk BI, Cremer L, McCarthy K, Rodriguez-Galindo C (2007) Clinical field testing of an enhanced-activity intervention in hospitalized children with cancer. J Pain Symptom Manage 33:686–697
Lustig RH, Hinds PS, Ringwald-Smith K, Christensen RK, Kaste SC, Schreiber RE, Rai SN, Lensing SY, Wu S, Xiong X (2003) Octreotide therapy of pediatric hypothalamic obesity: a double-blind, placebo-controlled trial. J Clin Endocrinol Metab 88:2586–2592
Flavell JH (1979) Metacognitive and cognitive monitoring: a new area of cognitive developmental inquiry. Am Psychol 34:906–911
Schwartz BL, Perfect TJ, Perfect T (2002) Introduction: toward an applied metacognition. Applied metacognition. Cambridge University Press, West Nyack, p 1EP-10
Mahone EM, Zabel TA, Levey E, Verda M, Kinsman S (2002) Parent and self-report ratings of executive function in adolescents with myelomeningocele and hydrocephalus. Child Neuropsychol 8:258–270
Chen WH, Revicki DA, Lai JS, Cook KF, Amtmann D (2009) Linking pain items from two studies onto a common scale using item response theory. J Pain Symptom Manage 38:615–628
Castellon SA, Ganz PA, Bower JE, Petersen L, Abraham L, Greendale GA (2004) Neurocognitive performance in breast cancer survivors exposed to adjuvant chemotherapy and tamoxifen. J Clin Exp Neuropsychol 26:955–969
Bennett-Levy J, Polkey CE, Powell GE (1980) Self-report of memory skills after temporal lobectomy: the effect of clinical variables. Cortex 16:543–557
Larrabee GJ, Levin HS (1986) Memory self-ratings and objective test performance in a normal elderly sample. J Clin Exp Neuropsychol 8:275–284
Acknowledgement
This project is supported by the National Cancer Institute (Grant number: R01CA125671; PI: Jin-Shei Lai). Dr. Butt’s time is supported in part by grant KL2RR0254740 from the National Center for Research Resources, National Institutes of Health.
Author information
Authors and Affiliations
Corresponding author
Appendix
Appendix
Rights and permissions
About this article
Cite this article
Lai, JS., Zelko, F., Butt, Z. et al. Parent-perceived child cognitive function: results from a sample drawn from the US general population. Childs Nerv Syst 27, 285–293 (2011). https://doi.org/10.1007/s00381-010-1230-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00381-010-1230-y