Abstract
Purpose
In biopsy naïve men suspected for prostate cancer (PCa), it is uncertain how a risk-calculator and bi-parametric (bp) MRI should be combined to decide on prostate biopsy, balancing cancer detection rates and diagnostic burden.
Methods
Prospective, single centre cohort study (August 2018–April 2019). All patients referred with serum PSA ≥ 3 ng/ml or abnormal digital rectal examination received bpMRI and risk for PCa was calculated using the ERSPC risk-calculator. Men with either PI-RADS ≥ 3 or calculator risk-score > 20% were recommended to undergo systematic biopsy (SB) and targeted biopsy (TB) of any visible lesion (reference pathway). Eight different derived diagnostic pathways were compared to the reference pathway regarding cancer detection, number of biopsies and bpMRIs performed.
Results
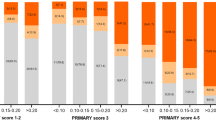
Of 496 patients; 233 (47%) had a risk-calculator score of > 20%; 201 (41%) had PI-RADS score ≥ 3. The reference pathway detected PCa in 32.1%, clinically significant (cs) PCa in 19.4%, with 41% avoided biopsies, but 0% avoided bpMRI. Stratification with only risk-calculator: 76% csPCa diagnosed, 53% avoided biopsies and 100% avoided bpMRI. Stratification with only bpMRI: 97% csPCa diagnosed, 59% avoided biopsies, but 0% avoided bpMRI. A pathway with risk-calculator first, followed only with bpMRI when high-risk: 81% csPCa diagnosed, 72% avoided biopsies and 53% avoided bpMRI.
Conclusion
Upfront bpMRI as a risk stratification tool outperforms risk-calculator in detecting significant disease. Applying the risk-calculator first to decide on performing an MRI, avoids 1 out of 2 MRIs, but up to 1 out of 5 significant cancers are missed.



Similar content being viewed by others
Data availability
Anonymized data available upon request.
References
Ahmed HU, El-Shater Bosaily A, Brown LC et al (2017) Diagnostic accuracy of multi-parametric MRI and TRUS biopsy in prostate cancer (PROMIS): a paired validating confirmatory study. Lancet 389(10071):815–822. https://doi.org/10.1016/S0140-6736(16)32401-1
Fine SW, Epstein JI (2008) A contemporary study correlating prostate needle biopsy and radical prostatectomy Gleason score. J Urol 179(4):1335–1338. https://doi.org/10.1016/j.juro.2007.11.057(discussion 1338-9)
Kasivisvanathan V, Rannikko AS, Borghi M et al (2018) MRI-targeted or standard biopsy for prostate-cancer diagnosis. N Engl J Med 378(19):1767–1777. https://doi.org/10.1056/NEJMoa1801993
Mottet N, Bellmunt J, Bolla M et al (2017) EAU-ESTRO-SIOG guidelines on prostate cancer. Part 1: Screening, diagnosis, and local treatment with curative intent. Eur Urol 71(4):618–629. https://doi.org/10.1016/j.eururo.2016.08.003
Mannaerts CK, Kajtazovic A, Lodeizen OAP et al (2019) The added value of systematic biopsy in men with suspicion of prostate cancer undergoing multiparametric MRI-targeted biopsy. Urol Oncol 37(5):298.e1-298.e9. https://doi.org/10.1016/j.urolonc.2019.01.005
Moldovan PC, Van den Broeck T, Sylvester R et al (2017) What Is the negative predictive value of multiparametric magnetic resonance imaging in excluding prostate cancer at biopsy? A systematic review and meta-analysis from the European association of urology prostate cancer guidelines panel. Eur Urol 72(2):250–266. https://doi.org/10.1016/j.eururo.2017.02.026
Roobol MJ, Steyerberg EW, Kranse R et al (2010) A risk-based strategy improves prostate-specific antigen-driven detection of prostate cancer. Eur Urol 57(1):79–85. https://doi.org/10.1016/j.eururo.2009.08.025
Schoots IG, Padhani AR (2020) Personalizing prostate cancer diagnosis with multivariate risk prediction tools: how should prostate MRI be incorporated? World J Urol 38(3):531–545. https://doi.org/10.1007/s00345-019-02899-0
Nederlandse vereniging voor Urologie (2007) Prostaatcarcinoom. Landelijke richtlijn, versie 2.0. Integr Kankercent Ned 285. https://www.nhg.org/sites/default/files/content/nhg_org/uploads/prostaatcarcinoom.pdf
Barentsz JO, Richenberg J, Clements R et al (2012) ESUR prostate MR guidelines 2012. Eur Radiol 22(4):746–757. https://doi.org/10.1007/s00330-011-2377-y
Kuru TH, Roethke MC, Rieker P et al (2013) Histology core-specific evaluation of the European society of urogenital radiology (ESUR) standardised scoring system of multiparametric magnetic resonance imaging (mpMRI) of the prostate. BJU Int 112(8):1080–1087. https://doi.org/10.1111/bju.12259
Epstein JI, Amin MB, Beltran H et al (2014) Proposed morphologic classification of prostate cancer with neuroendocrine differentiation. Am J Surg Pathol 38(6):756–767. https://doi.org/10.1097/PAS.0000000000000208
Siddiqui MM, Rais-Bahrami S, Turkbey B et al (2015) Comparison of MR/ultrasound fusion-guided biopsy with ultrasound-guided biopsy for the diagnosis of prostate cancer. JAMA 313(4):390–397. https://doi.org/10.1001/jama.2014.17942
Tonttila PP, Lantto J, Pääkkö E et al (2016) Prebiopsy multiparametric magnetic resonance imaging for prostate cancer diagnosis in biopsy-naive men with suspected prostate cancer based on elevated prostate-specific antigen values: results from a randomized prospective blinded controlled trial. Eur Urol 69(3):419–425. https://doi.org/10.1016/j.eururo.2015.05.024
Elkhoury FF, Felker ER, Kwan L et al (2019) Comparison of targeted vs. systematic prostate biopsy in men who are biopsy naive: the prospective assessment of image registration in the diagnosis of prostate cancer (PAIREDCAP) study. JAMA Surg 154(9):811–818. https://doi.org/10.1001/jamasurg.2019.1734
Drost F-JH, Osses DF, Nieboer D et al (2019) Prostate MRI, with or without MRI-targeted biopsy, and systematic biopsy for detecting prostate cancer. Cochrane database Syst Rev 4:CD012663. https://doi.org/10.1002/14651858.CD012663.pub2
van der Leest M, Cornel E, Israël B et al (2019) Head-to-head comparison of transrectal ultrasound-guided prostate biopsy versus multiparametric prostate resonance imaging with subsequent magnetic resonance-guided biopsy in biopsy-naïve men with elevated prostate-specific antigen: a large prospective mu. Eur Urol 75(4):570–578. https://doi.org/10.1016/j.eururo.2018.11.023
Stolk TT, de Jong IJ, Kwee TC et al (2019) False positives in PIRADS (V2) 3, 4, and 5 lesions: relationship with reader experience and zonal location. Abdom Radiol (NY) 44(3):1044–1051. https://doi.org/10.1007/s00261-019-01919-2
Vargas HA, Hötker AM, Goldman DA et al (2016) Updated prostate imaging reporting and data system (PIRADS v2) recommendations for the detection of clinically significant prostate cancer using multiparametric MRI: critical evaluation using whole-mount pathology as standard of reference. Eur Radiol 26(6):1606–1612. https://doi.org/10.1007/s00330-015-4015-6
Kang Z, Min X, Weinreb J et al (2019) Abbreviated biparametric versus standard multiparametric MRI for diagnosis of prostate cancer: a systematic review and meta-analysis. AJR Am J Roentgenol 212(2):357–365. https://doi.org/10.2214/AJR.18.20103
Funding
This study did not receive any funding.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethics approval
The study has been approved by the local research ethics committee of the St. Antonius Hospital Utrecht/Nieuwegein (W17.087) and was conducted in accordance with Good Clinical Practice Guidelines.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Reesink, D.J., Schilham, M.G.M., van der Hoeven, E.J.R.J. et al. Comparison of risk-calculator and MRI and consecutive pathways as upfront stratification for prostate biopsy. World J Urol 39, 2453–2461 (2021). https://doi.org/10.1007/s00345-020-03488-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00345-020-03488-2