Abstract
Background
The aims of our study were to identify studies that evaluated patient satisfaction after transsexual surgery, analyze existing questionnaires, and summarize their development, psychometric properties, and content.
Methods
A systematic review of the English-language literature was performed. Patient-reported outcome measures designed to assess patient satisfaction and quality of life following transsexual surgery were identified. Qualifying instruments were assessed for content and adherence to international guidelines for development and validation.
Results
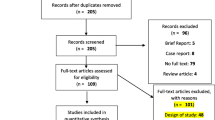
From 796 articles, 19 studies had sufficient data and met the inclusion criteria. Included were a total of 2299 patients and 17 patient-reported outcome measures: 10 generic instruments that assessed quality of life, 4 specific for female genital or sexual satisfaction, 2 specific for transsexual body image or gender dysphoria, and 1 specific for plastic surgery. The questionnaires were analyzed by reviewers to assess the adherence to the rules of the US FDA and the Scientific Advisory Committee of the Medical Outcomes Trust. We identified 17 individual questionnaires that were included. All measures were limited by either their development, their validation, or their content.
Conclusions
There is a need for a new self-assessment tool, which should include functional, psychorelational, and cosmetic components, to measure satisfaction and quality of life of patients who have undergone transsexual surgery.
Level of Evidence III
This journal requires that authors assign a level of evidence to each article. For a full description of these Evidence-Based Medicine ratings, please refer to the Table of Contents or the online Instructions to Authors www.springer.com/00266.

Similar content being viewed by others
References
Cash TF (2004) Body image: past, present, and future. Body Image 1:1–5
van de Grift TC, Cohen-Kettenis PT, Elaut E, De Cuypere G, Richter-Appelt H, Haraldsen IR, Kreukels BP (2016) A network analysis of body satisfaction of people with gender dysphoria. Body Image 17:184–190
Jones BA, Haycraft E, Murjan S, Arcelus J (2016) Body dissatisfaction and disordered eating in trans people: a systematic review of the literature. Int Rev Psychiatry 28:81–94
Meyer W III, Bockting WO, Cohen-Kettenis P, Coleman E, DiCeglie D, Devor H (2001) The standards of care for gender identity disorders, 6th version. Symposion, Dusseldorf
Hess J, Rossi Neto R, Panic L, Rübben H, Senf W (2014) Satisfaction with male-to-female gender reassignment surgery. Dtsch Arztebl Int 111:795–801
Di Stefano N (2014) Irriducibilità e originarietà del Leib: riflessioni a partire dal transessualismo. Fenomenologia e Società 2:156–171
Tambone V, Cogliandro A, Di Stefano N (2012) Quale estetica per la medicina? Un inquadramento teoretico. In: Persichetti P, Russo MT, Tambone V (eds) Cosm-Etica. Chirurgia estetica, corpo e bellezza. McGraw-Hill, Milano, pp 5–38
Di Stefano N (2014) Verso l’indifferenziato: rimozione del limite e perdita dell’identità. Chirurgia estetica, gender e transumanesimo. In: Pagliacci D (ed) Differenze e Relazioni. Aracne, Roma, pp 235–244
http://www.dsm5.org/documents/gender%20dysphoria%20fact%20sheet.pdf
Coleman E, Bockting W, Botzer M et al (2012) Standards of care for the health of transsexual, transgender, and gender-nonconforming people, Version 7. Int J Transgend 13:67
Barone M, Cogliandro A, La Monaca G, Tambone V, Persichetti P (2015) Cognitive investigation study of patients admitted for cosmetic surgery: information, expectations, and consent for treatment. Arch Plast Surg 42:46–51
Lasch KE, Marquis P, Vigneux M, Abetz L, Arnould B, Bayliss M, Crawford B, Rosa K (2010) PRO development: rigorous qualitative research as the crucial foundation. Qual Life Res 19:1087–1096
Klassen AF, Cano SJ, East CA, Baker SB, Badia L, Schwitzer JA, Pusic AL (2016) Development and Psychometric Evaluation of the FACE-Q Scales for patients undergoing rhinoplasty. JAMA Facial Plast Surg 18:27–35
Pusic AL, Chen CM, Cano S, Klassen A, McCarthy C, Collins ED, Cordeiro PG (2007) Measuring quality of life in cosmetic and reconstructive breast surgery: a systematic review of patient-reported outcomes instruments. Plast Reconstr Surg 120:823–837
Barone M, Cogliandro A, Di Stefano N, Tambone V, Persichetti P (2016) A systematic review of patient-reported outcome measures after rhinoplasty. Eur Arch Otorhinolaryngol Oct 31. [Epub ahead of print]
U.S. Food and Drug Administration (2006) Guidance for industry. patient-reported outcome measures: use in medical product development to support labeling claims. FDA web site. http://www.fda.gov/cder/guidance/index
Lohr KN (2002) Assessing health status and quality-of-life instruments: attributes and review criteria. Qual Life Res 11:193–205
Brown TA, Cash TF, Mikulka PJ (1990) Attitudinal body-image assessment: factor analysis of the Body-Self Relations Questionnaire. J Personal Assess 55:135–144
Cash TF, Melnyk SE, Hrabosky JI (2004) The assessment of body image investment: an extensive revision of the Appearance Schemas Inventory. Int J Eat Disord 35:305–316
Cash TF, Fleming EC (2002) The impact of body-image experiences: development of the Body Image Quality of Life Inventory. Int J Eat Disord 31:455–460
Rosenberg M (1965) Society and the adolescent self-image. Princeton University Press, Princeton
Lyubomirsky S, Lepper HS (1999) A measure of subjective happiness: preliminary reliability and construct validation. Soc Indic Res 46:137–155
Diener E, Emmons RA, Larsen RJ (1985) The Satisfaction With Life Scale. J Personal Assess 49:71–75
Cantril H (1965) The patterns of human concerns. Rutgers University Press, New Brunswick
Bjelic-Radisic V, Dorfer M, Tamussino K, Greimel E (2005) Psychometric properties and validation of the German-language King’s Health Questionnaire in women with stress urinary incontinence. Neurourol Urodyn 24:63–68
Ware JE, Snow KK, Kosinski M, Gandek B (1993) SF-36 Health Survey Manual and Interpretation Guide. The Health Institute, Boston
Andrews G, Singh M, Bond M (1993) The Defense Style Questionnaire. J Nerv Ment Dis 181:246–256
Rosen R, Brown C, Heiman J, Leiblum S, Meston C, Shabsigh R, Ferguson D, D’Agostino R Jr (2000) The Female Sexual Function Index (FSFI): a multidimensional self-report instrument for the assessment of female sexual function. J Sex Marital Ther 26:191–208
Herbenick D, Reece M (2010) Development and validation of the female genital self-image scale. J Sex Med 7:1822–1830
Postma R, Bicanic I, van der Vaart H, Laan E (2013) Pelvic floor muscle problems mediate sexual problems in young adult rape victims. J Sex Med 10:1978–1987
van der Sluis WB, Bouman MB, de Boer NK, Buncamper ME, van Bodegraven AA, Neefjes-Borst EA, Kreukels BP, Meijerink WJ, Mullender MG (2016) Long-term follow-up of transgender women after secondary intestinal vaginoplasty. J Sex Med 13:702–710
Lindgren TW, Pauly IB (1975) A body image scale for evaluating transsexuals. Arch Sex Behav 4:639–656
Cash TF (2002) The situational inventory of body-image dysphoria: psychometric evidence and development of a short form. Int J Eat Disord 32:362–366
Pusic AL, Klassen AF, Scott AM, Klok JA, Cordeiro PG, Cano SJ (2009) Development of a new patient-reported outcome measure for breast surgery: the BREAST-Q. Plast Reconstr Surg 124:345–353
Kanhai RC, Hage JJ, Mulder JW (2000) Long-term outcome of augmentation mammaplasty in male-to-female transsexuals: a questionnaire survey of 107 patients. Br J Plast Surg 53:209–211
Nelson L, Whallett EJ, McGregor JC (2009) Transgender patient satisfaction following reduction mammaplasty. J Plast Reconstr Aesthet Surg 62:331–334
Weigert R, Frison E, Sessiecq Q, Al Mutairi K, Casoli V (2013) Patient satisfaction with breasts and psychosocial, sexual, and physical well-being after breast augmentation in male-to-female transsexuals. Plast Reconstr Surg 132:1421–1429
Antoszewski B, Bratoś R, Sitek A, Fijałkowska M (2012) Long-term results of breast reduction in female-to-male transsexuals. Pol Przegl Chir 84:144–151
van de Grift TC, Kreukels BP, Elfering L, Özer M, Bouman MB, Buncamper ME, Smit JM, Mullender MG (2016) Body image in transmen: multidimensional measurement and the effects of mastectomy. J Sex Med 13:1778–1786
Capitán L, Simon D, Kaye K, Tenorio T (2014) Facial feminization surgery: the forehead. Surgical techniques and analysis of results. Plast Reconstr Surg 134:609–619
Pavlidis L, Spyropoulou GA, Dionyssiou D, Demiri E (2016) Full facial feminization surgery: patient satisfaction assessment based on 180 procedures involving 33 consecutive patients. Plast Reconstr Surg 138:765–766
Bouman MB, van der Sluis WB, van Woudenberg Hamstra LE, Buncamper ME, Kreukels BP, Meijerink WJ, Mullender MG (2016) Patient-reported esthetic and functional outcomes of primary total laparoscopic intestinal vaginoplasty in transgender women with penoscrotal hypoplasia. J Sex Med 13:1438–1444
Wierckx K, Van Caenegem E, Elaut E, Dedecker D, Van de Peer F, Toye K, Weyers S, Hoebeke P, Monstrey S, De Cuypere G, T’Sjoen G (2011) Quality of life and sexual health after sex reassignment surgery in transsexual men. J Sex Med 8:3379–3388
Kuhn A, Bodmer C, Stadlmayr W, Kuhn P, Mueller MD, Birkhäuser M (2009) Quality of life 15 years after sex reassignment surgery for transsexualism. Fertil Steril 92:1685–1689
Newfield E, Hart S, Dibble S, Kohler L (2006) Female-to-male transgender quality of life. Qual Life Res 15:1447–1457
Rehman J, Lazer S, Benet AE, Schaefer LC, Melman A (1999) The reported sex and surgery satisfactions of 28 postoperative male-to-female transsexual patients. Arch Sex Behav 28:71–89
Lawrence AA (2003) Factors associated with satisfaction or regret following male-to-female sex reassignment surgery. Arch Sex Behav 32:299–315
McGuire JK, Doty JL, Catalpa JM, Ola C (2016) Body image in transgender young people: findings from a qualitative, community based study. Body Image 18:96–107
Lobato MI, Koff WJ, Crestana T, Chaves C, Salvador J, Petry AR, Silveira E, Henriques AA, Cervo F, Böhme ES, Massuda R (2009) Using the Defensive Style Questionnaire to evaluate the impact of sex reassignment surgery on defensive mechanisms in transsexual patients. Rev Bras Psiquiatr 31:303–306
Jokić-Begić N, Lauri Korajlija A, Jurin T (2014) Psychosocial adjustment to sex reassignment surgery: a qualitative examination and personal experiences of six transsexual persons in croatia. ScientificWorld Journal 25:2014
Melloni C, Melloni G, Rossi M, Rolle L, Carmisciano M, Timpano M, Falcone M, Frea B, Cordova A (2016) Lower urinary tract symptoms in male-to-female transsexuals: short terms results and proposal of a new questionnaire. Plast Reconstr Surg Globe Open 18(4):655
Patrick DL, Burke LB, Powers JH, Scott JA, Rock EP, Dawisha S, O’Neill R, Kennedy DL (2007) Patient reported outcomes to support medical product labelling claims: FDA perspective. Value Health 10:S125–S137
Cagli B, Cogliandro A, Barone M, Persichetti P (2014) Quality-of-life outcomes between mastectomy alone and breast reconstruction: comparison of patient-reported BREAST-Q and other health-related quality-of-life measures. Plast Reconstr Surg 133:594–595
Klassen AF, Cano SJ, Scott A, Snell L, Pusic AL (2010) Measuring patient-reported outcomes in facial aesthetic patients: development of the FACE-Q. Facial Plast Surg 26:303–309
Cohen WA, Mundy LR, Ballard TN, Klassen A, Cano SJ, Browne J, Pusic AL (2016) The BREAST-Q in surgical research: a review of the literature 2009–2015. J Plast Reconstr Aesthet Surg 69:149–162
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflicts of interest to disclose.
Ethical Approval
“All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.”
Rights and permissions
About this article
Cite this article
Barone, M., Cogliandro, A., Di Stefano, N. et al. A Systematic Review of Patient-Reported Outcome Measures Following Transsexual Surgery. Aesth Plast Surg 41, 700–713 (2017). https://doi.org/10.1007/s00266-017-0812-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00266-017-0812-4