Abstract
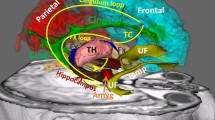
Pain perception can be altered by activity in the periaqueductal gray (PAG). The PAG can decrease the incoming nociceptive signals at the level of the spinal dorsal horn, but it is not clear whether the PAG can also affect the sensory thalamus, ventral posterolateral and ventral posteromedial thalamic nuclei, to modulate pain. However, the PAG and the thalamus have direct connections with each other; so we postulated that the PAG may also modulate pain by inhibiting the sensory nuclei in the thalamus, and that these may also reciprocally influence the PAG. Here, by analyzing the local field potentials recorded from the sensory thalamus and the PAG in chronic pain patients with deep brain stimulation electrodes, we show that PAG stimulation inhibited the sensory thalamus with decreasing thalamic delta, theta, alpha and beta power, and sensory thalamus stimulation excited the PAG with increasing PAG delta and theta power. We demonstrate that the PAG and the sensory thalamus interact reciprocally at short latency, which may be related to pain modulation.


Similar content being viewed by others
References
Bandler R, Shipley MT (1994) Columnar organization in the midbrain periaqueductal gray—modules for emotional expression. Trends Neurosci 17:379–389. doi:10.1016/0166-2236(94)90047-7
Bandler R, Keay KA, Floyd N, Price J (2000) Central circuits mediating patterned autonomic activity during active vs. passive emotional coping. Brain Res Bull 53:95–104. doi:10.1016/s0361-9230(00)00313-0
Basbaum AI, Fields HL (1984) Endogenous pain control systems: brainstem spinal pathways and endorphin circuitry. Annu Rev Neurosci 7:309–338. doi:10.1146/annurev.neuro.7.1.309
Benarroch EE (2012) Periaqueductal gray: an interface for behavioral control. Neurology 78:210–217
Bittar RG, Burn SC, Bain PG, Owen SL, Joint C, Shlugman D, Aziz TZ (2005a) Deep brain stimulation for movement disorders and pain. J Clin Neurosci 12:457–463. doi:10.1016/j.jocn.2004.09.001
Bittar RG, Kar-Purkayastha I, Owen SL, Bear RE, Green A, Wang SY, Aziz TZ (2005b) Deep brain stimulation for pain relief: a meta-analysis. J Clin Neurosci 12:515–519. doi:10.1016/j.jocn.2004.10.005
Boccard SG Pereira EA, Moir L, Aziz TZ, Green AL (2013) Long-term outcomes of deep brain stimulation for neuropathic pain. Neurosurgery 72(2):221–230
Budai D, Harasawa I, Fields HL (1998) Midbrain periaqueductal gray (PAG) inhibits nociceptive inputs to sacral dorsal horn nociceptive neurons through alpha(2)-adrenergic receptors. J Neurophysiol 80:2244–2254
Craig AD (2002) How do you feel? Interoception: the sense of the physiological condition of the body. Nat Rev Neurosci 3:655–666. doi:10.1038/nrn894
Craig ADB (2003) A new view of pain as a homeostatic emotion. Trends Neurosci 26:303–307. doi:10.1016/s0166-2236(03)00123-1
Cruccu G, Iannetti GD, Agostino R, Romaniello A, Truini A, Manfredi M (2000) Conduction velocity of the human spinothalamic tract as assessed by laser evoked potentials. Neuroreport 11:3029–3032. doi:10.1097/00001756-200009110-00040
Denker M, Roux S, Linden H, Diesmann M, Riehle A, Grun S (2011) The local field potential reflects surplus spike synchrony. Cereb Cortex 21:2681–2695. doi:10.1093/cercor/bhr040
Green AL, Wang SY, Owen SLF et al (2005) Deep brain stimulation can regulate arterial blood pressure in awake humans. Neuroreport 16:1741–1745. doi:10.1097/01.wnr.0000183904.15773.47
Green AL, Wang SY, Owen SLF, Paterson DJ, Stein JF, Aziz TZ (2006a) Controlling the heart via the brain: a potential new therapy for orthostatic hypotension. Neurosurgery 58:1176–1182. doi:10.1227/01.neu.0000215943.78685.01
Green AL, Wang SY, Owen SLF et al (2006b) Stimulating the human midbrain to reveal the link between pain and blood pressure. Pain 124:349–359
Hadjipavlou G, Dunckley P, Behrens TE, Tracey I (2006) Determining anatomical connectivities between cortical and brainstem pain processing regions in humans: a diffusion tensor imaging study in healthy controls. Pain 123:169–178. doi:10.1016/j.pain.2006.02.027
Heinricher MM, Tavares I, Leith JL, Lumb BM (2009) Descending control of nociception: specificity, recruitment and plasticity. Brain Res Rev 60:214–225. doi:10.1016/j.brainresrev.2008.12.009
Hosobuchi Y, Adams JE, Linchitz R (1977) Pain relief by electrical stimulation of central gray matter in humans and its reversal by naloxone. Science 197:183–186. doi:10.1126/science.301658
Hyam JA, Kringelbach ML, Silburn PA, Aziz TZ, Green AL (2012) The autonomic effects of deep brain stimulation—a therapeutic opportunity. Nat Rev Neurol 8:391–400. doi:10.1038/nrneurol.2012.100
Knyazev GG (2012) EEG delta oscillations as a correlate of basic homeostatic and motivational processes. Neurosci Biobehav Rev 36:677–695. doi:10.1016/j.neubiorev.2011.10.002
Krout KE, Loewy AD (2000) Periaqueductal gray matter projections to midline and intralaminar thalamic nuclei of the rat. J Comp Neurol 424:111–141. doi:10.1002/1096-9861(20000814)424:1<111:aid-cne9>3.0.co;2-3
Lenz FA, Kwan HC, Dostrovsky JO, Tasker RR (1989) Characteristics of the bursting pattern of action-potentials that occurs in the thalamus of patients with central pain. Brain Res 496:357–360. doi:10.1016/0006-8993(89)91088-3
Lenz FA, Kwan HC, Martin R, Tasker R, Richardson RT, Dostrovsky JO (1994) Characteristics of somatotopic organization and spontaneous neuronal activity in the region of the thalamic principal sensory nucleus in patients with spinal cord transection. J Neurophysiol 72:1570–1587
Levy R, Deer TR, Henderson J (2010) Intracranial neurostimulation for pain control: a review. Pain Physician 13:157–165
Linnman C, Moulton EA, Barmettler G, Becerra L, Borsook D (2012) Neuroimaging of the periaqueductal gray: state of the field. Neuroimage 60:505–522. doi:10.1016/j.neuroimage.2011.11.095
Mantyh PW (1983) Connections of midbrain periaqueductal gray in the monkey. 1. Ascending efferent projections. J Neurophysiol 49:567–581
Millan MJ (2002) Descending control of pain. Prog Neurobiol 66:355–474
Montgomery EB, Gale JT (2008) Mechanism of action of deep brain stimulation (DBS). Neurosci Biobehav Rev 32:388–407
Nandi D, Liu XG, Joint C, Stein J, Aziz T (2002) Thalamic field potentials during deep brain stimulation of periventricular gray in chronic pain. Pain 97:47–51. doi:10.1016/s0304-3959(01)00486-9
Nandi D, Aziz T, Carter H, Stein J (2003) Thalamic field potentials in chronic central pain treated by periventricular gray stimulation—a series of eight cases. Pain 101:97–107. doi:10.1016/s0304-3959(02)00277-4
Pereira EAC, Green AL, Bradley KM, Soper N, Moir L, Stein JF, Aziz TZ (2007) Regional cerebral perfusion differences between periventricular grey, thalamic and dual target deep brain stimulation for chronic neuropathic pain. Stereotact Funct Neurosurg 85:175–183. doi:10.1159/000101296
Reynolds DV (1969) Surgery in rat during electrical analgesia induced by focal brain stimulation. Science 164:444–445. doi:10.1126/science.164.3878.444
Richardson DE, Akil H (1977a) Pain reduction by electrical brain-stimulation in man. 1. Acute administration in periaqueductal and periventricular sites. J Neurosurg 47:178–183. doi:10.3171/jns.1977.47.2.0178
Richardson DE, Akil H (1977b) Pain reduction by electrical brain-stimulation in man. 2. Chronic self-administration in periventricular gray-matter. J Neurosurg 47:184–194. doi:10.3171/jns.1977.47.2.0184
Rinvik E, Wiberg M (1990) Demonstration of a reciprocal connection between the periaqueductal gray matter and the reticular nucleus of the thalamus. Anat Embryol 181:577–584
Roberts VJ, Dong WK (1994) The effect of thalamic nucleus submedius lesions on nociceptive responding in rats. Pain 57:341–349. doi:10.1016/0304-3959(94)90010-8
Rossi P, Serrao M, Amabile G, Parisi L, Pierelli F, Pozzessere G (2000) A simple method for estimating conduction velocity of the spinothalamic tract in healthy humans. Clin Neurophysiol 111:1907–1915. doi:10.1016/s1388-2457(00)00442-9
Sillery E, Bittar RG, Robson MD, Behrens TEJ, Stein J, Aziz TZ, Johansen-Berg H (2005) Connectivity of the human periventricular–periaqueductal gray region. J Neurosurg 103:1030–1034. doi:10.3171/jns.2005.103.6.1030
Tang J-S, Qu C-L, Huo F-Q (2009) The thalamic nucleus submedius and ventrolateral orbital cortex are involved in nociceptive modulation: a novel pain modulation pathway. Prog Neurobiol (Oxford) 89:383–389. doi::10.1016/j.pneurobio.2009.10.002
Tran TD, Inui K, Hoshiyama M, Lam K, Kakigi R (2002) Conduction velocity of the spinothalamic tract following CO(2) laser stimulation of C-fibers in humans. Pain 95:125–131. doi:10.1016/s0304-3959(01)00386-4
Xie KN, Wang SY, Aziz TZ, Stein JF, Liu XG (2006) The physiologically modulated electrode potentials at the depth electrode-brain interface in humans. Neurosci Lett 402:238–243. doi:10.1016/j.neulet.2006.04.015
Acknowledgments
This work was supported by educational grants from the Oxford Biomedical Research Centre of the UK National Institute for Health and Research, the Charles Wolfson Charitable Trust and the Norman Collisson Foundation. The authors thank Professor Peter Brown for his critical review of the manuscript.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Wu, D., Wang, S., Stein, J.F. et al. Reciprocal interactions between the human thalamus and periaqueductal gray may be important for pain perception. Exp Brain Res 232, 527–534 (2014). https://doi.org/10.1007/s00221-013-3761-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00221-013-3761-4