Abstract
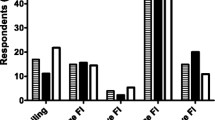
The aim of this study was to evaluate the prevalence of urinary, fecal and double incontinence in the elderly, through a population-based cross-sectional survey. The study included all patients aged 60 and over of nine general practices in the Nijmegen Monitoring Project. Patients living in a home for the elderly were excluded, as well as patients with dementia, patients who were too ill to participate and patients with a catheter. There were 5278 selected patients who received a postal questionnaire. Of these, 88% returned it. Nineteen percent of the respondents had involuntary loss of urine twice a month or more, 6% loss of feces and 3% both. The prevalence of urinary, fecal and double incontinence increased with age in both men and women, and especially in men in the oldest age group. Urinary incontinence was more prevalent in women than in men. The prevalence of fecal incontinence showed no sex differences, but the type of fecal incontinence did differ between men and women. In men loss of mucus was twice as common as in women. Double incontinence was also equally prevalent in men and women, except in the age group 65–74 years. In conclusion, urinary, fecal and double incontinence are common conditions in the community-dwelling population. The prevalence rates increase with age. Urinary incontinence is more prevalent in women. There were no sex differences in the prevalence of fecal incontinence but the type of fecal incontinence was different in men and women.
Similar content being viewed by others
Abbreviations
- FI:
-
Fecal incontinence
- UI:
-
Urinary incontinence
References
Robinson D, Pearce KF, Preisser JS, Dugan E, Suggs PK, Cohen SJ (1998) Relationship between patient reports of urinary incontinence symptoms and quality of life measures. Obstet Gynecol 91:224–228
Simeonova Z, Milsom I, Kullendorff AM, Molander U, Bengtsson C (1999) The prevalence of urinary incontinence and its influence on the quality of life in women from an urban Swedish population. Acta Obstet Gynecol Scand 78:546–551
Valk M (1999) Urinary incontinence in psychogeriatric nursing home patients. Conceps, causes and prevalence. A literature overview [dissertation]. University of Utercht,Utrecht
Felt-Bersma RJ, Cuesta MA (1994) Faecal incontinence 1994: which test and which treatment? Neth J Med 44:182–188
Johanson JF, Lafferty J (1996) Epidemiology of fecal incontinence: the silent affliction. Am Gastroenterol 91:33–36
Brocklehurst JC (1993) Urinary incontinence in the community--analysis of a MORI poll. Br Med J 306:832–834
Nygaard IE, Lemke JH (1996) Urinary incontinence in rural older women: prevalence, incidence and remission. J Am Geriatr.Soc 44:1049–1054
Branch LG, Walker LA, Wetle TT, DuBeau CE, Resnick NM (1994) Urinary incontinence knowledge among community-dwelling people 65 years of age and older. J Am Geriatr Soc 42:1257–1262
Damian J, Martin-Moreno JM, Lobo F et al. (1998) Prevalence of urinary incontinence among Spanish older people living at home. Eur Urol 34:333–338
Diokno AC, Brock BM, Brown MB, Herzog AR (1986) Prevalence of urinary incontinence and other urological symptoms in the noninstitutionalized elderly. J Urol 36:1022–1025
Jitapunkul S, Khovidhunkit W (1998) Urinary incontinence in Thai elderly living in Klong Toey slum. J Med Assoc Thai 81:160–168
Kok AL, Voorhorst FJ, Burger CW, van Houten P, Kenemans P, Janssens J (1992) Urinary and faecal incontinence in community-residing elderly women. Age Aging 21:211–215
Maggi S, Minicuci N, Langlois J, Pavan M, Enzi G, Crepaldi G (2001) Prevalence rate of urinary incontinence in community-dwelling elderly individuals: the Veneto study. J Gerontol A Biol Sci Med Sci 56:M14–M18
Molander U (1993) Urinary incontinence and related urogenital symptoms in elderly women. Acta Obstet Gynecol Scand.(Suppl):1581–1522
Teasdale TA, Taffet GE, Luchi RJ, Adam E (1988) Urinary incontinence in a community-residing elderly population. J Am Geriatr Soc 36:600–606
Thomas TM, Plymat KR, Blannin J, Meade TW (1980) Prevalence of urinary incontinence. Br Med J 281:1243–1245
Tseng IJ, Chen YT, Chen MT, Kou HY, Tseng SF (2000) Prevalence of urinary incontinence and intention to seek treatment in the elderly. J Formos Med Assoc 99:753–758
Vetter NJ, Jones DA, Victor CR (1981) Urinary incontinence in the elderly at home. Lancet 2:1275–1277
Nakanishi N, Tatara K, Naramura H, Fujiwara H, Takashima Y, Fukuda H (1997) Urinary and fecal incontinence in a community-residing older population in Japan. J Am Geriatr Soc 45:215–219
Talley NJ, O’Keefe EA, Zinsmeister AR, Melton LJ (1992) Prevalence of gastrointestinal symptoms in the elderly: a population-based study. Gastroenterology 102:895–901
Thomas TM, Egan M, Walgrove A, Meade TW (1984) The prevalence of faecal and double incontinence. Community Med 6:216–220
Baigis-Smith J, Smith DA, Rose M, Newman DK (1989) Managing urinary incontinence in community-residing elderly persons. Gerontologist 29:229–233
Burgio KL, Engel BT(1990) Biofeedback-assisted behavioral training for elderly men and women. J Am Geriatr Soc 38:338–340
Fantl JA, Wyman JF, McClish DK et al. (1991) Efficacy of bladder training in older women with urinary incontinence. JAMA 265:609–613
Molander U, Milsom I, Ekelund P, Arvidsson L, Eriksson O (1991) A health care program for the investigation and treatment of elderly women with urinary incontinence and related urogenital symptoms. Acta Obstet Gynecol Scand 70:137–142
Norton PA, MacDonald LD, Sedgwick PM, Stanton SL (1988) Distress and delay associated with urinary incontinence, frequency, and urgency in women. Br Med J 297:1187–1189
van Weel C, Smith H, Beasley JW (2000) Family practice research networks. Experiences from 3 countries. J Fam Pract 49:938–943
Lagro-Janssen AL, Smith H, Breedveldt Boer HP, van Dongen JJ (1995) NHG-Standaard: Incontinentie voor Urine [Dutch College Guidelines on Urinary Incontinence]. Huisarts Wet 38:71–80
Author information
Authors and Affiliations
Corresponding author
Additional information
Editorial Comment: This large population-based survey looked at the prevalence of urinary, fecal, and double incontinence in women and men in the Netherlands. The fact that the authors were able to get an 88% return on their questionnaire demonstrates the utility of having primary care physicians involved in gaining pertinent information from patients. The response rate for specialists attempting such surveys on their own is grossly inferior to what these authors were able to accomplish. Although there was a higher prevalence of urinary incontinence in women, there was no difference between men and women in the prevalence of fecal incontinence. More studies like this are needed to establish prevalence data for pelvic floor dysfunction in general.
An erratum to this article can be found at http://dx.doi.org/10.1007/s00192-003-1047-2
Rights and permissions
About this article
Cite this article
Teunissen, T.A.M., Lagro-Janssen, A.L.M., van den Bosch, W.J.H.M. et al. Prevalence of urinary, fecal and double incontinence in the elderly living at home. Int Urogynecol J 15, 10–13 (2004). https://doi.org/10.1007/s00192-003-1106-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00192-003-1106-8