Abstract
Background
A recent national survey in South Korea indicated that the 12-month prevalence rate of major depressive disorder was 2.5%. Depressive disorders may lead to disability, premature death, and severe suffering of patients and their families. This study estimates the economic burden of depression in Korea from a societal perspective.
Methods
Annual direct healthcare costs associated with depression were calculated based on the National Health Insurance database. Annual direct non-healthcare costs were estimated for transport. Annual indirect costs were estimated for the following components of productivity loss due to illness such as morbidity (absenteeism and presenteeism) and premature mortality. Indirect costs were estimated using the large national psychiatric epidemiological surveys in Korea. The human capital approach was used to estimate indirect costs.
Result
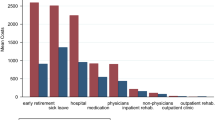
The total cost of depression was estimated to be $4,049 million, of which $152.6 million represents a direct healthcare cost. Total direct non-healthcare costs were estimated to be $15.9 million. Indirect costs were estimated at $3,880.5 million. The morbidity cost was $2,958.9 million and the mortality cost was $921.6 million. The morbidity cost was identified as the largest component of overall cost.
Conclusion
Depression is a considerable burden on both society and the individual, especially in terms of incapacity to work. The Korean society should increase the public health effort to prevent and detect depression in order to ensure that appropriate treatment is provided. Such actions will lead to a significant reduction in the total burden resulting from depression.
Similar content being viewed by others
References
Murray CJL, Lopez AD (1996) Alternative visions of the future: projecting mortality and disability, 1990–2020. Published by the Harvard School of Public Health on behalf of the World Health Organization and the World Bank; Distributed by Harvard University Press, Cambridge
Cassano P, Fava M (2002) Depression and public health: an overview. J Psychosom Res; 53(4):849–857
Kessler RC, Walters EE, Forthofer MS (1998) The social consequences of psychiatric disorders, III: probability of marital stability. Am J Psychiatry 155(8):1092–1096
Cho MJ, Kim JK, Jeon HJ, Suh T, Chung IW, Hong JP, Bae JN, Lee DW, Park JI, Cho SJ, Lee CK, Hahm BJ (2007) Lifetime and 12-month prevalence of DSM-IV psychiatric disorders among Korean adults. J Nerv Ment Dis 195(3):203–210
Cho MJ, Chang SM, Hahm BJ, Chung IW, Bae A, Lee YM, Ahn JH, Won SH, Son JW, Hong JP, Bae JN, Lee DW, Cho SJ, Park JI, Lee JY, Kim JY, Jeon HJ, Lee HW (2009) Prevalence and correlates of major mental disorders among Korean adults: a 2006 National Epidemiologic Survey. J Korean Neuropsychiatr Assoc 48:143–152
Korean National Statistical Office: annual report on the cause of death statistics. Daejon, Korean National Stastical Office (2008)
Thomas CM, Morris S (2003) Cost of depression among adults in England in 2000. Br J Psychiatry 183:514–519
Berto P, D’Ilario D, Ruffo P, Di Virgilio R, Rizzo F (2000) Depression: cost-of-illness studies in the international literature, a review. J Ment Health Policy Econ 3(1):3–10
Hu TW, He Y, Zhang M, Chen N (2007) Economic costs of depression in China. Soc Psychiatry Psychiatr Epidemiol 42(2):110–116
Luppa M, Heinrich S, Angermeyer MC, Konig HH, Riedel-Heller SG (2007) Cost-of-illness studies of depression: a systematic review. J Affect Disord 98(1–2):29–43
National Health Insurance Corporation (2005) Statistical information system, in 2009 April, National Health Insurance Corporation. http://www.nhic.or.kr/
Song YJ (2009) The South Korean health care system. JMAJ 52(3):206–209
Chang SM, Cho SJ, Jeon HJ, Hahm BJ, Lee HJ, Park JI, Cho MJ (2008) Economic burden of schizophrenia in South Korea. J Korean Med Sci 23(2):167–175
Greenberg PE, Kessler RC, Birnbaum HG, Leong SA, Lowe SW, Berglund PA, Corey-Lisle PK (2003) The economic burden of depression in the United States: how did it change between 1990 and 2000? J Clin Psychiatry 64(12):1465–1475
Sohn JH, Cho MJ, Lee JY, Choi JH, Lee HW, Jeon HJ, Hahm BJ, Chang SM (2008) Impact of mental disorders on functional disability: effect of non-psychotic common mental disorders on work loss days. J Korean Neuropsychiatr Assoc 47(1):81–87
Kim W, Tae-Yeun H, Byoung-Joo H, Joon-Seok L, Byung-Hwi C, Se Joo K, Yong-Jin S, Eun-Ho K, Jong-Min W (2007) The impact of major depressive disorder on productivity in workers:a preliminary study using WHO-HPQ (Health and Work Performance Questionnaire). J Korean Neuropsychiatr Assoc; 46(6):587–595
Labor Statistics of Korea (2005) Survey report on wage structure, in 2009 April, Ministry of Labor. http://laborstat.molab.go.kr
Cho MJ, Nam JJ, Suh GH (1998) Prevalence of symptoms of depression in a nationwide sample of Korean adults. Psychiatry Res 81(3):341–352
Sobocki P, Jonsson B, Angst J, Rehnberg C (2006) Cost of depression in Europe. J Ment Health Policy Econ 9(2):87–98
Korean Ministry of Health & Welfare, Seoul National University: The epidemiological survey of psychiatric illness in Korea 2006, Korean Ministry of Health & Welfare, 2007, pp 317–321
Kind P, Sorensen J (1993) The costs of depression. Int Clin Psychopharmacol 7(3–4):191–195
Hawthorne G, Cheok F, Goldney R, Fisher L (2003) The excess cost of depression in South Australia: a population-based study. Aust N Z J Psychiatry 37(3):362–373
Chan AL, Yang TC, Chen JX, Yu LH, Leung HW (2006) Cost of depression of adults in Taiwan. Int J Psychiatry Med 36(1):131–135
Stewart WF, Ricci JA, Chee E, Hahn SR, Morganstein D (2003) Cost of lost productive work time among US workers with depression. Jama 289(23):3135–3144
Stewart WF, Ricci JA, Chee E, Morganstein D (2003) Lost productive work time costs from health conditions in the United States: results from the American Productivity Audit. J Occup Environ Med 45(12):1234–1246
Katzelnick DJ, Kobak KA, Greist JH, Jefferson JW, Henk HJ (1997) Effect of primary care treatment of depression on service use by patients with high medical expenditures. Psychiatr Serv 48(1):59–64
Rupp A (1995) The economic consequences of not treating depression. Br J Psychiatry 27(Suppl):29–33
Rutz W, Carlsson P, von Knorring L, Walinder J (1992) Cost-benefit analysis of an educational program for general practitioners by the Swedish Committee for the Prevention and Treatment of Depression. Acta Psychiatr Scand 85(6):457–464
Simon GE, Revicki D, Heiligenstein J, Grothaus L, VonKorff M, Katon WJ, Hylan TR (2000) Recovery from depression, work productivity, and health care costs among primary care patients. Gen Hosp Psychiatry 22(3):153–162
van den Hout WB (2010) The value of productivity: human-capital versus friction-cost method. Ann Rheum Dis 69 (Suppl 1):i89–i91
Spitzer RL, Williams JB, Kroenke K, Linzer M, deGruy FV, Hahn SR 3rd, Brody D, Johnson JG (1994) Utility of a new procedure for diagnosing mental disorders in primary care. The PRIME-MD 1000 study. Jama 272(22):1749–1756
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Chang, S.M., Hong, JP. & Cho, M.J. Economic burden of depression in South Korea. Soc Psychiatry Psychiatr Epidemiol 47, 683–689 (2012). https://doi.org/10.1007/s00127-011-0382-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00127-011-0382-8