Abstract
Purpose
To investigate the impact of Mindfulness-Based Stress Reduction (MBSR) on gray matter volume (GMV) in female breast cancer survivors who suffer from chronic neuropathic pain (CNP).
Methods
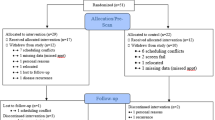
Voxel-based morphometry (VBM) was used to explore differences in GMV in 13 MBSR trainees and 10 waitlisted controls, with MRI scans and self-report measures completed pre- and post-8 weeks of training.
Results
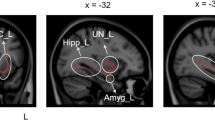
Compared to controls, the MBSR group had greater GMV in the angular gyrus and middle frontal gyrus post-training. The MBSR group’s right parahippocampal gyrus GMV increased from pre- to post-training, whereas the control group’s left parahippocampal gyrus, precuneus, middle temporal gyrus, and right cuneus GMV decreased over the same time period. Pain interference was significantly reduced and mindfulness was significantly increased following MBSR for the intervention group only.
Conclusions
MBSR was associated with increased GMV in regions where GMV is known to (1) increase with mindfulness and reorientation of attention and (2) decrease with the experience of chronic neuropathic pain. By contrast, the control group’s decreases in GMV may be due to the negative effects of CNP which potentially may be reduced with MBSR, though further research is needed.
Implications for cancer survivors
Given the poor efficiency of pharmacotherapies in a high percentage of women with neuropathic pain following breast cancer treatment, adjunct methods are required. MBSR may affect the brain to help alter attention and perception of pain, thus playing a potentially important role in the path to wellness for breast cancer survivors.


Similar content being viewed by others
Availability of data and material
The data that support the findings of this study are available from the corresponding author upon reasonable request.
Code availability
Not applicable.
References
Canadian Cancer Statistics Advisory Committee (2018) Canadian cancer statistics 2018. Canadian Cancer Society, Toronto, pp 12–13
Burton R, Stevenson C (2020) Assessment of breast cancer mortality trends associated with mammographic screening and adjuvant therapy from 1986 to 2013 in the state of Victoria. Australia JAMA Netw Open 3:e208249. https://doi.org/10.1001/jamanetworkopen.2020.8249
Hendrick RE, Baker JA, Helvie MA (2019) Breast cancer deaths averted over 3 decades. Cancer 125:1482–1488. https://doi.org/10.1002/cncr.31954
Berry DA, Cronin KA, Plevritis SK, Fryback DG, Clarke L, Zelen M, Mandelblatt JS, Yakovlev AY, Habbema JD, Feuer EJ (2005) Effect of screening and adjuvant therapy on mortality from breast cancer. N Engl J Med 353:1784–1792. https://doi.org/10.1056/NEJMoa050518
Bredal IS, Smeby NA, Ottesen S, Warncke T, Schlichting E (2014) Chronic pain in breast cancer survivors: comparison of psychosocial, surgical, and medical characteristics between survivors with and without pain. J Pain Symptom Manage 48:852–862. https://doi.org/10.1016/j.jpainsymman.2013.12.239
Bouhassira D, Attal N, Fermanian J, Alchaar H, Gautron M, Masquelier E, Rostaing S, Lanteri-Minet M, Collin E, Grisart J, Boureau F (2004) Development and validation of the neuropathic pain symptom inventory. Pain 108:248–257. https://doi.org/10.1016/j.pain.2003.12.024
Jung BF, Ahrendt GM, Oaklander AL, Dworkin RH (2003) Neuropathic pain following breast cancer surgery: proposed classification and research update. Pain 104:1–3. https://doi.org/10.1016/S0304-3959(03)00241-0
Otto J, Forstenpointner J, Binder A, Baron R (2019) Pharmacotherapy of chronic neuropathic pain. Internist (Berl). 60:711–723. https://doi.org/10.1007/s00108-019-0627-2
Renna ME, Shrout MR, Madison AA, Lustberg M, Povoski SP, Agnese DM, Reinbolt RE, Wesolowski R, Williams NO, Ramaswamy B, Sardesai SD (2021) Worry and rumination in breast cancer patients: perseveration worsens self-rated health. J Behav Med 44:253–259. https://doi.org/10.1007/s10865-020-00192-9
Vahdaninia M, Omidvari S, Montazeri A (2010) What do predict anxiety and depression in breast cancer patients? A follow-up study. Soc Psychiatry Psychiatr Epidemiol 45:355–361. https://doi.org/10.1007/s00127-009-0068-7
Lerman SF, Rudich Z, Brill S, Shalev H, Shahar G (2015) Longitudinal associations between depression, anxiety, pain, and pain-related disability in chronic pain patients. Psychosom Med 77:333–341. https://doi.org/10.1097/PSY.0000000000000158
Kawai K, Kawai AT, Wollan P, Yawn BP (2017) Adverse impacts of chronic pain on health-related quality of life, work productivity, depression and anxiety in a community-based study. Fam Pract 34:656–661. https://doi.org/10.1093/fampra/cmx034
Pereira S, Fontes F, Sonin T, Dias T, Fragoso M, Castro-Lopes J, Lunet N (2017) Neuropathic pain after breast cancer treatment: characterization and risk factors. J Pain Symptom Manage 54:877–888. https://doi.org/10.1016/j.jpainsymman.2017.04.011
Zeidan F, Baumgartner JN, Coghill RC (2019) The neural mechanisms of mindfulness-based pain relief: a functional magnetic resonance imaging-based review and primer. Pain Rep. https://doi.org/10.1097/PR9.0000000000000759
Reiner K, Tibi L, Lipsitz JD (2013) Do mindfulness-based interventions reduce pain intensity? A critical review of the literature. Pain Med 14:230–242. https://doi.org/10.1111/pme.12006
Chiesa A, Serretti A (2011) Mindfulness based cognitive therapy for psychiatric disorders: a systematic review and meta-analysis. Psychiatry Res 187:441–453. https://doi.org/10.1016/j.psychres.2010.08.011
Hilton L, Hempel S, Ewing BA, Apaydin E, Xenakis L, Newberry S, Colaiaco B, Maher AR, Shanman RM, Sorbero ME, Maglione MA (2017) Mindfulness meditation for chronic pain: systematic review and meta-analysis. Ann Behav Med 51:199–213. https://doi.org/10.1007/s12160-016-9844-2
Bawa FL, Mercer SW, Atherton RJ, Clague F, Keen A, Scott NW, Bond CM (2015) Does mindfulness improve outcomes in patients with chronic pain? Systematic review and meta-analysis. British J Gen Pract 65:e387-400. https://doi.org/10.3399/bjgp15X685297
Veehof MM, Trompetter HR, Bohlmeijer ET, Schreurs KM (2016) Acceptance-and mindfulness-based interventions for the treatment of chronic pain: a meta-analytic review. Cogn Behav Ther 45:5–31. https://doi.org/10.1080/16506073.2015.1098724
Anheyer D, Haller H, Barth J, Lauche R, Dobos G, Cramer H (2017) Mindfulness-based stress reduction for treating low back pain: a systematic review and meta-analysis. Ann Intern Med 166:799–807. https://doi.org/10.7326/M16-1997
Ball EF, Nur Shafina Muhammad Sharizan E, Franklin G, Rogozińska E (2017) Does mindfulness meditation improve chronic pain? A systematic review. Curr Opin Obstet Gynecol 29:359–366. https://doi.org/10.1097/GCO.0000000000000417
McClintock AS, McCarrick SM, Garland EL, Zeidan F, Zgierska AE (2019) Brief mindfulness-based interventions for acute and chronic pain: a systematic review. J Altern Complement Med 25:265–278. https://doi.org/10.1089/acm.2018.0351
Cramer H, Lauche R, Paul A, Dobos G (2012) Mindfulness-based stress reduction for breast cancer—a systematic review and meta-analysis. Curr Oncol 19:343–352. https://doi.org/10.3747/co.19.1016
Zainal NZ, Booth S, Huppert FA (2013) The efficacy of mindfulness-based stress reduction on mental health of breast cancer patients: a meta-analysis. Psychooncology 22:1457–1465. https://doi.org/10.1002/pon.3171
Haller H, Winkler MM, Klose P, Dobos G, Kuemmel S, Cramer H (2017) Mindfulness-based interventions for women with breast cancer: an updated systematic review and meta-analysis. Acta Oncol 56:1665–1676. https://doi.org/10.1080/0284186X.2017.1342862
Matchim Y, Armer JM, Stewart BR (2011) Mindfulness-based stress reduction among breast cancer survivors: a literature review and discussion. Oncol Nurs Forum. https://doi.org/10.1188/11.ONF.E61-E71
Zhang J, Xu R, Wang B, Wang J (2016) Effects of mindfulness-based therapy for patients with breast cancer: a systematic review and meta-analysis. Complement Ther Med 26:1. https://doi.org/10.1016/j.ctim.2016.02.012
Cifu G, Power MC, Shomstein S, Arem H (2018) Mindfulness-based interventions and cognitive function among breast cancer survivors: a systematic review. BMC Cancer 18:1–3. https://doi.org/10.1186/s12885-018-5065-3
Zhang Q, Zhao H, Zheng Y (2019) Effectiveness of mindfulness-based stress reduction (MBSR) on symptom variables and health-related quality of life in breast cancer patients—a systematic review and meta-analysis. Support Care Cancer 27:771–781. https://doi.org/10.1007/s00520-018-4570-x
Huang HP, He M, Wang HY, Zhou M (2016) A meta-analysis of the benefits of mindfulness-based stress reduction (MBSR) on psychological function among breast cancer (BC) survivors. Breast Cancer 23:568–576. https://doi.org/10.1007/s12282-015-0604-0
Schell LK, Monsef I, Wöckel A, Skoetz N (2019) Mindfulness-based stress reduction for women diagnosed with breast cancer. Cochrane Database Syst Rev. https://doi.org/10.1002/14651858.CD011518.pub2
Carlson LE (2016) Mindfulness-based interventions for coping with cancer. Ann N Y Acad Sci 1373:5–12. https://doi.org/10.1111/nyas.13029
Kabat-Zinn J (1994) Catalyzing movement towards a more contemplative/sacred-appreciating/non-dualistic society. In: Meeting of the Working Group
Ashburner J, Friston KJ (2000) Voxel-based morphometry—the methods. Neuroimage 11:805–821. https://doi.org/10.1006/nimg.2000.0582
Niu R, Du M, Ren J, Qing H, Wang X, Xu G, Lei D, Zhou P (2020) Chemotherapy-induced grey matter abnormalities in cancer survivors: a voxel-wise neuroimaging meta-analysis. Brain Imaging Behav. https://doi.org/10.1007/s11682-020-00402-7
Andryszak P, Wiłkość M, Izdebski P, Żurawski B (2017) A systemic literature review of neuroimaging studies in women with breast cancer treated with adjuvant chemotherapy. Contemp Oncol 21:6. https://doi.org/10.5114/wo.2017.66652
Feng Y, Zhang XD, Zheng G, Zhang LJ (2019) Chemotherapy-induced brain changes in breast cancer survivors: evaluation with multimodality magnetic resonance imaging. Brain Imaging Behav. https://doi.org/10.1007/s11682-019-00074-y
Smallwood RF, Laird AR, Ramage AE, Parkinson AL, Lewis J, Clauw DJ, Williams DA, Schmidt-Wilcke T, Farrell MJ, Eickhoff SB, Robin DA (2013) Structural brain anomalies and chronic pain: a quantitative meta-analysis of gray matter volume. J Pain 14:663–675. https://doi.org/10.1016/j.jpain.2013.03.001
Chen FY, Wei TA, Li YJ (2008) Advances in brain imaging of neuropathic pain. Chin Med J (Engl) 121:653–657. https://doi.org/10.1097/00029330-200804010-00015
Seifert F, Maihöfner C (2009) Central mechanisms of experimental and chronic neuropathic pain: findings from functional imaging studies. Cell Mol Life Sci 66:375–390. https://doi.org/10.1007/s00018-008-8428-0
Hatchard T, Mioduszewski O, Zambrana A, O’Farrell E, Caluyong M, Poulin PA, Smith AM (2017) Neural changes associated with mindfulness-based stress reduction (MBSR): current knowledge, limitations, and future directions. Psychol Neurosci 10:41. https://doi.org/10.1037/pne0000073
Reive C (2019) The biological measurements of mindfulness-based stress reduction: a systematic review. Explore 15:295–307. https://doi.org/10.1016/j.explore.2019.01.001
Hölzel BK, Carmody J, Vangel M, Congleton C, Yerramsetti SM, Gard T, Lazar SW (2011) Mindfulness practice leads to increases in regional brain gray matter density. Psychiatry Res Neuroimaging 191:36–43. https://doi.org/10.1016/j.pscychresns.2010.08.006
Hatchard T, Mioduszewski O, Khoo EL, Romanow H, Shergill Y, Tennant E, Leeming A, Fang Z, Poulin P, Smith AM (2021) Reduced emotional reactivity in breast cancer survivors with chronic neuropathic pain following mindfulness-based stress reduction (MBSR): an fMRI pilot investigation. Mindfulness 12:751–762. https://doi.org/10.1007/s12671-020-01546-9
Cleeland CS, Ryan KM (1994) Pain assessment: global use of hte Brief Pain Inventory. Ann Acad Med Singap 23(2):129–138
Baer RA, Smith GT, Hopkins J, Krietemeyer J, Toney L (2006) Using self-report assessment methods to explore facets of mindfulness. Assessment 13:27–45. https://doi.org/10.1177/1073191105283504
Pan PL, Zhong JG, Shang HF, Zhu YL, Xiao PR, Dai ZY, Shi HC (2015) Quantitative meta-analysis of grey matter anomalies in neuropathic pain. Eur J Pain 19:1224–1231. https://doi.org/10.1002/ejp.670
Xu X, Yuan H, Lei X (2016) Activation and connectivity within the default mode network contribute independently to future-oriented thought. Sci Rep 6:1. https://doi.org/10.1038/srep21001
Seghier ML (2013) The angular gyrus: multiple functions and multiple subdivisions. Neuroscientist 19:43–61. https://doi.org/10.1177/1073858412440596
Whitfield-Gabrieli S, Ford JM (2012) Default mode network activity and connectivity in psychopathology. Annu Rev Clin Psychol 8:49–76. https://doi.org/10.1146/annurev-clinpsy-032511-143049
Baliki MN, Mansour AR, Baria AT, Apkarian AV (2014) Functional reorganization of the default mode network across chronic pain conditions. PLoS ONE 9:e106133. https://doi.org/10.1371/journal.pone.0106133
Malfliet A, Coppieters I, Van Wilgen P, Kregel J, De Pauw R, Dolphens M et al (2017) Brain changes associated with cognitive and emotional factors in chronic pain: a systematic review. Eur J Pain 21:769–786. https://doi.org/10.1002/ejp.1003
Baliki MN, Geha PY, Apkarian AV, Chialvo DR (2008) Beyond feeling: chronic pain hurts the brain, disrupting the default-mode network dynamics. J Neurosci 28:1398–1403. https://doi.org/10.1523/JNEUROSCI.4123-07.2008
Loggia ML, Kim J, Gollub RL, Vangel MG, Kirsch I, Kong J et al (2013) Default mode network connectivity encodes clinical pain: an arterial spin labeling study. Pain 154:24–33. https://doi.org/10.1016/j.pain.2012.07.029
Harrison R, Zeidan F, Kitsaras G, Ozcelik D, Salomons TV (2019) Trait mindfulness is associated with lower pain reactivity and connectivity of the default mode network. J Pain 20:645–654. https://doi.org/10.1016/j.jpain.2018.10.011
Smith AM, Leeming A, Fang Z, Hatchard T, Mioduszewski O, Schneider MA, Ferdossifard A, Shergill Y, Khoo EL, Poulin P (2020) Mindfulness-based stress reduction alters brain activity for breast cancer survivors with chronic neuropathic pain: preliminary evidence from resting-state fMRI. J Cancer Surviv. https://doi.org/10.1007/s11764-020-00945-0
Emerson NM, Zeidan F, Lobanov OV, Hadsel MS, Martucci KT, Quevedo AS, Starr CJ, Nahman-Averbuch H, Weissman-Fogel I, Granovsky Y, Yarnitsky D (2014) Pain sensitivity is inversely related to regional grey matter density in the brain. Pain 155:566–573. https://doi.org/10.1016/j.pain.2013.12.004
Kucyi A, Salomons TV, Davis KD (2013) Mind wandering away from pain dynamically engages antinociceptive and default mode brain networks. Proc Natl Acad Sci USA 110:18692–18697. https://doi.org/10.1073/pnas.1312902110
Sundermann B, Dehghan Nayyeri M, Pfleiderer B, Stahlberg K, Jünke L, Baie L, Dieckmann R, Liem D, Happe T, Burgmer M (2019) Subtle changes of gray matter volume in fibromyalgia reflect chronic musculoskeletal pain rather than disease-specific effects. Eur J Neurosci 50:3958–3967. https://doi.org/10.1111/ejn.14558
Leung MK, Chan CC, Yin J, Lee CF, So KF, Lee TM (2013) Increased gray matter volume in the right angular and posterior parahippocampal gyri in loving-kindness meditators. Soc Cogn Affect Neurosci 8:34–39. https://doi.org/10.1093/scan/nss076
Santarnecchi E, D’Arista S, Egiziano E, Gardi C, Petrosino R, Vatti G, Reda M, Rossi A (2014) Interaction between neuroanatomical and psychological changes after mindfulness-based training. PLoS ONE 9:e108359. https://doi.org/10.1371/journal.pone.0108359
Martel M, Harvey M-P, Houde F, Balg F, Goffaux P, Leonard G (2017) Unravelling the effect of experimental pain on the corticomotor system using transcranial magnetic stimulation and electroencephalography. Exp Brain Res 235:1223–1231. https://doi.org/10.1007/s00221-017-4880-0
Neeb L, Bastian K, Villringer K, Israel H, Reuter U, Fiebach JB (2017) Structural gray matter alterations in chronic migraine: implications for a progressive disease? Headache J Head Face Pain. 57:400–416. https://doi.org/10.1111/head.13012
Parise M, Kubo TT, Doring TM, Tukamoto G, Vincent M, Gasparetto EL (2014) Cuneus and fusiform cortices thickness is reduced in trigeminal neuralgia. J Headache Pain 15:1–9. https://doi.org/10.1186/1129-2377-15-17
Mao C, Wei L, Zhang Q, Liao X, Yang X, Zhang M (2013) Differences in brain structure in patients with distinct sites of chronic pain: a voxel-based morphometric analysis. Neural Regen Res 8:2981. https://doi.org/10.3969/j.issn.1673-5374.2013.32.001
Kong F, Wang X, Song Y, Liu J (2016) Brain regions involved in dispositional mindfulness during resting state and their relation with well-being. Soc Neurosci 11:331–343. https://doi.org/10.1080/17470919.2015.1092469
Ward AM, Schultz AP, Huijbers W, Van Dijk KR, Hedden T, Sperling RA (2014) The parahippocampal gyrus links the default-mode cortical network with the medial temporal lobe memory system. Human Brain Mapp 35:1061–1073. https://doi.org/10.1002/hbm.22234
Hölzel BK, Ott U, Gard T, Hempel H, Weygandt M, Morgen K, Vaitl D (2008) Investigation of mindfulness meditation practitioners with voxel-based morphometry. Soc Cogn Affect Neurosci 3:55–61. https://doi.org/10.1093/scan/nsm038
Ploghaus A, Narain C, Beckmann CF, Clare S, Bantick S, Wise R, Matthews PM, Rawlins JN, Tracey I (2001) Exacerbation of pain by anxiety is associated with activity in a hippocampal network. J Neurosci 21:9896–9903. https://doi.org/10.1523/JNEUROSCI.21-24-09896.2001
Obermann M, Rodriguez-Raecke R, Naegel S, Holle D, Mueller D, Yoon MS, Theysohn N, Blex S, Diener HC, Katsarava Z (2013) Gray matter volume reduction reflects chronic pain in trigeminal neuralgia. Neuroimage 74:352–358. https://doi.org/10.1016/j.neuroimage.2013.02.029
Grant JA, Courtemanche J, Duerden EG, Duncan GH, Rainville P (2010) Cortical thickness and pain sensitivity in zen meditators. Emotion 10:43. https://doi.org/10.1037/a0018334
Cavanna AE, Trimble MR (2006) The precuneus: a review of its functional anatomy and behavioural correlates. Brain 129:564–583. https://doi.org/10.1093/brain/awl004
Fox KC, Nijeboer S, Dixon ML, Floman JL, Ellamil M, Rumak SP, Sedlmeier P, Christoff K (2014) Is meditation associated with altered brain structure? A systematic review and meta-analysis of morphometric neuroimaging in meditation practitioners. Neurosci Biobehav Rev 43:48–73. https://doi.org/10.1016/j.neubiorev.2014.03.016
Murphy C, Jefferies E, Rueschemeyer SA, Sormaz M, Wang HT, Margulies DS, Smallwood J (2018) Distant from input: evidence of regions within the default mode network supporting perceptually-decoupled and conceptually-guided cognition. Neuroimage 171:393–401. https://doi.org/10.1016/j.neuroimage.2018.01.017
Choe MK, Lim M, Kim JS, Lee DS, Chung CK (2018) Disrupted resting state network of fibromyalgia in theta frequency. Sci Rep 8:1–9. https://doi.org/10.1038/s41598-017-18999-z
Shergilll Y, Rice D, Khoo EL, Jarvis G, Zhang T, Taljaard M, Monterio L (2022) Mindfulness-based stress reduction in breast cancer survivors with chronic neuropathic pain: a randomized controlled trial. Pain Res Manag (In press)
Acknowledgements
The authors wish to acknowledge and thank the MRI technologists from the Ottawa Hospital and the group leaders for the MBSR groups. Additionally, thanks and gratitude are given to Jason Berard and Aziza Byron-Alhassan for providing additional support in coordinating and facilitating the neuroimaging sessions.
Funding
This work was supported by the Canadian Institutes of Health Research and the Canadian Breast Cancer Foundation.
Author information
Authors and Affiliations
Contributions
TH: investigation, writing—original draft, writing—review and editing. SP: writing—original draft, writing—review and editing. OM: investigation. SC: writing—original draft. TT: writing—original draft. OB: writing—review and editing. SH: writing—review and editing. PP: conceptualization, resources, investigation, funding acquisition. AS: conceptualization, supervision, investigation, funding acquisition, formal analysis, resources, visualization, writing—original draft, writing—review and editing.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethics approval
All procedures performed in this study involving human participants were in accordance with the ethical standards of the institutional research committee and with the 1964 Helsinki Declaration and its later amendments or comparable ethical standards.
Consent to participate
Informed consent was obtained from all individual participants included in the study.
Consent for publication
The authors affirm that human research participants provided informed consent for publication of the images in Figs. 1 and 2.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Hatchard, T., Penta, S., Mioduzsewski, O. et al. Increased gray matter following mindfulness-based stress reduction in breast cancer survivors with chronic neuropathic pain: preliminary evidence using voxel-based morphometry. Acta Neurol Belg 122, 735–743 (2022). https://doi.org/10.1007/s13760-022-01877-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s13760-022-01877-5