Abstract
Objective
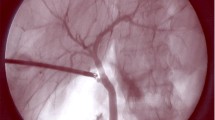
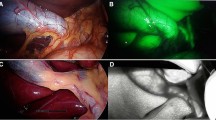
To compare indocyanine green dye fluorescence cholangiography (ICG-FC) with intra-operative cholangiography (IOC) in minimal access cholecystectomy for visualization of the extrahepatic biliary tree.
Background
Although studies have shown that ICG-FC is safe, feasible, and comparable to IOC to visualize the extrahepatic biliary tree, there is no comparative review.
Methods
We searched The Embase, PubMed, Cochrane Library, and Web of Science databases up to 8 April 2020 for all studies comparing ICG-FC with IOC in patients undergoing minimal access cholecystectomy. The primary outcomes were percentage visualization of the cystic duct (CD), common bile duct (CBD), CD-CBD junction, and the common hepatic duct (CHD). We used RevMan v5.3 software to analyze the data.
Results
Seven studies including 481 patients were included. Five studies, comprising 275 patients reported higher CD (RR = 0.90, p = 0.12, 95% CI 0.79–1.03, I2 = 74%) and CBD visualization rates (RR = 0.82, p = 0.09, 95% CI 0.65–1.03, I2 = 87%) by ICG-FC. Four studies, comprising 223 patients, reported higher CD-CBD junction visualization rates using ICG-FC compared to IOC (RR = 0.68, p = 0.06, 95% CI = 0.45–1.02, I2 = 94%). Four studies, comprising 210 patients, reported higher CHD visualization rates using ICG-FC compared to IOC (RR = 0.58, p = 0.03, 95% CI 0.35–0.93, I2 = 91%).
Conclusion
ICG-FC is safe, and it improves visualization of CHD.





Similar content being viewed by others
References
Stinton LM, Shaffer EA (2012) Epidemiology of gallbladder disease: cholelithiasis and cancer. Gut Liver 6(2):172–187
Strasberg SM (2018) Tokyo guidelines for the diagnosis of acute cholecystitis. J Am Coll Surg 227(6):624
Dempsey DT, Agrawal S (2018) Open cholecystectomy. In: Ashley SW (ed) UpToDate. https://www.uptodate.com/contents/open-cholecystectomy. Accessed 21 Apr 2020
Reynolds Jr W (2001) The first laparoscopic cholecystectomy. JSLS 5(1):89–94
Soper NJ, Stockmann PT, Dunnegan DL, Ashley SW (1992) Laparoscopic cholecystectomy. The new ‘gold standard’? Arch Surg 127(8):917–921
Csikesz NG, Singla A, Murphy MM, Tseng JF, Shah SA (2010) Surgeon volume metrics in laparoscopic cholecystectomy. Dig Dis Sci 55(8):2398–2405
National Institutes of Health Consensus Development Conference Statement on Gallstones and Laparoscopic Cholecystectomy (1993) Am J Surg 165(4):390–398
Hassler KR, Jones MW (2019) Laparoscopic cholecystectomy. In: StatPearls. StatPearls Publishing, Treasure Island. https://www.ncbi.nlm.nih.gov/books/NBK448145/. Accessed 21 Apr 2020
Ludwig K, Bernhardt J, Lorenz D (2002) Value and consequences of routine intraoperative cholangiography during cholecystectomy. S Surg Laparosc Endosc Percutan Tech 12(3):154–159
Woods MS (1996) Estimated costs of biliary tract complications in laparoscopic cholecystectomy based upon Medicare cost/charge ratios. A case-control study. Surg Endosc 10(10):1004–1007
Carroll BJ, Birth M, Phillips EH (1998) Common bile duct injuries during laparoscopic cholecystectomy that result in litigation. Surg Endosc 12(4):310–314
Altieri MS, Yang J, Obeid N, Zhu C, Talamini M, Pryor A (2018) Increasing bile duct injury and decreasing utilization of intraoperative cholangiogram and common bile duct exploration over 14 years: an analysis of outcomes in New York State. Surg Endosc 32(2):667–674
Nuzzo G, Giuliante F, Giovannini I, Ardito F, D’Acapito F, Vellone M, Murazio M, Capelli G (2005) Bile duct injury during laparoscopic cholecystectomy: results of an Italian national survey on 56 591 cholecystectomies. Arch Surg 140(10):986–992
Francoeur JR, Wiseman K, Buczkowski AK, Chung SW, Scudamore CH (2003) Surgeons’ anonymous response after bile duct injury during cholecystectomy. Am J Surg 185(5):468–475
Yamashita Y, Kimura T, Matsumoto S (2010) A safe laparoscopic cholecystectomy depends upon the establishment of a critical view of safety. Surg Today 40(6):507–513
Osayi SN, Wendling MR, Drosdeck JM, Chaudhry UI, Perry KA, Noria SF, Mikami DJ, Needleman BJ, Muscarella P 2nd, Abdel-Rasoul M, Renton DB, Melvin WS, Hazey JW, Narula VK (2015) Near-infrared fluorescent cholangiography facilitates identification of biliary anatomy during laparoscopic cholecystectomy. Surg Endosc 29(2):368–75
Reinhart MB, Huntington CR, Blair LJ, Heniford BT, Augenstein VA (2016) Indocyanine green: historical context, current applications, and future considerations. Surg Innov 23(2):166–175
Vlek SL, van Dam DA, Rubinstein SM, de Lange-de Klerk ESM, Schoonmade LJ, Tuynman JB, Meijerink WJHJ, Ankersmit M (2017) Biliary tract visualization using near-infrared imaging with indocyanine green during laparoscopic cholecystectomy: results of a systematic review. Surg Endosc 31(7):2731–2742
Lehrskov LL, Westen M, Larsen SS, Jensen AB, Kristensen BB, Bisgaard T (2020) Fluorescence or X-ray cholangiography in elective laparoscopic cholecystectomy: a randomized clinical trial. Br J Surg 107(6):655–661
Diana M, Soler L, Agnus V, D’Urso A, Vix M, Dallemagne B, Faucher V, Roy C, Mutter D, Marescaux J, Pessaux P (2017) Prospective evaluation of precision multimodal gallbladder surgery navigation: virtual reality, near-infrared fluorescence, and X-ray-based intraoperative cholangiography. Ann Surg 266(5):890–897
Moher D, Liberati A, Tezlaff J, Altman DG (2009) Preferred reporting items for systematic reviews and meta-analyses: the PRISMA statement. PLoS Med 6(7):e1000097
Thomson H, Sterne J, Higgins J (2015) ACROBAT-NRSi (A Cochrane risk of bias assessment tool: for non-randomized studies of interventions) for non-clinical community-based studies: a participatory workshop using a worked example from public health. In: Abstracts of the 23rd Cochrane Colloquium. https://abstracts.cochrane.org/2015-vienna/acrobat-nrsi-cochrane-risk-bias-assessment-tool-non-randomized-studies-interventions-non
Sterne JAC, Savović J, Page MJ, Elbers RG, Blencowe NS, Boutron I, Cates CJ, Cheng H-Y, Corbett MS, Eldridge SM, Hernán MA, Hopewell S, Hróbjartsson A, Junqueira DR, Jüni P, Kirkham JJ, Lasserson T, Li T, McAleenan A, Reeves BC, Shepperd S, Shrier I, Stewart LA, Tilling K, White IR, Whiting PF, Higgins JPT (2019) RoB 2: a revised tool for assessing risk of bias in randomised trials. BMJ 366:l4898
Review Manager (RevMan) [Computer program]. Version 5.3. (2014). The Nordic Cochrane Centre, The Cochrane Collaboration, Copenhagen
Quaresima S, Balla A, Palmieri L, Seitaj A, Fingerhut A, Ursi P, Paganini AM (2020) Routine near infra-red indocyanine green fluorescent cholangiography versus intraoperative cholangiography during laparoscopic cholecystectomy: a case-matched comparison. Surg Endosc 34(5):1959–1967
Dip F, Roy M, Lo Menzo E, Simpfendorfer C, Szomstein S, Rosenthal RJ (2015) Routine use of fluorescent incisionless cholangiography as a new imaging modality during laparoscopic cholecystectomy. Surg Endosc 29(6):1621–1626
Dip FF, Nahmod M, Alle L, Sarotto L, Anzorena FS, Ferraina P (2013) Fluorescence cholangiography in laparoscopic cholecystectomy experience in Argentina. Front Gastrointest Res 31:80–85
Prevot F, Rebibo L, Cosse C, Browet F, Sabbagh C, Regimbeau JM (2014) Effectiveness of intraoperative cholangiography using indocyanine green (versus contrast fluid) for the correct assessment of extrahepatic bile ducts during day-case laparoscopic cholecystectomy. J Gastrointest Surg 18(8):1462–1468
Indocyanine Green kit (2010) PULSION, 2010. http://dailymed.nlm.nih.gov/dailymed/drugInfo.cfm?id=15096. Accessed on 24 Apr 2020
Alander JT, Kaartinen I, Laakso A, Pätilä T, Spillmann T, Tuchin VV, Venermo M, Välisuo P (2012) A review of indocyanine green fluorescent imaging in surgery. Int J Biomed Imaging 2012:940585
Mordon S, Devoisselle JM, Soulie-Gegu S, Desmettre T (1998) Indocyanine green: physiochemical factors affecting its fluorescence in vivo. Microvasc Res 55:146–152
van den Bos J, Wieringa FP, Bouvy ND, Stassen LPS (2018) Optimizing the image of fluorescence cholangiography using ICG: a systematic review and ex vivo experiments. Surg Endosc 32:4820–4832
Way LW, Stewart L, Gantert W, Liu K, Lee CM, Whang K, Hunter JG (2003) Causes and prevention of laparoscopic bile duct injuries: analysis of 252 cases from a human factors and cognitive psychology perspective. Ann Surg 237(4):460–469
Roy M, Dip F, Nguyen D, Simpfendorfer CH, Menzo EL, Szomstein S, Rosenthal RJ (2017) Fluorescent incisionless cholangiography as a teaching tool for identification of Calot’s triangle. Surg Endosc 31(6):2483–2490
Author information
Authors and Affiliations
Corresponding author
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Lim, S.H., Tan, H.T.A. & Shelat, V.G. Comparison of indocyanine green dye fluorescent cholangiography with intra-operative cholangiography in laparoscopic cholecystectomy: a meta-analysis. Surg Endosc 35, 1511–1520 (2021). https://doi.org/10.1007/s00464-020-08164-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00464-020-08164-5