Purpose:
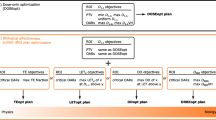
To investigate technical feasibilities of noncoplanar proton-beam therapy (PBT) on dose reduction to critical organs.
Material and Methods:
The degree of mechanical precision, rotational limitations of the gantry and the treatment couch were evaluated, and dose-volume histograms were compared for noncoplanar and coplanar PBT. Following these studies, three patients with tumors proximal to the optic nerve underwent noncoplanar PBT.
Results:
Noncoplanar PBT offered advantage in dose reduction to the optic nerve when compared to coplanar therapy. This advantage was more significant if the tumor reduced in size during treatment. None experienced radiation injury to the optic nerve during a short follow-up time of 7–12 months.
Conclusion:
Noncoplanar PBT appears to reduce doses to organs at risk.
Ziel:
Untersuchung der technischen Möglichkeiten der nichtkoplanaren Protonenstrahlentherapie (PST) im Hinblick auf die Reduktion der Dosisbelastung von kritischen Organen.
Material und Methodik:
Evaluiert wurden der Grad der mechanischen Präzision, die Rotationsbeschränkungen der Gantry und des Behandlungstischs, und es wurden Dosis-Volumen-Histogramme für die nichtkoplanare und koplanare PST verglichen. Im Anschluss daran wurden drei Patienten mit proximal des Sehnervs gelegenen Tumoren einer nichtkoplanaren PST unterzogen.
Ergebnisse:
Die nichtkoplanare PST war im Hinblick auf die Reduktion der Dosisbelastung des Sehnervs im Vergleich zur koplanaren Therapie von Vorteil. Dieser Vorteil war in den Fällen, in denen die Tumorgröße während der Behandlung abnahm, signifikanter. Bei keinem der Patienten traten während eines kurzen Nachuntersuchungszeitraums von 7–12 Monaten Strahlenschäden am Sehnerv auf.
Schlussfolgerung:
Die nichtkoplanare PST scheint die Dosisbelastung für Risikoorgane zu reduzieren.
Similar content being viewed by others
References
Baumert BG, Norton IA, Lomax AJ, et al. Dose conformation of intensity-modulated stereotactic photon beams, proton beams, and intensity-modulated proton beams for intracranial lesions. Int J Radiat Oncol Biol Phys 2004;60:1314–24.
Bekkering GE, Rutjes AW, Vlassov VV, et al. The effectiveness and safety of proton radiation therapy for indications of the eye. A systematic review. Strahlenther Onkol 2010;185:211–21.
Cardinale R, Won M, Choucair A, et al. A phase II trial of accelerated radiotherapy using weekly stereotactic conformal boost for supratentorial glioblastoma multiforme: RTOG 0023. Int J Radiat Oncol Biol Phys 2006;65:1422–8.
Chang JY, Zhang X, Wang X, et al. Significant reduction of normal tissue dose by proton radiotherapy compared with three-dimensional conformal or intensity-modulated radiation therapy in stage I or stage III non-small-cell lung cancer. Int J Radiat Oncol Biol Phys 2006;65:1087–96.
Chapet O, Khodri M, Jalade P, et al. Potential benefits of using non coplanar field and intensity modulated radiation therapy to preserve the heart in irradiation of lung tumors in the middle and lower lobes. Radiother Oncol 2006;80:333–40.
Clair WH, Adams JA, Bues M, et al. Advantage of protons compared to conventional X-ray or IMRT in the treatment of a pediatric patient with medulloblastoma. Int J Radiat Oncol Biol Phys 2004;58:727–34.
Cozzi L, Clivio A, Vanetti E, et al. Comparative planning study for proton radiotherapy of benign brain tumors. Strahlenther Onkol 2006;182:376–81.
Debus J, Wuendrich M, Pirzkall A, et al. High efficacy of fractionated stereotactic radiotherapy of large base-of-skull meningiomas: long-term results. J Clin Oncol 2001;19:3547–53.
Douglas JG, Einck J, Austin-Seymour M, et al. Neutron radiotherapy for recurrent pleomorphic adenomas of major salivary glands. Head Neck 2001;23:1037–42.
Emami B, Lyman J, Brown A, et al. Tolerance of normal tissue to therapeutic irradiation. Int J Radiat Oncol Biol Phys 1991;21:109–22.
Fuss M, Hug EB, Schaefer RA, et al. Proton radiation therapy (PRT) for pediatric optic pathway gliomas: comparison with 3D planned conventional photons and a standard photon technique. Int J Radiat Oncol Biol Phys 1999;45:1117–26.
Georg D, Georg P, Hillbrand M, et al. Assessment of improved organ at risk sparing for advanced cervix carcinoma utilizing precision radiotherapy techniques. Strahlenther Onkol 2008;184:586–91.
Gerweck LE, Kozin SV. Relative biological effectiveness of proton beams in clinical therapy. Radiother Oncol 1999;50:135–42.
Kocher M, Frommolt P, Borberg SK, et al. Randomized study of postoperative radiotherapy and simultaneous temozolomide without adjuvant chemotherapy for glioblastoma. Strahlenther Onkol 2008;184:572–9.
Kozak KR, Katz A, Adams J, et al. Dosimetric comparison of proton and photon three-dimensional, conformal, external beam accelerated partial breast irradiation techniques. Int J Radiat Oncol Biol Phys 2006;65:1572–8.
Krayenbuehl J, Davis JB, Ciernik IF. Dynamic intensity-modulated non-coplanar arc radiotherapy (INCA) for head and neck cancer. Radiother Oncol 2006;81:151–7.
Lee CT, Bilton SD, Famiglietti RM, et al. Treatment planning with protons for pediatric retinoblastoma, medulloblastoma, and pelvic sarcoma: how do protons compare with other conformal techniques? Int J Radiat Oncol Biol Phys 2005;63:362–72.
Ma’aita JK, Al-Kaisi N, Al-Tamimi S, et al. Salivary gland tumors in Jordan: a retrospective study of 221 patients. Croat Med J 1999;40:539–42.
Milker-Zabel S, Zabel-du Bois A, Huber P, et al. Intensity-modulated radiotherapy for complex-shaped meningioma of the skull base: long-term experience of a single institution. Int J Radiat Oncol Biol Phys 2007;68:858–63.
Mizumoto M, Tsuboi K, Igaki H, et al. Phase I/II trial of hyperfractionated concomitant boost proton radiotherapy for supratentorial glioblastoma multiforme. Int J Radiat Oncol Biol Phys 2010: in press (Epub 2009 Aug 19).
Mock U, Bogner J, Georg D, et al. Comparative treatment planning on localized prostate carcinoma conformal photon- versus proton-based radiotherapy. Strahlenther Onkol 2005;181:448–55.
Mock U, Georg D, Bogner J, et al. Treatment planning comparison of conventional, 3D conformal, and intensity-modulated photon (IMRT) and proton therapy for paranasal sinus carcinoma. Int J Radiat Oncol Biol Phys 2004;58:147–54.
Mu X, Bjork-Eriksson T, Nill S, et al. Does electron and proton therapy reduce the risk of radiation induced cancer after spinal irradiation for childhood medulloblastoma? A comparative treatment planning study. Acta Oncol 2005;44:554–62.
Nicolini G, Fogliata A, Cozzi L. Critical appraisal of a non-coplanar technique for radiotherapy of breast minimizing lung involvement. Radiother Oncol 2005;76:319–25.
Sterzing F, Schubert K, Sroka-Perez G, et al. Helical tomotherapy. Experiences of the first 150 patients in Heidelberg. Strahlenther Onkol 2008;184:8–14.
Tsunashima Y, Sakae T, Shioyama Y, et al. Correlation between the respiratory waveform measured using a respiratory sensor and 3D tumor motion in gated radiotherapy. Int J Radiat Oncol Biol Phys 2004;60:951–8.
Vargas C, Fryer A, Mahajan C, et al. Dose-volume comparison of proton therapy and intensity-modulated radiotherapy for prostate cancer. Int J Radiat Oncol Biol Phys 2008;70:744–51.
Wang C, Nakayama H, Sugahara S, et al. Comparisons of dose-volume histograms for proton-beam versus 3-D conformal X-ray therapy in patients with stage I non-small cell lung cancer. Strahlenther Onkol 2010;185:231–4.
Weber DC, Bogner J, Verwey J, et al. Proton beam radiotherapy versus fractionated stereotactic radiotherapy for uveal melanomas: a comparative study. Int J Radiat Oncol Biol Phys 2005;63:373–84.
Weber DC, Trofimov AV, Delaney TF, et al. A treatment planning comparison of intensity modulated photon and proton therapy for paraspinal sarcomas. Int J Radiat Oncol Biol Phys 2004;58:1596–606.
Author information
Authors and Affiliations
Corresponding author
Additional information
An erratum to this article can be found at http://dx.doi.org/10.1007/s00066-010-7001-6
Rights and permissions
About this article
Cite this article
Mizumoto, M., Nakayama, H., Tokita, M. et al. Technical Considerations for Noncoplanar Proton-Beam Therapy of Patients with Tumors Proximal to the Optic Nerve. Strahlenther Onkol 186, 36–39 (2010). https://doi.org/10.1007/s00066-009-2019-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00066-009-2019-3