Abstract
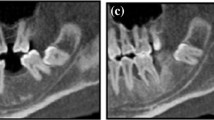
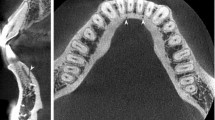
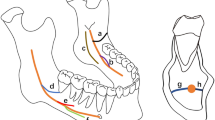
The neurovascular bundle may be vulnerable during surgical procedures involving the mandible, especially when anatomical variations are present. Increased demand of implant surgeries, wider availability of three-dimensional exams, and lack of clear definitions in the literature indicate that features of anatomical variations should be revisited. The objective of the study was to evaluate features of anatomical variations related to mandibular canal (MC), such as bifid canals, anterior loop of mental nerve, and corticalization of MC. Additionally, bone trabeculation at the submandibular gland fossa region (SGF) was assessed and related to visibility of MC. Cone beam computed tomography exams from 100 patients (200 hemimandibles) were analyzed and the following parameters were registered: diameter and corticalization of MC; trabeculation in SGF region; presence of bifid MC, position of bifurcations, diameter, and direction of bifid canals; and measurement of anterior loops by two methods. Corticalization of the MC was observed in 59% of hemimandibles. In 23%, MC could be identified despite absence of corticalization. Diameter of MC was between 2.1 and 4 mm for nearly three quarters of the sample. In 80% of the sample trabeculation at the SGF was either decreased or not visible, and such cases showed correlation with absence of MC corticalization. Bifid MC affected 19% of the patients, mostly associated with additional mental foramina. Clinically significant anterior loop (>2 mm of anterior extension) was observed in 22–28%, depending on the method. Our findings, together with previously reported limitations of conventional exams, draw attention to the unpredictability related to anatomical variations in neurovascularization, showing the contribution of individual assessment through different views of three-dimensional imaging prior to surgical procedures in the mandible.



Similar content being viewed by others
References
Jacobs R, Lambrichts I, Liang X, Martens W, Mraiwa N, Adriaensens P, Gelan J (2007) Neurovascularization of the anterior jaw bones revisited using high resolution magnetic resonance imaging. Oral Surg Oral Med Oral Pathol Oral Radiol Endod 103:683–693
Juodzbalys G, Wang H, Sabalys G (2010) Anatomy of mandibular vital structures. Part I: mandibular canal and inferior alveorlar neurovascular bundle in relation with dental implantology. J Oral Maxillofac Res 1:e2
Kilic C, Kamburoglu K, Ozen T, Balcioglu HA, Kurt B, Kutoglu T, Ozan H (2010) The position of the mandibular canal and histologic feature of the inferior alveolar nerve. Clin Anat 23:34–42
Mardinger O, Chaushu G, Arensburg B, Taicher S, Kaffe I (2000) Anterior loop of the mental canal: an anatomical-radiologic study. Implant Dent 9:120–125
Kuzmanovic DV, Payne AGT, Kieser JA, Dias GJ (2003) Anterior loop of the mental nerve: a morphological and radiographic study. Clin Oral Implants Res 14:464–471
Hu KS, Yun HS, Hur MS, Kwon HJ, Abe S, Kim HJ (2007) Branching patterns and intraosseous course of the mental nerve. J Oral Maxillofac Surg 65:2288–2294
Uchida Y, Yamashita Y, Goto M, Hanihara T (2007) Measurement of anterior loop length for the mandibular canal and diameter of the mandibular incisive canal to avoid nerve damage when installing endosseous implants in the interforaminal region. J Oral Maxillofac Surg 65:1772–1779
Kaya Y, Sencimen M, Sahin S, Okcu KM, Dogan N, Bahcecitapar M (2008) Retrospective radiographic evaluation of the anterior loop of the mental nerve: comparison between panoramic radiography and spiral computerized tomography. Int J Oral Maxillofac Implants 23:919–925
Ngeow WC, Dionysius DD, Ishak H, Nambiar P (2009) A radiographic study on the visualization of the anterior loop in dentate subjects of different age groups. J Oral Sci 51:231–237
Uchida Y, Noguchi N, Goto M, Yamashita Y, Hanihara T, Takamori H, Sato I, Kawai T (2009) Measurement of anterior loop length for the mandibular canal and diameter of the mandibular incisive canal to avoid nerve damage when installing endosseous implants in the interforaminal region: a second attempt introducing cone beam computed tomography. J Oral Maxillofac Surg 67:744–750
Liang X, Jacobs R, Hassan B, Li LM, Pauwels R, Corpas L, Couto Souza P, Martens M, Shahbazian M, Alonso A, Lambrichts I (2010) A comparative evaluation of Cone Beam Computed Tomography (CBCT) and Multi-Slice CT (MSCT)—Part I: on subjective image quality. Eur J Radiol 75:265–269
Lew K, Townsend G (2006) Failure to obtain adequate anaesthesia associated wiyh a bifid mandibular canal: a case report. Aust Dent J 51:86–90
Nortjé CJ, Farman AG, Grotepass FW (1977) Variations in the anatomy normal of the inferior dental (mandibular) canal: a retrospective study of panoramic radiographs from 3612 routine dental patients. Br J Oral Surg 15:55–63
Langlais RP, Broadus R, Glass BJ (1985) Bifid mandibular canals in panoramic radiographs. JADA 110:923–926
Sanchis JM, Peñarrocha M, Soler F (2003) Bifid mandibular canal. J Oral Maxillofac Surg 61:422–424
Naitoh M, Hiraiwa Y, Aimiya H, Ariji E (2009) Observation of bifid mandibular canal using cone-beam computerized tomography. Int J Oral Maxillofac Implants 24:155–159
Kuribayashi A, Watanabe H, Imaizumi A, Tantanapornkul W, Katakami K, Kurabayashi T (2010) Bifid mandibular canals: cone beam computed tomography evaluation. Dentomaxillofac Radiol 39:235–239
Chávez-Lomeli ME, Mansilla-Lory J, Pompa JA, Kjær I (1996) The human mandibular canal arises from three separate canals innervating different tooth groups. J Dent Res 75:1540–1544
Sawyer DR, Kiely ML (1991) Retromolar foramen: a mandibular variant important to dentistry. Ann Dent 50:16–18
Bilecenoglu B, Tuncer N (2006) Clinical and anatomical study of retromolar foramen and canal. J Oral Maxillofac Surg 64:1493–1497
Parnia F, Fard EM, Mahboud F, Hafzeqoran A, Gavgani FE (2010) Tomographic volume evaluation of submandibular fossa in patients requiring dental implants. Oral Surg Oral Med Oral Pathol Oral Radiol Endod 109:e32–e36
Oliveira-Santos C, Rubira-Bullen IR, Dezzoti MSG, Capelozza ALA, Fischer CM, Poleti ML (2011) Visibility of the mandibular canal on CBCT cross-sectional images. J Appl Oral Sci 19:130–133
Lofthag-Hansen S, Gröndahl K, Ekestubbe A (2009) Cone-beam CT for preoperative implant planning in the posterior mandible: visibility of anatomic landmarks. Clin Implant Dent Relat Res 11:246–255
Liang X, Jacobs R, Corpas LS, Semal P, Lambrichts I (2009) Chronologic and geographic variability of neurovascular structures in the human mandible. Forensic Sci Int 190:24–32
Gijbels F, Jacobs R, Bogaerts R, Debaveye D, Verlinden S, Sanderink G (2005) Dosimetry of digital panoramic imaging. Part I: patient exposure. Dento-Maxillo-Facial Radiol 34:145–149
Ludlow JB, Davies-Ludlow LE, White SC (2008) Patient risk related to common dental radiographic examinations: the impact of 2007 international commission on radiological protection recommendations regarding dose calculation. J Am Dent Assoc 139:1237–1243
Pauwels R, Beinsberger J, Collaertb B, Theodorakou C, Rogers J, Walker A, Cockmartin L, Bosmans H, Jacobs R, Bogaerts R, Horner K (2011) Effective dose range for dental cone beam computed tomography scanners. Eur J Radiol (in press), doi:10.1016/j.ejrad.2010.11.028
Loubele M, Bogaerts R, Van Dijck E, Pauwels R, Vanheusden S, Suetens P, Marchal G, Sanderink G, Jacobs R (2009) Comparison between effective radiation dose of CBCT and MSCT scanners for dentomaxillofacial applications. Eur J Radiol 71:461–468
Acknowledgments
Author COS was granted PDEE scholarship—doctorate program with part of studies developed abroad, from CAPES-Brazil (Brazilian Government Agency).
Conflicts of interest
The authors declare no conflicts of interest regarding the manuscript and publication of the manuscript and its potential implications.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
de Oliveira-Santos, C., Souza, P.H.C., de Azambuja Berti-Couto, S. et al. Assessment of variations of the mandibular canal through cone beam computed tomography. Clin Oral Invest 16, 387–393 (2012). https://doi.org/10.1007/s00784-011-0544-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00784-011-0544-9